Motor neuron disease
| Motor neurone disease | |
 | |
|---|---|
| ICD-10 | G12.2 |
| ICD-9 | 335.2 |
| DiseasesDB | 8358 |
| MeSH | D016472 |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
The motor neuron diseases (or motor neurone diseases) (MND) are a group of progressive neurological disorders that destroy motor neurons, the cells that control voluntary muscle activity such as speaking, walking, breathing, and swallowing.
Forms
Forms of motor neuron disease include:
- amyotrophic lateral sclerosis (ALS) (sometimes called Lou Gehrig's disease)
- primary lateral sclerosis (PLS)
- progressive muscular atrophy (PMA)
- bulbar[1]
- pseudobulbar palsy - spastic
- progressive bulbar palsy - spastic and flaccid
Spinal muscular atrophy (SMA) is sometimes (but not always) considered a form of MND.
Terminology
In this article, MND refers to a group of diseases which affect the motor neurons. In the United States, the term ALS is more commonly used, where it is also known as Lou Gehrig's disease, after the baseball player. Although previously described by other neurologists of the 19th century, it was Jean-Martin Charcot, a French neurologist, who suggested grouping together a number of disparate conditions all affecting the lateral horn of the spinal cord in 1869. In France the disease is sometimes known as Maladie de Charcot (Charcot's disease), although it may also be referred to by the direct translation of ALS, Sclerose Laterale Amyotrophique (SLA). To help prevent confusion, the annual scientific research conference dedicated to the study of MND is called the International ALS/MND Symposium.
Signs and symptoms
Neurological examination presents specific signs associated with upper and lower motor neurone degeneration. Signs of upper motor neurone damage include spasticity, brisk reflexes and the Babinski sign. Signs of lower motor neurone damage include weakness and muscle atrophy.
Note that every muscle group in the body requires both upper and lower motor neurones to function. It is a common misconception that "upper" motor neurones control the arms, whilst "lower" motor neurones control the legs. The signs described above can occur in any muscle group, including the arms, legs, torso, and bulbar region.
Symptoms usually present between the ages of 50-70, and include progressive weakness, muscle wasting, and muscle fasciculations; spasticity or stiffness in the arms and legs; and overactive tendon reflexes. Patients may present with symptoms as diverse as a dragging foot, unilateral muscle wasting in the hands, or slurred speech.
The symptoms described above may resemble a number of other rare diseases, known as "MND Mimic Disorders". These include, but are not limited to multifocal motor neuropathy, Kennedy's disease, hereditary spastic paraplegia, spinal muscular atrophy and monomelic amyotrophy. A small subset of familial MND cases occur in children, such as "juvenile ALS", Madras syndrome, and individuals who have inherited the ALS2 gene. However, these are not typically referred to as MND, but by their specific names.
Diagnosis
The diagnosis of MND is a clinical one, established by a neurologist on the basis of history and neurological examination. There is no diagnostic test for MND. Investigations such as blood tests, electromyography (EMG), magnetic resonance imaging (MRI), and sometimes genetic testing are useful to rule out other disorders that may mimic MND. However, the diagnosis of MND remains a clinical one. Having excluded other diseases, a relatively rapid progression of symptoms is a strong diagnostic factor. Although an individual's progression may sometimes "plateau", it will not recover or slow down.
A set of diagnostic criteria called the El Escorial criteria[2][3] have been defined by the World Federation of Neurologists for use in research, particularly as inclusion/exclusion criteria for clinical trials. Due to a lack of clinical diagnostic criteria, some neurologists use the El Escorial criteria during the diagnostic process, although strictly speaking this is functionality creep, and some have questioned the appropriateness of the criteria in a clinical setting.[4]
- MND in the presence of both upper and lower motor neurone degeneration is ALS.
- Where the illness affects only the upper motor neurones it is PLS.
- Where the illness affects only the lower motor neurones it is PMA.
- Progressive bulbar palsy is degeneration of the lower motor neurones innervating the bulbar region (mouth, face, and throat).
- Pseudobulbar palsy refers to degeneration of the upper motor neurones to the same region.
It it possible that Transcranial Magnetic Stimulation can be used to diagnose MND. [5]
Prognosis
Most cases of MND progress quite quickly, with noticeable decline occurring over the course of months. Although symptoms may present in one region, they will typically spread. If restricted to one side of the body they are more likely to progress to the same region on the other side of the body before progressing to a new region. After several years, most patients require help to carry out activities of daily living such as self care, feeding, and transportation.
