Strongyloidiasis
(Redirected from Anguillulosis)
This page is about clinical aspects of the disease. For microbiologic aspects of the causative organism(s), see Strongyloides stercoralis.
| Strongyloidiasis | |
| Classification and external resources | |
| |
|---|---|
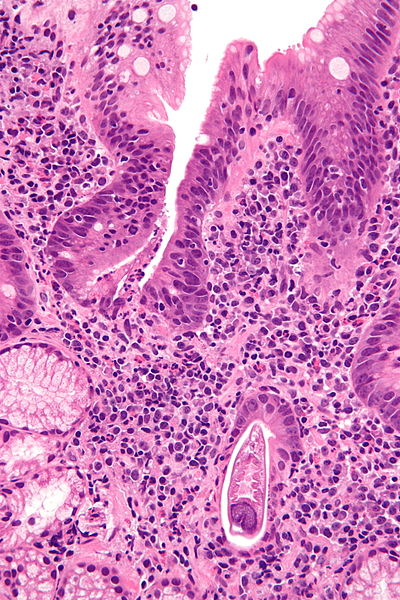
| Micrograph showing strongyloidiasis; a fragment of a worm is seen in the lower right hand corner. H&E stain. Source: https://commons.wikimedia.org/wiki/File%3AStrongyloides_-_very_high_mag_-_2.jpg |
For patient information, click here
|
Strongyloidiasis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Strongyloidiasis On the Web |
|
American Roentgen Ray Society Images of Strongyloidiasis |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Aditya Ganti M.B.B.S. [2]
Synonyms and keywords: Strongyloides infection, Hyperinfection syndrome, Intestinal strongyloidiasis, Infection by strongylus.
Overview
Historical Perspective
Classification
Pathophysiology
Causes
Differentiating Strongyloidiasis from other Diseases
Epidemiology and Demographics
Risk Factors
Screening
Natural History, Complications and Prognosis
Diagnosis
History and Symptoms | Physical Examination | Laboratory Findings | X-ray | CT scan| Ultrasound | Other Imaging findings | Other Diagnostic Studies
Treatment
Medical Therapy | Surgery | Primary Prevention | Secondary Prevention | Cost-Effectiveness of Therapy | Future or Investigational Therapies