Thrombophilia medical therapy: Difference between revisions
No edit summary |
|||
| Line 26: | Line 26: | ||
'''Treatment algorithms are presented below:''' | '''Treatment algorithms are presented below:''' | ||
[[Image: Thrombophilia_Management_Thrombosis.jpg|thumb|center| | [[Image: Thrombophilia_Management_Thrombosis.jpg|thumb|center|500px|Management of acute thrombosis in patients with inherited thrombophilias]] | ||
[[Image: Thrombophilia_Inherited_Management.jpg|thumb|center|500px|Management of asymptomatic patients with inherited thrombophilias]] | [[Image: Thrombophilia_Inherited_Management.jpg|thumb|center|500px|Management of asymptomatic patients with inherited thrombophilias]] | ||
Revision as of 05:39, 19 July 2016
|
Thrombophilia Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Thrombophilia medical therapy On the Web |
|
American Roentgen Ray Society Images of Thrombophilia medical therapy |
|
Risk calculators and risk factors for Thrombophilia medical therapy |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Asiri Ediriwickrema, M.D., M.H.S. [2]
Overview
The treatment for thrombophilia depends on the underlying hypercoagulable state and the clinical presentation.[1][2][3] The mainstay of therapy for thrombophilia is anticoagulation with either warfarin, low molecular weight heparin, direct Xa inhibitors, or direct thrombin inhibitors.[4][5][6] Treatment should be tailored to the individual patient. The risks and benefits, required monitoring, and costs associated with each form of anticoagulation should be discussed with the patient prior to initiation of therapy. All patients on anticoagulation should be monitored for bleeding.
Medical Therapy
- Patients with provoked venous thrombosis from reversible risk factors should receive 3-6 months of anticoagulation[4]
- Response to anticoagulation can be monitored clinically, with repeat ultrasongraphy for deep vein thrombosis or measuring D-dimer levels after treatment
- Direct oral anticoagulants, including direct Xa inhibitors and direct thrombin inhibitors, should be used for long term treatment of most patients[4]
- Low molecular weight heparin is recommended for anticoagulation for the following acquired thrombophilias:
