Seborrheic dermatitis: Difference between revisions
Aysha Aslam (talk | contribs) |
Aysha Aslam (talk | contribs) |
||
| Line 93: | Line 93: | ||
*[[Vitamin B deficiency]] | *[[Vitamin B deficiency]] | ||
===Differential diagnosis in Adults=== | ===Differential diagnosis in Adults=== | ||
* | *Systemic lupus erytheramatosus | ||
*[[candidiasis]] | *[[candidiasis]] | ||
*[[Erythrasma]] | *[[Erythrasma]] | ||
| Line 101: | Line 101: | ||
*[[Tinea corporis]] | *[[Tinea corporis]] | ||
*[[Secondary syphilis]] | *[[Secondary syphilis]] | ||
* | *Pemphigous foliaceous | ||
==Epidemiology and Demographics== | ==Epidemiology and Demographics== | ||
Revision as of 18:15, 12 August 2016
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Jesus Rosario Hernandez, M.D. [2]; Aysha Anwar, M.B.B.S[3]
Synonyms and keywords: Seborrheic eczema
Overview
Seborrhoeic eczema (also known as Seborrheic dermatitis AmE, seborrhea) is a skin disorder affecting the scalp, face, and trunk. Seborrhoeic dermatitis causes flaky, itchy, red skin and temporary hair loss. It particularly affects the sebum-gland rich areas of skin. Causes of seborrhoeic dermatitis include Malassezia furfur (formerly known as Pityrosporum