Astrocytoma CT: Difference between revisions
Jump to navigation
Jump to search
| Line 18: | Line 18: | ||
* Cystic or [[fluid]] attenuation components are also encountered, particularly in gemistocytic and protoplasmic varieties. | * Cystic or [[fluid]] attenuation components are also encountered, particularly in gemistocytic and protoplasmic varieties. | ||
====Fibrillary Astrocytoma<ref name=Radiopaedia2-2015>{{cite web | title = Fibrillary Astrocytoma [Dr Frank Gaillard]| url = http://radiopaedia.org/articles/fibrillary-astrocytoma }}</ref>==== | ====Fibrillary Astrocytoma<ref name=Radiopaedia2-2015>{{cite web | title = Fibrillary Astrocytoma [Dr Frank Gaillard]| url = http://radiopaedia.org/articles/fibrillary-astrocytoma }}</ref>==== | ||
* Typically fibrillary low grade infiltrating astrocytomas appear as isodense or hypodense regions of positive [[mass]] effect, usually without any enhancement (in fact presence of enhancement would suggest high grade, e.g. WHO III or IV | * Typically fibrillary low grade infiltrating astrocytomas appear as isodense or hypodense regions of positive [[mass]] effect, usually without any enhancement (in fact presence of enhancement would suggest high grade, e.g. WHO III or IV tumors. | ||
* [[Calcification]] is not infrequently seen (10-20% of cases)1 but is more common in mixed [[tumor]]s relating to an oligodendroglial components (i.e. oligoastrocytoma). | * [[Calcification]] is not infrequently seen (10-20% of cases)1 but is more common in mixed [[tumor]]s relating to an oligodendroglial components (i.e. oligoastrocytoma). | ||
* Cystic or [[fluid]] attenuation components are also encountered although this is far more common in gemistocytic and protoplasmic variants. | * Cystic or [[fluid]] attenuation components are also encountered although this is far more common in gemistocytic and protoplasmic variants. | ||
====Protoplasmic Astrocytoma<ref name=Radiopaedia3-2015>{{cite web | title = Protoplasmic astrocytoma [Dr Yuranga Weerakkody and Dr Frank Gaillard]| url = http://radiopaedia.org/articles/protoplasmic-astrocytoma }}</ref>==== | ====Protoplasmic Astrocytoma<ref name=Radiopaedia3-2015>{{cite web | title = Protoplasmic astrocytoma [Dr Yuranga Weerakkody and Dr Frank Gaillard]| url = http://radiopaedia.org/articles/protoplasmic-astrocytoma }}</ref>==== | ||
* Typically protoplasmic low grade infiltrating astrocytomas appear as hypodense regions of positive [[mass]] effect, usually without any enhancement (in fact presence of enhancement would suggest high grade [[tumor]]s). Areas of the [[tumor]] appear of [[fluid]] attenuation, due to the aforementioned prominent mucinous microcystic component. | * Typically protoplasmic low grade infiltrating astrocytomas appear as hypodense regions of positive [[mass]] effect, usually without any enhancement (in fact presence of enhancement would suggest high grade [[tumor]]s). Areas of the [[tumor]] appear of [[fluid]] attenuation, due to the aforementioned prominent mucinous microcystic component. | ||
===Anaplastic astrocytomas<ref name=Radiopaedia 2015 Anaplastic astrocytoma>{{cite web | title = Anaplastic astrocytoma [Dr Bruno Di Muzio and Dr Frank Gaillard]| url = http://radiopaedia.org/articles/anaplastic-astrocytoma }}</ref>=== | ===Anaplastic astrocytomas<ref name=Radiopaedia 2015 Anaplastic astrocytoma>{{cite web | title = Anaplastic astrocytoma [Dr Bruno Di Muzio and Dr Frank Gaillard]| url = http://radiopaedia.org/articles/anaplastic-astrocytoma }}</ref>=== | ||
* [[CT]] appearances are intermediate, appearing as regions of low attenuation with positive [[mass]] effect. Enhancement is variable. | * [[CT]] appearances are intermediate, appearing as regions of low attenuation with positive [[mass]] effect. Enhancement is variable. | ||
Revision as of 17:33, 24 August 2015
|
Astrocytoma Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Study |
|
Astrocytoma CT On the Web |
|
American Roentgen Ray Society Images of Astrocytoma CT |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [2]; Associate Editor(s)-in-Chief: Ammu Susheela, M.D. [3]
Overview
On cranial CT, astrocytoma is characterized by isodense or hypodense regions of positive mass effect, often without any enhancement. Calcification and either cystic or fluid attenuation components are also encountered in CT depending on the type and grade of the tumor.
