Automated external defibrillator

Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
An Automated External Defibrillator or AED is a portable electronic device that automatically diagnoses the potentially life threatening cardiac arrhythmias of ventricular fibrillation and ventricular tachycardia in a patient,[1] and is able to treat them by application of electrical therapy which stops the arrhythmia, allowing the heart to re-establish an effective rhythm.
AEDs are designed to be simple to use for the layman, and the use of AEDs is taught in many first aid, first responder and basic life support (BLS) level CPR classes.[2]
Usage
An automated external defibrillator is used in cases of life threatening cardiac arrhythmias, which may lead, or have led to cardiac arrest. The rhythms the device will treat is usually limited to:
- Ventricular fibrillation (shortened to VF or V-Fib)
- Pulseless Ventricular tachycardia (shortened to VT or V-Tach)[1]
AEDs (and all other defibrillators) are not designed to shock asystole or 'flat line' patterns, as this will not have a positive clinical outcome. The asystolic patient only has a chance of survival if, through a combination of CPR and cardiac stimulant drugs, one of the shockable rhythms can be established, which makes it imperative for CPR to be carried out by any lay rescuer prior to the arrival of a defibrillator.
In each of the two types of shockable cardiac arrhythmia, the heart is in activity (possibly even beating), yet in an unusual pattern, which can be life-threatening if left uncorrected. In ventricular fibrillation, the electrical activity of the heart becomes chaotic, preventing the ventricle from effectively pumping blood. In ventricular tachycardia, the heart beats too fast to effectively pump blood. Frequently, ventricular tachycardia leads to ventricular fibrillation. The fibrillation in the heart decreases over time, and will eventually reach Asystole, with an absence of any rhythm.
Uncorrected, these cardiac conditions rapidly lead to irreversible brain damage and death. After approximately three minutes, irreversible brain/tissue damage occurs. For every minute that a person in cardiac arrest goes without being successfully treated (by defibrillation), the chance of survival decreases by 10 percent.
AED's are designed to be used by laypersons, who ideally should have received specialist training. They are usually limited in their interventions to delivering high joule shocks for VF and VT. This is in contrast to more sophisticated manual and semi-automatic defibrillators used by health professionals, which can act as a pacemaker if the heart rate is too slow (bradycardia) and perform other functions which require a skilled operator, able to read electrocardiograms.
Placement
Automated external defibrillators are generally either held by trained personnel who will attend incidents, or are public access units which can be found in places including corporate and government offices, shopping centers, airports, restaurants, casinos, hotels, sports stadiums, schools and universities, community centers, fitness centers and health clubs.
The locating of a public access AED should take in to account where large groups of people gather, and the risk category associated with these people, to ascertain whether the risk of a sudden cardiac arrest incident is high. For example, a centre for teenage children is a particularly low risk category (as children very rarely enter heart rhythms such as VF or VT, being generally young and fit, and the most common cause of paediatric cardiac arrest is trauma - where an AED is no use), whereas a large office building with a high ratio of males over 50 is a very high risk environment.
In many areas, emergency services vehicles are likely to carry AEDs, with some Ambulances carrying an AED in addition to a manual unit. In addition, some police or fire service vehicles carry an AED for first responder use. Some areas have dedicated community first responders, who are volunteers tasking with keeping an AED and taking it to any victims in their area. It is also increasingly common to find AEDs on transport such as commercial airlines and cruise ships.
In order to make them highly visible, public access AEDs often are brightly coloured, and are mounted in protective cases near the entrance of a building. When these protective cases are opened, and the defibrillator removed, some will sound a buzzer to alert nearby staff to their removal but do not necessarily summon emergency services. All trained AED operators should also know to phone for an Ambulance when sending for or using an AED, as the patient will be unconscious, which always requires ambulance attendance.


A trend now being seen is the purchase of AEDs to be kept and used in the home, particularly by those with known existing heart conditions.[3] The number of devices in the community has grown as prices have fallen to affordable levels (in line with a large television). There has been some concern amongst medical professionals that these home users do not necessarily have appropriate training,[4] and many advocate the more widespread use of community responders, who can be appropriately trained and managed.
Typically, an AED kit will contain a face shield, for providing a barrier between patient and first aider during rescue breathing; a pair of Nitrile rubber non-allergenic gloves; a pair of Tuff cuts scissors, for cutting through a patient's clothing to expose the chest; a small towel for wiping away any moisture on the chest and a razor for shaving those with very hairy chests.
Preparation for operation
Most manufacturers recommend checking the AED before every 'duty' or on a regular basis if a fixed unit. Some units need to be switched on in order to perform its self check. Other models, such as the one pictured, have a self check system built in, with a visible indicator.
All manufacturers mark their pads with an expiry date, and it is important to ensure that the pads are in date. This is usually marked on the outside of the pads. Some models are designed to make this date visible through a 'window', although others will require the opening of the case to find the date stamp.