ovale), as well as genetic, environmental, hormonal, and immune-system factors. Medical therapy for seborrhoeic dermatitis includes antifungal agents, corticosteroids, and lithium salts.
Historical Perspective
Classification
There is no established classification system for seborrheic dermatitis.However, seborrheic dermatitis can be classified on the basis of following factors:[1][2][3][4]
- Localised
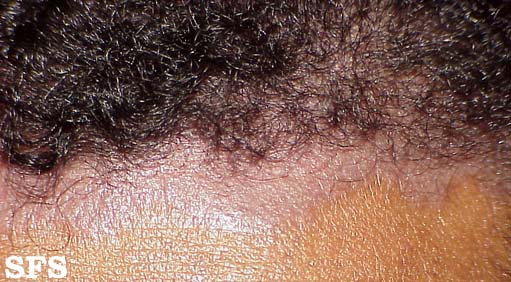
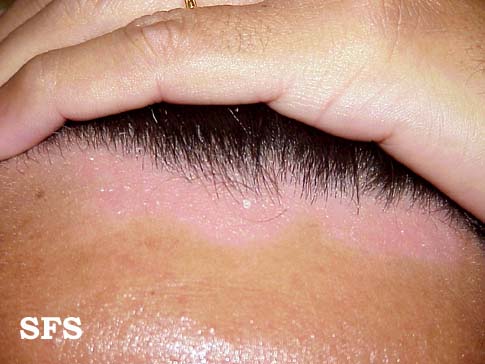
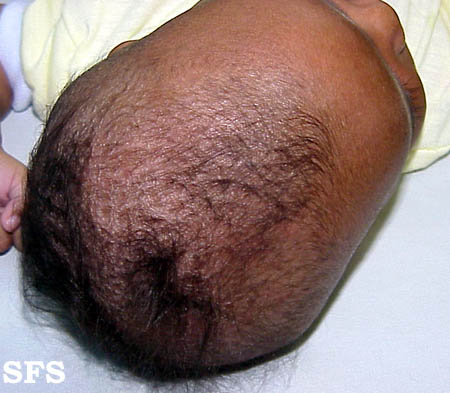
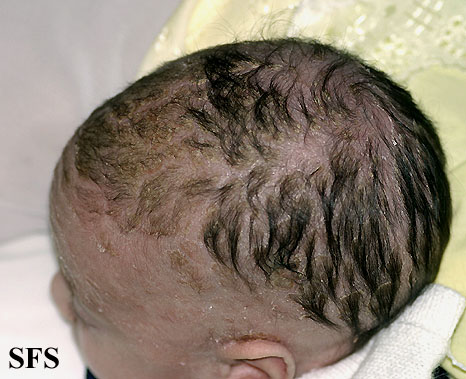
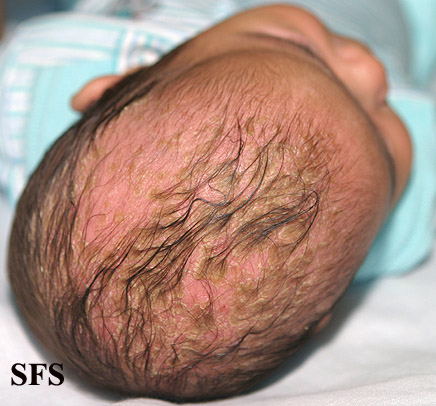
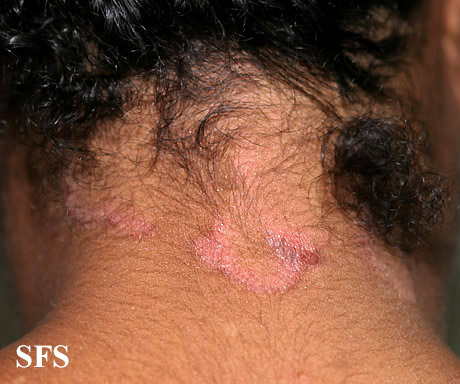
- Scalp: In infants its called Cradle Cap. Its the most common presentation in infants and appear as red yellow plaques coated by thick greasy scales, commonly appearing in first three months of age.In adults, presentation of disease is mild desquamationto honey coloured crusts which can extend to involve forehead called "corona seborrheica"
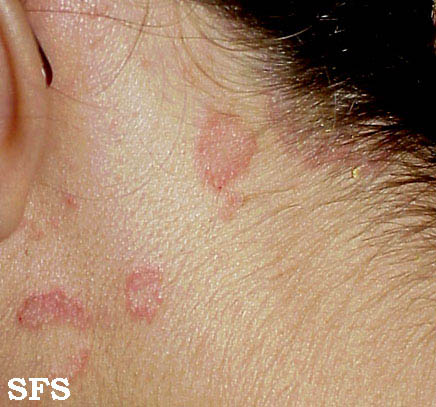
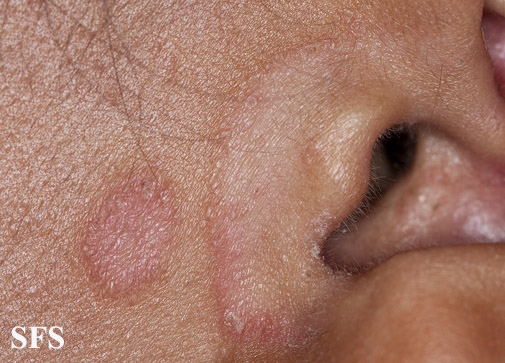
- Face: It most commonly involves eyelids, eyebrows and nasolabial folds. Eyes are involved resulting in blephritis.