CT findings
- A Computed Tomography (CT) or Magnetic Resonance Imaging (MRI) scan is necessary to characterize the anatomy of this tumor (size, location, consistency).
- CT will usually show distortion of third and lateral ventricles with displacement of anterior and middle cerebral arteries.
- During a CT scan, x rays of the patient's brain are taken from many different directions. These are then combined by a computer, producing a cross-sectional image of the brain.
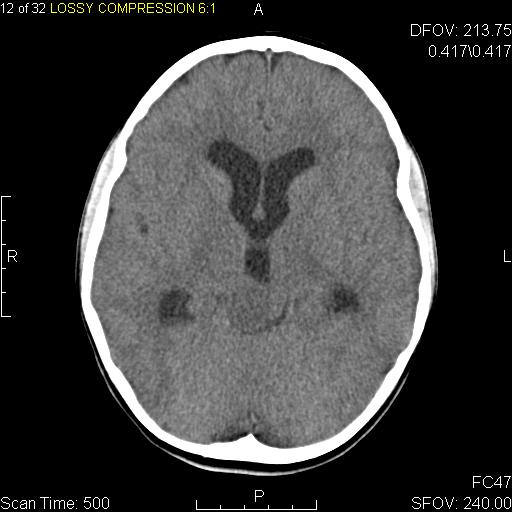 |
Low grade infiltrative astrocytoma[2]
- Typically low grade infiltrating astrocytomas appear as isodense or hypodense regions of positive mass effect, often without any enhancement (in fact presence of enhancement would suggest high tumors), although particularly gemistocytic astrocytomas can demonstrates wispy enhancement.
- Calcification is not seldom (10-20% of cases)1 and may be related to oligodendroglial components (i.e oligoastrocytoma).
- Cystic or fluid attenuation components are also encountered, particularly in gemistocytic and protoplasmic varieties.
Fibrillary Astrocytoma[3]
- Typically fibrillary low grade infiltrating astrocytomas appear as isodense or hypodense regions of positive mass effect, usually without any enhancement (in fact presence of enhancement would suggest high grade, e.g. WHO III or IV tumors.
- Calcification is not infrequently seen (10-20% of cases)1 but is more common in mixed tumors relating to an oligodendroglial components (i.e. oligoastrocytoma).
- Cystic or fluid attenuation components are also encountered although this is far more common in gemistocytic and protoplasmic variants.
Protoplasmic Astrocytoma[4]
- Typically protoplasmic low grade infiltrating astrocytomas appear as hypodense regions of positive mass effect, usually without any enhancement (in fact presence of enhancement would suggest high grade tumors). Areas of the tumor appear of fluid attenuation, due to the aforementioned prominent mucinous microcystic component.
Anaplastic astrocytomas
- CT appearances are intermediate, appearing as regions of low attenuation with positive mass effect. Enhancement is variable.
Subependymal Giant Cell Astrocytoma[5]
- The foramen of Monro is the classic location, and the tumor arises when a subependymal nodule transforms into subependymal giant cell astrocytoma over a period of time..
- Typically appears as an intraventricular mass near the foramen of Monro.
- They are usually larger than 1 cm.
- Lesions are iso- or slightly hypoattenuating to grey matter.
- Calcification is common and hemorrhage is possible
- Accompanying hydrocephalus may be present
- Often shows marked contrast enhancement (subependymal nodules also enhance)
Pleomorphic xanthoastrocytomas (PXA)[6]
- Pleomorphic xanthoastrocytomas are typically hypo or isodense and may be well or poorly demarcated, usually with little surrounding edema. Calcification is rare. Due to its superfical location it may cause scalloping of the overlying bone .[7]
- Often there is a cystic component (50-60%) with an enhancing mural nodule. Additionally they are one of the tumors that may exhibit a dural tail, which is reactive rather than due to direct dural invasion, which is rare .
References
- ↑ "Wikipedia".
- ↑ "Low grade infiltrative astrocytoma [Dr Bruno Di Muzio and Dr Frank Gaillard]".
- ↑ "Fibrillary Astrocytoma [Dr Frank Gaillard]".
- ↑ "Protoplasmic astrocytoma [Dr Yuranga Weerakkody and Dr Frank Gaillard]".
- ↑ "Subependymal giant cell astrocytoma [Dr Bruno Di Muzio and Dr Jeremy Jones]".
- ↑ "Pleomorphic xanthoastrocytomas [Dr Bruno Di Muzio and Dr Frank Gaillard]".
- ↑ Koeller KK, Rushing EJ (2004). "From the archives of the AFIP: pilocytic astrocytoma: radiologic-pathologic correlation". Radiographics. 24 (6): 1693–708. doi:10.1148/rg.246045146. PMID 15537977.