Glioblastoma multiforme MRI: Difference between revisions
Jump to navigation
Jump to search
No edit summary |
Farima Kahe (talk | contribs) No edit summary |
||
| (33 intermediate revisions by 4 users not shown) | |||
| Line 1: | Line 1: | ||
__NOTOC__ | __NOTOC__ | ||
{{Glioblastoma multiforme}} | {{Glioblastoma multiforme}} | ||
{{CMG}} | {{CMG}}{{AE}}{{SR}} | ||
==Overview== | ==Overview== | ||
Brain MRI is helpful in the diagnosis of glioblastoma multiforme. On brain MRI, glioblastoma multiforme is characterized by a butterfly shaped mass, which is hypointense on T1-weighted [[MRI]] and hyperintense on T2-weighted MRI. | |||
==MRI== | ==MRI== | ||
Brain MRI is helpful in the diagnosis of glioblastoma multiforme. On brain [[MRI]], glioblastoma multiforme is characterized by: | |||
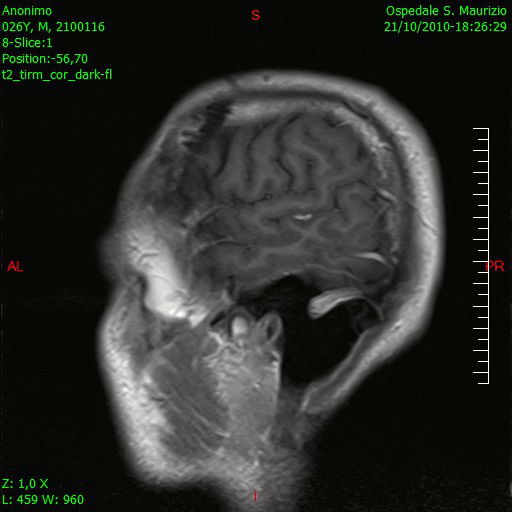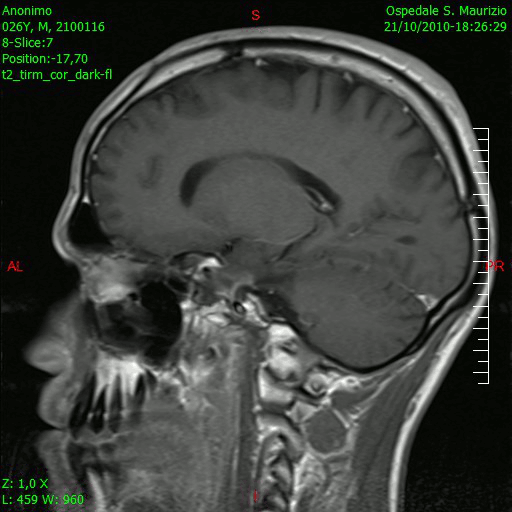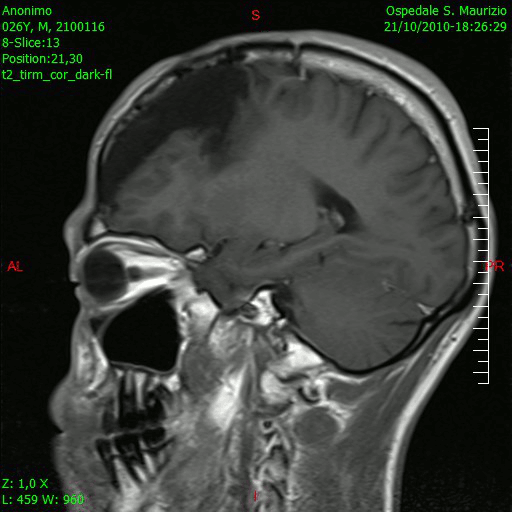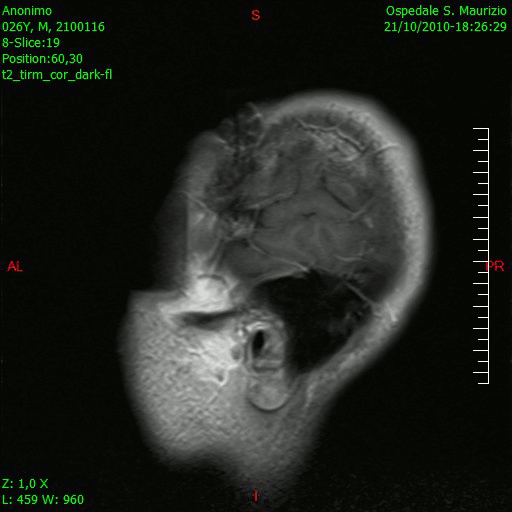
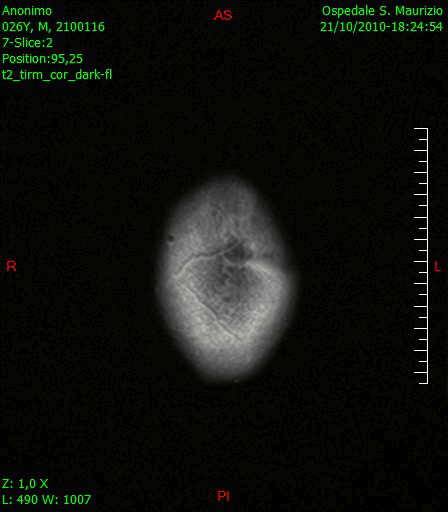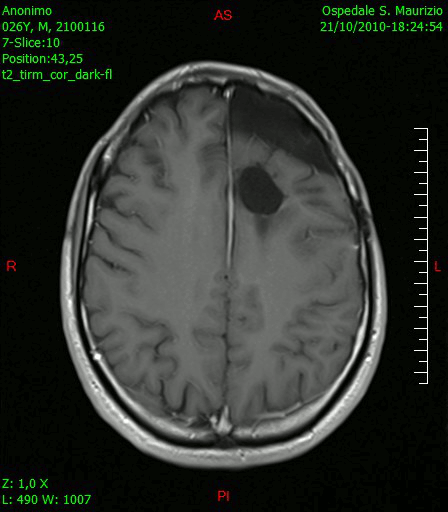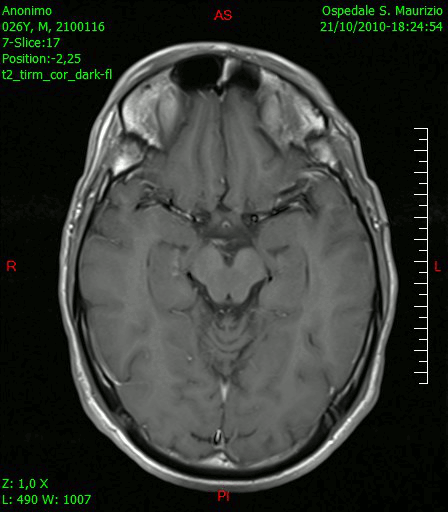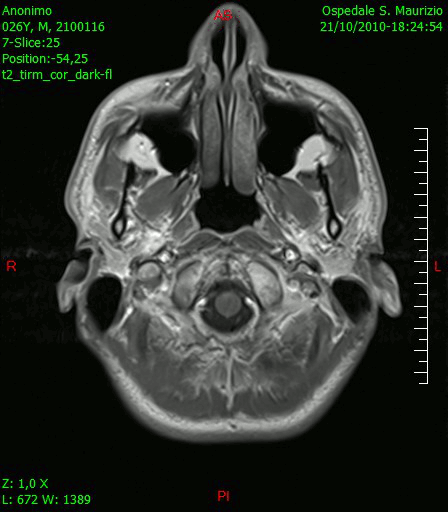
[[File:Glioblastoma-GIF1.gif|thumb|200px|sagital section of brain showing Glioblastoma multiforme [https://upload.wikimedia.org/wikipedia/commons/b/b2/Animazione_RMN_saggittale_dopo_rimozione_glioblastoma.gif Source:Wikimedia Commons] ]] | |||
[[File:GlioblastomaGIF2.gif|thumb|200px|Transverse section of brain showing Glioblastoma multiforme [https://upload.wikimedia.org/wikipedia/commons/c/ce/Animazione_RMN_trasversale_dopo_rimozione_glioblastoma.gif Source:Wikimedia Commons] ]] | |||
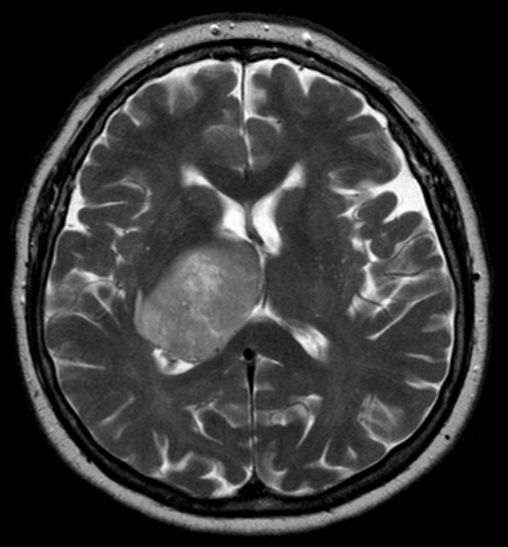
[[File:Glioblastoma multiforme - MRi.jpg|thumb|200px|Transverse section of brain showing Glioblastoma multiforme [https://upload.wikimedia.org/wikipedia/commons/0/0f/Glioblastoma_multiforme_-_MRT_T2_ax.jpg Source:Wikimedia Commons] ]] | |||
{| style="border: 0px; font-size: 90%; margin: 3px; width: 600px" align="center" | |||
| valign="top" | | |||
|+ | |||
! style="background: #4479BA; width: 200px;" | {{fontcolor|#FFF|MRI component}} | |||
