Intraocular lens
|
WikiDoc Resources for Intraocular lens |
|
Articles |
|---|
|
Most recent articles on Intraocular lens Most cited articles on Intraocular lens |
|
Media |
|
Powerpoint slides on Intraocular lens |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Intraocular lens at Clinical Trials.gov Trial results on Intraocular lens Clinical Trials on Intraocular lens at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Intraocular lens NICE Guidance on Intraocular lens
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Intraocular lens Discussion groups on Intraocular lens Patient Handouts on Intraocular lens Directions to Hospitals Treating Intraocular lens Risk calculators and risk factors for Intraocular lens
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Intraocular lens |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-in-Chief: Kenneth J. Hoffer, M.D. [1], Clinical Professor of Ophthalmology, UCLA, St. Mary's Eye Center
Overview
An intraocular lens (IOL) is an implanted lens in the eye, usually replacing the existing crystalline lens because it has been clouded over by a cataract, or as a form of refractive surgery to change the eye's optical power. It usually consists of a small plastic lens with plastic side struts, called haptics, to hold the lens in place within the capsular bag inside the eye. IOLs were traditionally made of an inflexible material (PMMA) though this largely been superseded by the use of flexible materials. Most IOLs fitted today are fixed monofocal lenses matched to distance vision. However, other types are available, such as multifocal IOLs which provide the patient with multiple-focused vision at far and reading distance, and adaptive IOLs which provide the patent with limited visual accommodation.
Insertion of an intraocular lens for the treatment of cataracts is the most commonly performed eye surgical procedure. The procedure can be done under local anesthesia with the patient awake throughout the operation. The use of a flexible IOL enables the lens to be rolled for insertion into the capsule through a very small incision, thus avoiding the need for stitches, and this procedure usually takes less than 30 minutes in the hands of an experienced ophthalmologist. The recovery period is about 2-3 weeks. After surgery, patients should avoid strenuous exercise or anything else that significantly increases blood pressure. They should also visit their ophthalmologists regularly for several months so as to monitor the implants.
IOL implantation carries several risks associated with eye surgeries, such as infection, loosening of the lens, lens rotation, inflammation, night time halos. Though IOLs enable some patients to have reduce dependence on glasses, most patents still rely on glasses for driving and reading.
History
Sir Harold Ridley was the first to successfully implant an intraocular lens on November 29, 1949, at St Thomas' Hospital at London. That first intraocular lens was manufactured by the Rayner company of Brighton, East Sussex, England from Perspex CQ made by ICI. It is said that idea of implanting an intraocular lens came to him after an intern asked him why he was not replacing the lens he had removed during cataract surgery. The first lenses used were made of glass, they were heavy and were prone to shatter during Nd:YAG capsulotomy. Plastic materials were used later, when someone noticed that they were inert, after seeing pilots of World War II with pieces of shattered windshields in their eyes. The intraocular lens did not find widespread acceptance in cataract surgery until the 1970s, when further developments in lens design and surgical techniques had come about. Currently, more than a million IOLs are implanted annually in the United States.
Materials used for intraocular lenses
Polymethylmethacrylate (PMMA) was the first material to be used successfully in intraocular lenses. British ophthalmologist Sir Harold Ridley observed that Royal Air Force pilots who sustained eye injuries during World War II involving PMMA windshield material did not show any rejection or foreign body reaction. Deducing that the transparent material was inert and useful for implantation in the eye, Ridley designed and implanted the first intraocular lens in a human eye.
Advances in technology have brought about the use of silicone and acrylic, both of which are soft foldable inert materials. This allows the lens to be folded and inserted into the eye through a smaller incision. PMMA and acrylic lenses can also be used with small incisions and are a better choice in people who have a history of uveitis, have diabetic retinopathy requiring vitrectomy with replacement by silicone oil or are at high risk of retinal detachment. Acrylic is not always an ideal choice due to its added expense. Latest advances include IOLs with square-edge design, non-glare edge design and yellow dye added to the IOL.
In the United States, a new category of intraocular lenses was opened with the approval by the Food and Drug Administration in 2003 of the only accommodating IOL called Crystalens. The position of the lens can be changed by the ciliary muscles of the eye, allowing for natural focusing. Crystalens is a 360 degree square edged plate silicone lens with hinges to allow for position changes for near, intermediate and distance vision, like the natural crystalline lens. In 2006, the crystalens Five-O was re-designed to allow for a larger optic and greater stability while retaining the same natural focusing power. The crystalens allows for a small surgical incision, using similar cataract surgical procedure. There is less risk of glare, halos and night vision problems because unlike multifocal lenses, crystalens has a single point of focus, projects only 1 image to the back of the retina, and does not split or lose light rays as multifocal lenses do. The crystalens is similarly priced as multi-focal or multi-image lenses.
