Skin grafting
|
WikiDoc Resources for Skin grafting |
|
Articles |
|---|
|
Most recent articles on Skin grafting Most cited articles on Skin grafting |
|
Media |
|
Powerpoint slides on Skin grafting |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Skin grafting at Clinical Trials.gov Trial results on Skin grafting Clinical Trials on Skin grafting at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Skin grafting NICE Guidance on Skin grafting
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Skin grafting Discussion groups on Skin grafting Patient Handouts on Skin grafting Directions to Hospitals Treating Skin grafting Risk calculators and risk factors for Skin grafting
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Skin grafting |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: Michel C. Samson, M.D., FRCSC, FACS [1]
Please Take Over This Page and Apply to be Editor-In-Chief for this topic: There can be one or more than one Editor-In-Chief. You may also apply to be an Associate Editor-In-Chief of one of the subtopics below. Please mail us [2] to indicate your interest in serving either as an Editor-In-Chief of the entire topic or as an Associate Editor-In-Chief for a subtopic. Please be sure to attach your CV and or biographical sketch.
Overview
Skin grafting is a type of medical grafting involving the transplantation of skin. The transplanted tissue is called a skin graft.
Skin grafting is often used to treat:
- Extensive wounding or trauma
- Burns
- Areas of prior infection with extensive skin loss
- Specific surgeries that may require skin grafts for healing to occur
Skin grafts are often employed after serious injuries when some of the body's skin is damaged. Surgical removal (excision or debridement) of the damaged skin is followed by skin grafting. The grafting serves two purposes: it can reduce the course of treatment needed (and time in the hospital), and it can improve the function and appearance of the area of the body which receives the skin graft. There are two types of skin grafts, the more common type is where a thin layer is removed from a healthy part of the (body the donor section) like peeling a potato, (see donor section) or a full thickness skin graft, which involves pitching and cutting skin away from the donor section. A full thickness skin graft is more risky, in terms of the body accepting the skin, yet it leaves only a scar line on the donor section, similar to a Cesarean section scar. For full thickness skin grafts, the donor section will often heal a lot quicker then injury. and not only heals quicker but is less painful then a partial thickness skin graft.
Graft taxonomy
- Autologous: The donor and recipient are the same (also known as an autograft).
- Isogeneic: The donor and recipient are genetically identical (e.g., monozygotic twins, animals of a single inbred strain; isograft or syngraft).
- Allogeneic: The donor and recipient are of the same species (human→human, dog→dog; allograft).
- Xenogeneic: The donor and recipient are of different species (e.g., bovine cartilage; xenograft or heterograft).
- Prosthetic: Lost tissue is replaced with synthetic materials such as metal, plastic, or ceramic (prosthetic implants).[1]
Donor selection
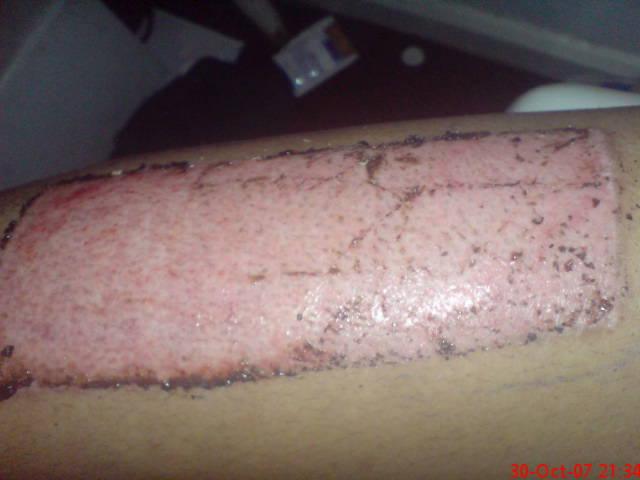
-
Skin Graft Donor site 8 days after the skin was taken
When grafts are taken from other animals, they are known as heterografts or xenografts. By definition, they are temporary biologic dressings which the body will reject within days to a few weeks. They are useful in reducing the bacterial concentration of an open wound, as well as reducing fluid loss.
For more extensive tissue loss, a full-thickness skin graft, which includes the entire thickness of the skin, may be necessary. This is often performed for defects of the face and hand where contraction of the graft should be minimized. The general rule is that the thicker the graft, the less the contraction and deformity.
Cell cultured epithelial autograft (CEA) procedures take skin cells from the patient to grow new skin cells in sheets in a laboratory. The new sheets are used as grafts, and because the original skin cells came from the patient, the body does not reject them. Because these grafts are very thin (only a few cell layers thick) they do not stand up to trauma, and the "take" is often less than 100%. Newer grafting procedures combine CEA with a dermal matrix for more support. Research is investigating the possibilities of combining CEA and a dermal matrix in one product.