MND is typically fatal within 2-5 years. Around 50% die within 14 months of diagnosis. The remaining 50% will not necessarily die within the next 14 months as the distribution is significantly skewed. As a rough estimate, 1 in 5 patients survive for 5 years, and 1 in 10 patients survive 10 years. Stephen Hawking is a well-known example of a person with MND, and has lived for more than 40 years with the disease.
Mortality results when control of the diaphragm is impaired and the ability to breathe is lost. One exception is PLS, which may last for upwards of 25 years. Given the typical age of onset, this effectively leaves most PLS patients with a normal life span. PLS can progress to ALS, decades later.
Pathology
Causes
About 90% of cases of MND are "sporadic", meaning that the patient has no family history of ALS and the case appears to have occurred with no known cause. Genetic factors are suspected to be important in determining an individual's susceptibility to disease, and there is some weak evidence to suggest that onset can be "triggered" by as yet unknown environmental factors (see 'Epidemiology' below).
Approximately 10% of cases are "familial MND", defined either by a family history of MND or by testing positive for a known genetic mutation associated with the disease. The following genes are known to be linked to ALS: Cu/Zn superoxide dismutase SOD1, ALS2, NEFH (a small number of cases), senataxin (SETX) and vesicle associated protein B (VAPB).
Of these, SOD1 mutations account for some 20% of familial MND cases. The SOD1 gene codes for the enzyme superoxide dismutase, a free radical scavenger that reduces the oxidative stress of cells throughout the body. So far over 100 different mutations in the SOD1 gene have been found, all of which cause some form of ALS(ALSOD database). In North America, the most commonly occurring mutation is known as A4V and occurs in up to 50% of SOD1 cases. In people of Scandinavian extraction there is a relatively benign mutation called D90A which is associated with a slow progression. Future research is concentrating on identifying new genetic mutations and the clinical syndrome associated with them. Familial MND may also confer a higher risk of developing cognitive changes such as fronto-temporal dementia or executive dysfunction (see 'extra-motor change in MND' below).
It is thought that SOD1 mutations confer a toxic gain, rather than a loss, of function to the enzyme. SOD1 mutations may increase the propensity for the enzyme to form protein aggregates which are toxic to nerve cells.
Pathophysiology
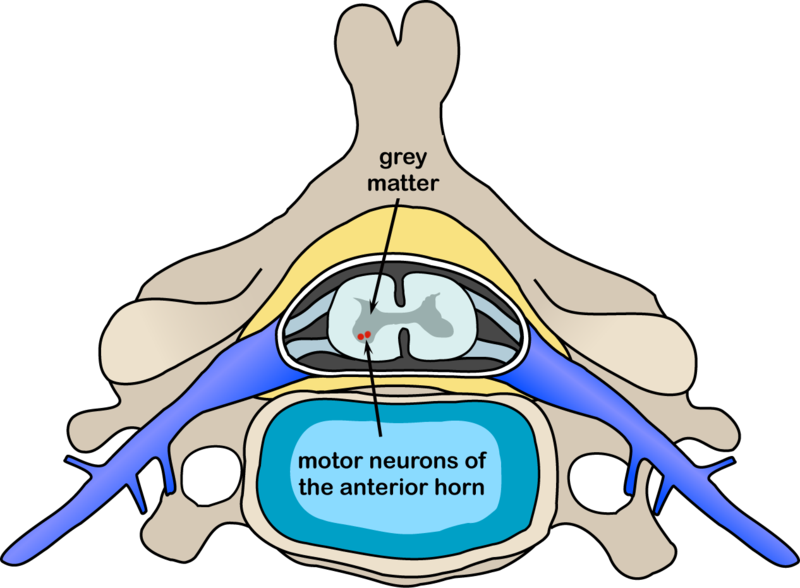
Skeletal muscles are innervated by a group of neurones (lower motor neurones) located in the ventral horns of the spinal cord which project out the ventral roots to the muscle cells. These nerve cells are themselves innervated by the corticospinal tract or upper motor neurones that project from the motor cortex of the brain. On macroscopic pathology, there is a degeneration of the ventral horns of the spinal cord, as well as atrophy of the ventral roots. In the brain, atrophy may be present in the frontal and temporal lobes. On microscopic examination, neurones may show spongiosis, the presence of astrocytes, and a number of inclusions including characteristic "skein-like" inclusions, bunina bodies, and vacuolisation.
There is a role in excitotoxicity and oxidative stress, presumably secondary to mitochondrial dysfunction. In animal models, death by apoptosis has also been identified.
Emotional lability / pseudobulbar affect
Around a third of all MND patients experience labile affect, also known as emotional lability, pseudobulbar affect, or pathological laughter and crying. Patients with pseudobulbar palsy are particularly likely to be affected, as are patients with PLS.
