Guselkumab
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Sonya Gelfand
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Guselkumab is a human monoclonal IgG1λ antibody that is FDA approved for the treatment of moderate-to-severe plaque psoriasis in adults who are candidates for systemic therapy or phototherapy. Common adverse reactions include upper respiratory infections, headache, injection site reactions, arthralgia, diarrhea, gastroenteritis, tinea infections, and herpes simplex infections.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Dosage Forms and Strengths
- Injection: 100 mg/mL in a single-dose prefilled syringe.
- Guselkumab is a clear and colorless to light yellow solution that may contain small translucent particles.
Dosage
- Guselkumab is administered by subcutaneous injection. The recommended dose is 100 mg at Week 0, Week 4, and every 8 weeks thereafter.
Tuberculosis Assessment Prior to Initiation of Guselkumab
- Evaluate patients for tuberculosis (TB) infection prior to initiating treatment with guselkumab.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding guselkumab Off-Label Guideline-Supported Use and Dosage (Adult) in the drug label.
Non–Guideline-Supported Use
There is limited information regarding guselkumab Off-Label Non-Guideline-Supported Use and Dosage (Adult) in the drug label.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
There is limited information regarding Guselkumab FDA-Labeled Indications and Dosage (Pediatric) in the drug label.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding guselkumab Off-Label Guideline-Supported Use and Dosage (Pediatric) in the drug label.
Non–Guideline-Supported Use
There is limited information regarding guselkumab Off-Label Non-Guideline-Supported Use and Dosage (Pediatric) in the drug label.
Contraindications
- None.
Warnings
Infections
- Guselkumab may increase the risk of infection. In clinical trials, infections occurred in 23% of subjects in the guselkumab group versus 21% of subjects in the placebo group through 16 weeks of treatment. Upper respiratory tract infections, gastroenteritis, tinea infections, and herpes simplex infections occurred more frequently in the guselkumab group than in the placebo group. The rate of serious infections for the guselkumab group and the placebo group was ≤ 0.2%. Treatment with guselkumab should not be initiated in patients with any clinically important active infection until the infection resolves or is adequately treated.
- In patients with a chronic infection or a history of recurrent infection, consider the risks and benefits prior to prescribing guselkumab. Instruct patients to seek medical help if signs or symptoms of clinically important chronic or acute infection occur. If a patient develops a clinically important or serious infection or is not responding to standard therapy, monitor the patient closely and discontinue guselkumab until the infection resolves.
Pre-treatment Evaluation for Tuberculosis
- Evaluate patients for tuberculosis (TB) infection prior to initiating treatment with guselkumab. Initiate treatment of latent TB prior to administering guselkumab. In clinical studies, 105 subjects with latent TB who were concurrently treated with guselkumab and appropriate TB prophylaxis did not develop active TB (during the mean follow-up of 43 weeks). Monitor patients for signs and symptoms of active TB during and after guselkumab treatment. Consider anti-TB therapy prior to initiating guselkumab in patients with a past history of latent or active TB in whom an adequate course of treatment cannot be confirmed. Do not administer guselkumab to patients with active TB infection.
Immunizations
- Prior to initiating therapy with guselkumab, consider completion of all age appropriate immunizations according to current immunization guidelines. Avoid use of live vaccines in patients treated with guselkumab. No data are available on the response to live or inactive vaccines.
Adverse Reactions
Clinical Trials Experience
- The following adverse reactions are discussed in greater detail in other sections of labeling:
- Infections
Clinical Trials Experience
- Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
- In clinical trials, a total of 1748 subjects with moderate-to-severe plaque psoriasis received guselkumab. Of these, 1393 subjects were exposed to guselkumab for at least 6 months and 728 subjects were exposed for at least 1 year.
- Data from two placebo- and active-controlled trials (VOYAGE 1 and VOYAGE 2) in 1441 subjects (mean age 44 years; 70% males; 82% white) were pooled to evaluate the safety of guselkumab (100 mg administered subcutaneously at Weeks 0 and 4, followed by every 8 weeks).
