Blepharitis pathophysiology: Difference between revisions
No edit summary |
m (Bot: Removing from Primary care) |
||
| (85 intermediate revisions by 7 users not shown) | |||
| Line 1: | Line 1: | ||
__NOTOC__ | __NOTOC__ | ||
{{Blepharitis}} | {{Blepharitis}} | ||
{{CMG}} {{AE}} {{SaraM}} | {{CMG}}; {{AE}} {{SaraM}} | ||
==Overview== | ==Overview== | ||
The exact [[pathogenesis]] of blepharitis is not fully understood. | |||
[[ | It is thought that blepharitis is caused by either bacterial colonization in the [[eyelids]] or [[meibomian gland]] dysfunction. | ||
Blepharitis may also be caused by [[allergens]] and [[mite]]s that affect the eyelashes.<ref name="pmid24055901">{{cite journal| author=Bunya VY, Brainard DH, Daniel E, Massaro-Giordano M, Nyberg W, Windsor EA et al.| title=Assessment of signs of anterior blepharitis using standardized color photographs. | journal=Cornea | year= 2013 | volume= 32 | issue= 11 | pages= 1475-82 | pmid=24055901 | doi=10.1097/ICO.0b013e3182a02e0e | pmc=3947496 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=24055901 }} </ref><ref name="pmid3957566">{{cite journal| author=Dougherty JM, McCulley JP| title=Bacterial lipases and chronic blepharitis. | journal=Invest Ophthalmol Vis Sci | year= 1986 | volume= 27 | issue= 4 | pages= 486-91 | pmid=3957566 | doi= | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=3957566 }} </ref> | |||
==Pathophysiology== | ==Pathophysiology== | ||
===Pathogenesis=== | ===Pathogenesis=== | ||
The exact [[pathogenesis]] of blepharitis is not fully understood. | |||
It is thought that blepharitis is caused by either bacterial colonization in the [[eyelids]] or [[meibomian gland]] dysfunction. However, in most cases of blepharitis, there is a considerable pathogenesis overlap between anterior and posterior blepharitis. | |||
====Anterior blepharitis==== | ====Anterior blepharitis==== | ||
The exact pathogenesis of anterior blepharitis is | Anterior blepharitis is often associated with [[staphylococcal infection]] or [[seborrhoeic dermatitis]]. The exact [[pathogenesis]] of anterior blepharitis is not fully understood. | ||
It is thought that blepharitis is caused by bacterial colonization (''[[Staphylococcus aureus]]'' or ''[[Staphylococcus epidermidis]]'') in the eyelids. Following bacterial colonization, bacterial lipase changes [[meibomian gland]] secretions and increases cholesterol concentration. These changes may result in an environment that affects the [[ocular|ocular surface]] and tear evaporation. It is thought that anterior blepharitis may also be caused by allergic response to bacterial [[antigens]] (mostly [[staphylococcal]] antigens).<ref name="pmid24055901">{{cite journal| author=Bunya VY, Brainard DH, Daniel E, Massaro-Giordano M, Nyberg W, Windsor EA et al.| title=Assessment of signs of anterior blepharitis using standardized color photographs. | journal=Cornea | year= 2013 | volume= 32 | issue= 11 | pages= 1475-82 | pmid=24055901 | doi=10.1097/ICO.0b013e3182a02e0e | pmc=3947496 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=24055901 }} </ref><ref name="pmid3957566">{{cite journal| author=Dougherty JM, McCulley JP| title=Bacterial lipases and chronic blepharitis. | journal=Invest Ophthalmol Vis Sci | year= 1986 | volume= 27 | issue= 4 | pages= 486-91 | pmid=3957566 | doi= | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=3957566 }} </ref> | |||
[[ | |||
====Posterior blepharitis==== | ====Posterior blepharitis==== | ||
Posterior blepharitis is often associated with skin | The exact pathogenesis of posterior blepharitis is not fully understood. It is thought that the abnormal [[meibomian gland]] secretions may result in posterior blepharitis. | ||
Demodex folliculorum | Posterior blepharitis is often associated with skin conditions, such as [[rosacea]] or [[seborrhoeic dermatitis]]. These conditions are associated with [[sebaceous glands]] and gland orifices abnormalities. | ||
It is thought that the abnormal meibomian gland secretions may cause a direct toxic effect on the [[ocular|ocular surface]]. Sebaceous glands abnormalities may also result in an environment that affect bacterial growth.<ref name=Blepharitis-1> Blepharitis. American Academy of Ophthalmology/eyewiki (2014). http://eyewiki.aao.org/Blepharitis Accessed on July 14, 2016 </ref> | |||
