Denosumab: Difference between revisions
(Blanked the page) |
No edit summary |
||
| Line 1: | Line 1: | ||
{{DrugProjectFormSinglePage | |||
|authorTag={{SS}} | |||
|genericName=Denosumab | |||
|aOrAn=a | |||
|drugClass=Monoclonal Antibody | |||
|indicationType=treatment | |||
|indication=Postmenopausal Women with [[Osteoporosis]] at High Risk for Fracture, Increase Bone Mass in Men with [[Osteoporosis]], Bone Loss in Men Receiving [[Androgen Deprivation Therapy]] for [[Prostate Cancer]], Bone Loss in Women Receiving Adjuvant [[Aromatase Inhibitor]] Therapy for [[Breast Cancer]] | |||
|adverseReactions=[[Hypercholesterolemia]], [[Diarrhea]], [[Nausea]], [[Vomiting]], [[Arthralgia]], [[Backache]], Pain in limb, [[Asthenia]], [[Headache]], [[Cystitis]], [[Nasopharyngitis]], [[Upper respiratory infection]], [[Fatigue]] | |||
|blackBoxWarningTitle=<b><span style="color:#FF0000;">TITLE</span></b> | |||
|blackBoxWarningBody=<i><span style="color:#FF0000;">Condition Name:</span></i> (Content) | |||
|fdaLIADAdult=<H4>Recommended Dosage</H4> | |||
* Prolia should be administered by a healthcare professional. | |||
* Recommended dose '''60 mg IV SC once every 6 months'''. | |||
:* Administer Prolia via subcutaneous injection in the upper arm, the upper thigh, or the abdomen. | |||
:* All patients should receive calcium 1000 mg daily and at least 400 IU vitamin D daily | |||
:* If a dose of Prolia is missed, administer the injection as soon as the patient is available. Thereafter, schedule injections every 6 months from the date of the last injection. | |||
<h4>Preparation and Administration</h4> | |||
* Visually inspect Prolia for particulate matter and discoloration prior to administration whenever solution and container permit. Prolia is a clear, colorless to pale yellow solution that may contain trace amounts of translucent to white proteinaceous particles. Do not use if the solution is discolored or cloudy or if the solution contains many particles or foreign particulate matter. | |||
* <u>Latex Allergy</u>: People sensitive to latex should not handle the grey needle cap on the single-use prefilled syringe, which contains dry natural rubber (a derivative of latex). | |||
Prior to administration, Prolia may be removed from the refrigerator and brought to room temperature (up to 25°C/77°F) by standing in the original container. This generally takes 15 to 30 minutes. Do not warm Prolia in any other way. | |||
<u>Instructions for Prefilled Syringe with Needle Safety Guard</u> | |||
'''IMPORTANT''': In order to minimize accidental needlesticks, the Prolia single-use prefilled syringe will have a green safety guard; manually activate the safety guard after the injection is given. | |||
'''DO NOT''' slide the green safety guard forward over the needle before administering the injection; it will lock in place and prevent injection. | |||
[[File:Denosumab_administration_01.png|thumb|none|400px|This image is provided by the National Library of Medicine.]] | |||
Activate the green safety guard (slide over the needle) after the injection. | |||
The grey needle cap on the single-use prefilled syringe contains dry natural rubber (a derivative of latex); people sensitive to latex should not handle the cap. | |||
<i><u>Step 1: Remove Grey Needle Cap</u></i> | |||
[[File:Denosumab_administration_02.png|thumb|none|400px|This image is provided by the National Library of Medicine.]] | |||
<i><u>Step 2: Administer Subcutaneous Injection</u></i> | |||
[[File:Denosumab_administration_03.png|thumb|none|400px|This image is provided by the National Library of Medicine.]] | |||
'''DO NOT''' put grey needle cap back on needle. | |||
<i><u>Step 3: Immediately Slide Green Safety Guard Over Needle</u></i> | |||
With the needle pointing away from you… | |||
Hold the prefilled syringe by the clear plastic finger grip with one hand. Then, with the other hand, grasp the green safety guard by its base and gently slide it towards the needle until the green safety guard locks securely in place and/or you hear a “click.” '''DO NOT''' grip the green safety guard too firmly – it will move easily if you hold and slide it gently. | |||
[[File:Denosumab_administration_04.png|thumb|none|400px|This image is provided by the National Library of Medicine.]] | |||
Immediately dispose of the syringe and needle cap in the nearest sharps container. DO NOT put the needle cap back on the used syringe. | |||
<i><u>Instructions for Single-use Vial</u></i> | |||
For administration of Prolia from the single-use vial, use a 27-gauge needle to withdraw and inject the 1 mL dose. Do not re-enter the vial. Discard vial and any liquid remaining in the vial. | |||
|offLabelAdultGuideSupport=There is limited information regarding <i>Off-Label Guideline-Supported Use</i> of Denosumab in adult patients. | |||
|offLabelAdultNoGuideSupport=There is limited information regarding <i>Off-Label Non–Guideline-Supported Use</i> of Denosumab in adult patients. | |||
|fdaLIADPed=Prolia is not recommended in pediatric patients | |||
|offLabelPedGuideSupport=There is limited information regarding <i>Off-Label Guideline-Supported Use</i> of Denosumab in pediatric patients. | |||
|offLabelPedNoGuideSupport=There is limited information regarding <i>Off-Label Non–Guideline-Supported Use</i> of Denosumab in pediatric patients. | |||
|contraindications=====[[Hypocalcemia]]==== | |||
Pre-existing [[hypocalcemia]] must be corrected prior to initiating therapy with Prolia. | |||
====Pregnancy==== | |||
Prolia may cause fetal harm when administered to a pregnant woman. In utero denosumab exposure in cynomolgus monkeys resulted in increased fetal loss, stillbirths, and postnatal mortality, along with evidence of absent lymph nodes, abnormal bone growth and decreased neonatal growth. Prolia is contraindicated in women who are pregnant. If this drug is used during pregnancy, or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential hazard to a fetus. | |||
====[[Hypersensitivity]]==== | |||
Prolia is contraindicated in patients with a history of systemic [[hypersensitivity]] to any component of the product. Reactions have included [[anaphylaxis]], [[facial swelling]] and [[urticaria]] | |||
|warnings=====Drug Products with Same Active Ingredient==== | |||
Prolia contains the same active ingredient (denosumab) found in Xgeva. Patients receiving Prolia should not receive Xgeva. | |||
====[[Hypersensitivity]]==== | |||