Weeks 0 to 16
- In the 16-week placebo-controlled period of the pooled clinical trials (VOYAGE 1 and VOYAGE 2), adverse events occurred in 49% of subjects in the guselkumab group compared to 47% of subjects in the placebo group and 49% of subjects in the U.S. licensed adalimumab group. Serious adverse events occurred in 1.9% of the guselkumab group (6.3 events per 100 subject-years of follow-up) compared to 1.4% of the placebo group (4.7 events per 100 subject-years of follow-up), and in 2.6% of U.S. licensed adalimumab group (9.9 events per 100 subject-years of follow-up).
- Table 1 summarizes the adverse reactions that occurred at a rate of at least 1% and at a higher rate in the guselkumab group than in the placebo group during the 16-week placebo-controlled period.
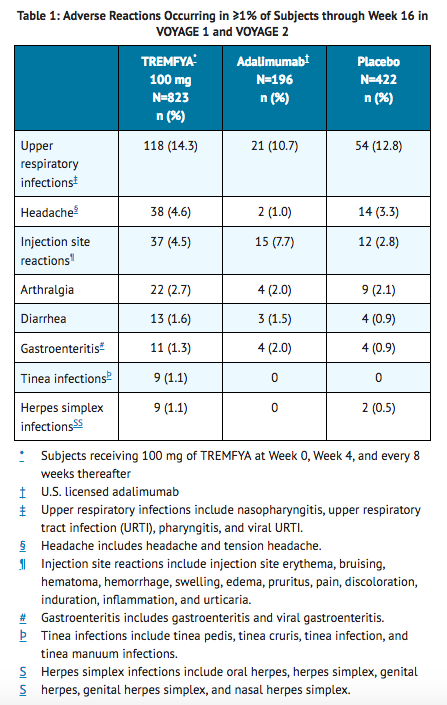
- Adverse reactions that occurred in < 1% but > 0.1% of subjects in the guselkumab group and at a higher rate than in the placebo group through Week 16 in VOYAGE 1 and VOYAGE 2 were migraine, candida infections, and urticaria.
Specific Adverse Reactions
Infections
- Infections occurred in 23% of the guselkumab group compared to 21% of the placebo group.
- The most common (≥ 1%) infections were upper respiratory infections, gastroenteritis, tinea infections, and herpes simplex infections; all cases were mild to moderate in severity and did not lead to discontinuation of guselkumab.
Elevated Liver Enzymes
- Elevated liver enzymes were reported more frequently in the guselkumab group (2.6%) than in the placebo group (1.9%). Of the 21 subjects who were reported to have elevated liver enzymes in the guselkumab group, all events except one were mild to moderate in severity and none of the events led to discontinuation of guselkumab.
Safety through Week 48
- Through Week 48, no new adverse reactions were identified with guselkumab use and the frequency of the adverse reactions was similar to the safety profile observed during the first 16 weeks of treatment.
Immunogenicity
- As with all therapeutic proteins, there is the potential for immunogenicity with guselkumab. The detection of antibody formation is highly dependent on the sensitivity and specificity of the assay. Additionally, the observed incidence of antibody (including neutralizing antibody) positivity in an assay may be influenced by several factors including assay methodology, sample handling, timing of sample collection, concomitant medications, and underlying disease. For these reasons, comparison of incidence of antibodies to guselkumab with the incidences of antibodies to other products may be misleading.
- Up to Week 52, approximately 6% of subjects treated with guselkumab developed antidrug antibodies. Of the subjects who developed antidrug antibodies, approximately 7% had antibodies that were classified as neutralizing antibodies. Among the 46 subjects who developed antibodies to guselkumab and had evaluable data, 21 subjects exhibited lower trough levels of guselkumab, including one subject who experienced loss of efficacy after developing high antibody titers. However, antibodies to guselkumab were generally not associated with changes in clinical response or development of injection-site reactions.
