Clindamycin hydrochloride (oral): Difference between revisions
Kiran Singh (talk | contribs) No edit summary |
Kiran Singh (talk | contribs) No edit summary |
||
| Line 5: | Line 5: | ||
|drugClass=antibiotic | |drugClass=antibiotic | ||
|indicationType=treatment | |indicationType=treatment | ||
|indication=[[empyema]], anaerobic [[pneumonitis]], and [[lung abscess]]; serious skin and [[soft tissue infections]]; [[septicemia]]; intra-abdominal infections such as [[peritonitis]] and | |indication=[[empyema]], anaerobic [[pneumonitis]], and [[lung abscess]]; serious skin and [[soft tissue infections]]; [[septicemia]]; intra-abdominal infections such as [[peritonitis]] and intra-abdominal abscess | ||
|hasBlackBoxWarning=Yes | |hasBlackBoxWarning=Yes | ||
|adverseReactions=[[abdominal pain]], [[pseudomembranous colitis]], [[esophagitis]], [[nausea]], [[vomiting]], and [[diarrhea]] | |adverseReactions=[[abdominal pain]], [[pseudomembranous colitis]], [[esophagitis]], [[nausea]], [[vomiting]], and [[diarrhea]] | ||
Revision as of 14:27, 16 December 2014
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Kiran Singh, M.D. [2]
Disclaimer
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Black Box Warning
|
WARNING
See full prescribing information for complete Boxed Warning.
Clostridium difficile associated diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including CLEOCIN HCl and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon, leading to overgrowth of C. difficle.
Because CLEOCIN HCl therapy has been associated with severe colitis which may end fatally, it should be reserved for serious infections where less toxic antimicrobial agents are inappropriate, as described in the INDICATIONS AND USAGE section. It should not be used in patients with nonbacterial infections such as most upper respiratory tract infections. C. difficile produces toxins A and B, which contribute to the development of CDAD. Hypertoxin producing strains of C. difficile cause increased morbidity and mortality, as these infections can be refractory to antimicrobial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibiotic use. Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents. If CDAD is suspected or confirmed, ongoing antibiotic use not directed against C. difficile may need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibiotic treatment of C. difficile, and surgical evaluation should be instituted as clinically indicated. |
Overview
Clindamycin hydrochloride (oral) is an antibiotic that is FDA approved for the treatment of empyema, anaerobic pneumonitis, and lung abscess; serious skin and soft tissue infections; septicemia; intra-abdominal infections such as peritonitis and intra-abdominal abscess. There is a Black Box Warning for this drug as shown here. Common adverse reactions include abdominal pain, pseudomembranous colitis, esophagitis, nausea, vomiting, and diarrhea.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Indications
- Clindamycin is indicated in the treatment of serious infections caused by susceptible anaerobic bacteria.
- Clindamycin is also indicated in the treatment of serious infections due to susceptible strains of streptococci, pneumococci, and staphylococci. Its use should be reserved for penicillin-allergic patients or other patients for whom, in the judgment of the physician, a penicillin is inappropriate. Because of the risk of colitis, as described in the WARNING box, before selecting clindamycin, the physician should consider the nature of the infection and the suitability of less toxic alternatives (e.g., erythromycin).
- Anaerobes: Serious respiratory tract infections such as empyema, anaerobic pneumonitis, and lung abscess; serious skin and soft tissue infections; septicemia; intra-abdominal infections such as peritonitis and intra-abdominal abscess (typically resulting from anaerobic organisms resident in the normal gastrointestinal tract); infections of the female pelvis and genital tract such as endometritis, nongonococcal tubo-ovarian abscess, pelvic cellulitis, and postsurgical vaginal cuff infection.
- Streptococci: Serious respiratory tract infections; serious skin and soft tissue infections.
- Staphylococci: Serious respiratory tract infections; serious skin and soft tissue infections.
- Pneumococci: Serious respiratory tract infections.
- Bacteriologic studies should be performed to determine the causative organisms and their susceptibility to clindamycin.
