Periodontal ligament
Overview
The periodontal ligament, commonly abbreviated as the PDL is a group of specialized connective tissue fibers that essentially attach a tooth to the alveolar bone within which it sits. These fibers help the tooth withstand the naturally substantial compressive forces which occur during chewing and remain embedded in the bone.
Another function of the PDL is to serve as a source of proprioception, or sensory innervation, so that the brain can detect the forces being placed on the teeth and react accordingly. To achieve this end, there are pressure sensitive receptors within the PDL which allow the brain to discern the amount of force being placed on a tooth during chewing, for example. This is important because the exposed surface of the tooth, called enamel, has no such sensory receptors itself.
In addition to the PDL fibers, there is another set of fibers, known as the gingival fibers, which attach the teeth to their adjacent gingival tissue. Both the gingival fibers, as well as the PDL fibers, are composed primarily of type I collagen.[1]
Development of the PDL
Shortly after the beginning of root formation and the formation of the outer dentinal layer of root, the PDL is formed. The external and internal dental epithelia proliferate from the cervical loop of the dental organ to form Hertwig's epithelial root sheath. This sheath is double layered. Because of growth changes, the root sheath is stretched and subsequently fragments to form discrete clusters of the epithelial cells known as epithelial cell rests of Malassez (ERM). It is now in the development of the tooth that PDL formation occurs. The enamel organ and Hertwig’s epithelial root sheath are surrounded by a dental sac that is formed by condensed cells. A thin layer of these cells lies adjacent to the dental (enamel) organ, known as the dental follicle. The cells of the dental follicle divide and differentiate into cementoblasts, fibroblasts and osteoblasts. The fibroblasts synthesize fibers and ground substance that become the PDL. These fibers of then embed themselves into the newly formed cementum laid down by cementoblasts at one end, and into the bone laid down by osteoblasts at their other end.
When a tooth erupts into the oral cavity, these fibers become oriented in a particularly specific array, to be explained in detail in the sections below. The fiber bundles of the periodontal ligament gradually thicken after the teeth have been in function for a while.
Structure of the PDL
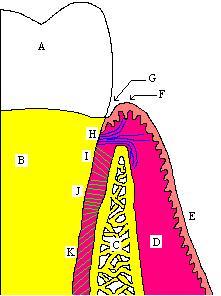
The periodontal ligament is one of the four supporting tissue of a the tooth, otherwise referred to as the periodontium. They are about 0.2 mm in width, and these dimensions decrease with age. As stated, the PDL fibers are composed primarily of type I collagen, although type III fibers are also involved. Compared to most other ligaments of the body, these are highly vascularized.
Types of fibers
Individual fibers of the ligament have a diameter of 55 nm. The PDL fibers are categorized according to their orientation and location along the tooth.
Transeptal fibers
Transeptal fibers run between two adjacent teeth in the same jaw. They run from the cementum just apical to where the gums attach to a tooth and insert at the cementum of an adjacent tooth at about the same level. Transeptal fibers are believed to be responsible for returning teeth to their original state after orthodontic therapy. Although technically part of the gingival ligament, these fibers are frequently included in studies involving the periodontal ligament.
Alveolar crest fibers
Alveolar crest fibers attach to the cementum just apical to the cementoenamel junction, run downward, and insert into the alveolar bone.
Horizontal fibers
Horizontal fibers attach to the cementum apical to the alveolar crest fibers and run perpendicularly from the root of the tooth to the alveolar bone.
Oblique fibers
Oblique fibers are the most numerous fibers in the periodontal ligament. They attach apical to the horizontal fibers and run diagonally toward the crown of the tooth inserting to the alveolar bone there. Because they are the most numerous, these fibers are believed to be primarily responsible in absorbing the chewing forces on the tooth. They are hence the main support of the tooth.
Apical fibers
Apical fibers are at the apex of a root. They attach from the cementum and insert to the surrounding bone at the base of the socket. They are also the first to offer resistance to movement of the tooth in an occlusal direction (e.g. when the tooth is being extracted)
Interradicular fibers
Interradicular fibers are only found between the roots of multi-rooted teeth, such as a molars. They also attach from the cementum and insert to the nearby alveolar bone.
See also
References
- Sources consulted
- Ten Cate, A. R. (1998) [1980]. Oral Histology: development, structure, and function (5th ed. ed.). St. Louis: Mosby. ISBN 0-8151-2952-1.
- Endnotes
- ↑ Carranza's Clinical Periodontology, 9th Ed., W.B. Saunders, 2002, page 26