Postmarketing Experience
There is limited information regarding Guselkumab Postmarketing Experience in the drug label.
Drug Interactions
- Live Vaccinations
- CYP450 Substrates
Live Vaccinations
- Avoid use of live vaccines in patients treated with guselkumab.
CYP450 Substrates
- The formation of CYP450 enzymes can be altered by increased levels of certain cytokines (e.g., IL-1, IL-6, IL-10, TNFα, interferon) during chronic inflammation.
- Results from an exploratory drug-drug interaction study in subjects with moderate-to-severe psoriasis suggested a low potential for clinically relevant drug interactions for drugs metabolized by CYP3A4, CYP2C9, CYP2C19 and CYP1A2 but the interaction potential cannot be ruled out for drugs metabolized by CYP2D6. However, the results were highly variable because of the limited number of subjects in the study.
- Upon initiation of guselkumab in patients who are receiving concomitant CYP450 substrates, particularly those with a narrow therapeutic index, consider monitoring for therapeutic effect or drug concentration and consider dosage adjustment as needed
Use in Specific Populations
Pregnancy
Risk Summary
- There are no available data on guselkumab use in pregnant women to inform a drug associated risk of adverse developmental outcomes. Human IgG antibodies are known to cross the placental barrier; therefore, guselkumab may be transmitted from the mother to the developing fetus. In a combined embryofetal development and pre- and post-natal development study, no adverse developmental effects were observed in infants born to pregnant monkeys after subcutaneous administration of guselkumab during organogenesis through parturition at doses up to 30 times the maximum recommended human dose (MRHD). Neonatal deaths were observed at 6- to 30-times the MRHD (see DATA). The clinical significance of these nonclinical findings is unknown.
- All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Data (Animal)
- In a combined embryofetal development and pre- and post-natal development study, pregnant cynomolgus monkeys were administered weekly subcutaneous doses of guselkumab up to 50 mg/kg (30 times the MRHD based on a mg/kg comparison) from the beginning of organogenesis to parturition. Neonatal deaths occurred in the offspring of one control monkey, three monkeys administered guselkumab at 10 mg/kg/week (6 times the MRHD based on a mg/kg comparison) and three monkeys administered guselkumab at 50 mg/kg/week (30 times the MRHD based on a mg/kg comparison). The clinical significance of these findings is unknown. No guselkumab-related effects on functional or immunological development were observed in the infants from birth through 6 months of age.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Guselkumab in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Guselkumab during labor and delivery.
Nursing Mothers
Risk Summary
- There are no data on the presence of guselkumab in human milk, the effects on the breastfed infant, or the effects on milk production. Guselkumab was not detected in the milk of lactating cynomolgus monkeys. Maternal IgG is known to be present in human milk. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for guselkumab and any potential adverse effects on the breastfed infant from guselkumab or from the underlying maternal condition.
Pediatric Use
- The safety and efficacy of guselkumab in pediatric patients (less than 18 years of age) have not been established.
Geriatic Use
- Of the 1748 subjects with plaque psoriasis exposed to guselkumab, a total of 93 subjects were 65 years or older, and 4 subjects were 75 years or older. No overall differences in safety or effectiveness were observed between older and younger subjects who received guselkumab. However, the number of subjects aged 65 years and older was not sufficient to determine whether they respond differently from younger subjects.
Gender
There is no FDA guidance on the use of Guselkumab with respect to specific gender populations.
Race
There is no FDA guidance on the use of Guselkumab with respect to specific racial populations.
Renal Impairment
There is no FDA guidance on the use of Guselkumab in patients with renal impairment.
Hepatic Impairment
There is no FDA guidance on the use of Guselkumab in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Guselkumab in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Guselkumab in patients who are immunocompromised.
Administration and Monitoring
Administration
Important Administration Instructions
- Administer guselkumab subcutaneously. Each prefilled syringe is for single-dose only. Instruct patients to inject the full amount (1 mL), which provides 100 mg of guselkumab.