! style="background: #4479BA; width: 400px;" | {{fontcolor|#FFF|Features}} | |||
|- | |||
| style="padding: 5px 5px; background: #DCDCDC; font-weight: bold" | | |||
:T1 | |||
| style="padding: 5px 5px; background: #F5F5F5;" | | |||
*Butterfly shaped mass | |||
*Hypo to isointense mass within [[white matter]] | |||
*Central heterogenous signal ([[necrosis]], intratumoral [[hemorrhage]]) | |||
|- | |||
| style="padding: 5px 5px; background: #DCDCDC;font-weight: bold" | | |||
:T1 C+ (Gd) | |||
| style="padding: 5px 5px; background: #F5F5F5;" | | |||
*Enhancement is variable | |||
*Typically peripheral and irregular with [[nodular]] components | |||
*Usually completely surrounds [[necrosis]] | |||
|- | |||
| style="padding: 5px 5px; background: #DCDCDC;font-weight: bold" | | |||
:T2/FLAIR | |||
| style="padding: 5px 5px; background: #F5F5F5;" | | |||
*Hyperintense | |||
*Surrounded by vasogenic [[edema]] | |||
*Flow voids | |||
|- | |||
| style="padding: 5px 5px; background: #DCDCDC;font-weight: bold" | | |||
:GE/SWI | |||
| style="padding: 5px 5px; background: #F5F5F5;" | | |||
*Susceptibility artifact on T2 from blood products (or occasionally [[calcification]]) | |||
*Low intensity rim from blood product | |||
*Located inside the peripheral enhancing component | |||
*Absent dual rim sign | |||
|- | |||
| rowspan="3" style="padding: 5px 5px; background: #DCDCDC;font-weight: bold" |DWI/ADC | |||
| style="padding: 5px 5px; background: #F5F5F5;" | | |||
*Solid component | |||
:* Elevated signal on DWI is common in solid / enhancing component | |||
:* Diffusion restriction is typically intermediate similar to normal [[white matter]], but significantly elevated compared to surrounding vasogenic [[edema]] (which has facilitated diffusion) | |||
|- | |||
| style="padding: 5px 5px; background: #F5F5F5;" | | |||
* ADC values correlate with grade: | |||
:* WHO IV (GBM) = 745 ± 135 x 10-6 mm2/s | |||
:* WHO III (anaplastic) = 1067 ± 276 x 10-6 mm2/s | |||
:* WHO II (low grade) = 1273 ± 293 x 10-6 mm2/s | |||
:* ADC threshold value of 1185 x 10-6 mm2/s sensitivity (97.6%) and specificity (53.1%) in the discrimination of high-grade (WHO grade III & IV) and low-grade (WHO grade II) gliomas | |||
