Cauda equina syndrome
| Cauda equina syndrome | ||
 | ||
|---|---|---|
| Cauda equina and filum terminale seen from behind. | ||
| ICD-10 | G83.4 | |
| ICD-9 | 344.6 | |
| DiseasesDB | 31115 | |
| MeSH | C10.668.829.800.750.700 | |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Joanna Ekabua, M.D. [2]
Overview
The cauda equina is a collection of nerves at the end of the spinal cord. These nerves consist of the spinal nerves L2-L5, S1-S5 and the coccygeal nerve. Cauda equina syndrome first described by Hutchinson in 1889 is due to compression of the cauda equina in the lumbosacral region of the spinal canal. It is an emergency medical condition requiring acute intervention in the form of acute decompression surgery to prevent permanent neurological damage to the urinary bladder, Intestine, sex organs and lower limbs. The most common cause of cauda equina syndrome is lumbar disc herniation. It can be classified into two major groups, cauda equina syndrome complete with urinary retention and cauda equina syndrome incomplete. Prognosis of cauda equina syndrome depends on time from onset of symptoms to decompression and the degree of nerve damage at the time of surgery.
Historical perspective
- Cauda equina was named by the French anatomist Andreas Lazarius (André du Laurens) in the 17th century after its resemblance to a horse's tail (Latin: cauda equina).
- Cauda equina syndrome was first discovered by Jonathan Hutchinson, a British dermatologist and surgeon in 1889, following a hemorrhoidectomy in a 42-year-old man in which general anesthesia of ether and a crushing clamp was used. Postop, the patient had painless urinary retention and constipation. During catheterization, he felt no pain, by postop day 3, he was fecal incontinent without knowledge. The patient was seen by Hutchinson 6 months later, where examination showed the anus to be patulous and acontractile. An enema or manual evacuation had to be used to empty bowel. The patient was unaware of the passage of feces. When patient self-catheterized three times a day, he had no sensation on catheter passage. He, however, could empty his bladder by straining. The patient had partial anesthesia around the anus and buttocks. He had no problems with his bladder or bowels before the operation, but he did have a past medical history of alternating sciatica bilaterally which was not very common. During the sciatica attacks, he felt numb on the buttocks. There is no record of the state of the muscles of his lower limbs. Hutchinson diagnosed a form of ascending neuritis induced by crushing of his pile. He was unhappy with these findings since there was no interval between the operation and the development of the urinary retention. Hutchinson could not establish a diagnosis. Evidence is presented to suggest that this was the first case of disc prolapsed, causing a cauda equina syndrome because of anesthesia and manipulation.[1]
- In 1977/1978, MRI was developed by Raymond Damadian to diagnose cancer. It has since been used to diagnose other pathologies and is the gold standard for the diagnosis of cauda equina syndrome.[2][3][4]
Classification
Cauda equina syndrome may be classified into complete and incomplete.[5][3]
- Cauda equina syndrome complete with urinary retention
- Cauda equina syndrome incomplete
| Cauda equina syndrome | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Complete with urinary retention | Incomplete | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Lumbar +/- leg pain, sensory and motor deficency in lower extremities, painless urine retention with overflow incontinence, total perianal sensory loss, and fecal incontinece. | Lumbar +/- leg pain, sensory and motor deficency in lower extremities, loss of micturition reflex, altered urinary sensation and hesitancy, partial saddle anesthesia, and decreased anal sphinter tone. | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Pathophysiology
- It is thought that cauda equina syndrome is the result of direct mechanical compression of the lumbar and sacral nerves roots arising below the conus medullaris and venous congestion or ischemia.[3][6]
- Mechanical compression can be due to space-occupying lesion such as
- Spinal disc herniation
- Infections/abscess
- Hematoma
- Fractured vertebrae
- Metastasis
- Lumbosacral and pelvic hydatid cyst within lumbosacral region of the spinal canal
- The proximal region of the cauda equina is relatively hypovascular leading to neuroischemic symptoms with compression. [6][7]
Causes
Cauda equina syndrome may be caused by[2]
- Lumbar disc herniation[2]
- Conus medullaris infarction[8]
- Complication of lumbar spinal surgery[9]
- Lumbar spinal stenosis[9]
- Vertebrae fracture/trauma[10][11]
- Spinal lesions or tumor[12]
- Epidural venous plexus engorgement/thrombosis[13][4][14]
- Primary lumbosacral and pelvic hydatid cyst[15]
- Infections/abscess[4][16]
Differentiating cauda equina syndrome from other Diseases
- Cauda equina syndrome must be differentiated from spinal disc herniation, epidural hematoma, spinal tumor/metastasis, spinal stenosis, and diabetic amyotrophy.[17][4][18][19]
Epidemiology and Demographics
- The incidence of cauda equina syndrome is 2 in 100,000/year.[5][4]
- Patients of all age groups may develop cauda equina syndrome.