- Do not inject guselkumab into areas where the skin is tender, bruised, red, hard, thick, scaly, or affected by psoriasis.
- Guselkumab is intended for use under the guidance and supervision of a physician. guselkumab may be administered by a health care professional, or a patient may self-inject after proper training in subcutaneous injection technique.
- The guselkumab Instructions for Use contains more detailed patient instructions on the preparation and administration of guselkumab.
Preparation for Use of Guselkumab Prefilled Syringe
- Before injection, remove guselkumab prefilled syringe from the refrigerator and allow guselkumab to reach room temperature (30 minutes) without removing the needle cap.
- Inspect guselkumab visually for particulate matter and discoloration prior to administration. Guselkumab is a clear and colorless to light yellow solution that may contain small translucent particles. Do not use if the liquid contains large particles, is discolored or cloudy. Guselkumab does not contain preservatives; therefore, discard any unused product remaining in the prefilled syringe.
Instructions for Use

Monitoring
There is limited information regarding Guselkumab Monitoring in the drug label.
IV Compatibility
There is limited information regarding the compatibility of Guselkumab and IV administrations.
Overdosage
- In the event of overdosage, monitor the patient for any signs or symptoms of adverse reactions and administer appropriate symptomatic treatment immediately.
Pharmacology
Mechanism of Action
- Guselkumab is a human monoclonal IgG1λ antibody that selectively binds to the p19 subunit of interleukin 23 (IL-23) and inhibits its interaction with the IL-23 receptor. IL-23 is a naturally occurring cytokine that is involved in normal inflammatory and immune responses. Guselkumab inhibits the release of proinflammatory cytokines and chemokines.
Structure
(Description with picture)
Pharmacodynamics
- Guselkumab reduced serum levels of IL-17A, IL-17F and IL-22 relative to pretreatment levels in evaluated subjects with psoriasis based on exploratory analysis of the pharmacodynamic markers. The relationship between these pharmacodynamic markers and the mechanism(s) by which guselkumab exerts its clinical effects is not fully understood.
Pharmacokinetics
- Guselkumab exhibited linear pharmacokinetics in healthy subjects and subjects with psoriasis following subcutaneous injections. In subjects with psoriasis, following subcutaneous administration of 100 mg of guselkumab at Weeks 0 and 4, and every 8 weeks thereafter, mean steady-state trough serum guselkumab concentration was approximately 1.2 mcg/mL.
Absorption
- Following a single 100 mg subcutaneous injection in healthy subjects, guselkumab reached a mean (± SD) maximum serum concentration of 8.09 ± 3.68 mcg/mL by approximately 5.5 days post dose. The absolute bioavailability of guselkumab following a single 100 mg subcutaneous injection was estimated to be approximately 49% in healthy subjects.
Distribution
- In subjects with plaque psoriasis, apparent volume of distribution was 13.5 L.
Elimination
- Apparent clearance in subjects with plaque psoriasis was 0.516 L/day. Mean half-life of guselkumab was approximately 15 to 18 days in subjects with plaque psoriasis across studies.
Metabolism
- The exact pathway through which guselkumab is metabolized has not been characterized. As a human IgG monoclonal antibody, guselkumab is expected to be degraded into small peptides and amino acids via catabolic pathways in the same manner as endogenous IgG.
Specific Populations
- No apparent differences in clearance were observed in subjects ≥ 65 years of age compared to subjects < 65 years of age, suggesting no dose adjustment is needed for elderly patients. Clearance and volume of distribution of guselkumab increases as body weight increases, however, observed clinical trial data indicate that dose adjustment for body weight is not warranted. No specific studies have been conducted to determine the effect of renal or hepatic impairment on the pharmacokinetics of guselkumab.
Drug Interactions
- Population pharmacokinetic analyses indicated that concomitant use of ibuprofen, acetylsalicylic acid, or acetaminophen did not affect the clearance of guselkumab.
