Herpes zoster pathophysiology
|
Herpes zoster Microchapters |
|
Diagnosis |
|---|
|
History and Symptoms |
|
Treatment |
|
Case Studies |
|
Herpes zoster pathophysiology On the Web |
|
American Roentgen Ray Society Images of Herpes zoster pathophysiology |
|
Risk calculators and risk factors for Herpes zoster pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; L. Katie Morrison, MD; Associate Editor(s)-In-Chief: Cafer Zorkun, M.D., Ph.D. [2]
Nomenclature
Multiple names are used to refer to same virus, creating some confusion. Varicella virus, zoster virus, human herpes 3 (HHV-3), and Varicella Zoster Virus (VZV) all refer to the same viral pathogen. The disease caused by this pathogen is called chickenpox or Varicella disease during the initial infection. A reactivation of the infection is commonly called shingles, herpes zoster or simply zoster.
Morphology
VZV is closely related to the herpes simplex viruses (HSV), sharing much genome homology. The known envelope glycoproteins (gB, gC, gE, gH, gI, gK, gL) correspond with those in HSV, however there is no equivalent of HSV gD. VZV virons are spherical and 150-200 nm in diameter. Their lipid envelope encloses the nucleocapsid of 162 capsomeres arranged in a hexagonal form. Its DNA is a single, linear, double-stranded molecule, 125,000 nt long.
The virus is very susceptible to disinfectants, notably sodium hypochlorite. Within the body it can be treated by a number of drugs and therapeutic agents including aciclovir, zoster-immune globulin (ZIG), and vidarabine.
Human disease
Primary VZV infection results in chickenpox (varicella), which may rarely result in complications including VZV encephalitis or pneumonia. Even when clinical symptoms of varicella have resolved, VZV remains dormant in the nervous system of the host in the trigeminal and dorsal root ganglia. In about 10-20% of cases, VZV reactivates later in life producing a disease known as herpes zoster or shingles. Serious complications of shingles include post-herpetic neuralgia, zoster multiplex, myelitis, herpes ophthalmicus, or zoster sine herpete.
Pathophysiology
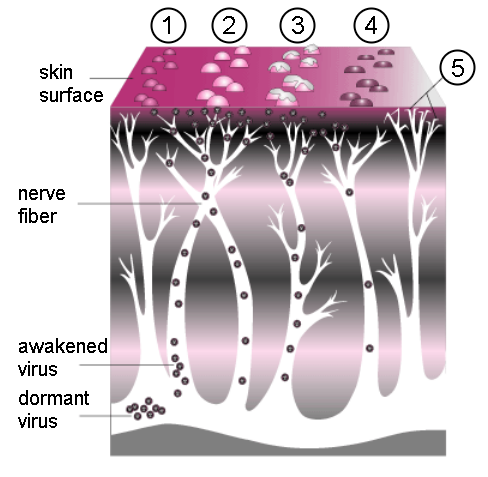
The causative agent for herpes zoster is varicella zoster virus (VZV), a double-stranded DNA virus related to the Herpes simplex virus group. Most people are infected with this virus as children, and suffer from an episode of chickenpox. The immune system eventually eliminates the virus from most locations, but it remains dormant (or latent) in the ganglia adjacent to the spinal cord (called the dorsal root ganglion) or the ganglion semilunare (ganglion Gasseri) in the base of the skull.[1] However, repeated attacks of herpes zoster are rare,[2] and it is extremely rare for patients to suffer more than three recurrences.[1]
Herpes zoster occurs only in people who have had chickenpox, and although it can occur at any age, the majority of sufferers are more than 50 years old.[3] The disease results from the virus reactivating in a single sensory ganglion.[4] In contrast to Herpes simplex virus, the latency of VZV is poorly understood. The virus has not been recovered from human nerve cells by cell culture and the location and structure of the viral DNA is not known. Virus-specific proteins continue to be made by the infected cells during the latent period, so true latency, as opposed to a chronic low-level infection, has not been proven.[5][6] Although VZV has been detected in autopsies of nervous tissue, there are no methods to find dormant virus in the ganglia in living people.