- To reduce the development of drug-resistant bacteria and maintain the effectiveness of CLEOCIN HCl and other antibacterial drugs, CLEOCIN HCl should be used only to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
Dosage
- If significant diarrhea occurs during therapy, this antibiotic should be discontinued.
- Adults: Serious infections – 150 to 300 mg every 6 hours. More severe infections – 300 to 450 mg every 6 hours. Pediatric Patients: Serious infections – 8 to 16 mg/kg/day (4 to 8 mg/lb/day) divided into three or four equal doses. More severe infections – 16 to 20 mg/kg/day (8 to 10 mg/lb/day) divided into three or four equal doses.
- To avoid the possibility of esophageal irritation, CLEOCIN HCl Capsules should be taken with a full glass of water.
- Serious infections due to anaerobic bacteria are usually treated with CLEOCIN PHOSPHATE® Sterile Solution. However, in clinically appropriate circumstances, the physician may elect to initiate treatment or continue treatment with CLEOCIN HCl Capsules.
- In cases of β-hemolytic streptococcal infections, treatment should continue for at least 10 days.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
Indications and Dosing
- Due to risk of severe colitis, reserve use of clindamycin for serious infections when other options are inappropriate.
- Babesiosis: 600 mg ORALLY every 8 hours plus quinine 650 mg ORALLY every 6 to 8 hours for 7 to 10 days.
- Bacterial endocarditis; Prophylaxis: (high-risk patients; dental, respiratory, or infected skin/skin structure or musculoskeletal tissue procedures) 600 mg ORALLY 30 to 60 minutes prior to procedure.
- Bacterial infectious disease (Severe), Susceptible infections due to anaerobic organisms, staphylococci, streptococci, pneumococci: 150 to 300 mg ORALLY every 6 hours; use 300 to 450 mg ORALLY every 6 hours for more severe infections (manufacturer dosing); (MRSA-associated) 300 to 450 mg ORALLY 3 times daily for cellulitis and 600 mg ORALLY 3 times daily for complicated skin and soft tissue infections (cSSTIs), pneumonia, and bone and joint infections; duration is 5 to 10 days for cellulitis, 7 to 14 days for hospital-associated cSSTIs, 7 to 21 days for pneumonia, 8 weeks for osteomyelitis, and 3 to 4 weeks for septic arthritis (guideline dosing).
- Bacterial vaginosis: 300 mg ORALLY twice daily for 7 days.
- HIV infection - Pneumocystis pneumonia: 300 to 450 mg ORALLY every 6 to 8 hours, in combination with primaquine 15 to 30 mg (base) ORALLY once daily for 21 days.
- HIV infection - Toxoplasmosis: (encephalitis) alternative therapy, 600 mg ORALLY every 6 hours, in combination with pyrimethamine 200 mg ORALLY for 1 dose, then 50 mg (less than 60 kg) or 75 mg (60 kg or greater) ORALLY daily plus leucovorin 10 to 25 mg (can increase to 50 mg) ORALLY daily for at least 6 weeks.
- HIV infection - Toxoplasmosis; Prophylaxis: secondary prophylaxis (alternative regimen), 600 mg ORALLY every 8 hours, in combination with pyrimethamine 25 to 50 mg ORALLY daily plus leucovorin 10 to 25 mg ORALLY daily.
- Impetigo: (Staphylococcus and Streptococcus species) 300 to 400 mg ORALLY 4 times daily for 7 days, depending on clinical response (guideline dosing).
- Infection of skin AND/OR subcutaneous tissue (Severe): 150 to 300 mg ORALLY every 6 hours; use 300 to 450 mg ORALLY every 6 hours for more severe infections (manufacturer dose) [4]; MRSA-associated, 300 mg to 450 mg ORALLY 3 times daily for 5 to 10 days (purulent and nonpurulent cellulitis) or 600 mg ORALLY 3 times daily (complicated skin and soft tissue infections [cSSTIs]), generally for 7 to 14 days for hospital-associated cSSTIs; individualize to patient response.
- Infection of skin AND/OR subcutaneous tissue (Severe): Methicillin-susceptible Staphylococcus aureus or MRSA, 300 to 450 mg ORALLY 3 or [5] 4 times daily [8]; for purulent or nonpurulent cellulitis continue treatment for 5 to 10 days.
