Strongyloides stercoralis
| Threadworm | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
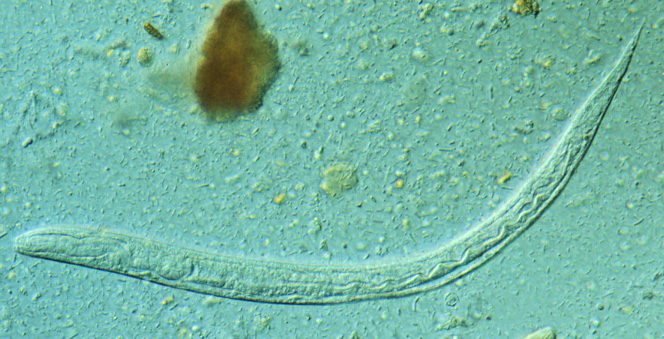 First stage larva (L1) of S. stercoralis
| ||||||||||||||
| Scientific classification | ||||||||||||||
| ||||||||||||||
| Binomial name | ||||||||||||||
| Strongyloides stercoralis Bavay, 1876 |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
|
Strongyloidiasis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Strongyloides stercoralis On the Web |
|
American Roentgen Ray Society Images of Strongyloides stercoralis |
|
Risk calculators and risk factors for Strongyloides stercoralis |
Overview
Strongyloides stercoralis is the scientific name of a human parasitic roundworm causing the disease of strongyloidiasis.
Strongyloides stercoralis is a nematode, 2.5 mm-long, that is a parasite of humans. The adult parasitic stage lives in tunnels in the mucosa of the small intestine. The genus Strongyloides contains 53 species and S. stercoralis is the type species. S. stercoralis has been reported in other primates and occasionally in dogs. However, it seems that the species in dogs is typically not S. stercoralis, but another species S. canis. Non-human primates are more commonly infected with S. fuelleborni and S. cebus although S. stercoralis has been reported in captive primates. Other species of Strongyloides naturally parasitic in humans, but with restricted distributions, are S. fuelleborni in central Africa and S. kellyi in Papua New Guinea.
Life Cycle
For S. stercoralis first stage larvae (L1) pass out in the feces and develop in feces on the ground to infective larvae (IL). This development can occur via two routes: directly from L1 to IL via three moults or indirectly. The indirect route results first in the development of free-living adult females and males which mate, females lay eggs which hatch and then develop to IL. The direct route gives IL faster (3 days) versus the indirect route (7-10 days), However, the indirect route results in an increase in the number of IL produced. Speed of development of IL is traded off for increased numbers. The free-living males and females of S. stercoralis die after one generation; they do not persist in the soil.
The infectious larvae penetrate the skin when there is contact with the soil. Some of them enter the superficial veins and ride the blood vessels to the lungs, where they enter the alveoli. They are then coughed up and swallowed into the gut, where they parasitise the intestinal mucosa (duodenum and jejunum). However, research in dogs has shown that most of the larvae that penetrate the skin migrate randomly through the body until they reach the small intestine. Only females will reach reproductive adulthood in the intestine. Female strongyloides reproduce through parthenogenesis. The eggs hatch in the intestine and young larvae are then excreted in the feces. It takes about two weeks to reach egg development from the initial skin penetration. By this process, S. stercoralis can cause both respiratory and gastrointestinal symptoms. Adult worms can live up to a year in dogs.
Auto-infection
An unusual feature of S. stercoralis is autoinfection. Only one other species in the Strongyloides genus, S. felis, has the trait of autoinfection. Autoinfection is the development of L1 into small infective larvae in the gut of the host. These autoinfective larvae penetrate the wall of the lower ileum or colon or the skin of the perianal region, enter the circulation again, up to the lungs, and back down to the small intestine thus repeating the cycle. Autoinfection makes strongyloidiasis due to S. stercoralis an infection with several unusual features.
Persistence of infection is the first of these important features. Because of autoinfection, humans have been known to still be infected up to 65 years after they were first exposed to the parasite (e.g. Vietnam veterans). Once a host is infected with S. stercoralis, infection is life-long unless effective treatment eliminates all adult parasites and migrating autoinfective larvae.
Strongyloidiasis
Strongyloidiasis in immunocompetant individuals is usually an indolent disease. However, in immunocompromised individuals strongyloidiasis can cause a hyperinfective syndrome (also called disseminated strongyloidiasis). This hyperinfective syndrome has a mortality rate of close to 90%.
Immunosuppressive drugs, such as those used for tissue transplantation, (especially corticosteroids) can increase the rate of autoinfection to the point where there is an overwhelming number of larvae migrating through the lungs, and in many cases this can prove fatal. Additionally, diseases such as HTLV-1 (Human T-cell Lymphotropic Virus 1), which enhance the Th1 arm of the immune system and lessen the Th2 arm, increase the disease state. Another consequence of autoinfection is that the autoinfective larvae can carry gut bacteria back into the body. About 50% of people with hyperinfection present with bacterial disease due to enteric bacteria. Finally, a unique effect of autoinfective larvae is larva currens due to the larvae migrating rapidly through the skin. Larva currens appears as a red line that appears, moves rapidly (>5 cm/day) and then quickly disappears. It is pathogonomic for autoinfective larvae and can be used as a diagnostic criterion for strongyloidiasis due to S. stercoralis.
Geographic Distribution
S. stercoralis has a very low prevalence in societies where faecal contamination of soil is rare. Hence, it is a very rare infection in developed market economies and is less prevalent in urban areas in developing countries than in rural areas. Strongyloidiasis was first described in the nineteenth century in French soldiers returning home from expeditions in IndoChina. Today, the countries of the old IndoChina (Vietnam, Cambodia and Laos) still have endemic strongyloidiasis, typical prevalence being 10% or less. Regions of Japan used to have endemic strongyloidiasis, but control programs have probably reduced prevalence markedly. Strongyloidiasis appears to have a high prevalence in some areas of Brazil and Central America. Strongyloidiasis is endemic in Africa, but the prevalence is typically low (1% or less). Pockets of strongyloidiasis have been reported from rural Italy, but current status is unknown. In the Pacific islands strongyloidiasis is rare although there have been reports of cases from Fiji. In tropical Australia, some rural and remote Australian Aboriginal communities have very high prevalence of strongyloidiasis . In some African countries (e.g., Zaire) S. fuelleborni was more common than S. stercoralis in parasite surveys from the 1970s, but current status is unknown. In Papua New Guinea, S. stercoralis is endemic, but prevalence is low. However, in some areas another species, S. kellyi, is a very common parasite of children in the PNG highlands and Western Province.
Knowledge of the geographic distribution of strongyloidiasis is of significance to travelers who may acquire the parasite during their stay in endemic areas.
Treatment
Ivermectin is the drug of first choice for treatment . Thiabendazole was used previously, but owing to its high prevalence of side effects and lower efficay, it has been superseded by ivermectin and as second line, albendazole. However, these drugs have little effect on the majority of these autoinfective larvae during their migration through the body. Hence, repeated treatments with ivermectin have to be administered to kill adults which develop from the autoinfective larvae.
References