Other IOLs include:
- Blue Light Filtering IOLs filter the UV and high-energy blue light present in natural and artificial light, both of which can cause vision problems.
- Toric IOLs (1998) correct astigmatic vision.
PMMA is still widely used in Asia and Africa for its low cost and favorable surgical results with high quality cataract surgery. Newer advances have brought about the use of silicone acrylate which is a soft material. This allows the lens to be folded and inserted into the eye through a smaller incision. Acrylic lenses can also be used with small incisions and are a better choice in people who have a history of uveitis or are at high risk of retinal detachment. Acrylic is not always an ideal choice due to its added expense. New FDA-approved multifocal intraocular lens implants allow most post operative cataract patients the advantage of glass-free vision. These new multifocal lenses are not a covered expense under most insurance plans (Medicare decided to stop covering them in May 2005) and can cost the patient upwards of $1500 per eye..
Phakic, aphakic and pseudophakic IOLs
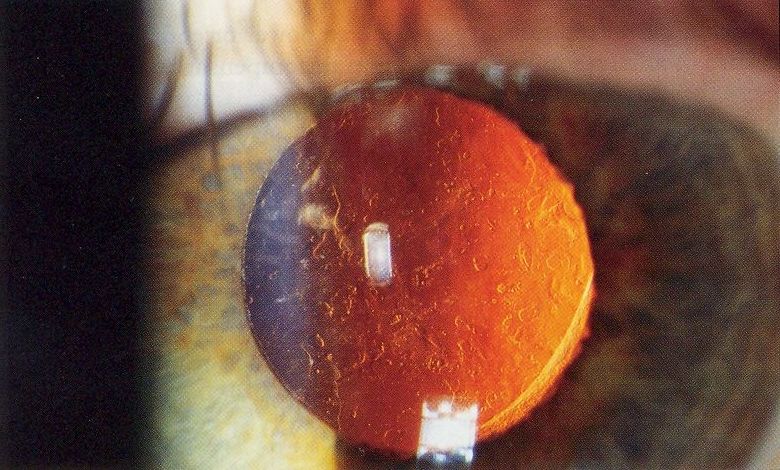
- Phakia is the presence of the natural crystalline lens.
- Aphakia is the absence of the natural crystalline lens, either from natural causes or because it has been removed.
- Pseudophakia is the substitution of the natural crystalline lens with a synthetic lens. Pseudophakic IOLs are used in cataract surgery.
The root of these words comes from the Greek word phakos 'lens'.
Intraocular lenses for correcting refractive errors
Intraocular lenses have been used since 1999 for correcting larger errors in myopic (near-sighted), hyperopic (far-sighted), and astigmatic eyes. This type of IOL is also called PIOL (phakic intraocular lens), and the crystalline lens is not removed.
More commonly, aphakic IOL's (that is, not PIOL's) are implanted via Clear Lens Extraction and Replacement (CLEAR) surgery. During CLEAR, the crystalline lens is extracted and an IOL replaces it in a process that is very similar to cataract surgery: both involve lens replacement, local anesthesia, both last approximately 30 minutes, and both require making a small incision in the eye for lens insertion. People recover from CLEAR surgery 1-7 days after the operation. During this time, they should avoid strenuous exercise or anything else that significantly raises blood pressure. They should also visit their ophthalmologists regularly for several months so as to monitor the IOL implants. CLEAR has a 90% success rate (risks include wound leakage, infection, inflammation, and astigmatism). CLEAR can only be performed on patients ages 40 and older. This is to ensure that eye growth, which disrupts IOL lenses, will not occur post-surgery.
Once implanted, IOL lenses have three major benefits. First, they are an alternative to LASIK, a form of eye surgery that does not work for people with serious vision problems. Effective IOL implants also entirely eliminate the need for glasses or contact lenses post-surgery. Cataract will not return, as the lens has been removed. The disadvantage is that the eye's ability to change focus (accommodate) has generally been reduced or eliminated, depending on the kind of lens implanted.
Most PIOLs have not yet been approved by FDA, but many are under investigation, and some of the risks that FDA have been found so far during a three year study of the Artisan lens, produced by Ophtec USA Inc, are:[1]
- a yearly loss of 1.8% of the endothelial cells,
- 0.6% risk of retinal detachment,
- 0.6% risk of cataract (other studies have shown a risk of 0.5 - 1.0%), and
- 0.4% risk of corneal swelling.
Other risks include:
- 0.03 - 0.05% eye infection risk, which in worst case can lead to blindness. This risk exists in all eye surgery procedures, and is not unique for IOLs.
- glaucoma,
- astigmatism,
- remaining near or far sightedness,
- rotation of the lens inside the eye within one or two days after surgery.
One of the causes of the risks above is that the lens can rotate inside the eye, because the PIOL is too short, or because the sulcus has a slightly oval shape (the height is slightly smaller than the width).