Clinically significant hypersensitivity including [[anaphylaxis]] has been reported with Prolia. Symptoms have included [[hypotension]], [[dyspnea]], throat tightness, facial and upper airway edema, [[pruritus]], and [[urticaria]]. If an anaphylactic or other clinically significant allergic reaction occurs, initiate appropriate therapy and discontinue further use of Prolia. | |||
====[[Hypocalcemia]] and Mineral Metabolism==== | |||
[[Hypocalcemia]] may be exacerbated by the use of Prolia. Pre-existing [[hypocalcemia]] must be corrected prior to initiating therapy with Prolia. In patients predisposed to [[hypocalcemia]] and disturbances of mineral metabolism (e.g. history of [[hypoparathyroidism]], thyroid surgery, parathyroid surgery, [[malabsorption syndromes]], excision of small intestine, severe renal impairment [creatinine clearance <30 mL/min] or receiving dialysis), clinical monitoring of calcium and mineral levels (phosphorus and magnesium) is highly recommended. | |||
[[Hypocalcemia]] following Prolia administration is a significant risk in patients with severe renal impairment [creatinine clearance <30 mL/min] or receiving dialysis. These patients may also develop marked elevations of serum parathyroid hormone (PTH). Instruct all patients with severe renal impairment, including those receiving [[dialysis]], about the symptoms of [[hypocalcemia]] and the importance of maintaining calcium levels with adequate calcium and vitamin D supplementation. | |||
Adequately supplement all patients with calcium and vitamin D. | |||
====[[Osteonecrosis]] of the Jaw==== | |||
[[Osteonecrosis]] of the jaw (ONJ), which can occur spontaneously, is generally associated with tooth extraction and/or local infection with delayed healing. ONJ has been reported in patients receiving denosumab. A routine oral exam should be performed by the prescriber prior to initiation of Prolia treatment. A dental examination with appropriate preventive dentistry should be considered prior to treatment with Prolia in patients with risk factors for ONJ such as invasive dental procedures (e.g. tooth extraction, dental implants, oral surgery), diagnosis of cancer, concomitant therapies (e.g. chemotherapy, corticosteroids), poor oral hygiene, and co-morbid disorders (e.g. periodontal and/or other pre-existing dental disease, [[anemia]], [[coagulopathy]], infection, ill-fitting dentures). Good oral hygiene practices should be maintained during treatment with Prolia. | |||
For patients requiring invasive dental procedures, clinical judgment of the treating physician and/or oral surgeon should guide the management plan of each patient based on individual benefit-risk assessment. | |||
Patients who are suspected of having or who develop ONJ while on Prolia should receive care by a dentist or an oral surgeon. In these patients, extensive dental surgery to treat ONJ may exacerbate the condition. Discontinuation of Prolia therapy should be considered based on individual benefit-risk assessment. | |||
====[[Atypical Subtrochanteric]] and [[Diaphyseal Femoral Fractures]]==== | |||
Atypical low-energy or low trauma fractures of the shaft have been reported in patients receiving Prolia. These fractures can occur anywhere in the femoral shaft from just below the lesser trochanter to above the supracondylar flare and are transverse or short oblique in orientation without evidence of comminution. Causality has not been established as these fractures also occur in osteoporotic patients who have not been treated with anti-resorptive agents. | |||
[[Atypical femoral fractures]] most commonly occur with minimal or no trauma to the affected area. They may be bilateral and many patients report prodromal pain in the affected area, usually presenting as dull, aching thigh pain, weeks to months before a complete fracture occurs. A number of reports note that patients were also receiving treatment with [[glucocorticoids]] (e.g. [[prednisone]]) at the time of fracture.During Prolia treatment, patients should be advised to report new or unusual thigh, hip, or groin pain. Any patient who presents with thigh or groin pain should be suspected of having an [[atypical fracture]] and should be evaluated to rule out an incomplete [[femur fracture]]. Patient presenting with an atypical [[femur fracture]] should also be assessed for symptoms and signs of fracture in the contralateral limb. Interruption of Prolia therapy should be considered, pending a risk/benefit assessment, on an individual basis. | |||
====Serious Infections==== | |||
In a clinical trial of over 7800 women with [[postmenopausal osteoporosis]], serious infections leading to hospitalization were reported more frequently in the Prolia group than in the placebo group. Serious skin infections, as well as infections of the abdomen, urinary tract, and ear, were more frequent in patients treated with Prolia. [[Endocarditis]] was also reported more frequently in Prolia-treated patients. The incidence of opportunistic infections was similar between placebo and Prolia groups, and the overall incidence of infections was similar between the treatment groups. Advise patients to seek prompt medical attention if they develop signs or symptoms of severe infection, including [[cellulitis]]. | |||
Patients on concomitant immunosuppressant agents or with impaired immune systems may be at increased risk for serious infections. Consider the benefit-risk profile in such patients before treating with Prolia. In patients who develop serious infections while on Prolia, prescribers should assess the need for continued Prolia therapy. | |||
====Dermatologic Adverse Reactions==== | |||
In a large clinical trial of over 7800 women with [[postmenopausal osteoporosis]], epidermal and dermal adverse events such as [[dermatitis]], [[eczema]], and [[rashes]] occurred at a significantly higher rate in the Prolia group compared to the placebo group. Most of these events were not specific to the injection site . Consider discontinuing Prolia if severe symptoms develop. | |||
====Musculoskeletal Pain==== | |||
In post-marketing experience, severe and occasionally incapacitating bone, joint, and/or muscle pain has been reported in patients taking Prolia. The time to onset of symptoms varied from one day to several months after starting Prolia. Consider discontinuing use if severe symptoms develop . | |||
====Suppression of Bone Turnover==== | |||
In clinical trials in women with [[postmenopausal osteoporosis]], treatment with Prolia resulted in significant suppression of bone remodeling as evidenced by markers of bone turnover and bone [[histomorphometry]]. The significance of these findings and the effect of long-term treatment with Prolia are unknown. The long-term consequences of the degree of suppression of bone remodeling observed with Prolia may contribute to adverse outcomes such as [[osteonecrosis]] of the jaw, [[atypical fractures]], and delayed fracture healing. Monitor patients for these consequences. | |||