- Infection of skin AND/OR subcutaneous tissue (Severe): MRSA, complicated skin and soft tissue infections (cSSTIs), 600 mg ORALLY 3 times daily, generally for 7 to 14 days for hospital-associated cSSTIs; individualize to patient response (guideline dose).
- Infectious disease of abdomen: 150 to 300 mg ORALLY every 6 hours; use 300 to 450 mg ORALLY every 6 hours for more severe infections.
- Lower respiratory tract infection (Severe), Empyema, abscess, pneumonitis: 150 to 300 mg ORALLY every 6 hours; use 300 to 450 mg ORALLY every 6 hours for more severe infections.
- Pelvic inflammatory disease: 900 mg IV every 8 hours plus gentamicin (IV or IM) loading dose of 2 mg/kg, followed by 1.5 mg/kg every 8 hours (single daily dosing of gentamicin 3 to 5 mg/kg may be substituted); discontinue IV/IM therapy 24 hours after clinical improvement and continue on clindamycin 450 mg ORALLY 4 times daily or doxycycline 100 mg ORALLY twice daily to complete a total of 14 days of therapy (guideline dosing).
- Pelvic inflammatory disease: 150 to 300 mg ORALLY every 6 hours; use 300 to 450 mg ORALLY every 6 hours for more severe infections (manufacturer dosing) .
- Septicemia: 150 to 300 mg ORALLY every 6 hours; use 300 to 450 mg ORALLY every 6 hours for more severe infections.
- Streptococcal pharyngitis: (penicillin-allergic patients) 20 mg/kg/day ORALLY in 3 divided doses (MAX 1.8 g/day).
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Clindamycin in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
There is limited information regarding Clindamycin hydrochloride (oral) FDA-Labeled Indications and Dosage (Pediatric) in the drug label.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
Indications and Dosage
- Due to risk of severe colitis, reserve use of clindamycin for serious infections when other options are inappropriate.
- Acute otitis media: 30 to 40 mg/kg/day ORALLY in 3 divided doses for 5 to 7 days (6 years or older with mild to moderate illness), 7 days (2 to 5 years with mild to moderate illness), or 10 days (younger than 2 years or with severe illness).
- Babesiosis: 7 to 10 mg/kg ORALLY every 6 to 8 hours (MAX 600 mg/dose) plus quinine 8 mg/kg ORALLY every 8 hours (MAX 650 mg/dose) for 7 to 10 days.
- Bacterial endocarditis; Prophylaxis: (high-risk patients; dental, respiratory, or infected skin/skin structure or musculoskeletal tissue procedures) 20 mg/kg ORALLY 30 to 60 minutes prior to procedure.
- Bacterial infectious disease (Severe), Susceptible infections due to anaerobic organisms, staphylococci, streptococci, pneumococci: 8 to 16 mg/kg/day ORALLY divided every 6 to 8 hours; use 16 to 20 mg/kg/day ORALLY divided every 6 to 8 hours for more severe infections; (MRSA-associated infections) 40 mg/kg/day orally divided every 6 to 8 hours (guideline dosing).
- HIV infection - Toxoplasmosis: (congenital toxoplasmosis) 5 to 7.5 mg/kg/dose (MAX 600 mg/dose) ORALLY 4 times daily plus pyrimethamine 2 mg/kg ORALLY once daily for 2 days, then 1 mg/kg ORALLY once daily for 2 to 6 months, then 1 mg/kg ORALLY 3 times weekly plus leucovorin 10 mg ORALLY or IM with each dose of pyrimethamine; total treatment duration is 12 months.
- HIV infection - Toxoplasmosis: (acquired toxoplasmosis) 5 to 7.5 mg/kg/dose (MAX 600 mg/dose) ORALLY 4 times daily plus pyrimethamine 2 mg/kg (MAX 50 mg) ORALLY once daily for 3 days, then 1 mg/kg (MAX 25 mg) ORALLY once daily plus leucovorin 10 to 25 mg ORALLY daily; continue for at least 6 weeks, followed by secondary prophylaxis.