Phakic IOLs
Special types of Phakic IOLs (PIOLs) are available in patients requiring IOL implantation without removal of crysalline human lens, particularly useful in refractive surgery for high myopia. For this, the eye surgeon has to determine the size of the PIOL. If the lens is of incorrect length, then it can rotate inside the eye, causing astigmatism, and/or damage to the natural lens. It can also block the natural flow of fluid inside the eye, causing glaucoma. The size is usually estimated, by measuring white-to-white, and estimating the ciliary sulcus diameter. However, the surgeon can perform 3D ultrasound biomicroscopy with for example Artemis for a completely accurate measurement. 3D ultrasound is to traditional 2D ultrasound as computer assisted tomography is to x-ray. Therefore, 3D ultrasound examination is strongly recommended, since the white-to-white guesstimate does not have a strong correlation with sulcus-to-sulcus - neither for myopic, nor for hyperopic. About 1% of sulcus-to-sulcus estimates based on white-to-white are so wrong that serious complications can arise. This type of phakic lens has to be ordered from the manufacturer, requiring a number of weeks before the surgery. However, on the other hand, the routine posterior chamber IOLs (PC-IOLs) used for routine cataract surgical cases are available with the surgical suite or doctor's office, and the cataract surgery can usually be performed without delay once the patient is cleared for surgery.
Types of PIOLs
Phakic IOLS (PIOLs) can be either spheric or toric - the latter is used for astigmatic eyes. The difference is that toric PIOLs have to be inserted in a specific angle, or the astigmatism will not be fully corrected, or it can even get worse.
According to placement site in the eyes phakic IOLs can be divided to:
- Angle supported PIOLs: those IOLs are placed in the anterior chamber. They are notorious for their negative impact on the corneal endothelial lining, which is vital for maintaining a healthy dry cornea.
- Iris supported PIOLs: this type is gaining more and more popularity. The IOL is attached by claws to the mid peripheral iris by a technique called enclavation. It is believed to have a lesser effect on corneal endothelium.
- Sulcus supported PIOLs: these IOLS are placed in the posterior chamber in front of the natural crystalline lens. They have special vaulting so as not to be in contact with the normal lens. The main complications with this type is their tendency to cause cataracts and/or pigment dispersion.
Intraocular contact lenses
Very different from contact lenses that are placed on the surface of the eye, an intraocular contact lens, also known as an implantable contact lens, is a small corrective lens that is surgically placed in the eye's posterior chamber behind the iris and in front of the lens to correct higher amounts of myopia and hyperopia.
IOL manufacturers and materials
There are many different manufacturers of intraocular lenses.
Acrylic:
- Hoya manufacturers high quality hydrophobic acrylic IOLS, distributed by Spectrum
- ERILENS produces hydrophilic acrylic lenses
- Medennium produces the Matrix Acrylic™ IOL, distributed by Medennium.
- Ophtec produces the Artisan® lens, distributed by Spectrum
- OII Intraocular Lenses produces hydrophilic acrylic IOLs.
- Corneal produces the I-Care®, hydrophobic acrylic IOL.
Silicone:
- AMO (Advanced Medical Optics) produces the Verisyse™ PIOL and the ReZoom™ multi-focal IOL.
- Tekia Inc. produces the Kelman Duet lens.
- The Vision Membrane phakic IOL is produced by Vision Membrane Technologies Inc., Apollo Optical Systems LLC, and Millennium Biomedical Inc.
- The PRL™ Phakic Refractive Lens is produced by Medennium, distributed by IOLTech.
Other:
- Staar produces the Visian ICL™ lens, in a material called Collamer®.
- Alcon produces the multi-focal AcrySof® ReSTOR® and the AcrySof® Toric IOLs.
- Eyeonics produces the Accommodating CrystalensIOL.
More information about IOLs
- US FDA Phakic Intraocular Lenses
- Transcript of ophthalmic devices advisory panel, 106th meeting
- Phakic intraocular lenses
- Phakic Intraocular Lenses - The New Focus in Refractive Surgery.
See also
Notes
- ↑ Staff (September 13, 2004). "FDA Approves Implanted Lens to Correct Nearsightedness (T03-38)". FDA Talk Paper. Food and Drug Administration. Retrieved May 21. Unknown parameter
|accessyear=ignored (|access-date=suggested) (help); Check date values in:|accessdate=(help)
References
- Shearing, Steven, MD. "History of the PMMA Intraocular Lens". Ophthalmic Hyperguide. Vindico Medical Education and Allergan. Note: requires login to reach article content
External links
- Keith P. Thompson (inventor). "Near Vision Accommodating Intraocular Lens with Adjustable Power" (PDF). U.S. patent No. 5,607,472. Retrieved 2007-02-04.
- Read a patient testimonial at danielmckinnon.com.