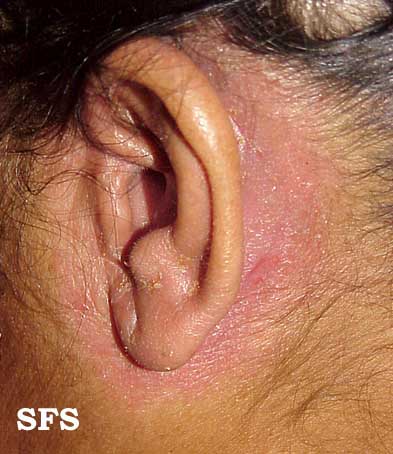
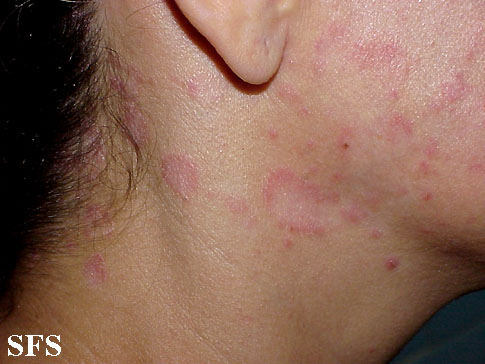
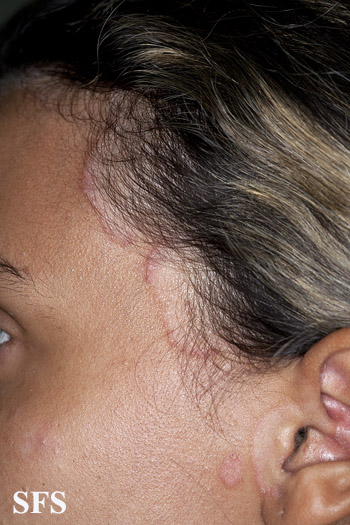
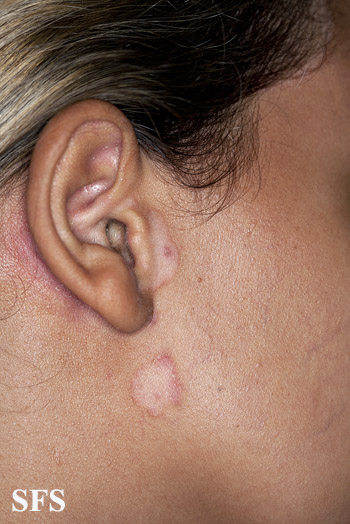
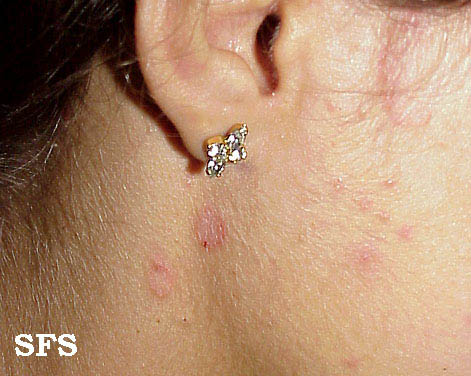
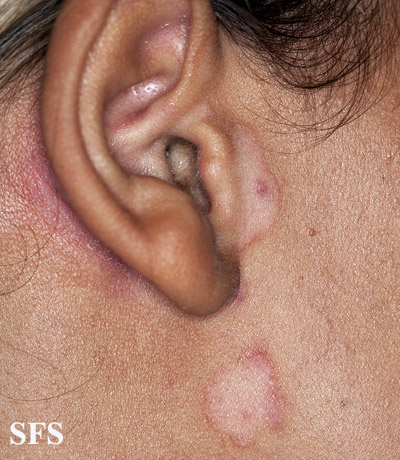
- Retroauricular: lt invloves crusting, oozing and fissuring in the affected area. It may also involve external ear resulting in otitis externa.
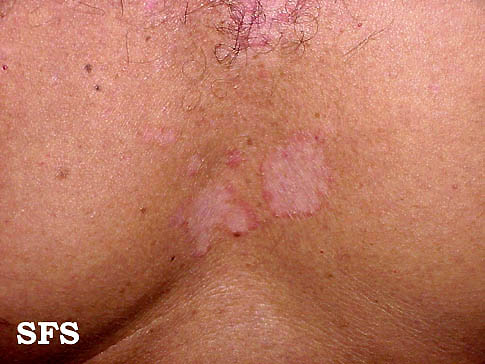
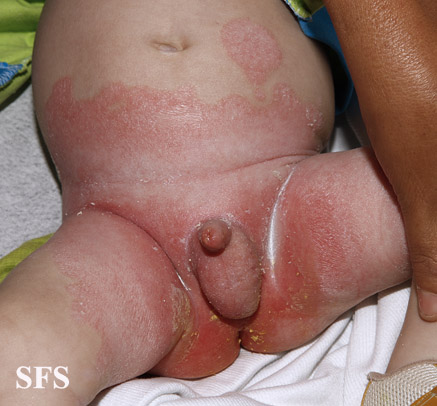
- Body folds: It usually affects axilla, breast folds, inguinal area and genital area. May progress to fissuring and secondary infection.