- Cauda equina syndrome usually affects individuals of all races, although African American individuals are less likely to develop cauda equina syndrome.[20][21][22]
- Cauda equina syndrome affects men and women equally.
Risk Factors
- The most potent risk factor in the development of cauda equina syndrome is spinal disc herniation.[23]
- Other risk factors include trauma, a spinal tumor, severe infection, spinal stenosis, spinal anesthesia,[24] obesity[25] and female sex.[26]
Screening
- There is insufficient evidence to recommend routine screening for cauda equina syndrome.
Natural History, Complications, and Prognosis
- If left untreated, 100% progress to permanent nerve damage and neurological deficit.
- Common complications of cauda equina syndrome include[4][27]
- Micturition dysfunction 48%
- Defecation dysfunction 42%,
- Sexual dysfunction 53%
- Sciatica 48%
- Altered sensation of the saddle area 57%.
- Prognosis of cauda equina syndrome depends on a number of factors, example time from onset of symptoms to decompression, the degree of nerve damage at the time of surgery and the type of cauda equina syndrome; with incomplete being more favourable.[28] Following surgery, the extent of recovery is variable.[4] Long term outcomes postsurgery are bladder, sexual, and motor dysfunction especially in patients with cauda equina syndrome complete with urinary retention.[29]
Diagnosis
Diagnostic Study of Choice
- There are no established criteria for the diagnosis of cauda equina syndrome. However, in the presence of Lower back pain, urinary retention, decreased muscle strength, and saddle anesthesia, MRI should be ordered to rule out cauda equina syndrome.
| Radiological imaging | Sensitivity | specificity | PPV | NPV |
|---|---|---|---|---|
| CT[30] | 98% | 86% | 72% | 99% |
| MRI[31] | 68% | 78% | 84% | 58% |
- Although CT is shown to be more sensitive and specific for the diagnosis of cauda equina syndrome, MRI is considered the goal standard because it can depict soft tissue clearer.[2][3][4]
History and Symptoms
The most common symptoms of cauda equina syndrome include
- Intermittent Lower back pain radiating to the lower extremities. [3][2][9][11][26]
- Decreased muscle strength bilaterally.[2][3][11][9]
- Fecal incontinence/retention[2][3][8][9][26][11]
- Urinary incontinence/ retention[5][2][3][9][26][11]
- Unilateral or bilateral sciatica[3][9][26][11]
- Saddle anesthesia[3][9][26]
- Paraparesis[8]
- Sexual dysfunction[8][26]
Physical Examination
Common physical examination findings of cauda equina syndrome include
- Hypesthesia[2][8]
- Saddle dysesthesia[8]
- Lasegue sign[2]
- Decreased knee and ankle reflex bilaterally. [2][8]
- Asymmetric calf wasting[8]
- Lower limb weakness[8]
- Positive Babinski sign[8]
- Impaired proprioception[8]
Laboratory findinds
- There are no diagnostic laboratory findings associated with cauda equina syndrome.
Echocardiography
- There are no ECG findings associated with cauda equina syndrome.
X-ray
- There are no x-ray findings associated with cauda equina syndrome.
Ultrasound
- There are no ultrasound findings associated with cauda equina syndrome.
CT Scan
- Lumbosacral CT scan may be helpful in the diagnosis of cauda equina syndrome.
- CT scan sensitivity for cauda equina syndrome has been estimated to be 98%; specificity, 86%; positive predictive value, 72%; and negative predictive value, 99%.[30]
- Findings on CT scan suggestive of/diagnostic of cauda equina syndrome include
- This CT scan shows compression of the spinal cord due to a fractured Vertebra.