Surgical procedure
In order to remove the thin and well preserved skin slices and stripes from the donor, surgeons use a special surgical instrument called a dermatome. This usually produces a split-thickness skin graft, which contains the epidermis with only a portion of the dermis. The dermis left behind at the donor site contains hair follicles and sebaceous glands, both of which contain epidermal cells which gradually proliferate out to form a new layer of epidermis. The donor site may be extremely painful and vulnerable to infection.
The graft is carefully spread on the bare area to be covered. It is held in place by a few small stitches or surgical staples. The graft is initially nourished by a process called plasmatic imbibition in which the graft literally "drinks plasma". New blood vessels begin growing from the recipient area into the transplanted skin within 36 hours in a process called capillary inosculation. To prevent the accumulation of fluid under the graft which can prevent its attachment and revascularization, the graft is frequently meshed by making lengthwise rows of short, interrupted cuts, each a few millimeters long, with each row offset by half a cut length like bricks in a wall. In addition to allowing for drainage, this allows the graft to both stretch and cover a larger area as well as to more closely approximate the contours of the recipient area.
An increasingly common aid to both pre-operative wound maintenance and post-operative graft healing is the use of negative pressure wound therapy (NPWT). This system works by placing a section of foam cut to size over the wound, then laying a perforated tube onto the foam. The arrangement is then secured with bandages. A vacuum unit then creates negative pressure, sealing the edges of the wound to the foam, and drawing out excess blood and fluids. This process typically helps to maintain cleanliness in the graft site, promotes the development of new blood vessels, and increases the chances of the graft successfully taking. NPWT can also be used between debridement and graft operations to assist an infected wound in remaining clean for a period of time before new skin is applied.
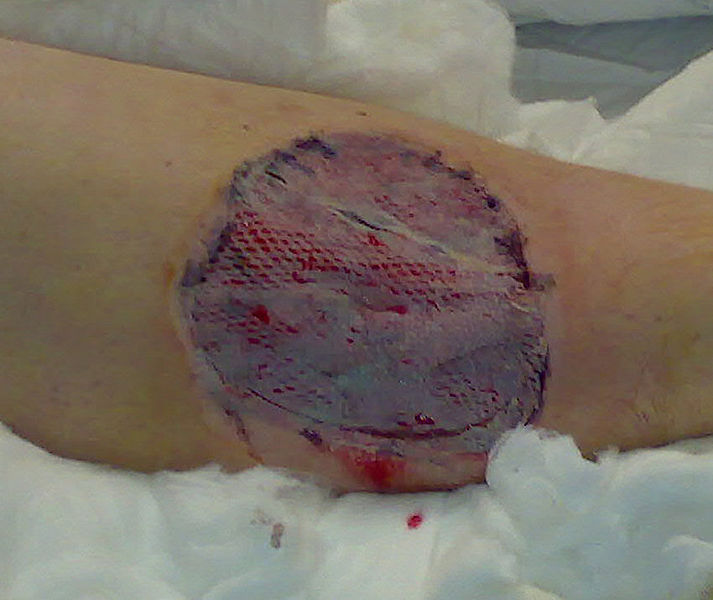
-
Skin graft on lower leg trauma injury, some 5 days after surgery. Take and healing aided by use of Vacuum Assisted Closure.
Risks
Risks for the skin graft surgery are:
- Bleeding
- Infection
- Loss of grafted skin
- Nerve damage
Rejection may occur in xenografts. To prevent this, the patient usually must be treated with long-term immunosuppressant drugs.
Prognosis
Most skin grafts are successful, but in some cases they do not heal well and require repeat grafting. The graft should also be monitored for good circulation. The recovery from surgery is usually rapid after split thickness skin grafting. The skin graft must be protected from trauma or significant stretching for 2-3 weeks. Depending on the location of the graft, a dressing may be necessary for 1-2 weeks. Exercise that might stretch or injure the graft should be avoided for 3-4 weeks.
External links
- Skin graft. MedlinePlus Medical Encyclopedia. Parts of this US Federal Government public domain text were used in the article.
- An introduction to the use of vacuum assisted closure.
References
- ↑ Hilko Weerda, Reconstructive Facial Plastic Surgery: A Problem-Solving Manual (2001), ISBN 1588900762
Template:Organ transplantation Template:Operations and other procedures of the integumentary system
|
Cleft lip and palate Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Skin grafting On the Web |
|
American Roentgen Ray Society Images of Skin grafting |