|clinicalTrials=The following serious adverse reactions are discussed below and also elsewhere in the labeling: | |||
* [[Hypocalcemia]] | |||
* Serious Infections | |||
* Dermatologic Adverse Reactions | |||
* [[Osteonecrosis]] of the Jaw | |||
* [[Atypical Subtrochanteric]] and [[Diaphyseal Femoral Fractures]] | |||
The most common adverse reactions reported with Prolia in patients with [[postmenopausal osteoporosis]] are back pain, pain in extremity, musculoskeletal pain, [[hypercholesterolemia]], and [[cystitis]]. | |||
The most common adverse reactions reported with Prolia in men with [[osteoporosis]] are back pain, [[arthralgia]], and [[nasopharyngitis]]. | |||
The most common (per patient incidence ≥ 10%) adverse reactions reported with Prolia in patients with bone loss receiving androgen deprivation therapy for [[prostate cancer]] or adjuvant [[aromatase inhibitor]] therapy for [[breast cancer]] are [[arthralgia]] and back pain. Pain in extremity and musculoskeletal pain have also been reported in clinical trials. | |||
The most common adverse reactions leading to discontinuation of Prolia in patients with [[postmenopausal osteoporosis]] are back pain and [[constipation]]. | |||
The Prolia Postmarketing Active Safety Surveillance Program is available to collect information from prescribers on specific adverse events. Please see www.proliasafety.com or call 1-800-772-6436 for more information about this program. | |||
Because clinical studies are conducted under widely varying conditions, adverse reaction rates observed in the clinical studies of a drug cannot be directly compared to rates in the clinical studies of another drug and may not reflect the rates observed in clinical practice. | |||
<u>Treatment of Postmenopausal Women with [[Osteoporosis]]</u> | |||
The safety of Prolia in the treatment of [[postmenopausal osteoporosis]] was assessed in a 3-year, randomized, double-blind, placebo-controlled, multinational study of 7808 postmenopausal women aged 60 to 91 years. A total of 3876 women were exposed to placebo and 3886 women were exposed to Prolia administered subcutaneously once every 6 months as a single 60 mg dose. All women were instructed to take at least 1000 mg of calcium and 400 IU of vitamin D supplementation per day. | |||
The incidence of all-cause mortality was 2.3% (n = 90) in the placebo group and 1.8% (n = 70) in the Prolia group. The incidence of nonfatal serious adverse events was 24.2% in the placebo group and 25.0% in the Prolia group. The percentage of patients who withdrew from the study due to adverse events was 2.1% and 2.4% for the placebo and Prolia groups, respectively. | |||
Adverse reactions reported in ≥ 2% of postmenopausal women with [[osteoporosis]] and more frequently in the Prolia-treated women than in the placebo-treated women are shown in the table below. | |||
[[File:Denosumab_adverse_01.png|thumb|none|400px|This image is provided by the National Library of Medicine.]] | |||
<i>[[Hypocalcemia]]</i> | |||
Decreases in serum calcium levels to less than 8.5 mg/dL at any visit were reported in 0.4% women in the placebo group and 1.7% women in the Prolia group. The nadir in serum calcium level occurs at approximately day 10 after Prolia dosing in subjects with normal renal function. | |||
In clinical studies, subjects with impaired renal function were more likely to have greater reductions in serum calcium levels compared to subjects with normal renal function. In a study of 55 subjects with varying degrees of renal function, serum calcium levels < 7.5 mg/dL or symptomatic [[hypocalcemia]] were observed in 5 subjects. These included no subjects in the normal renal function group, 10% of subjects in the creatinine clearance 50 to 80 mL/min group, 29% of subjects in the creatinine clearance < 30 mL/min group, and 29% of subjects in the [[hemodialysis]] group. These subjects did not receive calcium and vitamin D supplementation. In a study of 4550 postmenopausal women with [[osteoporosis]], the mean change from baseline in serum calcium level 10 days after Prolia dosing was -5.5% in subjects with creatinine clearance < 30 mL/min vs. -3.1% in subjects with creatinine clearance ≥ 30 mL/min. | |||
<i>Serious Infections</i> | |||
Receptor activator of nuclear factor kappa-B ligand (RANKL) is expressed on activated T and B lymphocytes and in lymph nodes. Therefore, a RANKL inhibitor such as Prolia may increase the risk of infection. | |||
In the clinical study of 7808 postmenopausal women with [[osteoporosis]], the incidence of infections resulting in death was 0.2% in both placebo and Prolia treatment groups. However, the incidence of nonfatal serious infections was 3.3% in the placebo and 4.0% in the Prolia groups. Hospitalizations due to serious infections in the abdomen (0.7% placebo vs. 0.9% Prolia), urinary tract (0.5% placebo vs. 0.7% Prolia), and ear (0.0% placebo vs. 0.1% Prolia) were reported. [[Endocarditis]] was reported in no placebo patients and 3 patients receiving Prolia. | |||
Skin infections, including [[erysipelas]] and [[cellulitis]], leading to hospitalization were reported more frequently in patients treated with Prolia (< 0.1% placebo vs. 0.4% Prolia). | |||
The incidence of opportunistic infections was similar to that reported with placebo. | |||
<i>Dermatologic Reactions</i> | |||
A significantly higher number of patients treated with Prolia developed epidermal and dermal adverse events (such as [[dermatitis]], [[eczema]], and [[rashes]]), with these events reported in 8.2% of the placebo and 10.8% of the Prolia groups (p < 0.0001). Most of these events were not specific to the injection site. | |||
<i>[[Osteonecrosis]] of the Jaw</i> | |||
ONJ has been reported in the osteoporosis clinical trial program in patients treated with Prolia. | |||
<I>[[Atypical Subtrochanteric]] and [[Diaphyseal Fractures]]</I> | |||
In the [[osteoporosis]] clinical trial program, [[atypical femoral fractures]] were reported in patients treated with Prolia. The duration of Prolia exposure to time of [[atypical femoral fracture]] diagnosis was as early as 2½ years. | |||
<i>[[Pancreatitis]]</i> | |||
[[Pancreatitis]] was reported in 4 patients (0.1%) in the placebo and 8 patients (0.2%) in the Prolia groups. Of these reports, 1 patient in the placebo group and all 8 patients in the Prolia group had serious events, including one death in the Prolia group. Several patients had a prior history of [[pancreatitis]]. The time from product administration to event occurrence was variable. | |||
