Schistosomiasis: Difference between revisions
Hardik Patel (talk | contribs) |
Hardik Patel (talk | contribs) |
||
| Line 16: | Line 16: | ||
{{CMG}} | {{CMG}} | ||
==Types== | ==Types== | ||
Revision as of 20:19, 10 October 2012
| Schistosomiasis | |
 | |
|---|---|
| Skin vesicles created by the penetration of Schistosoma. Source: CDC | |
| ICD-10 | B65 |
| ICD-9 | 120 |
| MeSH | D012552 |
|
WikiDoc Resources for Schistosomiasis |
|
Articles |
|---|
|
Most recent articles on Schistosomiasis Most cited articles on Schistosomiasis |
|
Media |
|
Powerpoint slides on Schistosomiasis |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Schistosomiasis at Clinical Trials.gov Trial results on Schistosomiasis Clinical Trials on Schistosomiasis at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Schistosomiasis NICE Guidance on Schistosomiasis
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Schistosomiasis Discussion groups on Schistosomiasis Patient Handouts on Schistosomiasis Directions to Hospitals Treating Schistosomiasis Risk calculators and risk factors for Schistosomiasis
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Schistosomiasis |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Types
There are five species of flatworms that cause schistosomiasis. Each causes a different clinical presentation of the disease. Schistosomiasis may localize in different parts of the body, and its localization determines its particular clinical profile.
- Schistosoma mansoni (ICD-10 B65.1) and Schistosoma intercalatum (B65.8) cause intestinal schistosomiasis
- Schistosoma haematobium (B65.0) causes urinary schistosomiasis
- Schistosoma japonicum (B65.2) and Schistosoma mekongi (B65.8) cause Asian intestinal schistosomiasis
Geographical distribution and epidemiology
The disease is found in tropical countries in Africa, Caribbean, eastern South America, east Asia and in the Middle East. Schistosoma mansoni is found in parts of South America and the Caribbean, Africa, and the Middle East; S. haematobium in Africa and the Middle East; and S. japonicum in the Far East. S. mekongi and S. intercalatum are found focally in Southeast Asia and central West Africa, respectively.
An estimated 207 million people have the disease, 120 million symptomatic. A few countries have eradicated the disease, and many more are working towards it. The World Health Organization is promoting efforts working towards this goal. In some cases, urbanization, pollution, and/or consequent destruction of snail habitat has reduced exposure, with a subsequent decrease in new infections. The most common way of getting schistosomiasis in developing countries is by wading or swimming in lakes, ponds and other bodies of water which are infested with the snails (usually of the Biomphalaria, Bulinus, or Oncomelania genus) that are the natural reservoirs of the Schistosoma pathogen.
Life cycle

Schistosomes have a typical trematode vertebrate-invertebrate lifecycle, with humans being the definitive host. The life cycles of all five human schistosomes are broadly similar: parasite eggs are released into the environment from infected individuals, hatching on contact with fresh water to release the free-swimming miracidium. Miracidia infect fresh-water snails by penetrating the snail's foot. After infection, close to the site of penetration, the miracidium transforms into a primary (mother) sporocyst. Germ cells within the primary sporocyst will then begin dividing to produce secondary (daughter) sporocysts, which migrate to the snail's hepatopancreas. Once at the hepatopancreas, germ cells within the secondary sporocyst begin to divide again, this time producing thousands of new parasites, known as cercariae, which are the larvae capable of infecting mammals.
Cercariae emerge daily from the snail host in a circadian rhythm, dependent on ambient temperature and light. Young cercariae are highly motile, alternating between vigorous upward movement and sinking to maintain their position in the water. Cercarial activity is particularly stimulated by water turbulence, by shadows and by chemicals found on human skin. Penetration of the human skin occurs after the cercaria have attached to and explored the skin. The parasite secretes enzymes that break down the skin's protein to enable penetration of the cercarial head through the skin. As the cercaria penetrates the skin it transforms into a migrating schistosomulum stage.
The newly transformed schistosomulum may remain in the skin for 2 days before locating a post-capillary venule; from here the schistosomulum travels to the lungs where it undergoes further developmental changes necessary for subsequent migration to the liver. Eight to ten days after penetration of the skin, the parasite migrates to the liver sinusoids. S. japonicum migrates more quickly than S. mansoni, and usually reaches the liver within 8 days of penetration. Juvenile S. mansoni and S. japonicum worms develop an oral sucker after arriving at the liver, and it is during this period that the parasite begins to feed on red blood cells. The nearly-mature worms pair, with the longer female worm residing in the gynaecophoric channel of the male. Adult worms are about 10 mm long. Worm pairs of S. mansoni and S. japonicum relocate to the mesenteric or rectal veins. S. haematobium schistosomula ultimately migrate from the liver to the perivesical venous plexus of the bladder, ureters, and kidneys through the hemorrhoidal plexus.