Mechanism of operation
An AED is called external because the operator applies the electrode pads to the bare chest of the victim, as opposed to internal defibrillators, which have electrodes surgically implanted inside the body of a patient.
The 'Automatic' part of the title refers to the unit's ability to autonomously analyse the patient's condition, and to assist this, the vast majority of units have spoken prompts, and some may also have visual displays to instruct the user.
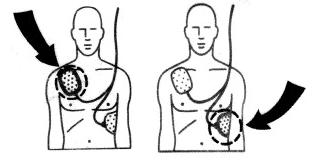
When turned on, or opened, the AED will instruct the user to connect the electrodes (pads) to the patient. Once the pads are attached to the patient, everyone should avoid touching the victim so as to avoid false readings by the unit. The pads allow the AED to examine the electrical output from the heart and determines if the patient is in a viable, shockable rhythm (either ventricular fibrillation or ventricular tachycardia). If the device determines that a shock is viable, it will use the battery to charge its internal capacitor in preparation to deliver the shock. This system is not only safer (charging only when required), but also allows for a faster delivery of the electrical current.
When charged, the device instructs the user to ensure no one is touching the victim and then to press a button to deliver the shock. Human intervention is usually required to deliver the shock to the patient, to avoid the possibility of accidents. After the shock is delivered, the device will either instruct the user to commence CPR, or will continue to monitor the heart rhythm of the patient to determine if another shock is necessary.
Many AED units have an 'event memory', which store the ECG of the patient along with details of the time the unit was activated and the number and strength of any shocks delivered. Some units also have voice recording facilities, to monitor the actions taken by the personnel, to ascertain if these had any impact on the survival outcome. All this memorised data can be either downloaded to a computer, or printed out, so that the providing organisation, or responsible body (such as a coroner) can see the effectiveness of both CPR and defibrillation on the patients heart.
AEDs available to the public may be semi-automatic or fully automatic. Fully automatic units are likely to have few buttons, often activating as soon as the case is opened, and possibly just one button to shock, or in some cases, this will be performed automatically. The user has no input in to the operation of the unit, apart from attaching the pads, and following the prompts. Health care professionals, and other trained persons, may use a Semi-Automatic defibrillator, which is likely to have an ECG readout display, and the possibility to override the rhythm analysis software. This allows trained personnel to give a higher standard of care, shocking at specific times in the cycle.
The first commercially available AEDS were all of a monophasic type, which gave a high-energy shock, up to 360 to 400 joules depending on the model. This caused increased cardiac injury and in some cases second- and third-degree burns around the shock pad sites. Newer AEDs (manufactured after late 2003) have tended to utilise biphasic algorithms which give two sequential lower-energy shocks of 120 - 200 joules, with each shock moving in an opposite polarity between the pads. This lower-energy waveform has proven more effective in clinical tests, as well as offering a reduced rate of complications and reduced recovery time.
Simplicity of use
Unlike regular defibrillators, an automated external defibrillator requires very little training to use. It automatically diagnoses the heart rhythm and determines if a shock is needed. Automatic models will administer the shock without the user's command. Semi-automatic models will tell the user that a shock is needed, but the user must tell the machine to do so, usually by pressing a button. In most circumstances, the user cannot override a "no shock" advisory by an AED. Some AEDs can even be used on children (those under 55 lbs [25 kg] in weight, or under age 8). If a particular model of AED is approved for pediatric use, all that is required is the use of more appropriate pads. Some organizations, such as the American Heart Association, recommend that if pediatric AED pads are not available, adult pads should be used to determine if the child is in a shockable rhythm. There is insufficient evidence to suggest that a child, in a shockable cardiac arrest, can be "hurt" by an adult defibrillation energy setting.
All AEDs approved for use in the United States use an electronic voice to prompt users through each step. Because the user of an AED may be deaf or hard of hearing, many AEDs now include a screen to provide visual prompts. Most units today are designed for use by non-medical operators. Their ease of use has given rise to the notion of public access defibrillation (PAD), which experts agree has the potential to be the single greatest advance in the treatment of out-of-hospital cardiac arrest since the invention of CPR [5].
Liability
Most health professionals agree that automated external defibrillators are so easy to use that most, if not all, states in the United States now include the "good faith" use of an AED by any person under the Good Samaritan laws. "Good faith" protection under a Good Samaritan law means that a first aid responder cannot be held civilly liable for the harm or death of a victim by providing improper or inadequate care, given that the harm or death was not intentional (and other certain circumstances). In the United States, Good Samaritan laws[6] provide protection for the use of AEDs by trained and untrained responders, to a point. Even for trained providers, AEDs provide little liability if used correctly, in fact even the NREMT-B and many state EMT and almost all CPR classes offered incorporate AED education as parts of their program. In addition to the Good Samaritan laws, Ontario in Canada also has the “Chase McEachern Act (Heart Defibrillator Civil Liability), 2007 (Bill 171 – Subsection N) ” passed in June, 2007[7] This legislation now protects individuals from liability for damages that may occur from their use of an AED to save someone’s life at the immediate scene of an emergency, unless damages are caused by gross negligence.
References
- ↑ 1.0 1.1 Kerber, Richard E (1997). "Automatic External Defibrillators for Public Access Defibrillation". Circulation. American Heart Association. 95 (1677–1682). Unknown parameter
|coauthors=ignored (help)Retrieved on 28 June 2007 - ↑ "CPR Adult Courses". American Red Cross.Retrieved on 28 June 2007
- ↑ "Heartstart Home Defibrillator". Philips Electronics.Retrieved on 15 June 2007
- ↑ Barnaby (3rd May 2005). "Do It Yourself: The Home Heart Defibrillator". Unknown parameter
|publication=ignored (help); Unknown parameter|First=ignored (|first=suggested) (help); Check date values in:|date=(help)Retrieved on 15 June 2007 - ↑ Introduction to the International Guidelines 2000 for CPR and ECC
- ↑ State Laws on Heart Attacks, Cardiac Arrest & Defibrillators
- ↑ Health System Improvement Act, 2007 Retrieved on 26 June 2007
See Also
External links
- American Heart Association: Learn & Live
- American Red Cross: Saving a Life is as Easy as A-E-D
- FDA Heart Health Online: Automated External Defibrillator (AED)
- Resuscitation Council (UK)
Template:Emergency medicine it:Defibrillatore semiautomatico nl:Automatische externe defibrillator