Magnetic resonance angiography
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
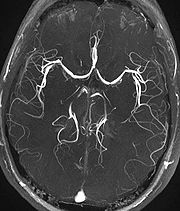
Magnetic Resonance Angiography is the imaging of blood vessels using Magnetic Resonance Imaging. Magnetic Resonance Angiography (MRA) is used to generate pictures of the arteries in order to evaluate them for stenosis (abnormal narrowing) or aneurysms (vessel wall dilatations, at risk of rupture). MRA is often used to evaluate the arteries of the neck and brain, the thoracic and abdominal aorta, the renal arteries, and the legs (called a "run-off"). A variety of techniques can be used to generate the pictures, such as administration of a paramagnetic contrast agent (gadolinium) or using a technique known as "flow-related enhancement" (e.g. 2D and 3D time-of-flight sequences), where most of the signal on an image is due to blood which has recently moved into that plane. Magnetic Resonance Venography (MRV) is a similar procedure that is used to image veins. In this method the tissue is now excited inferiorly while signal is gathered in the plane immediately superior to the excitation plane, and thus imaging the venous blood which has recently moved from the excited plane.
Acquisition
A variety of techniques can be used to generate the pictures, based on flow effects or on contrast (inherent or pharmacologically generated).
- Contrast enhanced (CE-MRA): Injection of MRI contrast agents is currently the most common method of acquiring MRA. The contrast medium is injected into a vein, and images are acquired during the first pass of the agent through the arteries. Provided that the timing is correct, this may result in images of very high quality. An alternative is to use a contrast agent that does not, as most agents, leave the vascular system within a few minutes, but remains in the circulation up to an hour (a "'blood-pool agent'"). Since longer time is available for image acquisition, higher resolution imaging is possible. A problem, however, is the fact that both arteries and veins are enhanced at the same time.
- Time-of-flight (TOF) or Inflow angiography, uses a short echo time and flow compensation to make flowing blood much brighter than stationary tissue. As flowing blood enters the area being imaged it has seen a limited number of excitation pulses so it is not saturated, this gives it a much higher signal than the saturated stationary tissue. As this method is dependent on flowing blood, areas with slow flow (such as large aneurysms) may not be well visualized. This is most commonly used in the head and neck and gives detailed high resolution images.
- Phase-contrast (PC-MRA): the phase of the MRI signal is manipulated by special gradients (varying magnetic fields) in such a way that it is directly proportional to velocity. Thus, quantitative measurements of blood flow are possible, in addition to imaging the flowing blood.
- Fresh blood imaging (FBI): An imaging technique using fast or super fast spin echo sequences (FSE/SFSE). Takes advantage of the longer T2 relaxation of blood compared to surrounding tissue. The images are acquired by fast spin echo sequences that can be synchronized with heart beats.
Similar procedures to flow effect based MRA can be used to image veins. Called Magnetic resonance venography (MRV) this can be achieved by exciting a plane inferiorly while signal is gathered in the plane immediately superior to the excitation plane, and thus imaging the venous blood which has recently moved from the excited plane. Differences in tissue signals, can also be used for MRA. This method is based on the different signal properties of blood compared to other tissues in the body, independent of MR flow effects. This is most successfully done with balanced pulse sequences such as TrueFISP or bTFE.
Visualization
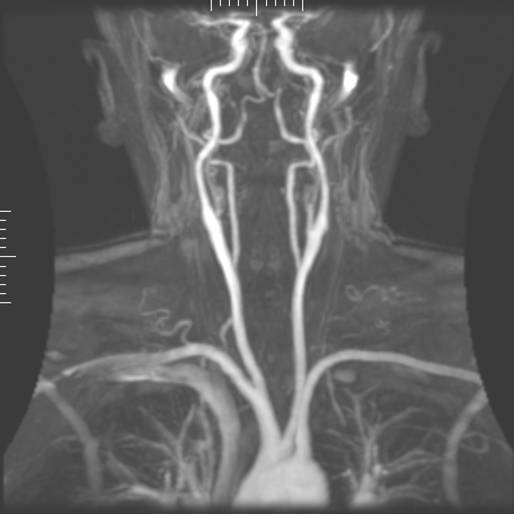
Occasionally, MRA directly produces (thick) slices that contain the entire vessel of interest. More commonly, however, the acquisition results in a stack of slices representing a 3D volume in the body. To display this 3D dataset on a 2D device such as a computer monitor, some rendering method has to be used. The most common method is Maximum intensity projection (MIP), where the computer simulates rays through the volume and selects the highest value for display on the screen. The resulting images resemble conventional catheter angiography images. If several such projections are combined into a cine loop or QuickTime VR object, the depth impression is improved, and the observer can get a good perception of 3D structure. An alternative to MIP is direct volume rendering where the MR signal is translated to properties like brightness, opacity and color and then used in an optical model.
Clinical use
MRA has been successful in studying many arteries in the body, including cerebral and other vessels in the head and neck, the aorta and its major branches in the thorax and abdomen, the renal arteries, and the arteries in the lower limbs. For the coronary arteries, however, MRA has been less successful than CT angiography or invasive catheter angiography. Most often, the underlying disease is atherosclerosis, but medical conditions like aneurysms or abnormal vascular anatomy can also be diagnosed.
An advantage of MRA compared to invasive catheter angiography is the non-invasive character of the examination (no catheters have to be introduced in the body). Another advantage, compared to CT angiography and catheter angiography, is that the patient is not exposed to any ionizing radiation. Also, contrast media used for MRI tend to be less toxic than those used for CT angiography and catheter angiography. The greatest drawbacks of the method are its comparatively high cost and its somewhat limited spatial resolution.