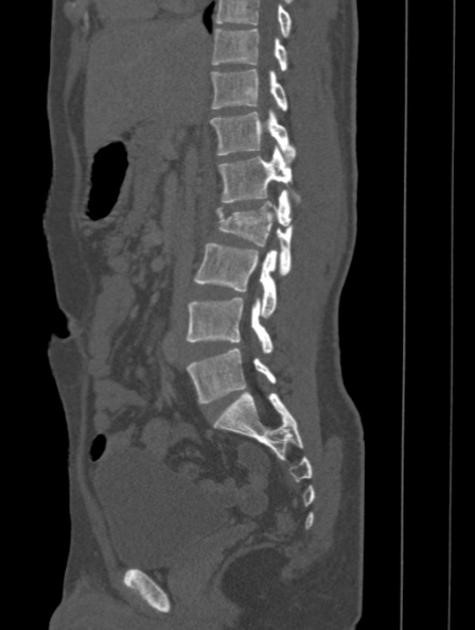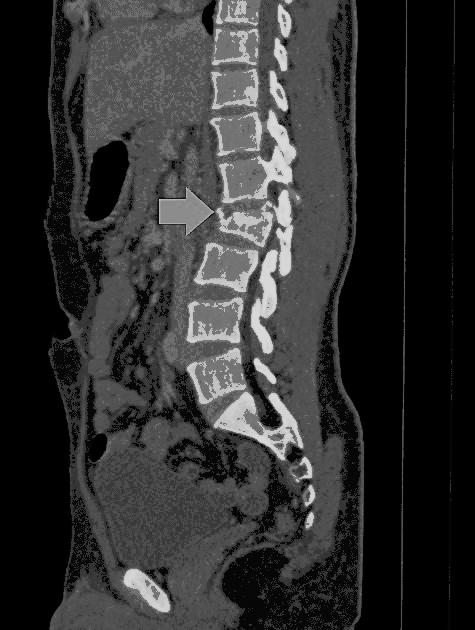
MRI
- Lumbosacral MRI is the gold standard in the diagnosis of cauda equina syndrome.[2][3][4]
- MRI sensitivity for cauda equina syndrome has been estimated to be 68%, specificity 78%, positive predictive value 84% and negative predictive value 58%.[32]
