|
|
| Line 22: |
Line 22: |
|
| |
|
| ==[[Strongyloidiasis differential diagnosis|Differentiating Strongyloidiasis from other Diseases]]== | | ==[[Strongyloidiasis differential diagnosis|Differentiating Strongyloidiasis from other Diseases]]== |
| {| class="wikitable"
| |
| ! colspan="7" |Differentiating Strongyloides stercoralis infection from other Nematode infections<ref name="Principles and Practice">Durand, Marlene (2015). "Chapter 288:Intestinal Nematodes (Roundworms)". Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases Updated Edition, Eighth Edition. Elsevier. pp. 3199–3207. ISBN 978-1-4557-4801-3.</ref><ref name="Murray and Nadel's Textbook of Respiratory Medicine">{{cite book |last1=Kim |first1=Kami |last2=Weiss |first2=Louis |last3=Tanowitz |first3=Herbert |title=Murray and Nadel's Textbook of Respiratory Medicine Sixth Edition |publisher=Elsevier |date=2016 |pages=682-698 |chapter=Chapter 39:Parasitic Infections |isbn=978-1-4557-3383-5}}</ref>
| |
| |-
| |
| |Nematode
| |
| |Transmission
| |
| |Direct Person-Person Transmission
| |
| |Duration of Infection
| |
| |Pulmonary Manifestation
| |
| |Location of Adult worm(s)
| |
| |Treatment
| |
| |-
| |
| |[[Ascaris lumbricoides]]
| |
| |Ingestion of infective ova
| |
| |No
| |
| |1-2 years
| |
| |
| |
| * [[Löffler's syndrome]] (usually about 9-12 days after exposure to ova)
| |
| * [[Cough]]
| |
| * Substernal discomfort
| |
| * [[Crackles]]
| |
| * [[Wheezing]]
| |
| * Transient opacities
| |
| |Free in the lumen of the small bowel
| |
| (primarily jejunum)
| |
| |
| |
| * [[Albendazole]]
| |
|
| |
| * [[Mebendazole]]
| |
|
| |
| * [[Pyrantel pamoate]]
| |
|
| |
| * [[Ivermectin]]
| |
|
| |
| * [[Levamisole]]
| |
|
| |
| * [[Piperazine]]
| |
| |-
| |
| |[[Trichuris trichiura]]
| |
| (whipworm)
| |
| |Ingestion of infective [[ova]]
| |
| |No
| |
| |1-3 years
| |
| |No pulmonary migration, therefore, no pulmonary manifestation
| |
| |Anchored in the superficial mucosa of cecum and colon
| |
| |
| |
| * [[Albendazole]]
| |
|
| |
| * [[Mebendazole]]
| |
| |-
| |
| |[[Hookworm]] ([[Necator americanus]] and [[Ancylostoma duodenale]])
| |
| |Skin penetration by filariform larvae
| |
| |No
| |
| |
| |
| * 3-5 years (Necator)
| |
| * 1 year (Ancylostoma)
| |
| |
| |
| * [[Löffler's syndrome]]
| |
| * Transient opacities
| |
| |Attached to the mucosa of mid-upper portion of the [[small bowel]]
| |
| |
| |
| * [[Albendazole]]
| |
|
| |
| * [[Mebendazole]]
| |
|
| |
| * [[Levamisole]]
| |
|
| |
| * [[Pyrantel pamoate]]
| |
| |-
| |
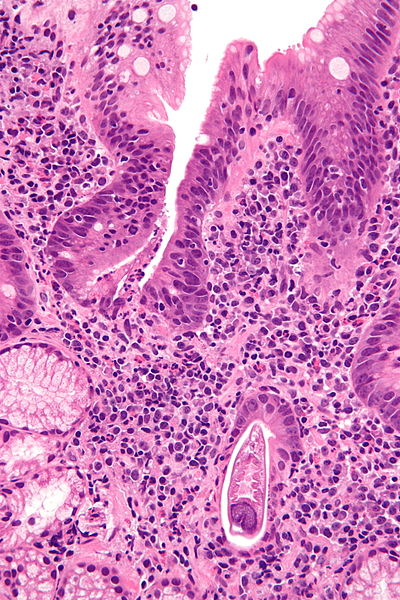
| |[[Strongyloides stercoralis]]
| |
| |Filariform larvae penetrates skin or bowel mucosa
| |
| |Yes
| |
| |Lifetime of the host
| |
| |
| |
| * [[Löffler's syndrome]]
| |
| * Chronic [[cough]]
| |
| * [[Pneumonia]] or [[sepsis]] in hyperinfection
| |
| |Embedded in the mucosa of the [[duodenum]], [[jejunum]]
| |
| |
| |
| * [[Ivermectin]]
| |
| * [[Albendazole]]
| |
| * [[Thiabendazole]]
| |
| |-
| |
| |[[Enterobius vermicularis]] ([[pinworm]])
| |
| |Ingestion of infective [[ova]]
| |
| |Yes
| |
| |1 month
| |
| |Extraintestinal migration is very rare<ref name="pmid21879805">{{cite journal| author=Serpytis M, Seinin D| title=Fatal case of ectopic enterobiasis: Enterobius vermicularis in the kidneys. | journal=Scand J Urol Nephrol | year= 2012 | volume= 46 | issue= 1 | pages= 70-2 | pmid=21879805 | doi=10.3109/00365599.2011.609834 | pmc= | url=https://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=21879805 }} </ref>
| |
| |Free in the lumen of [[cecum]], [[appendix]], adjacent [[colon]]
| |
| |
| |
| * [[Albendazole]]
| |
| * [[Mebendazole]]
| |
| * [[Pyrantel pamoate]]
| |
| * [[Ivermectin]]
| |
| * [[Levamisole]]
| |
| * [[Piperazine]]
| |
| |}
| |
|
| |
|
| ==[[Strongyloidiasis epidemiology and demographics|Epidemiology and Demographics]]== | | ==[[Strongyloidiasis epidemiology and demographics|Epidemiology and Demographics]]== |