====Acute blepharitis==== | |||
Acute blepharitis may be caused by [[irritant]] or [[allergen]] exposure.<ref name="pmid19383269">{{cite journal| author=Lemp MA, Nichols KK| title=Blepharitis in the United States 2009: a survey-based perspective on prevalence and treatment. | journal=Ocul Surf | year= 2009 | volume= 7 | issue= 2 Suppl | pages= S1-S14 | pmid=19383269 | doi= | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=19383269 }} </ref> | |||
====Chronic blepharitis==== | |||
''[[Demodex folliculorum]]'' is an external parasite in [[hair follicles]], [[sebaceous glands]], and [[meibomian glands]]. It may cause either anterior or posterior blepharitis. The exact pathogenesis of chronic blepharitis caused by the [[Demodex]] mites is not fully understood. It is thought that over-proliferation of ''Demodex folliculorum'' in meibomian glands may result in lid-margin infection and ocular discomfort. | |||
It is also thought demodex blepharitis may be caused by immune system reactions to the mites leading to [[inflammation]]. | |||
<ref name="pmid25371637">{{cite journal| author=Bhandari V, Reddy JK| title=Blepharitis: always remember demodex. | journal=Middle East Afr J Ophthalmol | year= 2014 | volume= 21 | issue= 4 | pages= 317-20 | pmid=25371637 | doi=10.4103/0974-9233.142268 | pmc=4219223 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=25371637 }} </ref><ref name="pmid15774912">{{cite journal| author=Viswalingam M, Rauz S, Morlet N, Dart JK| title=Blepharokeratoconjunctivitis in children: diagnosis and treatment. | journal=Br J Ophthalmol | year= 2005 | volume= 89 | issue= 4 | pages= 400-3 | pmid=15774912 | doi=10.1136/bjo.2004.052134 | pmc=1772603 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=15774912 }} </ref> | |||
===Associated Conditions=== | ===Associated Conditions=== | ||
Blepharitis | Many diseases are associated with blepharitis such as skin, systemic, and ocular disease. These include: | ||
*[[ | |||
*[[Atopy]] | *Systemic or skin disease:<ref name="pmid3156100">{{cite journal| author=McCulley JP, Dougherty JM| title=Blepharitis associated with acne rosacea and seborrheic dermatitis. | journal=Int Ophthalmol Clin | year= 1985 | volume= 25 | issue= 1 | pages= 159-72 | pmid=3156100 | doi= | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=3156100 }} </ref><ref name="pmid21276617">{{cite journal| author=Nemet AY, Vinker S, Kaiserman I| title=Associated morbidity of blepharitis. | journal=Ophthalmology | year= 2011 | volume= 118 | issue= 6 | pages= 1062-8 | pmid=21276617 | doi=10.1016/j.ophtha.2010.10.015 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=21276617 }} </ref> | ||
*[[Systemic lupus erythematosus|Systemic lupus erythematosus (SLE)]] | **[[Rosacea]] | ||
*[[Sjögren's | **[[Seborrheic dermatitis]] | ||
* | **[[Atopy]] | ||
Blepharitis | **[[Systemic lupus erythematosus|Systemic lupus erythematosus (SLE)]] | ||
*[[ | **[[Sjögren's syndrome]] | ||
*[[Keratitis]] | *Ocular disease:<ref name="pmid3156100">{{cite journal| author=McCulley JP, Dougherty JM| title=Blepharitis associated with acne rosacea and seborrheic dermatitis. | journal=Int Ophthalmol Clin | year= 1985 | volume= 25 | issue= 1 | pages= 159-72 | pmid=3156100 | doi= | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=3156100 }} </ref><ref name="pmid21276617">{{cite journal| author=Nemet AY, Vinker S, Kaiserman I| title=Associated morbidity of blepharitis. | journal=Ophthalmology | year= 2011 | volume= 118 | issue= 6 | pages= 1062-8 | pmid=21276617 | doi=10.1016/j.ophtha.2010.10.015 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=21276617 }} </ref><ref name=blepharitis-2> Blepharitis. Diseases Database (2016). http://www.diseasesdatabase.com/relationship.asp?glngUserChoice=1455&bytRel=2&blnBW=0&strBB=RL&blnClassSort=255 Accessed on July 15, 2016</ref> | ||
*[[Dry eye syndrome]] | **[[Conjunctivitis]] | ||
*[[Chalazion]] | **Meibomianitis (inflammation of the [[meibomian glands]]) | ||