- Findings on MRI suggestive of cauda equina syndrome include
- In Lumbar disc herniation, MRI shows a disc mass filling most of the spinal canal compressing the cauda equina.
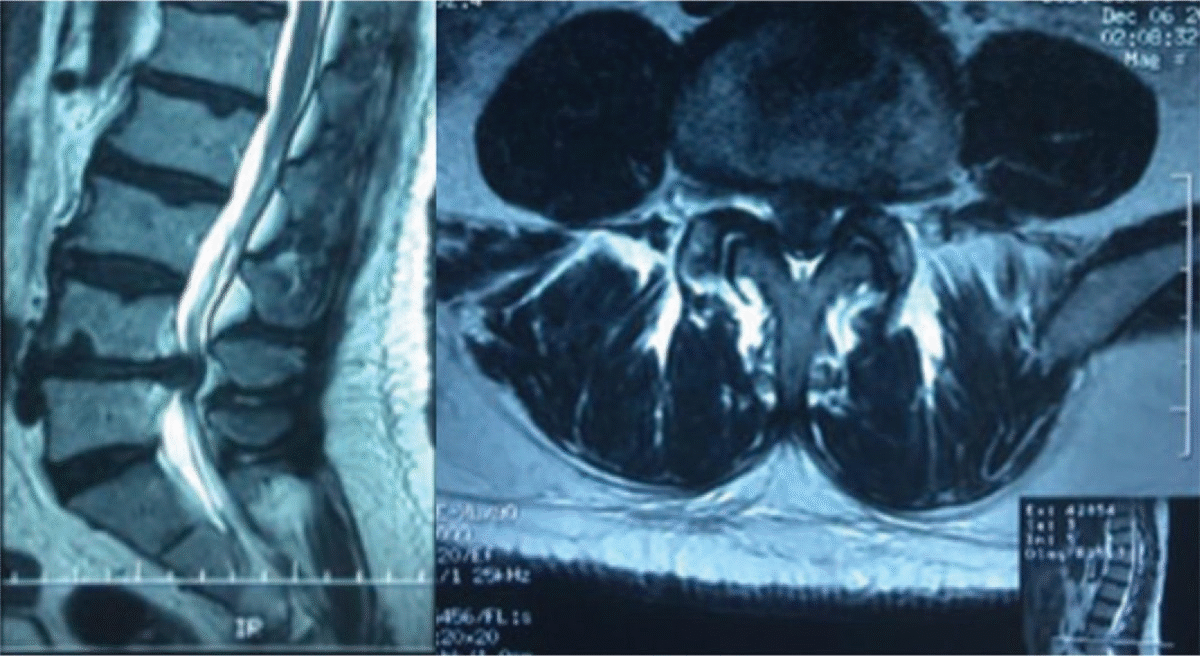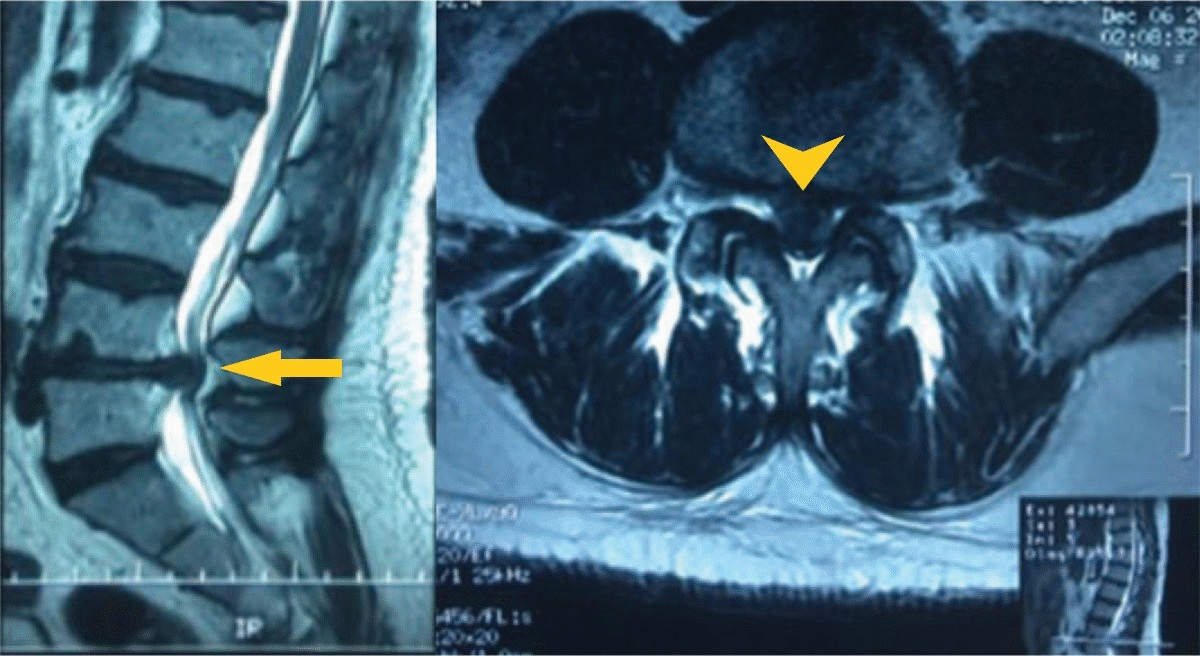
- In Pott's disease, MRI shows spinal cord compression by destroyed bone.