- Post-surgery prophylaxis[9][10][11]
- The duration of anticoagulation after surgery is variable. Most clinical trials have evaluated anticoagulation for 10-35 days
- General recommendations for thrombophrophylaxis is 7-10 days for standard risk patients and 10-35 days for higher risk patients as described in the algorithims below and for patients undergoing abdominal and pelvic surgeries for gynecologic malginancies[12]
- Pregnancy and postpartum[7]
- Patients who develop acute thrombosis during pregnancy should be anticoagulated for the remainder of the their pregnancy and 6 weeks postpartum for a minimum of 3 months
- A similar duration of anticoagulation is recommended for patients with high risk thrombophilias as described in the algorithims below
- Malignancy[8]
- Alternative agents include Warfarin and Fondaparinux
- Post-surgery prophylaxis[9][10][11]
Treatment algorithms are presented below:
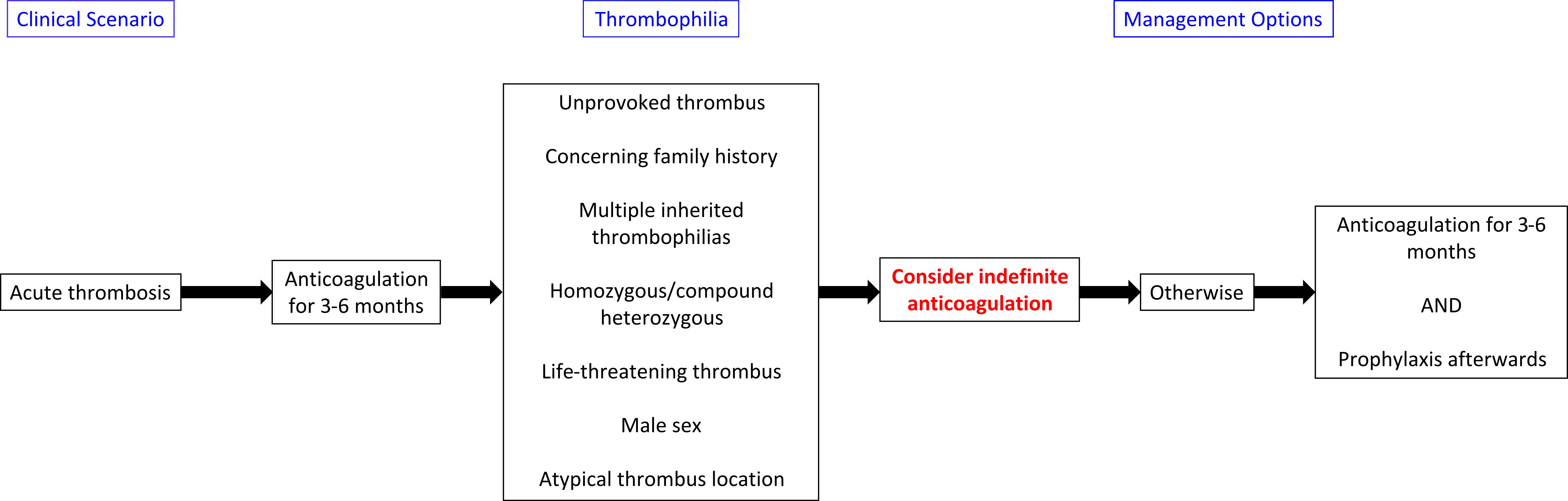
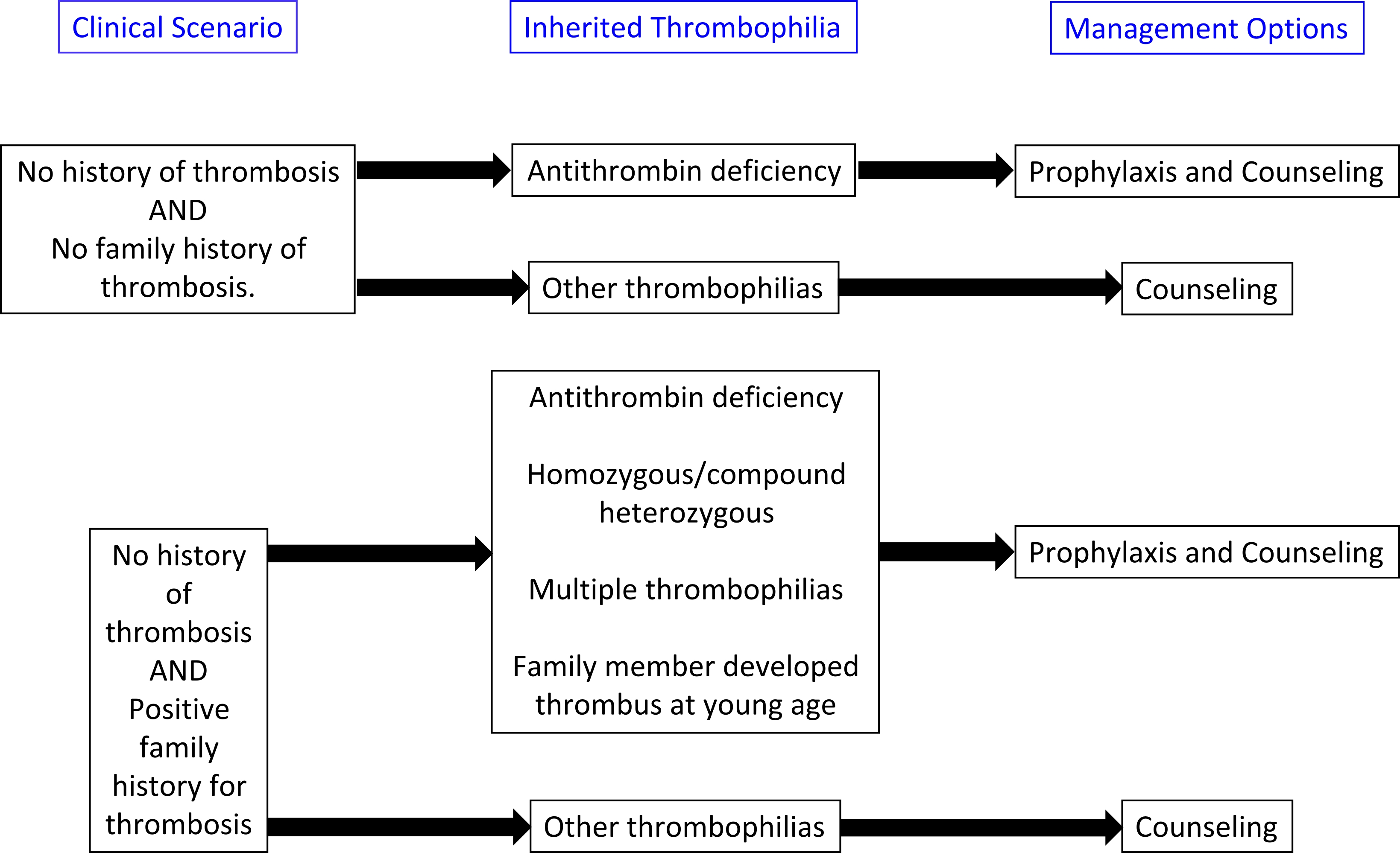
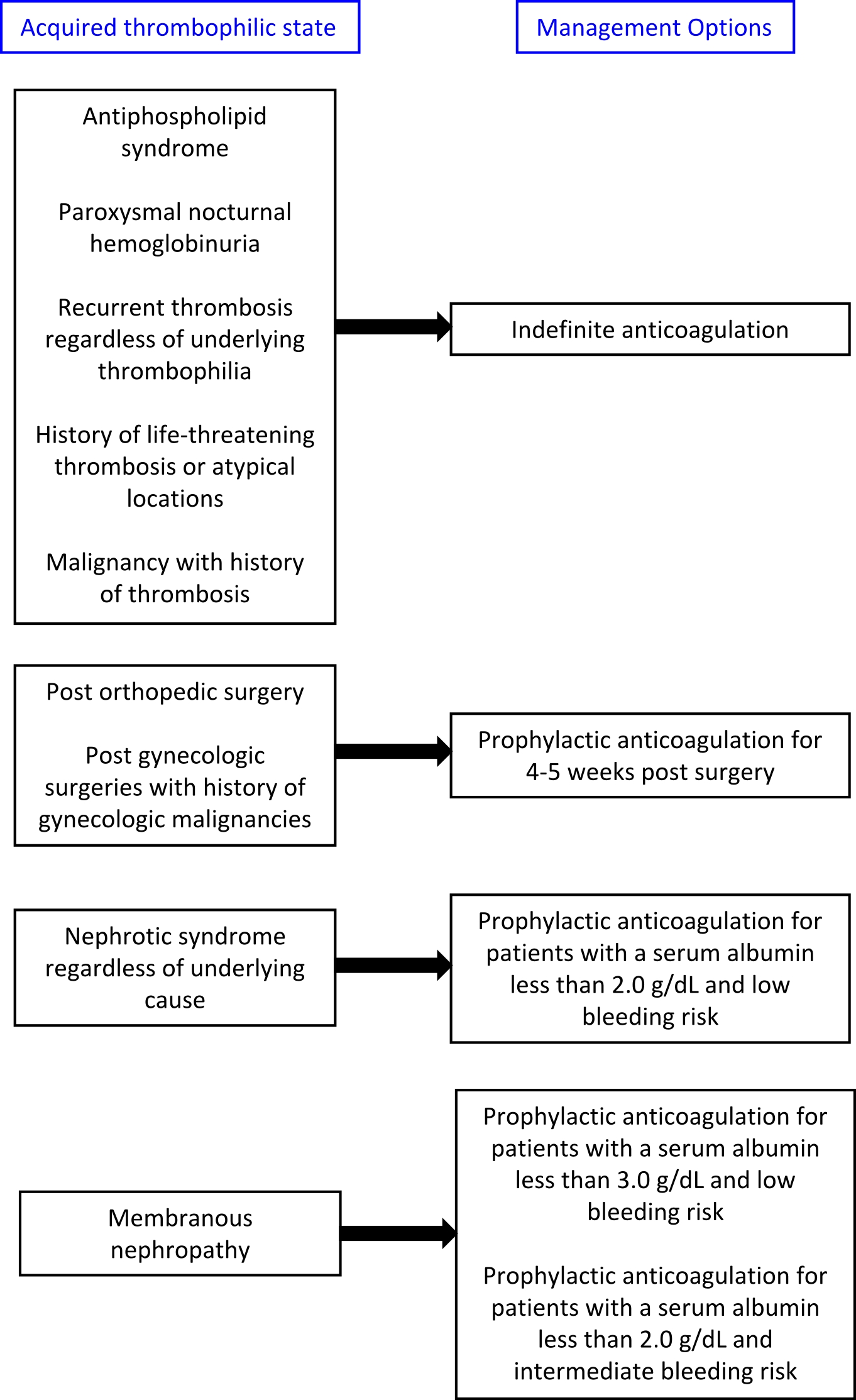
References
- ↑ DeLoughery TG. Hemostasis and Thrombosis: Springer International Publishing; 2014.