- HIV infection - Toxoplasmosis; Prophylaxis: secondary prophylaxis (alternative regimen), 20 to 30 mg/kg/day ORALLY divided into 3 to 4 doses plus pyrimethamine 1 mg/kg or 15 mg/m(2) (MAX 25 mg) ORALLY daily plus leucovorin 5 mg ORALLY every 3 days.
- Impetigo: (Staphylococcus and Streptococcus species) 20 mg/kg/day ORALLY in 3 divided doses for 7 days, depending on clinical response (guideline dosing).
- Infection of skin AND/OR subcutaneous tissue (Severe): 8 to 16 mg/kg/day ORALLY divided every 6 to 8 hours; use 16 to 20 mg/kg/day ORALLY divided every 6 to 8 hours for more severe infections (manufacturer dose).
- Infection of skin AND/OR subcutaneous tissue (Severe): Methicillin-susceptible Staphylococcus aureus, 25 to 30 mg/kg/day ORALLY in 3 divided doses (guideline dose).
- Infection of skin AND/OR subcutaneous tissue (Severe): MRSA, 30 to [8] 40 mg/kg/day [8][5] ORALLY in 3 or 4 divided doses (guideline dose).
- Infectious disease of abdomen: 8 to 16 mg/kg/day ORALLY divided every 6 to 8 hours; use 16 to 20 mg/kg/day ORALLY divided every 6 to 8 hours for more severe infections .
- Lower respiratory tract infection (Severe), Empyema, abscess, pneumonitis: 8 to 16 mg/kg/day ORALLY divided every 6 to 8 hours; use 16 to 20 mg/kg/day ORALLY divided every 6 to 8 hours for more severe infections.
- Lower respiratory tract infection (Severe), Empyema, abscess, pneumonitis: community-acquired pneumonia (older than 3 months) 30 to 40 mg/kg/day ORALLY in 3 to 4 divided doses (guideline dosing).
- Pelvic inflammatory disease: 8 to 16 mg/kg/day ORALLY divided every 6 to 8 hours; use 16 to 20 mg/kg/day ORALLY divided every 6 to 8 hours for more severe infections.
- Septicemia: 8 to 16 mg/kg/day ORALLY divided every 6 to 8 hours; 16 to 20 mg/kg/day ORALLY divided every 6 to 8 hours for more severe infections.
Streptococcal pharyngitis: (penicillin-allergic patients) 20 mg/kg/day ORALLY in 3 divided doses (MAX 1.8 g/day)
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Clindamycin in pediatric patients.
Contraindications
CLEOCIN HCl is contraindicated in individuals with a history of hypersensitivity to preparations containing clindamycin or lincomycin.
Warnings
|
WARNING
See full prescribing information for complete Boxed Warning.
Clostridium difficile associated diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including CLEOCIN HCl and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon, leading to overgrowth of C. difficle.
Because CLEOCIN HCl therapy has been associated with severe colitis which may end fatally, it should be reserved for serious infections where less toxic antimicrobial agents are inappropriate, as described in the INDICATIONS AND USAGE section. It should not be used in patients with nonbacterial infections such as most upper respiratory tract infections. C. difficile produces toxins A and B, which contribute to the development of CDAD. Hypertoxin producing strains of C. difficile cause increased morbidity and mortality, as these infections can be refractory to antimicrobial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibiotic use. Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents. If CDAD is suspected or confirmed, ongoing antibiotic use not directed against C. difficile may need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibiotic treatment of C. difficile, and surgical evaluation should be instituted as clinically indicated. |
There is limited information regarding Clindamycin hydrochloride (oral) Warnings' in the drug label.
Adverse Reactions
Clinical Trials Experience
The following reactions have been reported with the use of clindamycin.
Gastrointestinal: Abdominal pain, pseudomembranous colitis, esophagitis, nausea, vomiting, and diarrhea . The onset of pseudomembranous colitis symptoms may occur during or after antibacterial treatment . Esophageal ulcer has been reported.