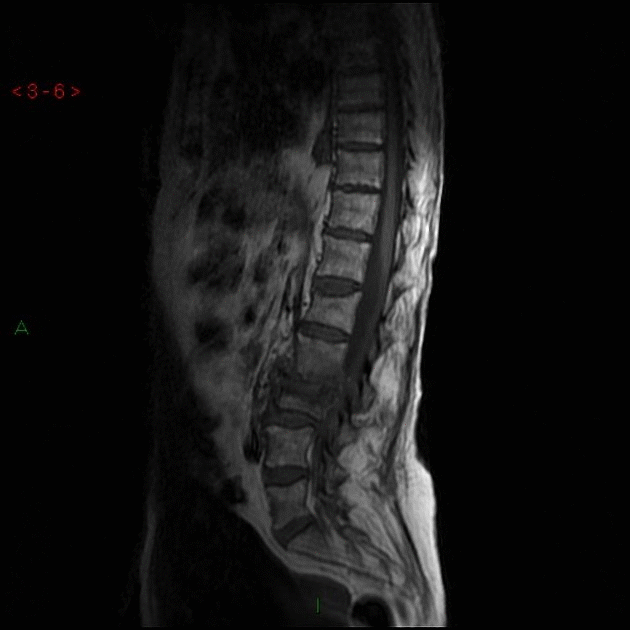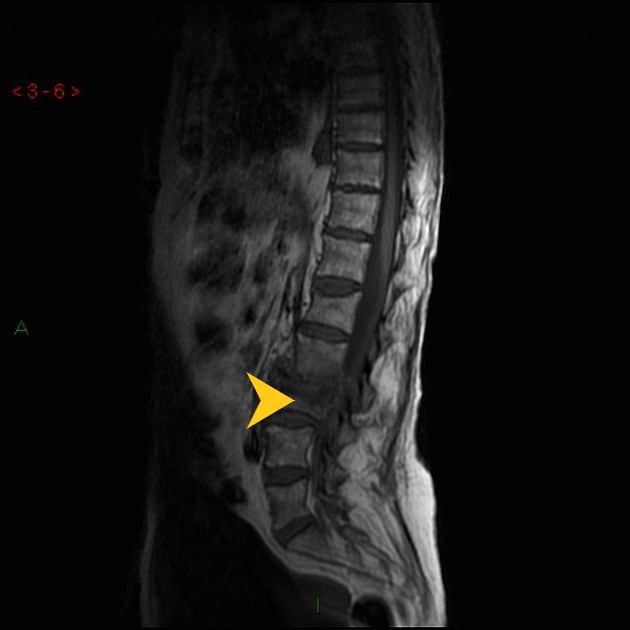
Other Imaging Findings
- There are no other imaging findings associated with cauda equina syndrome.
Other Diagnostic Findings
- Myelogram which demonstrates spinal cord compression due to Spinal disc herniation
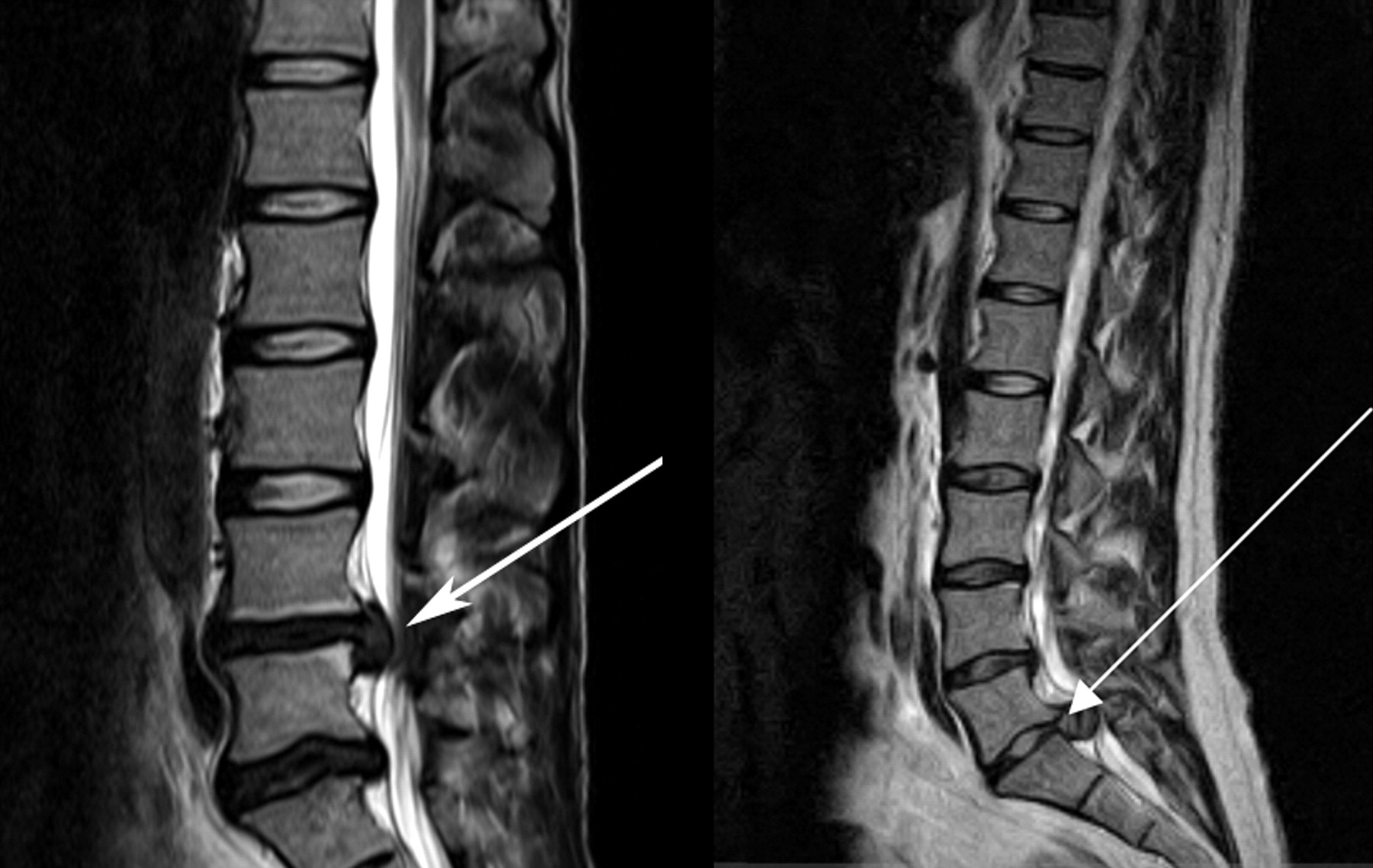
- Electromyography
- Pre and post-void bladder scan; if the post-void residual volume is >200ml, the probability of cauda equina syndrome is 43% (P < 0.000003) making bladder scan an adjunct in the diagnosis of cauda equina syndrome.[33]
Treatment
Medical Treatment
Cauda equina syndrome is a medical emergency and requires prompt treatment. Although the mainstay of treatment is surgery, The following medications are used.[9]
- 5.4 mg/kg·h of methylprednisolone (intravenous) for 2 days
- 5 mg of dexamethasone (intravenous) every 12 h for 3 days
- 0.5 mg of mecobalamin tablets (oral) every 8 h
- Chemotherapy for cases due to tumors
- Antibiotics for cases due to infection
Surgery
- Surgery is the mainstay of treatment for cauda equina syndrome.[3][2] Immediate surgical decompression is the best intervention associated with positive patient outcome.[34] Procedures used include
- Laminectomy and discectomy (most common)
- Hemilaminectomy
- Transforaminal lumbar interbody infusion
- Microdiscectomy
- positive outcomes in bladder and bowel functions, sensory and motor deficit are seen if decompresssion is performed within 48hours of symptoms.
Primary Prevention
- There are no established measures for the primary prevention of cauda equina syndrome.
Secondary Prevention