<i>New Malignancies</i> | |||
The overall incidence of new malignancies was 4.3% in the placebo and 4.8% in the Prolia groups. New malignancies related to the breast (0.7% placebo vs. 0.9% Prolia), reproductive system (0.2% placebo vs. 0.5% Prolia), and gastrointestinal system (0.6% placebo vs. 0.9% Prolia) were reported. A causal relationship to drug exposure has not been established. | |||
<u>Treatment to Increase Bone Mass in Men with [[Osteoporosis]]</u> | |||
The safety of Prolia in the treatment of men with [[osteoporosis]] was assessed in a 1-year randomized, double-blind, placebo-controlled study. A total of 120 men were exposed to placebo and 120 men were exposed to Prolia administered subcutaneously once every 6 months as a single 60 mg dose. All men were instructed to take at least 1000 mg of calcium and 800 IU of vitamin D supplementation per day. | |||
The incidence of all-cause mortality was 0.8% (n = 1) in the placebo group and 0.8% (n = 1) in the Prolia group. The incidence of nonfatal serious adverse events was 7.5% in the placebo group and 8.3% in the Prolia group. The percentage of patients who withdrew from the study due to adverse events was 0% and 2.5% for the placebo and Prolia groups, respectively. | |||
Adverse reactions reported in ≥ 5% of men with osteoporosis and more frequently with Prolia than in the placebo-treated patients were: back pain (6.7% placebo vs. 8.3% Prolia), [[arthralgia]] (5.8% placebo vs. 6.7% Prolia), and [[nasopharyngitis]] (5.8% placebo vs. 6.7% Prolia). | |||
<i>Serious Infections</i> | |||
Serious infection was reported in 1 patient (0.8%) in the placebo group and no patients in the Prolia group. | |||
<i>Dermatologic Reactions</i> | |||
Epidermal and dermal adverse events (such as [[dermatitis]], [[eczema]], and [[rashes]]) were reported in 4 patients (3.3%) in the placebo group and 5 patients (4.2%) in the Prolia group. | |||
<i>[[Osteonecrosis]] of the Jaw</i> | |||
No cases of ONJ were reported. | |||
<i>[[Pancreatitis]]</i> | |||
[[Pancreatitis]] was reported in 1 patient (0.8%) in the placebo group and 1 patient (0.8%) in the Prolia group. | |||
<i>New Malignancies</i> | |||
New malignancies were reported in no patients in the placebo group and 4 (3.3%) patients (3 prostate cancers, 1 basal cell carcinoma) in the Prolia group. | |||
<u>Treatment of Bone Loss in Patients Receiving Androgen Deprivation Therapy for [[Prostate Cancer]] or Adjuvant [[Aromatase Inhibitor]] Therapy for [[Breast Cancer]]</u> | |||
The safety of Prolia in the treatment of bone loss in men with nonmetastatic [[prostate cancer]] receiving [[androgen deprivation therapy]] (ADT) was assessed in a 3‑year, randomized, double-blind, placebo-controlled, multinational study of 1468 men aged 48 to 97 years. A total of 725 men were exposed to placebo and 731 men were exposed to Prolia administered once every 6 months as a single 60 mg subcutaneous dose. All men were instructed to take at least 1000 mg of calcium and 400 IU of vitamin D supplementation per day. | |||
The incidence of serious adverse events was 30.6% in the placebo group and 34.6% in the Prolia group. The percentage of patients who withdrew from the study due to adverse events was 6.1% and 7.0% for the placebo and Prolia groups, respectively. | |||
The safety of Prolia in the treatment of bone loss in women with nonmetastatic breast cancer receiving aromatase inhibitor (AI) therapy was assessed in a 2‑year, randomized, double-blind, placebo-controlled, multinational study of 252 postmenopausal women aged 35 to 84 years. A total of 120 women were exposed to placebo and 129 women were exposed to Prolia administered once every 6 months as a single 60 mg subcutaneous dose. All women were instructed to take at least 1000 mg of calcium and 400 IU of vitamin D supplementation per day. | |||
The incidence of serious adverse events was 9.2% in the placebo group and 14.7% in the Prolia group. The percentage of patients who withdrew from the study due to adverse events was 4.2% and 0.8% for the placebo and Prolia groups, respectively. | |||
Adverse reactions reported in ≥ 10% of Prolia-treated patients receiving ADT for prostate cancer or adjuvant AI therapy for breast cancer, and more frequently than in the placebo-treated patients were: arthralgia (13.0% placebo vs. 14.3% Prolia) and back pain (10.5% placebo vs. 11.5% Prolia). Pain in extremity (7.7% placebo vs. 9.9% Prolia) and musculoskeletal pain (3.8% placebo vs. 6.0% Prolia) have also been reported in clinical trials. Additionally in Prolia-treated men with nonmetastatic [[prostate cancer]] receiving ADT, a greater incidence of cataracts was observed (1.2% placebo vs. 4.7% Prolia). [[Hypocalcemia]] (serum calcium < 8.4 mg/dL) was reported only in Prolia-treated patients (2.4% vs. 0%) at the month 1 visit. | |||
|postmarketing=Because postmarketing reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. | |||
The following adverse reactions have been identified during post approval use of Prolia: | |||
* Drug-related hypersensitivity reactions: [[anaphylaxis]], [[rash]], [[urticaria]], facial swelling, and [[erythema]] | |||
* [[Hypocalcemia]]: severe symptomatic [[hypocalcemia]] | |||
* Musculoskeletal pain, including severe cases | |||
* [[Parathyroid Hormone]] (PTH): Marked elevation in serum PTH in patients with severe renal impairment (creatinine clearance < 30 mL/min) or receiving [[dialysis]]. | |||
|alcohol=Alcohol-Denosumab interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication. | |||
}} | |||
Revision as of 20:54, 20 August 2014
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Sheng Shi, M.D. [2]
Disclaimer
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Denosumab is a Monoclonal Antibody that is FDA approved for the treatment of Postmenopausal Women with Osteoporosis at High Risk for Fracture, Increase Bone Mass in Men with Osteoporosis, Bone Loss in Men Receiving Androgen Deprivation Therapy for Prostate Cancer, Bone Loss in Women Receiving Adjuvant Aromatase Inhibitor Therapy for Breast Cancer. Common adverse reactions include Hypercholesterolemia, Diarrhea, Nausea, Vomiting, Arthralgia, Backache, Pain in limb, Asthenia, Headache, Cystitis, Nasopharyngitis, Upper respiratory infection, Fatigue.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Recommended Dosage
- Prolia should be administered by a healthcare professional.