Hypersensitivity Reactions: Generalized mild to moderate morbilliform-like (maculopapular) skin rashes are the most frequently reported adverse reactions. Vesiculobullous rashes, as well as urticaria, have been observed during drug therapy. Severe skin reactions such as toxic epidermal necrolysis, some with fatal outcome, have been reported . Cases of acute generalized exanthematous pustulosis (AGEP), erythema multiforme, some resembling Stevens-Johnson syndrome, and anaphylactoid reactions have also been reported.
Skin and Mucous Membranes: Pruritus, vaginitis, and rare instances of exfoliative dermatitis have been reported.
Liver: Jaundice and abnormalities in liver function tests have been observed during clindamycin therapy.
Renal: Although no direct relationship of clindamycin to renal damage has been established, renal dysfunction as evidenced by azotemia , oliguria, and/or proteinuria has been observed.
Hematopoietic: Transient neutropenia (leukopenia) and eosinophilia have been reported. Reports of agranulocytosis and thrombocytopenia have been made. No direct etiologic relationship to concurrent clindamycin therapy could be made in any of the foregoing.
Immune System: Drug reaction with eosinophilia and systemic symptoms (DRESS) cases have been reported.
Musculoskeletal: Cases of polyarthritis have been reported.
Postmarketing Experience
There is limited information regarding Clindamycin hydrochloride (oral) Postmarketing Experience in the drug label.
Drug Interactions
There is limited information regarding Clindamycin hydrochloride (oral) Drug Interactions in the drug label.
Use in Specific Populations
Pregnancy
Pregnancy Category (FDA):
There is no FDA guidance on usage of Clindamycin hydrochloride (oral) in women who are pregnant.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Clindamycin hydrochloride (oral) in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Clindamycin hydrochloride (oral) during labor and delivery.
Nursing Mothers
There is no FDA guidance on the use of Clindamycin hydrochloride (oral) in women who are nursing.
Pediatric Use
There is no FDA guidance on the use of Clindamycin hydrochloride (oral) in pediatric settings.
Geriatic Use
There is no FDA guidance on the use of Clindamycin hydrochloride (oral) in geriatric settings.
Gender
There is no FDA guidance on the use of Clindamycin hydrochloride (oral) with respect to specific gender populations.
Race
There is no FDA guidance on the use of Clindamycin hydrochloride (oral) with respect to specific racial populations.
Renal Impairment
There is no FDA guidance on the use of Clindamycin hydrochloride (oral) in patients with renal impairment.
Hepatic Impairment
There is no FDA guidance on the use of Clindamycin hydrochloride (oral) in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Clindamycin hydrochloride (oral) in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Clindamycin hydrochloride (oral) in patients who are immunocompromised.
Administration and Monitoring
Administration
There is limited information regarding Clindamycin hydrochloride (oral) Administration in the drug label.
Monitoring
There is limited information regarding Clindamycin hydrochloride (oral) Monitoring in the drug label.
IV Compatibility
There is limited information regarding the compatibility of Clindamycin hydrochloride (oral) and IV administrations.
Overdosage
- Significant mortality was observed in mice at an intravenous dose of 855 mg/kg and in rats at an oral or subcutaneous dose of approximately 2618 mg/kg. In the mice, convulsions and depression were observed.
- Hemodialysis and peritoneal dialysis are not effective in removing clindamycin from the serum.
Pharmacology
Mechanism of Action
There is limited information regarding Clindamycin hydrochloride (oral) Mechanism of Action in the drug label.