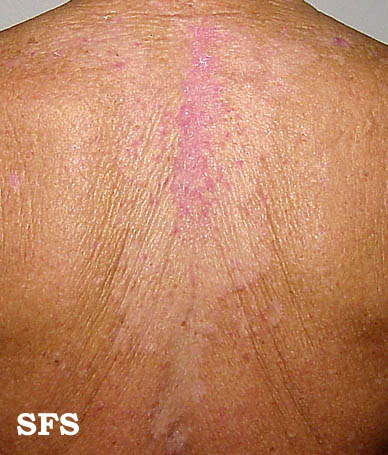
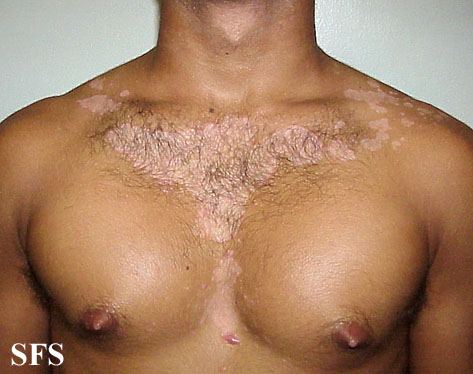
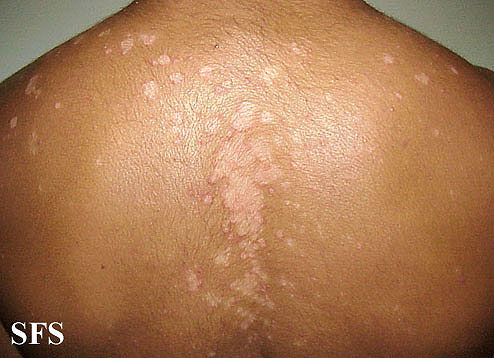
- Upper Chest: It is mostly seen in adults. Affected areas may present with one of the following presentation.
- Pityriasiform: It is usually in the form oval macules and patches ranging from 5-15mm in size which tend to involve intertriginous areas.
- Petaloid type: It appears as small papules with oily scales which enlarges to become patches giving it an appearance of petals of flower, hence the name.
- Trunk: common in infants and most common site of involvement is lower abdomen.
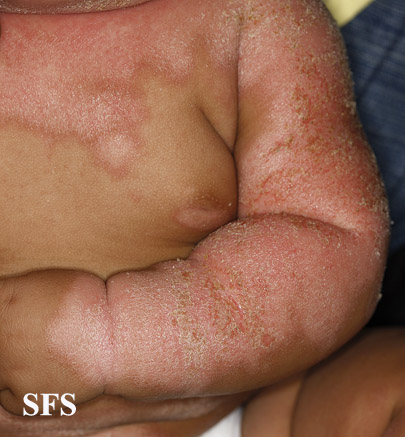
- Generalized: mostly seen in infants associated with leiner's disease and children with severe immunodeficiency. It usually is associated with diarrhea and failure to thrive and may resolve in few weeks.
Classification by Age
- Infantile: seen in first three months of life. It is mostly a self limited disease in children.
- Adults: occurs most commonly between 30-60 years of age. In adults, it usually appears as chronic relapsing condition invloving various parts of the body.
Classification by Symptomic Presentation
- Non pruritic: This type is most commonly seen in infants.
- Pruritic: This type is seen in older children and adults. This type is common with scalp involvement.
Classification by Etiology
Exact cause of seborrheic dermatitis is unknown.However, following causes may be related to pathogenesis of seborrheic dermatitis.