Cytochrome P450 Substrates
- The effects of guselkumab on the pharmacokinetics of midazolam (metabolized by CYP3A4), warfarin (metabolized by CYP2C9), omeprazole (metabolized by CYP2C19), dextromethorphan (metabolized by CYP2D6), and caffeine (metabolized by CYP1A2) were evaluated in an exploratory study with 6 to 12 evaluable subjects with moderate-to-severe plaque psoriasis. Changes in AUCinf of midazolam, S-warfarin, omeprazole, and caffeine after a single dose of guselkumab were not clinically relevant. For dextromethorphan, changes in AUCinf after guselkumab were not clinically relevant in 9 out of 10 subjects; however, a 2.9-fold change in AUCinf was observed in one individual.
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
- Animal studies have not been conducted to evaluate the carcinogenic or mutagenic potential of guselkumab.
- No effects on fertility parameters were observed after male guinea pigs were subcutaneously administered guselkumab at a dose of 25 mg/kg twice weekly (15 times the MRHD based on a mg/kg comparison).
- No effects on fertility parameters were observed after female guinea pigs were subcutaneously administered guselkumab at doses up to 100 mg/kg twice-weekly (60 times the MRHD based on a mg/kg comparison).
Clinical Studies
- Three multicenter, randomized, double-blind trials (VOYAGE 1 [NCT02207231], VOYAGE 2 [NCT02207244], and NAVIGATE [NCT02203032]) enrolled subjects 18 years of age and older with moderate-to-severe plaque psoriasis who were eligible for systemic therapy or phototherapy. Subjects had an Investigator's Global Assessment (IGA) score of ≥3 ("moderate") on a 5-point scale of overall disease severity, a Psoriasis Area and Severity Index (PASI) score ≥12, and a minimum affected body surface area (BSA) of 10%. Subjects with guttate, erythrodermic, or pustular psoriasis were excluded.
VOYAGE 1 and VOYAGE 2
- In VOYAGE 1 and VOYAGE 2, 1443 subjects were randomized to either guselkumab (100 mg at Weeks 0 and 4 and every 8 weeks thereafter), placebo or U.S. licensed adalimumab (80 mg at Week 0 and 40 mg at Week 1, followed by 40 mg every other week thereafter).
- Both trials assessed the responses at Week 16 compared to placebo for the two co-primary endpoints:
- the proportion of subjects who achieved an IGA score of 0 ("cleared") or 1 ("minimal");
- the proportion of subjects who achieved at least a 90% reduction from baseline in the PASI composite score (PASI 90).
- Comparisons between guselkumab and U.S. licensed adalimumab were secondary endpoints at the following time points:
- at Week 16 (VOYAGE 1 and VOYAGE 2), the proportions of subjects who achieved an IGA score of 0 or 1, a PASI 90, and a PASI 75 response;
- at Week 24 (VOYAGE 1 and VOYAGE 2), and at Week 48 (VOYAGE 1), the proportions of subjects achieving an IGA score of 0, an IGA score of 0 or 1, and a PASI 90 response.
- Other evaluated outcomes included improvement in psoriasis symptoms assessed on the Psoriasis Symptoms and Signs Diary (PSSD) and improvements in psoriasis of the scalp at Week 16.
- In both trials, subjects were predominantly men and white, with a mean age of 44 years and a mean weight of 90 kg. At baseline, subjects had a median affected BSA of approximately 21%, a median PASI score of 19, and 18% had a history of psoriatic arthritis. Approximately 24% of subjects had an IGA score of severe. In both trials, 23% had received prior biologic systemic therapy.
Clinical Response
- Table 2 presents the efficacy results at Week 16 in VOYAGE 1 and VOYAGE 2.

- Table 3 presents the results of an analysis of all the North America sites (i.e., U.S. and Canada), demonstrating superiority of guselkumab to U.S. licensed adalimumab.

- An improvement was seen in psoriasis involving the scalp in subjects randomized to guselkumab compared to placebo at Week 16.
- Examination of age, gender, race, body weight, and previous treatment with systemic or biologic agents did not identify differences in response to guselkumab among these subgroups.