Structure
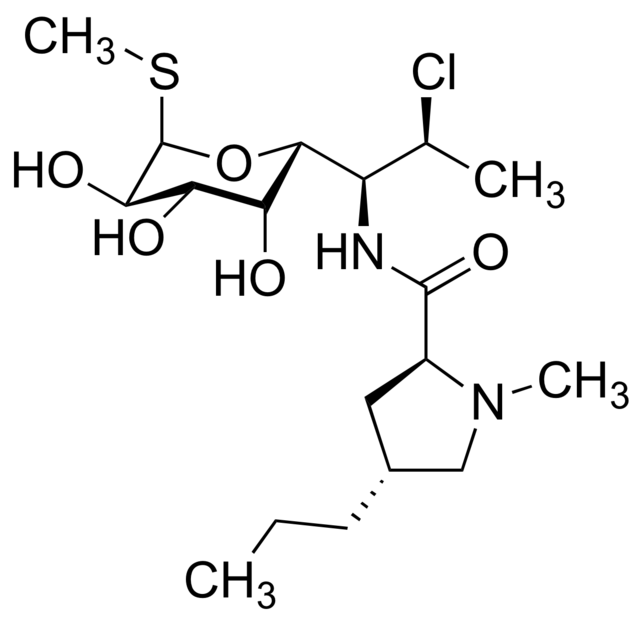
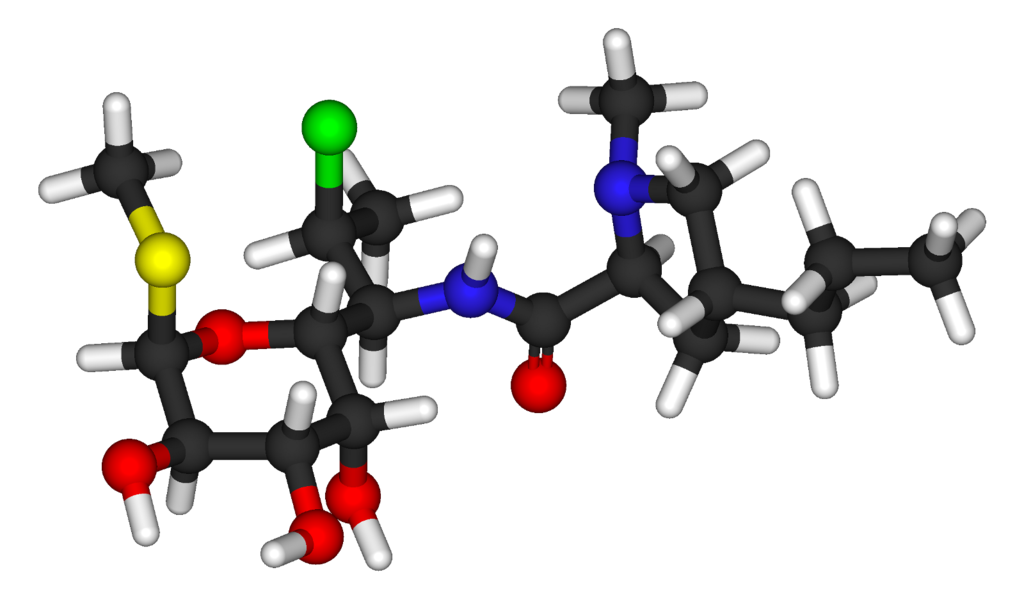
- Clindamycin hydrochloride is the hydrated hydrochloride salt of clindamycin. Clindamycin is a semisynthetic antibiotic produced by a 7(S)-chloro-substitution of the 7(R)-hydroxyl group of the parent compound lincomycin.
- CLEOCIN HCl Capsules contain clindamycin hydrochloride equivalent to 75 mg, 150 mg, or 300 mg of clindamycin.
- Inactive ingredients: 75 mg – corn starch, FD&C blue no. 1, FD&C yellow no. 5, gelatin, lactose, magnesium stearate, and talc; 150 mg – corn starch, FD&C blue no. 1, FD&C yellow no. 5, gelatin, lactose, magnesium stearate, talc and titanium dioxide; 300 mg – corn starch, FD&C blue no. 1, gelatin, lactose, magnesium stearate, talc, and titanium dioxide.
The structural formula is represented below:

- The chemical name for clindamycin hydrochloride is Methyl 7-chloro-6,7,8-trideoxy-6-(1-methyl-trans-4-propyl-L-2-pyrrolidinecarboxamido)-1-thio-L-threo-α-D-galacto-octopyranoside monohydrochloride.
Pharmacodynamics
There is limited information regarding Clindamycin hydrochloride (oral) Pharmacodynamics in the drug label.