Parasites reach maturity in six to eight weeks, at which time they begin to produce eggs. Adult S. mansoni pairs residing in the mesenteric vessels may produce up to 300 eggs per day during their reproductive lives. S. japonicum may produce up to 3000 eggs per day. Many of the eggs pass through the walls of the blood vessels, and through the intestinal wall, to be passed out of the body in faeces. S. haematobium eggs pass through the ureteral or bladder wall and into the urine. Only mature eggs are capable of crossing into the digestive tract, possibly through the release of proteolytic enzymes, but also as a function of host immune response, which fosters local tissue ulceration. Up to half the eggs released by the worm pairs become trapped in the mesenteric veins, or will be washed back into the liver, where they will become lodged. Worm pairs can live in the body for an average of four and a half years, but may persist up to 20 years.
Trapped eggs mature normally, secreting antigens that elicit a vigorous immune response. The eggs themselves do not damage the body. Rather it is the cellular infiltration resultant from the immune response that causes the pathology classically associated with schistosomiasis.
Pathology
Above all, schistosomiasis is a chronic disease. Pathology of S. mansoni and S. japonicum schistosomiasis includes: Katayama fever, hepatic perisinusoidal egg granulomas, Symmers’ pipe stem periportal fibrosis, portal hypertension, and occasional embolic egg granulomas in brain or spinal cord. Pathology of S. haematobium schistosomiasis includes: hematuria, scarring, calcification, squamous cell carcinoma, and occasional embolic egg granulomas in brain or spinal cord. Bladder Cancer diagnosis and mortality are generally elevated in affected areas.
Laboratory diagnosis
Microscopic identification of eggs in stool or urine is the most practical method for diagnosis. The stool exam is the more common of the two. For the measurement of eggs in the feces of presenting patients the scientific unit used is epg or eggs per gram. Stool examination should be performed when infection with S. mansoni or S. japonicum is suspected, and urine examination should be performed if S. haematobium is suspected.
Eggs can be present in the stool in infections with all Schistosoma species. The examination can be performed on a simple smear (1 to 2 mg of fecal material). Since eggs may be passed intermittently or in small amounts, their detection will be enhanced by repeated examinations and/or concentration procedures (such as the formalin-ethyl acetate technique). In addition, for field surveys and investigational purposes, the egg output can be quantified by using the Kato-Katz technique (20 to 50 mg of fecal material) or the Ritchie technique.
Eggs can be found in the urine in infections with (recommended time for collection: between noon and 3 PM) S. japonicum' and with S. intercalatum. Detection will be enhanced by centrifugation and examination of the sediment. Quantification is possible by using filtration through a nucleopore membrane of a standard volume of urine followed by egg counts on the membrane. Investigation of S. haematobium should also include a pelvic x-ray as bladder wall calcificaition is highly characteristic of chronic infection.
Recently a field evaluation of a novel handheld microscope was undertaken in Uganda for the diagnosis of intestinal schistosomiasis by a team led by Dr. Russell Stothard who heads the Schistosomiasis Control Iniative at the Natural History Museum, London. His report abstract may be found here: [2]
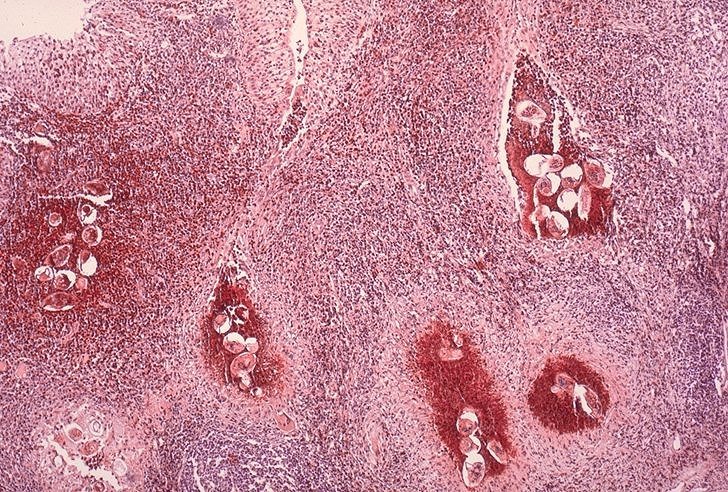
Tissue biopsy (rectal biopsy for all species and biopsy of the bladder for S. haematobium) may demonstrate eggs when stool or urine examinations are negative.
The eggs of S. haematobium are ellipsoidal with a terminal spine, S. mansoni eggs are also ellipsoidal but with a lateral spine, S. japonicum eggs are spheroidal with a small knob.
Antibody detection can be useful in both clinical management and for epidemiologic surveys.
Treatment
Schistosomiasis is readily treated using a single oral dose of the drug Praziquantel. While Praziquantel is safe and highly effective in curing an infected patient, it does not prevent re-infection by cercariae and is thus not an optimum treatment for people living in endemic areas. As with other major parasitic diseases, there is ongoing and extensive research into developing a vaccine that will prevent the parasite from completing its life cycle in humans.