Unless the immune system is compromised, it suppresses reactivation of the virus and prevents herpes zoster. Why this suppression sometimes fails is poorly understood,[7] but herpes zoster is more likely to occur in people whose immune system is impaired due to aging, immunosuppressive therapy, psychological stress, or other factors.[8] Upon reactivation, the virus replicates in the nerve cells, and virions are shed from the cells and carried down the axons to the area of skin served by that ganglion. In the skin, the virus causes local inflammation and blisters. The short and long-term pain caused by herpes zoster comes from the widespread growth of the virus in the infected nerves, which causes inflammation.[9]
The symptoms of herpes zoster cannot be transmitted to another person.[10] However, during the blister phase, direct contact with the rash can spread VZV to a person who has no immunity to the virus. This newly-infected individual may then develop chickenpox, but will not immediately develop shingles. Until the rash has developed crusts, a person is extremely contagious. A person is also not infectious before blisters appear, or during postherpetic neuralgia (pain after the rash is gone). The person is no longer contagious after the virus has disappeared.[11]
References
- ↑ 1.0 1.1 Steiner I, Kennedy PG, Pachner AR (2007). "The neurotropic herpes viruses: herpes simplex and varicella-zoster". Lancet Neurol. 6 (11): 1015–28. doi:10.1016/S1474-4422(07)70267-3. PMID 17945155.
- ↑ Stankus, SJ (2000). "Management of Herpes Zoster (Shingles) and Postherpetic Neuralgia". American Family Physician. 61 (8): 2437–2447. PMID 10794584. Retrieved 2007-04-08. Unknown parameter
|coauthors=ignored (help) - ↑ Weinberg JM (2007). "Herpes zoster: epidemiology, natural history, and common complications". J Am Acad Dermatol. 57 (6 Suppl): S130–5. doi:10.1016/j.jaad.2007.08.046. PMID 18021864.
- ↑ Gilden DH, Cohrs RJ, Mahalingam R (2003). "Clinical and molecular pathogenesis of varicella virus infection". Viral Immunol. 16 (3): 243–58. doi:10.1089/088282403322396073. PMID 14583142.
- ↑ Kennedy PG (2002). "Varicella-zoster virus latency in human ganglia". Rev. Med. Virol. 12 (5): 327–34. doi:10.1002/rmv.362. PMID 12211045.
- ↑ Kennedy PG (2002). "Key issues in varicella-zoster virus latency". J. Neurovirol. 8 Suppl 2: 80–4. doi:10.1080/13550280290101058. PMID 12491156.
- ↑ Donahue JG, Choo PW, Manson JE, Platt R (1995). "The incidence of herpes zoster". Arch. Intern. Med. 155 (15): 1605–9. doi:10.1001/archinte.155.15.1605. PMID 7618983.
- ↑ Thomas SL, Hall AJ (2004). "What does epidemiology tell us about risk factors for herpes zoster?". Lancet Infect Dis. 4 (1): 26–33. doi:10.1016/S1473-3099(03)00857-0. PMID 14720565.
- ↑ Schmader K (2007). "Herpes zoster and postherpetic neuralgia in older adults". Clin. Geriatr. Med. 23 (3): 615–32, vii–viii. doi:10.1016/j.cger.2007.03.003. PMID 17631237.
- ↑ Schmader K (1999). "Herpes zoster in the elderly: issues related to geriatrics". Clin. Infect. Dis. 28 (4): 736–9. doi:10.1086/515205. PMID 10825029.
- ↑ Stankus SJ, Dlugopolski M, Packer D (2000). "Management of herpes zoster (shingles) and postherpetic neuralgia". American Family Physician. 61 (8): 2437–44, 2447–8. PMID 10794584. Retrieved 2012-02-09. Unknown parameter
|month=ignored (help)