Pharmacokinetics
Absorption
Serum level studies with a 150 mg oral dose of clindamycin hydrochloride in 24 normal adult volunteers showed that clindamycin was rapidly absorbed after oral administration. An average peak serum level of 2.50 mcg/mL was reached in 45 minutes; serum levels averaged 1.51 mcg/mL at 3 hours and 0.70 mcg/mL at 6 hours. Absorption of an oral dose is virtually complete (90%), and the concomitant administration of food does not appreciably modify the serum concentrations; serum levels have been uniform and predictable from person to person and dose to dose. Serum level studies following multiple doses of CLEOCIN HCl for up to 14 days show no evidence of accumulation or altered metabolism of drug. Doses of up to 2 grams of clindamycin per day for 14 days have been well tolerated by healthy volunteers, except that the incidence of gastrointestinal side effects is greater with the higher doses.
Distribution
Concentrations of clindamycin in the serum increased linearly with increased dose. Serum levels exceed the MIC (minimum inhibitory concentration) for most indicated organisms for at least six hours following administration of the usually recommended doses. Clindamycin is widely distributed in body fluids and tissues (including bones). No significant levels of clindamycin are attained in the cerebrospinal fluid, even in the presence of inflamed meninges.
Excretion
The average biological half-life is 2.4 hours. Approximately 10% of the bioactivity is excreted in the urine and 3.6% in the feces; the remainder is excreted as bioinactive metabolites.
Special Populations
Renal Impairment
Serum half-life of clindamycin is increased slightly in patients with markedly reduced renal function. Hemodialysis and peritoneal dialysis are not effective in removing clindamycin from the serum.
Use in Elderly
Pharmacokinetic studies in elderly volunteers (61–79 years) and younger adults (18–39 years) indicate that age alone does not alter clindamycin pharmacokinetics (clearance, elimination half-life, volume of distribution, and area under the serum concentration-time curve) after IV administration of clindamycin phosphate. After oral administration of clindamycin hydrochloride, elimination half-life is increased to approximately 4.0 hours (range 3.4–5.1 h) in the elderly compared to 3.2 hours (range 2.1 – 4.2 h) in younger adults. The extent of absorption, however, is not different between age groups and no dosage alteration is necessary for the elderly with normal hepatic function and normal (age-adjusted) renal function1.
Nonclinical Toxicology
There is limited information regarding Clindamycin hydrochloride (oral) Nonclinical Toxicology in the drug label.
Clinical Studies
There is limited information regarding Clindamycin hydrochloride (oral) Clinical Studies in the drug label.
How Supplied
CLEOCIN HCl Capsules are available in the following strengths, colors and sizes:
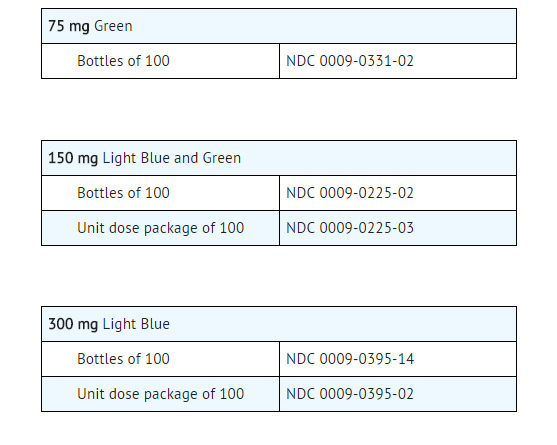
Storage
Store at controlled room temperature 20° to 25° C (68° to 77° F)
Images
Drug Images
{{#ask: Page Name::Clindamycin hydrochloride (oral) |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Clindamycin hydrochloride (oral) |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
There is limited information regarding Clindamycin hydrochloride (oral) Patient Counseling Information in the drug label.
Precautions with Alcohol
Alcohol-Clindamycin interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
There is limited information regarding Clindamycin hydrochloride (oral) Brand Names in the drug label.
Look-Alike Drug Names
There is limited information regarding Clindamycin hydrochloride (oral) Look-Alike Drug Names in the drug label.
Drug Shortage Status
Price
References
The contents of this FDA label are provided by the National Library of Medicine.