Antimony has been used in the past to treat the disease. In low doses, this toxic metalloid bonds to sulfur atoms in enzymes used by the parasite and kills it without harming the host. This treatment is not referred to in present-day peer-review scholarship; Praziquantel is universally used. Outside of the US, there is a second drug available for treating Schistosoma mansoni (exclusively) called Oxamniquine.
Mirazid, a new Egyptian drug, is under investigation for oral treatment of the disease.
Experiments have shown medicinal Castor oil as an oral anti-penetration agent to prevent Schistosomiasis and that praziquantel's effectiveness depended upon the vehicle used to administer the drug (e.g., Cremophor / Castor oil).[1]
Additionally Dr Chidzere of Zimbabwe researched the Gopo Berry (Phytolacca dodecandra) during the 1980's and found that the Gopo Berry could be used in the control of the freshwater snails which carry the bilharzia disease (Schistosomiasis parasite). Dr Chidzere in his interview to Andrew Blake (1989) reported concerns of muti-national chemical companies keen to rubbish the Gopu Berry alternative for snail control [2]. Reputedly Gopo Berries from hotter Ethiopia climates yield the best results. Later studies were between 1993-95 by the Danish Research Network for international health. [3]
Prevention through good design
The main focus of prevention is eliminating the water-borne snails which are natural reservoirs for the disease. This is usually done by identifying bodies of water, such as lakes, ponds, etc., which are infested, forbidding or warning against swimming and adding niclosamide, acrolein, copper sulfate, etc., to the water in order to kill the snails.
Unfortunately for many years from the 1950s onwards, despite the efforts of some clinicians to get civil engineers to take it into account in their designs, civil engineeers built vast dam and irrigation schemes, oblivious of the fact that they would cause a massive rise in water-borne infections from schistosomiasis, even though with a little care the schemes could have been designed to minimise such effects, the detailed specifications having been laid out in various UN documents since the 1950s. Irrigation schemes can be designed to make it hard for the snails to colonise the water, and to reduce the contact with the local population. [4]
Failure for engineers to take this into account is an interesting example of the Relevance Paradox and is a good example of the failure of formal education and information systems to transmit tacit knowledge.
Prevention and hygiene
Prevention is best accomplished by eliminating the water-dwelling snails which are the natural reservoir of the disease. Acrolein, copper sulfate, and niclosamide can be used for this purpose. Recent studies have suggested that snail populations can be controlled by the introduction or augmentation of existing crayfish populations; as with all ecological interventions, however, this technique must be approached with caution.
Individuals can guard against schistosomiasis infection by avoiding bodies of water known or likely to harbor the carrier snails.
In 1989, Aklilu Lemma and Legesse Wolde-Yohannes received the Right Livelihood Award for their research on the sapindus-Plant (Phytolacca dodecandra), as a preventative measure for the disease.
Histopathology: Rectum, Schistosomiasis
{{#ev:youtube|9VpqxnPRvL8}}
See also
References
- ↑ "Schistosoma mansoni: experimental chemoprophylaxis in mice using oral anti-penetration agents". pubmed. Retrieved 2007-01-25.
- ↑ The Gopu Berry p33. Part 4 School Journal number.2 1989 Dept of Education Wellington N.Z
- ↑ http://enrecahealth.ku.dk/postgrad_dbl_en/chihaka_abs/
- ↑ Charnock, Anne (1980) Taking Bilharziasis out of the irrigation equation. New Civil Engineer, 7 August. 1980 Bilharzia caused by poor civil engineering design due to ignorance of cause and prevention
External links
- World Health Organization Partners for Parasite Control website
- World Health Organization fact sheet on the disease
- Wellcome animation of the life cycle of the parasite
- Schistosomiasis Control Initiative
- CONTRAST, a research project on optimized schistosomiasis control in Sub-saharan Africa
- World Health Organization Tropical Disease Research programme
- Cambridge University Schistosomiasis Research Group
- York University Schistosomiasis Research Group
- Schistosomiasis (Bilharzia) Control and Prevention: The Carter Center Schistosomiasis Control Program
- Links to Schistosomiasis pictures (Hardin MD/Univ of Iowa)
- FIOCRUZ - Schistomiasis Research Group
- Sandler Center for Basic Research in Parasitic Diseases, University of California San Francisco
- Vacine developed in Queensland, Australia
- DBL - Centre for Health Research and Development
- 10. Charnock, Anne (1980) Taking Bilharziasis out of the irrigation equation. New Civil Engineer, 7 August. Bilharzia caused by poor civil engineering design due to ignorance of cause and prevention.
Template:Link FA
Template:Helminthiases
ar:بلهارسيا
de:Schistosomiasis
eo:Helika febro
it:Schistosomiasi
lt:Šistosomozė
nl:Schistosomiasis
fi:Skistosomiaasi
sv:Snäckfeber