Extra-motor change in MND
Cognitive change can and does occur in between 33–50% of patients. A small proportion exhibit a form of frontotemporal dementia characterised by behavioural abnormalities such as disinhibition, apathy, and personality changes. A small proportion of patients may also suffer from an aphasia, which causes difficulty in naming specific objects. A larger proportion (up to 50%) suffer from a milder version of cognitive change which primarily affects what is known as executive function. Briefly, this is the ability of an individual to initiate, inhibit, sustain, and switch attention and is involved in the organisation of complex tasks down to smaller components. Often patients with such changes find themselves unable to do the family finances or drive a car. Depression is surprisingly rare in MND (around 5–20%) relative to the frequency with which it is found in other, less severe, neurological disorders e.g. ~50% in multiple sclerosis and Parkinson's disease, ~20% in Epilepsy. Depression does not necessarily increase as the symptoms progress, and in fact many patients report being happy with their quality of life despite profound disability. This may reflect the use of coping strategies such as reevaluating what is important in life.
Although traditionally thought only to affect the motor system, sensory abnormalities are not necessarily absent, with some patients finding altered sensation to touch and heat, found in around 10% of patients. Patients with a predominantly upper motor neurone syndrome, and particularly PLS, often report an enhanced startle reflex to loud noises.
Neuroimaging and neuropathology has demonstrated extra-motor changes in the frontal lobes including the inferior frontal gyrus, superior frontal gyrus, anterior cingulate cortex, and superior temporal gyrus. The degree of pathology in these areas has been directly related to the degree of cognitive change experienced by the patient, if any. Patients with MND and dementia have been shown to exhibit marked frontotemporal lobe atrophy as revealed by MRI or SPECT neuroimaging.
Epidemiology
The incidence of MND is approximately 1–5 out of 100,000 people. Men have a slightly higher incidence rate than women. Approximately 5,600 cases are diagnosed in the U.S. every year. By far the greatest risk factor is age, with symptoms typically presenting between the ages of 50-70. Cases under the age of 50 years are called "young onset MND", whilst incidence rates appear to tail off after the age of 85.
Tentative environmental risk factors identified so far include: exposure to severe electrical shock leading to coma, having served in the first Gulf War, and playing professional football (soccer). However, these findings have not been firmly identified and more research is needed.
There are three "hot spots" of MND in the world. One is in the Kii peninsula of Japan, one amongst a tribal population in Papua New Guinea. Chamorro inhabitants from the island of Guam in the Pacific Ocean have an increased risk of developing a form of MND known as Guamanian ALS-PD-dementia complex or "lytico bodig", although the incidence rate has declined over the last 50 years and the average age of onset has increased.[6] Putative theories involve neurotoxins in the traditional diet including cycad nut flour and bats that have eaten cycad nuts.[7][8]
Treatment
Currently there is no cure for ALS. The only drug that affects the course of the disease is riluzole. The drug functions by blocking the effects of the neurotransmitter glutamate, and is thought to extend the lifespan of an ALS patient by only a few months.
The lack of effective medications to slow the progression of ALS does not mean that patients with ALS cannot be medically cared for. Instead, treatment of patients with ALS focuses on the relief of symptoms associated with the disease. This involves a variety of health professionals including neurologists, speech-language pathologists, physical therapists, occupational therapists, dieticians, respiratory therapists, social workers, palliative care specialists, specialist nurses and psychologists. A list of neurology clinics that specialize in the care of patients with ALS can be found on the World Federation of Neurology website (http://www.wfnals.org/clinics/).
Research efforts
The search for a drug that will slow MND progression is underway. For example, recent research using mouse models suggests that minocycline, a common antibiotic, may also be effective in extending the lifespan of MND sufferers.[9][10][11] This drug must pass clinical trials with ALS patients before it may be used as a general treatment for MND.
Minocycline extends the lifespan of MND mice with SOD1 mutations, but it does not prevent their eventual death. Other agents that are currently in trials include ceftriaxone, arimoclomol, IGF-1 and coenzyme Q10 to name but a few. A list of US-based clinical MND trials may be found at www.clinicaltrials.org or by contacting your local ALS/MND charity.
Etymology
Amyotrophic comes from the Greek language: A- means "no", myo refers to "muscle", and trophic means "nourishment"; amyotrophic therefore means "no muscle nourishment," which describes the characteristic atrophication of the sufferer's disused muscle tissue. Lateral identifies the areas in a person's spinal cord where portions of the nerve cells that are affected are located. As this area degenerates it leads to scarring or hardening ("sclerosis") in the region
History and prominent patients
U.S. baseball player Lou Gehrig brought national and international attention to the disease in 1939 when he abruptly retired after being diagnosed with ALS/MND; he would die two years later. Former guitar virtuoso Jason Becker and theoretical physicist Stephen Hawking also suffer from the disease.