|- | |||
| style="padding: 5px 5px; background: #F5F5F5;" | | |||
* Non-enhancing necrotic / cystic component | |||
:* Majority (>90%) have facilitated diffusion (ADC values > 1000 x 10-6 mm2/s) | |||
|- | |||
| style="padding: 5px 5px; background: #DCDCDC;font-weight: bold" | | |||
:MR perfusion | |||
| style="padding: 5px 5px; background: #F5F5F5;" | | |||
*rCBV elevated compared to lower grade [[tumors]] and normal [[brain]] | |||
|- | |||
| style="padding: 5px 5px; background: #DCDCDC;font-weight: bold" | | |||
:MR spectroscopy | |||
| style="padding: 5px 5px; background: #F5F5F5;" | | |||
*[[Choline]]: increased | |||
*[[Lactate]]: increased | |||
*[[Lipids]]: increased | |||
*[[N-Acetylaspartate|NAA]]: decreased | |||
*[[Myo-inositol]]: decreased | |||
|- | |||
|} | |||
<div align="left"></div> | |||
< | |||
</ | |||
==References== | ==References== | ||
[[Category:Neurosurgery]] | [[Category:Neurosurgery]] | ||
[[Category:Neurology]] | [[Category:Neurology]] | ||
[[Category:Types of cancer]] | [[Category:Types of cancer]] | ||
{{WikiDoc Help Menu}} | {{WikiDoc Help Menu}} | ||
{{WikiDoc Sources}} | {{WikiDoc Sources}} | ||
<references /> | |||
Latest revision as of 23:33, 15 April 2019
|
Glioblastoma multiforme Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Glioblastoma multiforme MRI On the Web |
|
American Roentgen Ray Society Images of Glioblastoma multiforme MRI |
|
Risk calculators and risk factors for Glioblastoma multiforme MRI |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]Associate Editor(s)-in-Chief: Sujit Routray, M.D. [2]
Overview
Brain MRI is helpful in the diagnosis of glioblastoma multiforme. On brain MRI, glioblastoma multiforme is characterized by a butterfly shaped mass, which is hypointense on T1-weighted MRI and hyperintense on T2-weighted MRI.
MRI
Brain MRI is helpful in the diagnosis of glioblastoma multiforme. On brain MRI, glioblastoma multiforme is characterized by:
| MRI component | Features |
|---|---|
|
|
|
|
|
|
|
|
| DWI/ADC |
|
| |
| |
|
|
|
|