- There are no established measures for the secondary prevention of cauda equina syndrome.
References
- ↑ Silver JR (2001). "The earliest case of cauda equina syndrome caused by manipulation of the lumbar spine under a general anaesthetic". Spinal Cord. 39 (1): 51–3. doi:10.1038/sj.sc.3101102. PMID 11224016.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 Luo D, Ji C, Xu H, Feng H, Zhang H, Li K (2020). "Intradural disc herniation at L4/5 level causing Cauda equina syndrome: A case report". Medicine (Baltimore). 99 (7): e19025. doi:10.1097/MD.0000000000019025. PMC 7035013 Check
|pmc=value (help). PMID 32049799 Check|pmid=value (help). - ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 Srikandarajah N, Wilby M, Clark S, Noble A, Williamson P, Marson T (2018). "Outcomes Reported After Surgery for Cauda Equina Syndrome: A Systematic Literature Review". Spine (Phila Pa 1976). 43 (17): E1005–E1013. doi:10.1097/BRS.0000000000002605. PMC 6104724. PMID 29432394.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 4.8 "StatPearls". 2020. PMID 30725885.
- ↑ 5.0 5.1 5.2 Srikandarajah N, Noble A, Clark S, Wilby M, Freeman BJC, Fehlings MG; et al. (2020). "Cauda Equina Syndrome Core Outcome Set (CESCOS): An international patient and healthcare professional consensus for research studies". PLoS One. 15 (1): e0225907. doi:10.1371/journal.pone.0225907. PMC 6953762 Check
|pmc=value (help). PMID 31923259. - ↑ 6.0 6.1 Spector LR, Madigan L, Rhyne A, Darden B, Kim D (2008). "Cauda equina syndrome". J Am Acad Orthop Surg. 16 (8): 471–9. doi:10.5435/00124635-200808000-00006. PMID 18664636.
