Orbital cellulitis pathophysiology
|
Orbital cellulitis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Orbital cellulitis pathophysiology On the Web |
|
American Roentgen Ray Society Images of Orbital cellulitis pathophysiology |
|
Risk calculators and risk factors for Orbital cellulitis pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Tarek Nafee, M.D. [2]
Overview
Orbital cellulitis occurs secondary to microbial infiltration of the deep soft tissue cells surrounding the eye, posterior to the orbital septum. The infiltration can occur by means of extension of an adjacent infection (e.g., rhinosinusitis), by direct inoculation through traumatic or iatrogenic pathways, or by hematogenous spread from a distant infected site. Regardless of the mode of infiltration of the retroseptal orbital space, symptoms may arise due to the immune system triggering a regional acute inflammatory response.[1][2][3][4][5]
Pathogenesis
Orbital cellulitis occurs secondary to microbial infiltration of the deep soft tissue cells surrounding the eye, posterior to the orbital septum.[1] Damage to the cells triggers an acute inflammatory response resulting in vasodilation, increased vascular permeability, and induction of a cascade of inflammatory markers and white blood cell chemoattractants.[4]
Extension of adjacent infection
Orbital cellulitis may spread through direct extension of acute or chronic adjacent infections. This is due to the fragility of the medial and inferior orbital walls, the presence of natural foramina and defects in these structures, and the medial check ligaments extending from extraocular structures and muscle sheaths to the thin medial orbital wall, which separates the orbital cavity from the paranasal sinuses. Some infections that may affect these structures include:[1][2][3]
- Rhinosinusitis (ethmoid sinusitis and pansinusitis)
- Dacryocystitis/Dacryoadenitis
- Panophthalmitis
- Infected tumor
- Otitis media
- Mucormycosis
- Dental abscess
Direct Inoculation
Traumatic Inoculation
Orbital cellulitis may occur as a result of microbial inoculation to the orbital space due to trauma. Examples of this include:[1]
Iatrogenic Inoculation
Orbital cellulitis may also occur as a result of direct inoculation during surgical procedures, such as:[1][2]
- Ocular or periocular surgeries
- Paranasal sinus surgeries
- Other ENT surgeries
Hematogenous Seeding
In some cases, infections from a distant source may seed to the retroseptal orbital soft tissue by means of hematogenous spread in patients with bacteremia. This highly vascularized space, coupled with a valveless inferior ophthalmic vein, has been implicated in facilitating this mode of infection.[1][2][5]
Associated Conditions
The following conditions are associated with orbital cellulitis:[2]
- Chronic sinusitis
- Upper respiratory tract infection
- Subperiosteal abscess
Gross Pathology
The following are gross pathology images of orbital cellulitis:[6][7]
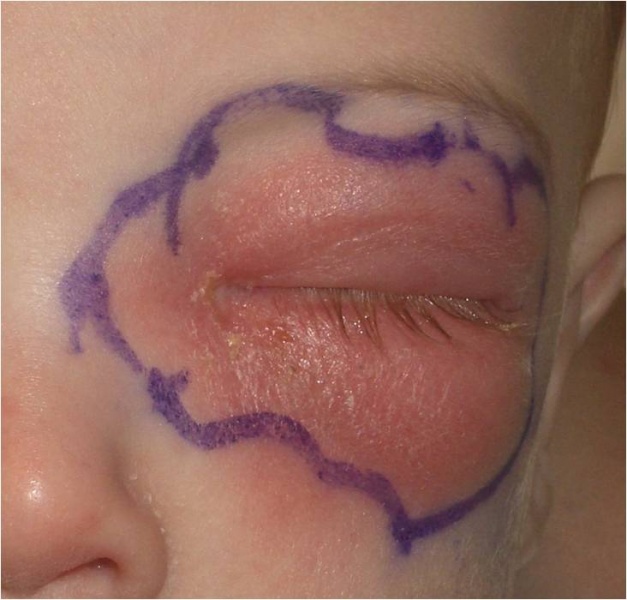
-
Orbital cellulitis in the left eye of a child
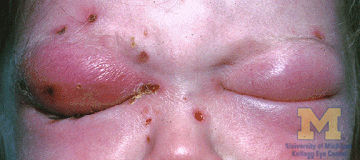
-
Bilateral orbital cellulitis gross pathology
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 Hasanee K, Sharma S (2004). "Ophthaproblem. Orbital cellulitis". Can Fam Physician. 50: 359, 365, 367. PMC 2214559. PMID 15318671.
- ↑ 2.0 2.1 2.2 2.3 2.4 Chaudhry IA, Al-Rashed W, Arat YO (2012). "The hot orbit: orbital cellulitis". Middle East Afr J Ophthalmol. 19 (1): 34–42. doi:10.4103/0974-9233.92114. PMC 3277022. PMID 22346113.
- ↑ 3.0 3.1 Turvey TA, Golden BA (2012). "Orbital anatomy for the surgeon". Oral Maxillofac Surg Clin North Am. 24 (4): 525–36. doi:10.1016/j.coms.2012.08.003. PMC 3566239. PMID 23107426.
- ↑ 4.0 4.1 U.S. National Library of Medicine Medlineplus(2014) https://medlineplus.gov/ency/article/000821.htm
- ↑ 5.0 5.1 Zhang J, Stringer MD (2010). "Ophthalmic and facial veins are not valveless". Clin Experiment Ophthalmol. 38 (5): 502–10. doi:10.1111/j.1442-9071.2010.02325.x. PMID 20491800.
- ↑ American Academy of Ophthalmology EyeWiki(2010)http://eyewiki.org/File%3AOrbital_cellulitis1.jpg
- ↑ University of Michigan Eyes Have It(2009)http://eyewiki.org/File%3AOrbital_cellulitis1.jpg