*[[Trichiasis]] | **[[Keratitis]] | ||
**[[Dry eye syndrome]] | |||
**[[Chalazion]] | |||
**[[Trichiasis]] | |||
===Gross Pathology=== | ===Gross Pathology=== | ||
On [[gross pathology]], lid margin swelling, misdirection of lashes, loss of lashes, oily or | On [[gross pathology]], lid margin swelling, misdirection of lashes, loss of lashes, oily or greasy deposits and crusting of anterior lid margin, , and [[hyperaemia|conjunctival hyperaemia]] are characteristic findings of blepharitis.<ref name="pmid23118519">{{cite journal| author=Benitez-Del-Castillo JM| title=How to promote and preserve eyelid health. | journal=Clin Ophthalmol | year= 2012 | volume= 6 | issue= | pages= 1689-98 | pmid=23118519 | doi=10.2147/OPTH.S33133 | pmc=3484726 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=23118519 }} </ref> | ||
===Microscopic Pathology=== | ===Microscopic Pathology=== | ||
On microscopic histopathological analysis, [[hyperkeratinization]] of the | On microscopic histopathological analysis, non granulomatous inflammation with [[neutrophils]], acanthosis, or parakeratosis are characteristic findings of staphylococcal blepharitis.<ref name="pmid2087299">{{cite journal| author=Seal D, Ficker L, Ramakrishnan M, Wright P| title=Role of staphylococcal toxin production in blepharitis. | journal=Ophthalmology | year= 1990 | volume= 97 | issue= 12 | pages= 1684-8 | pmid=2087299 | doi= | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=2087299 }} </ref> | ||
On microscopic histopathological analysis, | |||
On microscopic histopathological analysis, [[hyperkeratinization]] of the meibomian gland ductal epithelium, [[mononuclear]] cellular infiltrates, and spongiosis in eyelids are characteristic findings of seborrheic blepharitis.<ref name="pmid13274422">{{cite journal| author=THYGESON P, VAUGHAN DG| title=Seborrheic blepharitis. | journal=Trans Am Ophthalmol Soc | year= 1954 | volume= 52 | issue= | pages= 173-88 | pmid=13274422 | doi= | pmc=1312591 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=13274422 }} </ref> | |||
On microscopic histopathological analysis, chronic inflammatory changes, [[hyperplasia|epithelial hyperplasia]], and follicular plugging are characteristic findings of chronic blepharitis.<ref name="pmid24904668">{{cite journal| author=Wesolowska M, Knysz B, Reich A, Blazejewska D, Czarnecki M, Gladysz A et al.| title=Prevalence of Demodex spp. in eyelash follicles in different populations. | journal=Arch Med Sci | year= 2014 | volume= 10 | issue= 2 | pages= 319-24 | pmid=24904668 | doi=10.5114/aoms.2014.42585 | pmc=4042053 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=24904668 }} </ref> | |||
===Images=== | ===Images=== | ||
The following are gross images associated with blepharitis | The following are gross images associated with blepharitis: | ||
<gallery> | <gallery> | ||
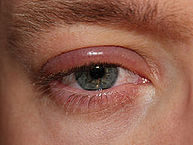
Image:193px-Blepharitis.JPG|Blepharitis | Image:193px-Blepharitis.JPG|Blepharitis of the right eye - By clubtable - Own work (Original text: eigenes Foto), Public Domain, https://commons.wikimedia.org/w/index.php?curid=20138102 | ||
Image:218px-Infant_with_blepharitis_on_the_right_side.jpg|Infant with blepharitis - By Sage Ross - Own work, CC BY-SA 3.0, https://commons.wikimedia.org/w/index.php?curid=8978907 | |||
</gallery> | </gallery> | ||
==References== | ==References== | ||
{{Reflist|2}} | {{Reflist|2}} | ||
[[Category: | [[Category:Disease]] | ||
[[Category:Up-To-Date]] | |||
[[Category:Ophthalmology]] | [[Category:Ophthalmology]] | ||
Latest revision as of 20:38, 29 July 2020
|
Blepharitis Microchapters | |
|
Diagnosis | |
|---|---|
|
Treatment | |
|
Case Studies | |
|
Blepharitis pathophysiology On the Web | |
|
American Roentgen Ray Society Images of Blepharitis pathophysiology | |
|
Risk calculators and risk factors for Blepharitis pathophysiology | |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Sara Mehrsefat, M.D. [2]
Overview
The exact pathogenesis of blepharitis is not fully understood. It is thought that blepharitis is caused by either bacterial colonization in the eyelids or meibomian gland dysfunction. Blepharitis may also be caused by allergens and mites that affect the eyelashes.[1][2]