- ↑ Parke WW, Gammell K, Rothman RH (1981). "Arterial vascularization of the cauda equina". J Bone Joint Surg Am. 63 (1): 53–62. PMID 7005240.
- ↑ 8.00 8.01 8.02 8.03 8.04 8.05 8.06 8.07 8.08 8.09 8.10 Weng YC, Chin SC, Wu YY, Kuo HC (2019). "Clinical, neuroimaging, and nerve conduction characteristics of spontaneous Conus Medullaris infarction". BMC Neurol. 19 (1): 328. doi:10.1186/s12883-019-1566-1. PMC 6916224 Check
|pmc=value (help). PMID 31847829. - ↑ 9.0 9.1 9.2 9.3 9.4 9.5 9.6 9.7 9.8 Yuan T, Zhang J, Yang L, Wu J, Tian H, Wan T; et al. (2019). "Cauda equina syndrome without motor dysfunction following lumbar spinal stenosis surgery: A case report". Medicine (Baltimore). 98 (29): e16396. doi:10.1097/MD.0000000000016396. PMC 6709168 Check
|pmc=value (help). PMID 31335689. - ↑ Li P, Qiu D, Shi H, Song W, Wang C, Qiu Z; et al. (2019). "Isolated Decompression for Transverse Sacral Fractures with Cauda Equina Syndrome". Med Sci Monit. 25: 3583–3590. doi:10.12659/MSM.916483. PMC 6532556 Check
|pmc=value (help). PMID 31089068. - ↑ 11.0 11.1 11.2 11.3 11.4 11.5 Harrop JS, Hunt GE, Vaccaro AR (2004). "Conus medullaris and cauda equina syndrome as a result of traumatic injuries: management principles". Neurosurg Focus. 16 (6): e4. doi:10.3171/foc.2004.16.6.4. PMID 15202874.
- ↑ Wu HY, Xu WB, Lu LW, Li HH, Tian JS, Li JM; et al. (2018). "Imaging features of spinal atypical teratoid rhabdoid tumors in children". Medicine (Baltimore). 97 (52): e13808. doi:10.1097/MD.0000000000013808. PMC 6314652. PMID 30593171.
- ↑ Tello Díaz C, Allegue Allegue N, Gil Sala D, Gonçalves Martins G, Boqué Torremorell M, Bellmunt Montoya S (2019). "Cauda Equina Syndrome Caused by Epidural Venous Plexus Engorgement in a Patient with May-Thurner Syndrome". Ann Vasc Surg. 60: 480.e7–480.e11. doi:10.1016/j.avsg.2019.04.002. PMID 31200048.
- ↑ Lavy C, James A, Wilson-MacDonald J, Fairbank J (2009). "Cauda equina syndrome". BMJ. 338: b936. doi:10.1136/bmj.b936. PMID 19336488.
- ↑ Adilay U, Tuğcu B, Gunes M, Günaldi O, Gunal M, Eseoglu M (2007). "Cauda equina syndrome caused by primary lumbosacral and pelvic hydatid cyst: a case report". Minim Invasive Neurosurg. 50 (5): 292–5. doi:10.1055/s-2007-973822. PMID 18058646.
- ↑ Cohen DB (2004). "Infectious origins of cauda equina syndrome". Neurosurg Focus. 16 (6): e2. doi:10.3171/foc.2004.16.6.2. PMID 15202872.
- ↑ Panos G, Watson DC, Karydis I, Velissaris D, Andreou M, Karamouzos V; et al. (2016). "Differential diagnosis and treatment of acute cauda equina syndrome in the human immunodeficiency virus positive patient: a case report and review of the literature". J Med Case Rep. 10: 165. doi:10.1186/s13256-016-0902-y. PMC 4895963. PMID 27268102.
- ↑ Jiménez-Ávila JM, Castañeda-Huerta JE, González-Cisneros AC (2019). "[Bruns Garland syndrome. Report of a case and differential diagnosis with cauda equina syndrome]". Acta Ortop Mex. 33 (1): 42–45. PMID 31480126.
- ↑ Zhou ZN, Canon C, Matrai C, Chapman-Davis E (2018). "Cauda equina syndrome secondary to leptomeningeal metastases from recurrent primary peritoneal carcinoma". Ecancermedicalscience. 12: 814. doi:10.3332/ecancer.2018.814. PMC 5834310. PMID 29515655.
