Mantoux test
|
WikiDoc Resources for Mantoux test |
|
Articles |
|---|
|
Most recent articles on Mantoux test Most cited articles on Mantoux test |
|
Media |
|
Powerpoint slides on Mantoux test |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Mantoux test at Clinical Trials.gov Clinical Trials on Mantoux test at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Mantoux test
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Mantoux test Discussion groups on Mantoux test Patient Handouts on Mantoux test Directions to Hospitals Treating Mantoux test Risk calculators and risk factors for Mantoux test
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Mantoux test |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Alejandro Lemor, M.D. [2]
Synonyms and keywords: PPD, TB skin test, TST, tst
Overview
The Mantoux tuberculin skin test (TST) is the standard method of determining whether a person is infected with Mycobacterium tuberculosis. Reliable administration and reading of the TST requires standardization of procedures, training, supervision, and practice.
Procedure
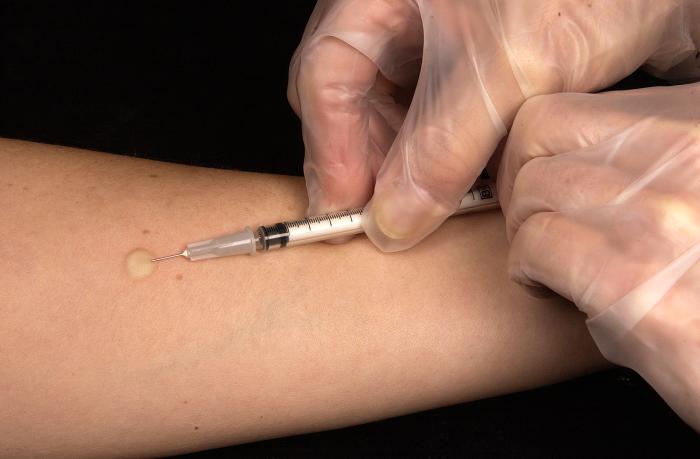
The TST is performed by injecting 0.1 ml of tuberculin purified protein derivative (PPD) into the inner surface of the forearm. The injection should be made with a tuberculin syringe, with the needle bevel facing upward. The TST is an intradermal injection. When placed correctly, the injection should produce a pale elevation of the skin (a wheal) 6 to 10 mm in diameter.
The skin test reaction should be read between 48 and 72 hours after administration. A patient who does not return within 72 hours will need to be rescheduled for another skin test.
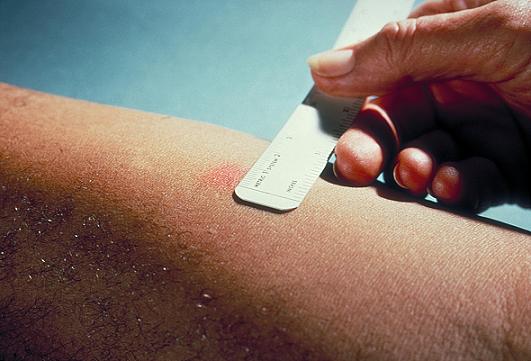
The reaction should be measured in millimeters of the induration (palpable, raised, hardened area or swelling). The reader should not measure erythema (redness). The diameter of the indurated area should be measured across the forearm (perpendicular to the long axis).
Classification of Tuberculin Reaction
Skin test interpretation depends on two factors:
- Measurement in millimeters of the induration.
- Person’s risk of being infected with TB and of progression to disease if infected.
| Tuberculin Reaction | Considered a Positive Result in: |
|---|---|
| ≥ 5 mm |
|
| ≥ 10 mm |
|
| ≥ 15 mm |
|
| Table adapted from CDC[1] | |
Contraindications
TST is contraindicated only for persons who have had a severe reaction (e.g., necrosis, blistering, anaphylactic shock, or ulcerations) to a previous TST. It is not contraindicated for any other persons, including infants, children, pregnant women, persons who are HIV-infected, or persons who have been vaccinated with BCG.
False-Poisitve and False-Negative Reactions
In some persons who are infected with M. tuberculosis, the ability to react to tuberculin may wane over time. When given a TST years after infection, these persons may have a false-negative reaction. However, the TST may stimulate the immune system, causing a positive, or boosted reaction to subsequent tests. Giving a second TST after an initial negative TST reaction is called two-step testing.
| False-Positive Reactions | False-Negative Reactions |
|---|---|
Some persons may react to the TST even though they are not infected with M. tuberculosis. The causes of these false-positive reactions may include, but are not limited to, the following:
|
Some persons may not react to the TST even though they are infected with M. tuberculosis. The reasons for these false-negative reactions may include, but are not limited to, the following:
|
| Table adapted from CDC[1] | |
Two-step Testing
Two-step testing is useful for the initial skin testing of adults who are going to be retested periodically, such as health care workers or nursing home residents. This two-step approach can reduce the likelihood that a boosted reaction to a subsequent TST will be misinterpreted as a recent infection.
See also
References