Picture archiving and communication system
Please Take Over This Page and Apply to be Editor-In-Chief for this topic: There can be one or more than one Editor-In-Chief. You may also apply to be an Associate Editor-In-Chief of one of the subtopics below. Please mail us [1] to indicate your interest in serving either as an Editor-In-Chief of the entire topic or as an Associate Editor-In-Chief for a subtopic. Please be sure to attach your CV and or biographical sketch.
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [2]
Assistant Editor-In-Chief: Anand Patel, MD [3]
Please Take Over This Page and Apply to be Editor-In-Chief for this topic: There can be one or more than one Editor-In-Chief. You may also apply to be an Associate Editor-In-Chief of one of the subtopics below. Please mail us [4] to indicate your interest in serving either as an Editor-In-Chief of the entire topic or as an Associate Editor-In-Chief for a subtopic. Please be sure to attach your CV and or biographical sketch.
Overview

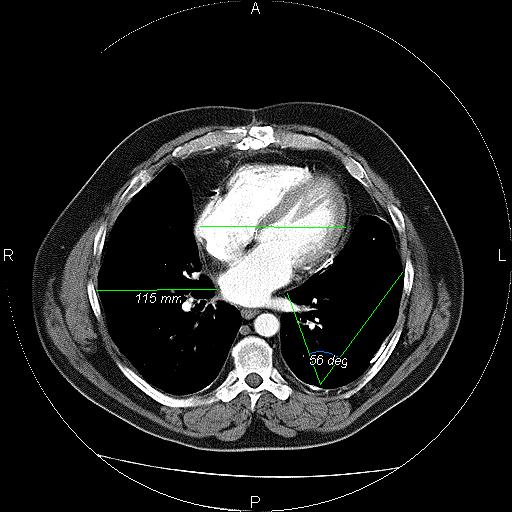
In medical imaging, picture archiving and communication systems (PACS) are computers or networks dedicated to the storage, retrieval, distribution and presentation of images. The medical images are stored in an independent format. The most common format for image storage is DICOM (Digital Imaging and Communications in Medicine).
Types of Images
Most PACSs handle images from various medical imaging instruments, including ultrasound, magnetic resonance, PET, computed tomography, endoscopy, mammograms and X-rays.
Uses
PACS replaces hard-copy based means of managing medical images, such as film archives. It expands on the possibilities of such conventional systems by providing capabilities of off-site viewing and reporting (distance education, tele-diagnosis). Additionally, it enables practitioners at various physical locations to access the same information simultaneously, (teleradiology). With the decreasing price of digital storage, PACS systems provide a growing cost and space advantage over film archives.
PACS is offered by virtually all the major medical imaging equipment manufacturers, medical IT companies and many independent software companies.
The most difficult area for PACS is interpreting the DICOM image format. DICOM has enough latitude to allow various vendors of medical imaging equipment to create DICOM compliant files that differ in the internal tags used to label the data and the metadata. A feature common to most PACS is to read the metadata from all the images into a central database. This allows the PACS user to retrieve all images with a common feature no matter the originating instrument. The differences between vendors' DICOM implementations make this a difficult task.
Architecture
Typically a PACS network consists of a central server that stores a database containing the images connected to one or more clients via a LAN or a WAN which provide or utilize the images. Web-based PACS is becoming more and more common: these systems utilize the Internet as their means of communication, usually via VPN (Virtual Private Network) or SSL (Secure Sockets Layer). The software (thin or smart client) is loaded via ActiveX, Java, or .NET Framework. Definitions vary, but most claim that for a system to be truly web based, each individual image should have its own URL. Client workstations can use local peripherals for scanning image films into the system, printing image films from the system and interactive display of digital images. PACS workstations offer means of manipulating the images (crop, rotate, zoom, brightness, contrast and others).
Modern radiology equipment, modalities, feed patient images directly to the PACS in digital form. For backwards compatibility, most hospital imaging departments and radiology practices employ a film digitizer.
Integration
A full PACS system should provide a single point of access for images and their associated data (i.e. it should support multiple modalities). It should also interface with existing hospital information systems: hospital information system (HIS) and radiology information system (RIS).
Interfacing between multiple systems provides a more consistent and more reliable dataset:
- Less risk of entering an incorrect patient ID for a study – modalities that support DICOM worklists can retrieve identifying patient information (patient name, patient number, accession number) for upcoming cases and present that to the technologist, preventing data entry errors during acquisition. Once the acquisition is complete, the PACS can compare the embedded image data with a list of scheduled studies from RIS, and can flag a warning if the image data does not match a scheduled study.
- Data saved in the PACS can be tagged with unique patient identifiers (such as a social security number or NHS number) obtained from HIS. Providing a robust method of merging datasets from multiple hospitals, even where the different centers use different ID systems internally.
An interface can also improve workflow patterns:
- When a study has been reported by a radiologist the PACS can mark it as read. This avoids needless double-reading. The report can be attached to the images and be viewable via a single interface.
- Improved use of online storage and nearline storage in the image archive. The PACS can obtain lists of appointments and admissions in advance, allowing images to be pre-fetched from nearline storage (for example, tape libraries or DVD jukeboxes) onto online disk storage (RAID array).
Recognition of the importance of integration has led a number of suppliers to develop fully integrated RIS/PACS systems. These may offer a number of advanced features:
- Dictation of reports can be integrated into a single system. The recording is automatically sent to a transcriptionist's workstation for typing, but it can also be made available for access by physicians, avoiding typing delays for urgent results, or retained in case of typing error.
- Provides a single tool for quality control and audit purposes. Rejected images can be tagged, allowing later analysis (as may be required under radiation protection legislation). Workloads and turn-around time can be reported automatically for management purposes.
History
The principles of PACS were first discussed at meetings of radiologists in 1982. Various people are credited with the coinage of the term PACS. Cardiovascular radiologist Dr Andre Duerinckx reported in 1983 that he had first used the term in 1981.[1] Dr Samuel Dwyer, though, credits Dr Judith M. Prewitt for introducing the term.[2]
References
- ↑ Duerinckx AJ, Pisa EJ. Filmless Picture Archiving and Communication System (PACS) in Diagnostic Radiology. Proc SPIE 1982;318;9-18. Reprinted in IEEE Computer Society Proceedings of PACS'82, order No 388.
- ↑ Samuel J. Dwyer III. A personalized view of the history of PACS in the USA. In: Proceedings of the SPIE, "Medical Imaging 2000: PACS Design and Evaluation: Engineering and Clinical Issues", edited by G. James Blaine and Eliot L. Siegel. 2000;3980:2-9.
See also
- X-ray
- DICOM
- Computed axial tomography
- Telemedicine
- Electronic health record (EHR)
- Electronic medical record (EMR)
External links
- PACS Administrator Resources
- Open source PACS at UCLA
- Raynux: OpenSource and Radiology
- Teleradiology, PACS and DICOM Software List of free PACS and DICOM software available on the web
- DICOM info and a list of free tools
- History of PACS
de:Picture Archiving and Communication System it:Picture archiving and communication system nl:Picture Archiving and Communication System no:Picture archiving and communication system sv:PACS Template:WH Template:WS