- Idiopathic : No known cause
- Infectious: Caused by fungus named Malssezia based on its response to antifungal agents.
- Autoimmune/Inflammatory:One hypothesis suggests it as a primary inflammatory dermatoses resulting in increased apoptosis, scaling and inflammation in epidermis[[.
Classification by Severity
- Mild to moderate disease: seen in immunocompetent individuals.
- Severe disease: Immunocomprised patients have more extensive disease which is mostly unresponsive to treatment.
Pathophysiology
Complete pathogenesis of seborrheic dermatitis is not fully understood.However, studies have demonstrated strong correlation between presence of fungal yeast Malasezia and seborrheic dermatitis.[5] There are two species of Malasezia that predominantly related to
Causes
The cause of seborrhoeic dermatitis remains unknown, although many factors have been implicated. The widely present yeast, Malassezia furfur (formerly known as Pityrosporum ovale), is involved,[6][7] as well as genetic, environmental, hormonal, and immune-system factors.[8][9] A suggestion that seborrhoeic dermatitis is an inflammatory response to this yeast has yet to be proven.[10] Those afflicted with seborrhoeic dermatitis have an unfavourable epidermic response to the infection, with the skin becoming inflamed and flaking.
In children, excessive vitamin A intake can cause seborrhoeic dermatitis.[11] Lack of biotin,[12] pyridoxine (vitamin B6)[12][13] and riboflavin (vitamin B2)[12] may also be a cause.
Differentiating Seborrheic dermatitis from Other Diseases
Differential diagnosis of seborrheic dermatitis can be classified into two types by age group
Differential diagnosis in infants
- Atopic dermatitis
- [[Candidiasis]
- Dermatophytosis
- Diaper dermatitis
- Langerhans cell histiocytosis: It usually presents as refractory seborrheic dermatitis or diaper dermatitis in infants. Diagnosis is confirmed by skin biopsy.
- Psoriasis
- Pityriasis amiantacea
- Rosacea
- Tinea capitis
- zinc deficiency
- Vitamin B deficiency
Differential diagnosis in Adults
- Systemic lupus erytheramatosus
- candidiasis
- Erythrasma
- Contact dermatitis
- Psoriasis
- Tinea versicolor
- Tinea corporis
- Secondary syphilis
- Pemphigous foliaceous
Epidemiology and Demographics
Risk Factors
Most common risk factors for Seborrheic dermatitis are[14][15]
- Immunocompromised Patients such as organ transplant recipients, patients with HIV, Hep C, chronic alcoholic pancreatitis and various malignancies such as lymphoma[16][17][18]
- Neurologic and psychiatric cases such as patients with Parkinsonism, patients with Depressive mood disorder, tardive dyskinesia, traumatic brain injury, epilepsy, facial nerve palsy, spinal cord injury
- Genetic disorders such as patients with Downs syndrome, Hailey Hailey disease, Cardiofaciocutaneous syndrome, mutation in (ZNF750) which codes for a zinc finger protein (C2H2) may be related to cause seborrhea like dermatitis
Other risk factors include
- Stress[19]
- Patients treated with psoralene and ultravoilet light A for psoriasis are seen to have a predisposition for seborrheic dermatitis.
- Male population is more prone to develop seborrheic dermatitis as compared to females.[20]
- Obesity, Diabetes Mellitus and other endocrine disorders causing alteration in glucose metabolism.[21]
- Seasonal changes such as low temperature and decreased humditiy may have a significant role in seborrheic dermatitis flare ups[22]
Screening
Natural History, Complications, and Prognosis
Natural History
Complications
Side effects to inflammation may include temporary hair loss. If severe outbreaks go untreated for long periods of time, permanent hair loss may result due to damaged hair follicles.