- ↑ Schoenfeld AJ, Bader JO (2012). "Cauda equina syndrome: an analysis of incidence rates and risk factors among a closed North American military population". Clin Neurol Neurosurg. 114 (7): 947–50. doi:10.1016/j.clineuro.2012.02.012. PMID 22402198.
- ↑ Radcliff KE, Kepler CK, Delasotta LA, Rihn JA, Harrop JS, Hilibrand AS; et al. (2011). "Current management review of thoracolumbar cord syndromes". Spine J. 11 (9): 884–92. doi:10.1016/j.spinee.2011.07.022. PMID 21889419.
- ↑ Small SA, Perron AD, Brady WJ (2005). "Orthopedic pitfalls: cauda equina syndrome". Am J Emerg Med. 23 (2): 159–63. doi:10.1016/j.ajem.2004.03.006. PMID 15765336.
- ↑ Kapetanakis S, Chaniotakis C, Kazakos C, Papathanasiou JV (2017). "Cauda Equina Syndrome Due to Lumbar Disc Herniation: a Review of Literature". Folia Med (Plovdiv). 59 (4): 377–386. doi:10.1515/folmed-2017-0038. PMID 29341941.
- ↑ Yorozu T, Matsumoto M, Hayashi S, Yamada T, Nakaohji T, Nakatsuka I (2002). "[Dibucaine for spinal anesthesia is a probable risk for cauda equina syndrome]". Masui. 51 (10): 1151–4. PMID 12428328.
- ↑ Cushnie D, Urquhart JC, Gurr KR, Siddiqi F, Bailey CS (2018). "Obesity and spinal epidural lipomatosis in cauda equina syndrome". Spine J. 18 (3): 407–413. doi:10.1016/j.spinee.2017.07.177. PMID 28756300.
- ↑ 26.0 26.1 26.2 26.3 26.4 26.5 26.6 Long B, Koyfman A, Gottlieb M (2020). "Evaluation and management of cauda equina syndrome in the emergency department". Am J Emerg Med. 38 (1): 143–148. doi:10.1016/j.ajem.2019.158402. PMID 31471075.
- ↑ Korse NS, Pijpers JA, van Zwet E, Elzevier HW, Vleggeert-Lankamp CLA (2017). "Cauda Equina Syndrome: presentation, outcome, and predictors with focus on micturition, defecation, and sexual dysfunction". Eur Spine J. 26 (3): 894–904. doi:10.1007/s00586-017-4943-8. PMID 28102451.
- ↑ Gardner A, Gardner E, Morley T (2011). "Cauda equina syndrome: a review of the current clinical and medico-legal position". Eur Spine J. 20 (5): 690–7. doi:10.1007/s00586-010-1668-3. PMC 3082683. PMID 21193933.
- ↑ Hazelwood JE, Hoeritzauer I, Pronin S, Demetriades AK (2019). "An assessment of patient-reported long-term outcomes following surgery for cauda equina syndrome". Acta Neurochir (Wien). 161 (9): 1887–1894. doi:10.1007/s00701-019-03973-7. PMC 6704093 Check
|pmc=value (help). PMID 31263950. - ↑ 30.0 30.1 Peacock, J.G.; Timpone, V.M. (2017). "Doing More with Less: Diagnostic Accuracy of CT in Suspected Cauda Equina Syndrome". American Journal of Neuroradiology. 38 (2): 391–397. doi:10.3174/ajnr.A4974. ISSN 0195-6108.
- ↑ . doi:10.1302/0301-620X. Missing or empty
|title=(help) - ↑ . doi:10.1302/0301-620X. Missing or empty
|title=(help) - ↑ Venkatesan M, Nasto L, Tsegaye M, Grevitt M (2019). "Bladder Scans and Postvoid Residual Volume Measurement Improve Diagnostic Accuracy of Cauda Equina Syndrome". Spine (Phila Pa 1976). 44 (18): 1303–1308. doi:10.1097/BRS.0000000000003152. PMID 31479434.
- ↑ Hogan WB, Kuris EO, Durand WM, Eltorai AEM, Daniels AH (2019). "Timing of Surgical Decompression for Cauda Equina Syndrome". World Neurosurg. 132: e732–e738. doi:10.1016/j.wneu.2019.08.030. PMID 31415897.
Template:Neuroscience-stub Template:Cerebral palsy and other paralytic syndromes [{Category:Needs patient information]] de:Cauda-equina-Syndrom