Pathophysiology
Pathogenesis
The exact pathogenesis of blepharitis is not fully understood. It is thought that blepharitis is caused by either bacterial colonization in the eyelids or meibomian gland dysfunction. However, in most cases of blepharitis, there is a considerable pathogenesis overlap between anterior and posterior blepharitis.
Anterior blepharitis
Anterior blepharitis is often associated with staphylococcal infection or seborrhoeic dermatitis. The exact pathogenesis of anterior blepharitis is not fully understood. It is thought that blepharitis is caused by bacterial colonization (Staphylococcus aureus or Staphylococcus epidermidis) in the eyelids. Following bacterial colonization, bacterial lipase changes meibomian gland secretions and increases cholesterol concentration. These changes may result in an environment that affects the ocular surface and tear evaporation. It is thought that anterior blepharitis may also be caused by allergic response to bacterial antigens (mostly staphylococcal antigens).[1][2]
Posterior blepharitis
The exact pathogenesis of posterior blepharitis is not fully understood. It is thought that the abnormal meibomian gland secretions may result in posterior blepharitis. Posterior blepharitis is often associated with skin conditions, such as rosacea or seborrhoeic dermatitis. These conditions are associated with sebaceous glands and gland orifices abnormalities. It is thought that the abnormal meibomian gland secretions may cause a direct toxic effect on the ocular surface. Sebaceous glands abnormalities may also result in an environment that affect bacterial growth.[3]
Acute blepharitis
Acute blepharitis may be caused by irritant or allergen exposure.[4]
Chronic blepharitis
Demodex folliculorum is an external parasite in hair follicles, sebaceous glands, and meibomian glands. It may cause either anterior or posterior blepharitis. The exact pathogenesis of chronic blepharitis caused by the Demodex mites is not fully understood. It is thought that over-proliferation of Demodex folliculorum in meibomian glands may result in lid-margin infection and ocular discomfort. It is also thought demodex blepharitis may be caused by immune system reactions to the mites leading to inflammation. [5][6]
Associated Conditions
Many diseases are associated with blepharitis such as skin, systemic, and ocular disease. These include:
- Systemic or skin disease:[7][8]
- Ocular disease:[7][8][9]
- Conjunctivitis
- Meibomianitis (inflammation of the meibomian glands)
- Keratitis
- Dry eye syndrome
- Chalazion
- Trichiasis
Gross Pathology
On gross pathology, lid margin swelling, misdirection of lashes, loss of lashes, oily or greasy deposits and crusting of anterior lid margin, , and conjunctival hyperaemia are characteristic findings of blepharitis.[10]
Microscopic Pathology
On microscopic histopathological analysis, non granulomatous inflammation with neutrophils, acanthosis, or parakeratosis are characteristic findings of staphylococcal blepharitis.[11]
On microscopic histopathological analysis, hyperkeratinization of the meibomian gland ductal epithelium, mononuclear cellular infiltrates, and spongiosis in eyelids are characteristic findings of seborrheic blepharitis.[12]
On microscopic histopathological analysis, chronic inflammatory changes, epithelial hyperplasia, and follicular plugging are characteristic findings of chronic blepharitis.[13]
Images
The following are gross images associated with blepharitis:
-
Blepharitis of the right eye - By clubtable - Own work (Original text: eigenes Foto), Public Domain, https://commons.wikimedia.org/w/index.php?curid=20138102
-
Infant with blepharitis - By Sage Ross - Own work, CC BY-SA 3.0, https://commons.wikimedia.org/w/index.php?curid=8978907
References
- ↑ 1.0 1.1 Bunya VY, Brainard DH, Daniel E, Massaro-Giordano M, Nyberg W, Windsor EA; et al. (2013). "Assessment of signs of anterior blepharitis using standardized color photographs". Cornea. 32 (11): 1475–82. doi:10.1097/ICO.0b013e3182a02e0e. PMC 3947496. PMID 24055901.