Prognosis
Diagnosis
Diagnostic Criteria
History and Symptoms
Physical Examination
Head
Ear
Neck
Trunk
Extremities
Genitals
Medical Therapy
- Seborrheic dermatitis[23]
- 1. Antifungal agents
- Preferred regimen (1): Ketoconazole 2% in shampoo, foam, gel, or cream
- Scalp: Twice/week for clearance THEN once/week or every other week for maintenance
- Other areas: From bid to twice/week for clearance THEN from twice/week to once every other week for maintenance
- Preferred regimen (2): Bifonazole 1% in shampoo or cream
- Scalp: 3 times/week for clearance
- Other areas: qd for clearance
- Preferred regimen (3): Ciclopirox olamine (also called ciclopirox) 1.0% or 1.5% in shampoo or cream
- Scalp: Twice to 3 times/week for clearance THEN once/week or every 2 week for maintenance
- Other areas: Twice daily for clearance THEN qd for maintenance
- 2. Corticosteroids
- Preferred regimen (1): Hydrocortisone 1% in cream areas other than scalp qd or bid
- Preferred regimen (2): Betamethasone dipropionate 0.05% in lotion scalp and other areas qd or bid
- Preferred regimen (3): Clobetasol 17- butyrate 0.05% in cream areas other than scalp qd or bid
- Preferred regimen (4): Clobetasol dipro- pionate 0.05% in shampoo
- Scalp: Twice weekly in a short- contact fashion (up to 10 min application, then washing)
- Preferred regimen (5): Desonide 0.05% lotion bid on scalp and other areas
- 3. Lithium salts
- Preferred regimen: Lithium succinate AND Zinc sulfate Ointment containing 8% Lithium succinate AND 0.05% Zinc sulfate
- Preferred regimen: Lithium gluconate 8% in gel bid on areas other than scalp
Plant-based treatments
The World Health Organization mentions Aloe vera gel as a yet to be scientifically proven traditional medicine treatment for Seborrhoeic dermatitis.[24]
- Arctium lappa (Burdock) oil[25]
- Chelidonium majus (Celandine)[25]
- Glycyrrhiza glabra (Licorice)[25]
- Melaleuca (Tea tree) species[25]
- Plantago (Plantain) species[25]
- Symphytum officinale (Comfrey)[25]
- Zingiber officinale (Ginger) root juice[25]
Imaging Findings
Other Diagnostic Studies
Treatment
Medical Therapy
Surgery
Prevention
Related Chapter
External Links
- Seborrhoeic Dermatitis at DermNet
- Seborrheic Dermatitis: An Overview - July 1, 2006 -- American Family Physician
References
- ↑ Schwartz RA, Janusz CA, Janniger CK (2006). "Seborrheic dermatitis: an overview". Am Fam Physician. 74 (1): 125–30. PMID 16848386.
- ↑ Dessinioti C, Katsambas A (2013). "Seborrheic dermatitis: etiology, risk factors, and treatments: facts and controversies". Clin Dermatol. 31 (4): 343–51. doi:10.1016/j.clindermatol.2013.01.001. PMID 23806151.
- ↑ Dessinioti, Clio, and Andreas Katsambas. "Seborrheic dermatitis: Etiology, risk factors, and treatments:: Facts and controversies." Clinics in dermatology 31.4 (2013): 343-351.
- ↑ ===Classification by Anatomical Location===Peyri, J., and M. Lleonart. "Clinical and therapeutic profile and quality of life of patients with seborrheic dermatitis." Actas Dermo-Sifiliográficas (English Edition) 98.7 (2007): 476-482.
- ↑ Soares RC, Zani MB, Arruda AC, Arruda LH, Paulino LC (2015). "Malassezia intra-specific diversity and potentially new species in the skin microbiota from Brazilian healthy subjects and seborrheic dermatitis patients". PLoS One. 10 (2): e0117921. doi:10.1371/journal.pone.0117921. PMC 4335070. PMID 25695430.
- ↑ Hay R, Graham-Brown R (1997). "Dandruff and seborrheic dermatitis: causes and management". Clin Exp Dermatol. 22 (1): 3–6. doi:10.1046/j.1365-2230.1997.d01-231.x. PMID 9330043.