Maintenance and Durability of Response
- To evaluate maintenance and durability of response (VOYAGE 2), subjects randomized to guselkumab at Week 0 and who were PASI 90 responders at Week 28 were re-randomized to either continue treatment with guselkumab every 8 weeks or be withdrawn from therapy (i.e. receive placebo).
- At Week 48, 89% of subjects who continued on guselkumab maintained PASI 90 compared to 37% of subjects who were re-randomized to placebo and withdrawn from guselkumab. For responders at Week 28 who were re-randomized to placebo and withdrawn from guselkumab, the median time to loss of PASI 90 was approximately 15 weeks.
Patient Reported Outcomes
- Greater improvements in symptoms of psoriasis (itch, pain, stinging, burning and skin tightness) at Week 16 in guselkumab compared to placebo were observed in both trials based on the Psoriasis Symptoms and Signs Diary (PSSD). Greater proportions of subjects on guselkumab compared to U.S. licensed adalimumab achieved a PSSD symptom score of 0 (symptom-free) at Week 24 in both trials.
NAVIGATE
- NAVIGATE evaluated the efficacy of 24 weeks of treatment with guselkumab in subjects (N=268) who had not achieved an adequate response, defined as IGA ≥2 at Week 16 after initial treatment with U.S. licensed ustekinumab (dosed 45 mg or 90 mg according to the subject's baseline weight at Week 0 and Week 4). These subjects were randomized to either continue with U.S. licensed ustekinumab treatment every 12 weeks or switch to guselkumab 100 mg at Weeks 16, 20, and every 8 weeks thereafter. Baseline characteristics for randomized subjects were similar to those observed in VOYAGE 1 and VOYAGE 2.
- In subjects with an inadequate response (IGA ≥2 at Week 16 to U.S. licensed ustekinumab), greater proportions of subjects on guselkumab compared to U.S. licensed ustekinumab achieved an IGA score of 0 or 1 with a ≥2 grade improvement at Week 28 (31% vs 14%, respectively; 12 weeks after randomization).
How Supplied
- Guselkumab Injection is a clear and colorless to light yellow solution that may contain small translucent particles. Guselkumab is supplied as a single-dose 100 mg/mL prefilled syringe:
- NDC: 57894-640-01
Storage
- Guselkumab is sterile and preservative-free. Discard any unused portion.
- Store in a refrigerator at 2ºC to 8ºC (36ºF to 46ºF).
- Store in original carton until time of use.
- Protect from light until use.
- Do not freeze.
- Do not shake.
- Keep out of reach of children.
Images
Drug Images
{{#ask: Page Name::Guselkumab |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel

{{#ask: Label Page::Guselkumab |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
- Advise the patient and/or caregiver to read the FDA-approved patient labeling before starting guselkumab therapy, and each time the prescription is renewed, as there may be new information they need to know.
Infections
- Instruct patients of the importance of communicating any history of infections to the healthcare provider and contacting their healthcare provider if they develop any symptoms of an infection
Instruction on Injection Technique
- Instruct the patient or caregivers to perform the first self-injection under the supervision and guidance of a qualified healthcare professional for proper training in subcutaneous injection technique. Instruct patients who are self-administering to inject the full dose of guselkumab.
- Instruct patients or caregivers in the technique of proper needle and syringe disposal. Needles and syringes should be disposed of in a puncture-resistant container. Advise patients and caregivers not to reuse needles or syringes.
- Remind patients if they forget to take their dose of guselkumab to inject their dose as soon as they remember. They should then take their next dose at the appropriate scheduled time.

Precautions with Alcohol
Alcohol-Guselkumab interaction has not been established. Talk to your doctor regarding the effects of taking alcohol with this medication.
Brand Names
- Tremfya
Look-Alike Drug Names
There is limited information regarding Guselkumab Look-Alike Drug Names in the drug label.
Drug Shortage
Price
References
The contents of this FDA label are provided by the National Library of Medicine.