Founder of care homes Leonard Cheshire VC, owner from 1957-1966 of Athelhampton House in Dorset Sir Robert Cooke F.R.C.S., theoretical physicist Victor Emery, Rangers football (soccer)|footballer Sam English, Hall of Fame pitcher Jim "Catfish" Hunter, blues singer and guitarist Leadbelly, Chinese Chairman Mao Zedong, jazz giant Charles Mingus, Hollywood actor David Niven, Richard Allen (abstract artist), legendary Leeds United manager and ex-football player, Don Revie, teacher and book subject Morrie Schwartz, American television actor Lane Smith, linguist Larry Trask, Guardian journalist Jill Tweedie, avant-garde guitarist [Derek Bailey, American soap opera veteran Michael Zaslow, libertarian writer, politician, and investment analyst, Harry Browne, The Shield executive producer Scott Brazil, and ex-Celtic Football (soccer)|football player Jimmy Johnstone died from the disease.
Diane Pretty was a British woman with the disease who was involved in a prominent right-to-die case in the early 2000s.
See also
- Kennedy disease
- Monomelic amyotrophy
- Primary lateral sclerosis
- Progressive muscular atrophy
- Riluzole
References
- ↑ Template:GPnotebook
- ↑ Brooks BR (1994). "El Escorial World Federation of Neurology criteria for the diagnosis of amyotrophic lateral sclerosis. Subcommittee on Motor Neuron Diseases/Amyotrophic Lateral Sclerosis of the World Federation of Neurology Research Group on Neuromuscular Diseases and the El Escorial "Clinical limits of amyotrophic lateral sclerosis" workshop contributors". J. Neurol. Sci. 124 Suppl: 96–107. PMID 7807156.
- ↑ "El Escorial Revisited: Revised Criteria for the Diagnosis of Amyotrophic Lateral Sclerosis - Requirements for Diagnosis". Retrieved 2007-06-06.
- ↑ Belsh JM (2000). "ALS diagnostic criteria of El Escorial Revisited: do they meet the needs of clinicians as well as researchers?". Amyotroph. Lateral Scler. Other Motor Neuron Disord. 1 Suppl 1: S57–60. PMID 11464928.
- ↑ "A Twitch of Potential". Time. Retrieved 2006-12-30.
- ↑ Waring, S.C; et al. (2004). "Incidence of Amyotrophic Lateral Sclerosis and of the Parkinsonism-Dementia Complex of Guam, 1950-1989". Neuroepidemiology. 23 (4): 192–199.
- ↑ "Flying fox linked to disease - The Boston Globe". Retrieved 2007-06-06.
- ↑ Miller G (2006). "Neurodegenerative disease. Guam's deadly stalker: on the loose worldwide?". Science. 313 (5786): 428–31. doi:10.1126/science.313.5786.428. PMID 16873621.
- ↑ Zhu S, Stavrovskaya IG, Drozda M; et al. (2002). "Minocycline inhibits cytochrome c release and delays progression of amyotrophic lateral sclerosis in mice". Nature. 417 (6884): 74–8. doi:10.1038/417074a. PMID 11986668.
- ↑ Van Den Bosch L, Tilkin P, Lemmens G, Robberecht W (2002). "Minocycline delays disease onset and mortality in a transgenic model of ALS". Neuroreport. 13 (8): 1067–70. PMID 12060810.
- ↑ Kriz J, Nguyen MD, Julien JP (2002). "Minocycline slows disease progression in a mouse model of amyotrophic lateral sclerosis". Neurobiol. Dis. 10 (3): 268–78. PMID 12270689.
External links
- Scottish Motor Neurone Disease Association
- ALS Therapy Development Foundation
- ALS Association
- ALS/MND Alliance
- MND Association
- ALS Liga Belgium (Dutch and French language)
- The Hereditary Motor Neurone Disease Foundation - Australian group seeking to find a cure for familial Motor Neurone Disease.
- ALSforums is a volunteer driven online support group for people affected by ALS/MND
- BUILD-UK Forum for people with ALS/MND (UK-Based)
- ALS Society of Canada
- MND Association of Australia
- Project A.L.S
- Template:GPnotebook
- Information about clinical trials
- Template:NINDS
- ALSOD Database of all known SOD1 mutations
Template:Diseases of the nervous system
de:Amyotrophe Lateralsklerose nl:Amyotrofische laterale sclerose no:Motonevronsykdom sv:Amyotrofisk lateralskleros ur:عصبون حرکی مرض