- Recommended dose 60 mg IV SC once every 6 months.
- Administer Prolia via subcutaneous injection in the upper arm, the upper thigh, or the abdomen.
- All patients should receive calcium 1000 mg daily and at least 400 IU vitamin D daily
- If a dose of Prolia is missed, administer the injection as soon as the patient is available. Thereafter, schedule injections every 6 months from the date of the last injection.
Preparation and Administration
- Visually inspect Prolia for particulate matter and discoloration prior to administration whenever solution and container permit. Prolia is a clear, colorless to pale yellow solution that may contain trace amounts of translucent to white proteinaceous particles. Do not use if the solution is discolored or cloudy or if the solution contains many particles or foreign particulate matter.
- Latex Allergy: People sensitive to latex should not handle the grey needle cap on the single-use prefilled syringe, which contains dry natural rubber (a derivative of latex).
Prior to administration, Prolia may be removed from the refrigerator and brought to room temperature (up to 25°C/77°F) by standing in the original container. This generally takes 15 to 30 minutes. Do not warm Prolia in any other way.
Instructions for Prefilled Syringe with Needle Safety Guard
IMPORTANT: In order to minimize accidental needlesticks, the Prolia single-use prefilled syringe will have a green safety guard; manually activate the safety guard after the injection is given. DO NOT slide the green safety guard forward over the needle before administering the injection; it will lock in place and prevent injection.

Activate the green safety guard (slide over the needle) after the injection. The grey needle cap on the single-use prefilled syringe contains dry natural rubber (a derivative of latex); people sensitive to latex should not handle the cap.
Step 1: Remove Grey Needle Cap
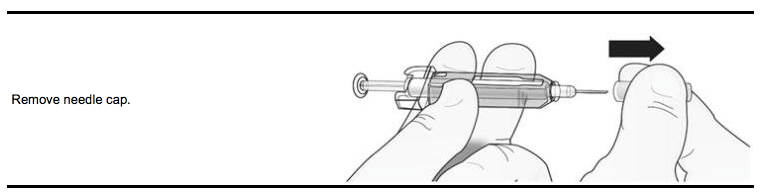
Step 2: Administer Subcutaneous Injection

DO NOT put grey needle cap back on needle.
Step 3: Immediately Slide Green Safety Guard Over Needle
With the needle pointing away from you… Hold the prefilled syringe by the clear plastic finger grip with one hand. Then, with the other hand, grasp the green safety guard by its base and gently slide it towards the needle until the green safety guard locks securely in place and/or you hear a “click.” DO NOT grip the green safety guard too firmly – it will move easily if you hold and slide it gently.

Immediately dispose of the syringe and needle cap in the nearest sharps container. DO NOT put the needle cap back on the used syringe.
Instructions for Single-use Vial
For administration of Prolia from the single-use vial, use a 27-gauge needle to withdraw and inject the 1 mL dose. Do not re-enter the vial. Discard vial and any liquid remaining in the vial.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Denosumab in adult patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Denosumab in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
Prolia is not recommended in pediatric patients
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Denosumab in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Denosumab in pediatric patients.
Contraindications
Hypocalcemia
Pre-existing hypocalcemia must be corrected prior to initiating therapy with Prolia.
Pregnancy
Prolia may cause fetal harm when administered to a pregnant woman. In utero denosumab exposure in cynomolgus monkeys resulted in increased fetal loss, stillbirths, and postnatal mortality, along with evidence of absent lymph nodes, abnormal bone growth and decreased neonatal growth. Prolia is contraindicated in women who are pregnant. If this drug is used during pregnancy, or if the patient becomes pregnant while taking this drug, the patient should be apprised of the potential hazard to a fetus.
Hypersensitivity
Prolia is contraindicated in patients with a history of systemic hypersensitivity to any component of the product. Reactions have included anaphylaxis, facial swelling and urticaria
Warnings
Drug Products with Same Active Ingredient
Prolia contains the same active ingredient (denosumab) found in Xgeva. Patients receiving Prolia should not receive Xgeva.
Hypersensitivity
Clinically significant hypersensitivity including anaphylaxis has been reported with Prolia. Symptoms have included hypotension, dyspnea, throat tightness, facial and upper airway edema, pruritus, and urticaria. If an anaphylactic or other clinically significant allergic reaction occurs, initiate appropriate therapy and discontinue further use of Prolia.