- ↑ Cohoon KP, Heit JA (2014). "Inherited and secondary thrombophilia". Circulation. 129 (2): 254–7. doi:10.1161/CIRCULATIONAHA.113.001943. PMC 3979345. PMID 24421360.
- ↑ Seligsohn U, Lubetsky A (2001). "Genetic susceptibility to venous thrombosis". N Engl J Med. 344 (16): 1222–31. doi:10.1056/NEJM200104193441607. PMID 11309638.
- ↑ 4.0 4.1 4.2 Streiff MB, Agnelli G, Connors JM, Crowther M, Eichinger S, Lopes R; et al. (2016). "Guidance for the treatment of deep vein thrombosis and pulmonary embolism". J Thromb Thrombolysis. 41 (1): 32–67. doi:10.1007/s11239-015-1317-0. PMC 4715858. PMID 26780738.
- ↑ Martinelli I, Franchini M, Mannucci PM (2008). "How I treat rare venous thromboses". Blood. 112 (13): 4818–23. doi:10.1182/blood-2008-07-165969. PMID 18805965.
- ↑ De Stefano V, Grandone E, Martinelli I (2013). "Recommendations for prophylaxis of pregnancy-related venous thromboembolism in carriers of inherited thrombophilia. Comment on the 2012 ACCP guidelines". J Thromb Haemost. 11 (9): 1779–81. doi:10.1111/jth.12330. PMID 23789890.
- ↑ 7.0 7.1 Bates SM, Greer IA, Middeldorp S, Veenstra DL, Prabulos AM, Vandvik PO; et al. (2012). "VTE, thrombophilia, antithrombotic therapy, and pregnancy: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest. 141 (2 Suppl): e691S–736S. doi:10.1378/chest.11-2300. PMC 3278054. PMID 22315276.
- ↑ 8.0 8.1 Lee AY, Levine MN, Baker RI, Bowden C, Kakkar AK, Prins M; et al. (2003). "Low-molecular-weight heparin versus a coumarin for the prevention of recurrent venous thromboembolism in patients with cancer". N Engl J Med. 349 (2): 146–53. doi:10.1056/NEJMoa025313. PMID 12853587. Review in: ACP J Club. 2004 Jan-Feb;140(1):10 Review in: J Fam Pract. 2003 Nov;52(11):843-4
- ↑ Falck-Ytter Y, Francis CW, Johanson NA, Curley C, Dahl OE, Schulman S; et al. (2012). "Prevention of VTE in orthopedic surgery patients: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest. 141 (2 Suppl): e278S–325S. doi:10.1378/chest.11-2404. PMC 3278063. PMID 22315265.
- ↑ Bergqvist D, Agnelli G, Cohen AT, Eldor A, Nilsson PE, Le Moigne-Amrani A; et al. (2002). "Duration of prophylaxis against venous thromboembolism with enoxaparin after surgery for cancer". N Engl J Med. 346 (13): 975–80. doi:10.1056/NEJMoa012385. PMID 11919306.
- ↑ Agnelli G (2004). "Prevention of venous thromboembolism in surgical patients". Circulation. 110 (24 Suppl 1): IV4–12. doi:10.1161/01.CIR.0000150639.98514.6c. PMID 15598646.
- ↑ Muntz J (2010). "Duration of deep vein thrombosis prophylaxis in the surgical patient and its relation to quality issues". Am J Surg. 200 (3): 413–21. doi:10.1016/j.amjsurg.2009.05.045. PMID 20409525.