Angiodysplasia
| Angiodysplasia | |
 | |
|---|---|
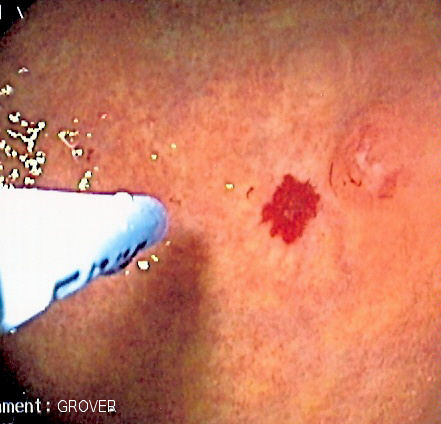
| An angiodysplasia in the colon being treated with argon plasma coagulation administered via probe through the colonoscope. The patient had multiple colonic angiodysplasiae in the setting of aortic stenosis. | |
| ICD-10 | K55.2 |
| ICD-9 | 569.84, 569.85 |
| DiseasesDB | 2963 |
| eMedicine | med/134 |
| MeSH | D016888 |
|
Angiodysplasia Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Angiodysplasia On the Web |
|
American Roentgen Ray Society Images of Angiodysplasia |
Synonyms and keywords: Colonic angiodysplasia; colonic arteriovenous malformation; vascular ectasia of the colon; angioectasia
Overview
In medicine (gastroenterology), angiodysplasia is a small vascular malformation of the gut. It is a common cause of otherwise unexplained gastrointestinal bleeding and anemia. Lesions are often multiple, and frequently involve the cecum or ascending colon, although they can occur at other places. Treatment may be with endoscopic interventions, medication, or occasionally surgery.
Signs and symptoms
Although some cases present with black, tarry stool (melena), the blood loss can be subtle, with the anemia symptoms predominating. Fecal occult blood testing is positive when bleeding is active. If bleeding is intermittent the test may be negative at times.
Diagnosis
Diagnosis of angiodysplasia is often accomplished with endoscopy, either colonoscopy or esophagogastroduodenoscopy (EGD). Although the lesions can be notoriously hard to find, the patient usually is diagnosed by endoscopy. A new technique, pill enteroscopy, has been a major advance in diagnosis, especially in the small bowel which is difficult to reach with traditional endoscopy. With this technique a pill that contains a video camera and radio transmitter is swallowed, and pictures of the small intestine are sent to a receiver worn by the patient.
Angiodysplasiae in the small bowel can also be diagnosed and treated with double-balloon enteroscopy, a technique involving a long endoscopic camera and overtube, both fitted with balloons, that allow the bowel to be accordioned over the camera.[1]
In cases with negative endoscopic findings and high clinical suspicion, selective angiography of the mesenteric arteries is sometimes necessary, but this allows for interventions at time of the procedure. An alternative is scintigraphy with red blood cells labeled with a radioactive marker; this shows the site of the bleeding on a gamma camera but tends to be unhelpful unless the bleeding is continuous and significant.[2]
Pathophysiology
Histologically, it resembles telangiectasia. Development is related to age and strain on the bowel wall, which is thought to influence the caliber change and proliferation of the vascular tissue.[3]
Although angiodysplasia is probably quite common, the risk of bleeding is increased in disorders of coagulation. A classic association is Heyde's syndrome (coincidence of aortic valve stenosis and bleeding from angiodysplasia). In this disorder, von Willebrand factor (vWF) is proteolysed due to high shear stress in the highly turbulent blood flow around the aortic valve. vWF is most active in vascular beds with high shear stress, including angiodysplasias, and deficiency of vWF increases the bleeding risk from such lesions.[3]
Warkentin et al argue that apart from aortic valve stenosis, some other conditions that feature high shear stress might also increase the risk of bleeding from angiodysplasia.[3]
Therapy
If the anemia is severe, blood transfusion is required before any other intervention is considered. Endoscopic treatment is an initial possibility, where cautery or argon plasma coagulation (APC) laser treatment is applied through the endoscope. Resection of the affected part of the bowel may be needed. However, the lesions may be widespread, making such treatment impractical. Embolisation through angiography is occasionally contemplated with severely bleeding lesions that cannot be visualised on colonoscopy.
If the bleeding is from multiple or inaccessible sites, systemic therapy with medication may be necessary. First-line options include the antifibrinolytics tranexamic acid or aminocaproic acid. Estrogens can be used to stop bleeding from angiodysplasia. Estrogens cause mild hypercoaguability of the blood. Estrogen side effects can be dangerous and unpleasant in both sexes. Changes in voice and breast swelling is bothersome in men, but older women often report improvement of libido and perimenopausal symptoms. (The worries about hormone replacement therapy/HRT, however, apply here as well.)
In difficult cases, there have been positive reports about octreotide[4] and thalidomide,[5]
In severe cases or cases not responsive to either endoscopic or medical treatment, surgery may be necessary to arrest the bleeding.
References
- ↑ Neumann H, Mönkemüller K, Malfertheiner P (2007). "Obscure overt GI bleeding secondary to angiodysplasias at the hepaticojejunostomy diagnosed and successfully treated with double-balloon enteroscopy". Gastrointest Endosc: 563. doi:10.1016/j.gie.2007.06.051. PMID 17981272.
- ↑ Mitchell SH, Schaefer DC, Dubagunta S (2004). "A new view of occult and obscure gastrointestinal bleeding". Am Fam Physician. 69 (4): 875–81. PMID 14989574.
- ↑ 3.0 3.1 3.2 Warkentin TE, Moore JC, Anand SS, Lonn EM, Morgan DG (2003). "Gastrointestinal bleeding, angiodysplasia, cardiovascular disease, and acquired von Willebrand syndrome". Transfusion medicine reviews. 17 (4): 272–86. doi:10.1016/S0887-7963(03)00037-3. PMID 14571395.
- ↑ Junquera F, Saperas E, Videla S, Feu F, Vilaseca J, Armengol JR, Bordas JM, Piqué JM, Malagelada JR (2007). "Long-term efficacy of octreotide in the prevention of recurrent bleeding from gastrointestinal angiodysplasia". Am. J. Gastroenterol. 102 (2): 254–60. doi:10.1111/j.1572-0241.2007.01053.x. PMID 17311647.
- ↑ Shurafa M, Kamboj G (2003). "Thalidomide for the treatment of bleeding angiodysplasias". Am. J. Gastroenterol. 98 (1): 221–2. doi:10.1111/j.1572-0241.2003.07201.x. PMID 12526972.