Hypocalcemia and Mineral Metabolism
Hypocalcemia may be exacerbated by the use of Prolia. Pre-existing hypocalcemia must be corrected prior to initiating therapy with Prolia. In patients predisposed to hypocalcemia and disturbances of mineral metabolism (e.g. history of hypoparathyroidism, thyroid surgery, parathyroid surgery, malabsorption syndromes, excision of small intestine, severe renal impairment [creatinine clearance <30 mL/min] or receiving dialysis), clinical monitoring of calcium and mineral levels (phosphorus and magnesium) is highly recommended. Hypocalcemia following Prolia administration is a significant risk in patients with severe renal impairment [creatinine clearance <30 mL/min] or receiving dialysis. These patients may also develop marked elevations of serum parathyroid hormone (PTH). Instruct all patients with severe renal impairment, including those receiving dialysis, about the symptoms of hypocalcemia and the importance of maintaining calcium levels with adequate calcium and vitamin D supplementation. Adequately supplement all patients with calcium and vitamin D.
Osteonecrosis of the Jaw
Osteonecrosis of the jaw (ONJ), which can occur spontaneously, is generally associated with tooth extraction and/or local infection with delayed healing. ONJ has been reported in patients receiving denosumab. A routine oral exam should be performed by the prescriber prior to initiation of Prolia treatment. A dental examination with appropriate preventive dentistry should be considered prior to treatment with Prolia in patients with risk factors for ONJ such as invasive dental procedures (e.g. tooth extraction, dental implants, oral surgery), diagnosis of cancer, concomitant therapies (e.g. chemotherapy, corticosteroids), poor oral hygiene, and co-morbid disorders (e.g. periodontal and/or other pre-existing dental disease, anemia, coagulopathy, infection, ill-fitting dentures). Good oral hygiene practices should be maintained during treatment with Prolia. For patients requiring invasive dental procedures, clinical judgment of the treating physician and/or oral surgeon should guide the management plan of each patient based on individual benefit-risk assessment. Patients who are suspected of having or who develop ONJ while on Prolia should receive care by a dentist or an oral surgeon. In these patients, extensive dental surgery to treat ONJ may exacerbate the condition. Discontinuation of Prolia therapy should be considered based on individual benefit-risk assessment.
Atypical Subtrochanteric and Diaphyseal Femoral Fractures
Atypical low-energy or low trauma fractures of the shaft have been reported in patients receiving Prolia. These fractures can occur anywhere in the femoral shaft from just below the lesser trochanter to above the supracondylar flare and are transverse or short oblique in orientation without evidence of comminution. Causality has not been established as these fractures also occur in osteoporotic patients who have not been treated with anti-resorptive agents. Atypical femoral fractures most commonly occur with minimal or no trauma to the affected area. They may be bilateral and many patients report prodromal pain in the affected area, usually presenting as dull, aching thigh pain, weeks to months before a complete fracture occurs. A number of reports note that patients were also receiving treatment with glucocorticoids (e.g. prednisone) at the time of fracture.During Prolia treatment, patients should be advised to report new or unusual thigh, hip, or groin pain. Any patient who presents with thigh or groin pain should be suspected of having an atypical fracture and should be evaluated to rule out an incomplete femur fracture. Patient presenting with an atypical femur fracture should also be assessed for symptoms and signs of fracture in the contralateral limb. Interruption of Prolia therapy should be considered, pending a risk/benefit assessment, on an individual basis.
Serious Infections
In a clinical trial of over 7800 women with postmenopausal osteoporosis, serious infections leading to hospitalization were reported more frequently in the Prolia group than in the placebo group. Serious skin infections, as well as infections of the abdomen, urinary tract, and ear, were more frequent in patients treated with Prolia. Endocarditis was also reported more frequently in Prolia-treated patients. The incidence of opportunistic infections was similar between placebo and Prolia groups, and the overall incidence of infections was similar between the treatment groups. Advise patients to seek prompt medical attention if they develop signs or symptoms of severe infection, including cellulitis. Patients on concomitant immunosuppressant agents or with impaired immune systems may be at increased risk for serious infections. Consider the benefit-risk profile in such patients before treating with Prolia. In patients who develop serious infections while on Prolia, prescribers should assess the need for continued Prolia therapy.
Dermatologic Adverse Reactions
In a large clinical trial of over 7800 women with postmenopausal osteoporosis, epidermal and dermal adverse events such as dermatitis, eczema, and rashes occurred at a significantly higher rate in the Prolia group compared to the placebo group. Most of these events were not specific to the injection site . Consider discontinuing Prolia if severe symptoms develop.
Musculoskeletal Pain
In post-marketing experience, severe and occasionally incapacitating bone, joint, and/or muscle pain has been reported in patients taking Prolia. The time to onset of symptoms varied from one day to several months after starting Prolia. Consider discontinuing use if severe symptoms develop .
Suppression of Bone Turnover
In clinical trials in women with postmenopausal osteoporosis, treatment with Prolia resulted in significant suppression of bone remodeling as evidenced by markers of bone turnover and bone histomorphometry. The significance of these findings and the effect of long-term treatment with Prolia are unknown. The long-term consequences of the degree of suppression of bone remodeling observed with Prolia may contribute to adverse outcomes such as osteonecrosis of the jaw, atypical fractures, and delayed fracture healing. Monitor patients for these consequences.
Adverse Reactions
Clinical Trials Experience
The following serious adverse reactions are discussed below and also elsewhere in the labeling:
- Hypocalcemia
- Serious Infections
- Dermatologic Adverse Reactions
- Osteonecrosis of the Jaw
- Atypical Subtrochanteric and Diaphyseal Femoral Fractures
The most common adverse reactions reported with Prolia in patients with postmenopausal osteoporosis are back pain, pain in extremity, musculoskeletal pain, hypercholesterolemia, and cystitis. The most common adverse reactions reported with Prolia in men with osteoporosis are back pain, arthralgia, and nasopharyngitis. The most common (per patient incidence ≥ 10%) adverse reactions reported with Prolia in patients with bone loss receiving androgen deprivation therapy for prostate cancer or adjuvant aromatase inhibitor therapy for breast cancer are arthralgia and back pain. Pain in extremity and musculoskeletal pain have also been reported in clinical trials. The most common adverse reactions leading to discontinuation of Prolia in patients with postmenopausal osteoporosis are back pain and constipation. The Prolia Postmarketing Active Safety Surveillance Program is available to collect information from prescribers on specific adverse events. Please see www.proliasafety.com or call 1-800-772-6436 for more information about this program.