- ↑ Nowicki R (2006). "[Modern management of dandruff]". Pol Merkur Lekarski. 20 (115): 121–4. PMID 16617752.
- ↑ Am Fam Physician 2000;61:2703-10,2713-4
- ↑ Janniger C, Schwartz R (1995). "Seborrheic dermatitis". Am Fam Physician. 52 (1): 149–55, 159–60. PMID 7604759.
- ↑ Parry M, Sharpe G (1998). "Seborrheic dermatitis is not caused by an altered immune response to Malassezia yeast". Br J Dermatol. 139 (2): 254–63. doi:10.1046/j.1365-2133.1998.02362.x. PMID 9767239.
- ↑ "MedlinePlus Medical Encyclopedia: Hypervitaminosis A". www.nlm.nih.gov. Retrieved 2008-03-19.
- ↑ 12.0 12.1 12.2 "Seborrheic Dermatitis: An Overview - July 1, 2006 -- American Family Physician". www.aafp.org. Retrieved 2008-03-19.
- ↑ "eMedicine - Nutritional Neuropathy : Article by R Andrew Sewell". www.emedicine.com. Retrieved 2008-03-19.
- ↑ Hastings GB, Leathar DS, Scott AC (1988). "Scottish attitudes to AIDS". Br Med J (Clin Res Ed). 296 (6627): 991–2. PMC 2545449. PMID 3129121.
- ↑ Lewak N (1974). "Letter: Mythology and SIDS". N Engl J Med. 291 (14): 740–1. doi:10.1056/NEJM197410032911423. PMID 4852869.
- ↑ Dunic I, Vesic S, Jevtovic DJ (2004). "Oral candidiasis and seborrheic dermatitis in HIV-infected patients on highly active antiretroviral therapy". HIV Med. 5 (1): 50–4. PMID 14731170.
- ↑ Soldatov IuN, Glushko AV (1974). "[Spontaneous rupture of the epigastric arteries simulating acute abdomen]". Klin Khir (11): 61–2. PMID 4280471.
- ↑ Özcan D, Seçkin D, Ada S, Haberal M (2013). "Mucocutaneous disorders in renal transplant recipients receiving sirolimus-based immunosuppressive therapy: a prospective, case-control study". Clin Transplant. 27 (5): 742–8. doi:10.1111/ctr.12215. PMID 23991694 : 23991694 Check
|pmid=value (help). - ↑ Misery L, Touboul S, Vinçot C, Dutray S, Rolland-Jacob G, Consoli SG; et al. (2007). "[Stress and seborrheic dermatitis]". Ann Dermatol Venereol. 134 (11): 833–7. PMID 18033062.
- ↑ Baran, Robert, and Howard Maibach, eds. Textbook of cosmetic dermatology. CRC Press, 2010.
- ↑ Dowlati, Bijan, et al. "Insulin quantification in patients with seborrheic dermatitis." Archives of dermatology 134.8 (1998): 1043-1045.
- ↑ Banerjee S, Gangopadhyay DN, Jana S, Chanda M (2010). "Seasonal variation in pediatric dermatoses". Indian J Dermatol. 55 (1): 44–6. doi:10.4103/0019-5154.60351. PMC 2856373. PMID 20418977.
- ↑ Stevens DL, Bisno AL, Chambers HF, Dellinger EP, Goldstein EJ, Gorbach SL; et al. (2014). "Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the infectious diseases society of America". Clin Infect Dis. 59 (2): 147–59. doi:10.1093/cid/ciu296. PMID 24947530.
- ↑ "WHO Monographs on Selected Medicinal Plants - Volume 1: Aloe Vera Gel". www.who.int. Retrieved 2008-03-18.
- ↑ 25.0 25.1 25.2 25.3 25.4 25.5 25.6 "The Green Pharmacy: New Discoveries ... - Google Book Search". books.google.com. Retrieved 2008-03-19.