- ↑ 2.0 2.1 Dougherty JM, McCulley JP (1986). "Bacterial lipases and chronic blepharitis". Invest Ophthalmol Vis Sci. 27 (4): 486–91. PMID 3957566.
- ↑ Blepharitis. American Academy of Ophthalmology/eyewiki (2014). http://eyewiki.aao.org/Blepharitis Accessed on July 14, 2016
- ↑ Lemp MA, Nichols KK (2009). "Blepharitis in the United States 2009: a survey-based perspective on prevalence and treatment". Ocul Surf. 7 (2 Suppl): S1–S14. PMID 19383269.
- ↑ Bhandari V, Reddy JK (2014). "Blepharitis: always remember demodex". Middle East Afr J Ophthalmol. 21 (4): 317–20. doi:10.4103/0974-9233.142268. PMC 4219223. PMID 25371637.
- ↑ Viswalingam M, Rauz S, Morlet N, Dart JK (2005). "Blepharokeratoconjunctivitis in children: diagnosis and treatment". Br J Ophthalmol. 89 (4): 400–3. doi:10.1136/bjo.2004.052134. PMC 1772603. PMID 15774912.
- ↑ 7.0 7.1 McCulley JP, Dougherty JM (1985). "Blepharitis associated with acne rosacea and seborrheic dermatitis". Int Ophthalmol Clin. 25 (1): 159–72. PMID 3156100.
- ↑ 8.0 8.1 Nemet AY, Vinker S, Kaiserman I (2011). "Associated morbidity of blepharitis". Ophthalmology. 118 (6): 1062–8. doi:10.1016/j.ophtha.2010.10.015. PMID 21276617.
- ↑ Blepharitis. Diseases Database (2016). http://www.diseasesdatabase.com/relationship.asp?glngUserChoice=1455&bytRel=2&blnBW=0&strBB=RL&blnClassSort=255 Accessed on July 15, 2016
- ↑ Benitez-Del-Castillo JM (2012). "How to promote and preserve eyelid health". Clin Ophthalmol. 6: 1689–98. doi:10.2147/OPTH.S33133. PMC 3484726. PMID 23118519.
- ↑ Seal D, Ficker L, Ramakrishnan M, Wright P (1990). "Role of staphylococcal toxin production in blepharitis". Ophthalmology. 97 (12): 1684–8. PMID 2087299.
- ↑ THYGESON P, VAUGHAN DG (1954). "Seborrheic blepharitis". Trans Am Ophthalmol Soc. 52: 173–88. PMC 1312591. PMID 13274422.
- ↑ Wesolowska M, Knysz B, Reich A, Blazejewska D, Czarnecki M, Gladysz A; et al. (2014). "Prevalence of Demodex spp. in eyelash follicles in different populations". Arch Med Sci. 10 (2): 319–24. doi:10.5114/aoms.2014.42585. PMC 4042053. PMID 24904668.