Because clinical studies are conducted under widely varying conditions, adverse reaction rates observed in the clinical studies of a drug cannot be directly compared to rates in the clinical studies of another drug and may not reflect the rates observed in clinical practice.
Treatment of Postmenopausal Women with Osteoporosis
The safety of Prolia in the treatment of postmenopausal osteoporosis was assessed in a 3-year, randomized, double-blind, placebo-controlled, multinational study of 7808 postmenopausal women aged 60 to 91 years. A total of 3876 women were exposed to placebo and 3886 women were exposed to Prolia administered subcutaneously once every 6 months as a single 60 mg dose. All women were instructed to take at least 1000 mg of calcium and 400 IU of vitamin D supplementation per day. The incidence of all-cause mortality was 2.3% (n = 90) in the placebo group and 1.8% (n = 70) in the Prolia group. The incidence of nonfatal serious adverse events was 24.2% in the placebo group and 25.0% in the Prolia group. The percentage of patients who withdrew from the study due to adverse events was 2.1% and 2.4% for the placebo and Prolia groups, respectively. Adverse reactions reported in ≥ 2% of postmenopausal women with osteoporosis and more frequently in the Prolia-treated women than in the placebo-treated women are shown in the table below.

Decreases in serum calcium levels to less than 8.5 mg/dL at any visit were reported in 0.4% women in the placebo group and 1.7% women in the Prolia group. The nadir in serum calcium level occurs at approximately day 10 after Prolia dosing in subjects with normal renal function. In clinical studies, subjects with impaired renal function were more likely to have greater reductions in serum calcium levels compared to subjects with normal renal function. In a study of 55 subjects with varying degrees of renal function, serum calcium levels < 7.5 mg/dL or symptomatic hypocalcemia were observed in 5 subjects. These included no subjects in the normal renal function group, 10% of subjects in the creatinine clearance 50 to 80 mL/min group, 29% of subjects in the creatinine clearance < 30 mL/min group, and 29% of subjects in the hemodialysis group. These subjects did not receive calcium and vitamin D supplementation. In a study of 4550 postmenopausal women with osteoporosis, the mean change from baseline in serum calcium level 10 days after Prolia dosing was -5.5% in subjects with creatinine clearance < 30 mL/min vs. -3.1% in subjects with creatinine clearance ≥ 30 mL/min.
Serious Infections
Receptor activator of nuclear factor kappa-B ligand (RANKL) is expressed on activated T and B lymphocytes and in lymph nodes. Therefore, a RANKL inhibitor such as Prolia may increase the risk of infection. In the clinical study of 7808 postmenopausal women with osteoporosis, the incidence of infections resulting in death was 0.2% in both placebo and Prolia treatment groups. However, the incidence of nonfatal serious infections was 3.3% in the placebo and 4.0% in the Prolia groups. Hospitalizations due to serious infections in the abdomen (0.7% placebo vs. 0.9% Prolia), urinary tract (0.5% placebo vs. 0.7% Prolia), and ear (0.0% placebo vs. 0.1% Prolia) were reported. Endocarditis was reported in no placebo patients and 3 patients receiving Prolia. Skin infections, including erysipelas and cellulitis, leading to hospitalization were reported more frequently in patients treated with Prolia (< 0.1% placebo vs. 0.4% Prolia). The incidence of opportunistic infections was similar to that reported with placebo.
Dermatologic Reactions
A significantly higher number of patients treated with Prolia developed epidermal and dermal adverse events (such as dermatitis, eczema, and rashes), with these events reported in 8.2% of the placebo and 10.8% of the Prolia groups (p < 0.0001). Most of these events were not specific to the injection site.
Osteonecrosis of the Jaw
ONJ has been reported in the osteoporosis clinical trial program in patients treated with Prolia.
Atypical Subtrochanteric and Diaphyseal Fractures
In the osteoporosis clinical trial program, atypical femoral fractures were reported in patients treated with Prolia. The duration of Prolia exposure to time of atypical femoral fracture diagnosis was as early as 2½ years.
Pancreatitis was reported in 4 patients (0.1%) in the placebo and 8 patients (0.2%) in the Prolia groups. Of these reports, 1 patient in the placebo group and all 8 patients in the Prolia group had serious events, including one death in the Prolia group. Several patients had a prior history of pancreatitis. The time from product administration to event occurrence was variable.
New Malignancies
The overall incidence of new malignancies was 4.3% in the placebo and 4.8% in the Prolia groups. New malignancies related to the breast (0.7% placebo vs. 0.9% Prolia), reproductive system (0.2% placebo vs. 0.5% Prolia), and gastrointestinal system (0.6% placebo vs. 0.9% Prolia) were reported. A causal relationship to drug exposure has not been established.
Treatment to Increase Bone Mass in Men with Osteoporosis
The safety of Prolia in the treatment of men with osteoporosis was assessed in a 1-year randomized, double-blind, placebo-controlled study. A total of 120 men were exposed to placebo and 120 men were exposed to Prolia administered subcutaneously once every 6 months as a single 60 mg dose. All men were instructed to take at least 1000 mg of calcium and 800 IU of vitamin D supplementation per day. The incidence of all-cause mortality was 0.8% (n = 1) in the placebo group and 0.8% (n = 1) in the Prolia group. The incidence of nonfatal serious adverse events was 7.5% in the placebo group and 8.3% in the Prolia group. The percentage of patients who withdrew from the study due to adverse events was 0% and 2.5% for the placebo and Prolia groups, respectively. Adverse reactions reported in ≥ 5% of men with osteoporosis and more frequently with Prolia than in the placebo-treated patients were: back pain (6.7% placebo vs. 8.3% Prolia), arthralgia (5.8% placebo vs. 6.7% Prolia), and nasopharyngitis (5.8% placebo vs. 6.7% Prolia).
Serious Infections
Serious infection was reported in 1 patient (0.8%) in the placebo group and no patients in the Prolia group.
Dermatologic Reactions
Epidermal and dermal adverse events (such as dermatitis, eczema, and rashes) were reported in 4 patients (3.3%) in the placebo group and 5 patients (4.2%) in the Prolia group.
Osteonecrosis of the Jaw
No cases of ONJ were reported.
Pancreatitis was reported in 1 patient (0.8%) in the placebo group and 1 patient (0.8%) in the Prolia group.
New Malignancies
New malignancies were reported in no patients in the placebo group and 4 (3.3%) patients (3 prostate cancers, 1 basal cell carcinoma) in the Prolia group.
Treatment of Bone Loss in Patients Receiving Androgen Deprivation Therapy for Prostate Cancer or Adjuvant Aromatase Inhibitor Therapy for Breast Cancer
The safety of Prolia in the treatment of bone loss in men with nonmetastatic prostate cancer receiving androgen deprivation therapy (ADT) was assessed in a 3‑year, randomized, double-blind, placebo-controlled, multinational study of 1468 men aged 48 to 97 years. A total of 725 men were exposed to placebo and 731 men were exposed to Prolia administered once every 6 months as a single 60 mg subcutaneous dose. All men were instructed to take at least 1000 mg of calcium and 400 IU of vitamin D supplementation per day. The incidence of serious adverse events was 30.6% in the placebo group and 34.6% in the Prolia group. The percentage of patients who withdrew from the study due to adverse events was 6.1% and 7.0% for the placebo and Prolia groups, respectively. The safety of Prolia in the treatment of bone loss in women with nonmetastatic breast cancer receiving aromatase inhibitor (AI) therapy was assessed in a 2‑year, randomized, double-blind, placebo-controlled, multinational study of 252 postmenopausal women aged 35 to 84 years. A total of 120 women were exposed to placebo and 129 women were exposed to Prolia administered once every 6 months as a single 60 mg subcutaneous dose. All women were instructed to take at least 1000 mg of calcium and 400 IU of vitamin D supplementation per day. The incidence of serious adverse events was 9.2% in the placebo group and 14.7% in the Prolia group. The percentage of patients who withdrew from the study due to adverse events was 4.2% and 0.8% for the placebo and Prolia groups, respectively. Adverse reactions reported in ≥ 10% of Prolia-treated patients receiving ADT for prostate cancer or adjuvant AI therapy for breast cancer, and more frequently than in the placebo-treated patients were: arthralgia (13.0% placebo vs. 14.3% Prolia) and back pain (10.5% placebo vs. 11.5% Prolia). Pain in extremity (7.7% placebo vs. 9.9% Prolia) and musculoskeletal pain (3.8% placebo vs. 6.0% Prolia) have also been reported in clinical trials. Additionally in Prolia-treated men with nonmetastatic prostate cancer receiving ADT, a greater incidence of cataracts was observed (1.2% placebo vs. 4.7% Prolia). Hypocalcemia (serum calcium < 8.4 mg/dL) was reported only in Prolia-treated patients (2.4% vs. 0%) at the month 1 visit.
Postmarketing Experience
Because postmarketing reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. The following adverse reactions have been identified during post approval use of Prolia:
- Drug-related hypersensitivity reactions: anaphylaxis, rash, urticaria, facial swelling, and erythema
- Hypocalcemia: severe symptomatic hypocalcemia
- Musculoskeletal pain, including severe cases
- Parathyroid Hormone (PTH): Marked elevation in serum PTH in patients with severe renal impairment (creatinine clearance < 30 mL/min) or receiving dialysis.
Drug Interactions
There is limited information regarding Denosumab Drug Interactions in the drug label.
Use in Specific Populations
Pregnancy
Pregnancy Category (FDA):
There is no FDA guidance on usage of Denosumab in women who are pregnant.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Denosumab in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Denosumab during labor and delivery.
Nursing Mothers
There is no FDA guidance on the use of Denosumab in women who are nursing.
Pediatric Use
There is no FDA guidance on the use of Denosumab in pediatric settings.
Geriatic Use
There is no FDA guidance on the use of Denosumab in geriatric settings.
Gender
There is no FDA guidance on the use of Denosumab with respect to specific gender populations.
Race
There is no FDA guidance on the use of Denosumab with respect to specific racial populations.
Renal Impairment
There is no FDA guidance on the use of Denosumab in patients with renal impairment.
Hepatic Impairment
There is no FDA guidance on the use of Denosumab in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Denosumab in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Denosumab in patients who are immunocompromised.
Administration and Monitoring
Administration
There is limited information regarding Denosumab Administration in the drug label.
Monitoring
There is limited information regarding Denosumab Monitoring in the drug label.
IV Compatibility
There is limited information regarding the compatibility of Denosumab and IV administrations.
Overdosage
There is limited information regarding Denosumab overdosage. If you suspect drug poisoning or overdose, please contact the National Poison Help hotline (1-800-222-1222) immediately.
Pharmacology
There is limited information regarding Denosumab Pharmacology in the drug label.
Mechanism of Action
There is limited information regarding Denosumab Mechanism of Action in the drug label.
Structure
There is limited information regarding Denosumab Structure in the drug label.
Pharmacodynamics
There is limited information regarding Denosumab Pharmacodynamics in the drug label.
Pharmacokinetics
There is limited information regarding Denosumab Pharmacokinetics in the drug label.
Nonclinical Toxicology
There is limited information regarding Denosumab Nonclinical Toxicology in the drug label.
Clinical Studies
There is limited information regarding Denosumab Clinical Studies in the drug label.
How Supplied
There is limited information regarding Denosumab How Supplied in the drug label.
Storage
There is limited information regarding Denosumab Storage in the drug label.
Images
Drug Images
{{#ask: Page Name::Denosumab |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Denosumab |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
There is limited information regarding Denosumab Patient Counseling Information in the drug label.
Precautions with Alcohol
Alcohol-Denosumab interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
There is limited information regarding Denosumab Brand Names in the drug label.
Look-Alike Drug Names
There is limited information regarding Denosumab Look-Alike Drug Names in the drug label.
Drug Shortage Status
Price
References
The contents of this FDA label are provided by the National Library of Medicine.