Diverticulitis CT
|
Diverticulitis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Diverticulitis CT On the Web |
|
American Roentgen Ray Society Images of Diverticulitis CT |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Cafer Zorkun, M.D., Ph.D. [2]
Overview
The CT scan is very sensitive (98%) in diagnosing diverticulitis. It may also identify patients with more complicated diverticulitis, such as those with an associated abscess. CT also allows for radiologically guided drainage of associated abscesses, possibly sparing a patient from immediate surgical intervention.[1][2][3][4]
Computed Tomography
CT scan is important in diagnosing diverticulitis for further management and treatment. The following can be observed in colon CT imaging:
- Colonic and paracolic inflammation in the presence of underlying diverticula (diverticula are identified on CT scans as outpouchings of the colonic wall).
- Symmetric thickening of the colonic of approximately 4-5 mm is common.
- Enhancement of the colonic wall is commonly noted. This usually has inner and outer high-attenuation layers, with a thick middle layer of low attenuation.
- Free diverticular perforation results in the extravasation of air and fluid into the pelvis and peritoneal cavity.
- Air in the bladder in the presence of a nearby segment of diverticulitis is suggestive of a colovesical fistula.
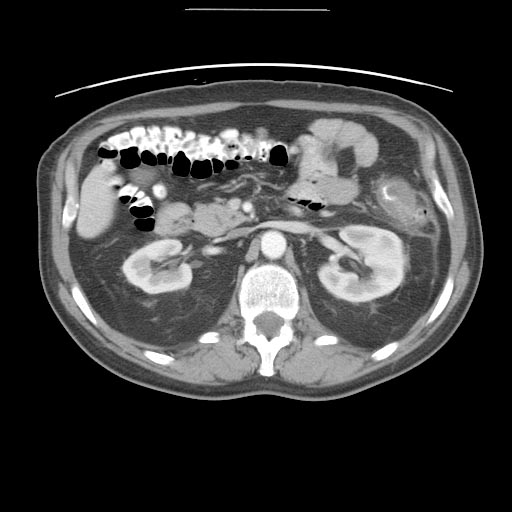
Patient #1: CT images demonstrate diverticulitis
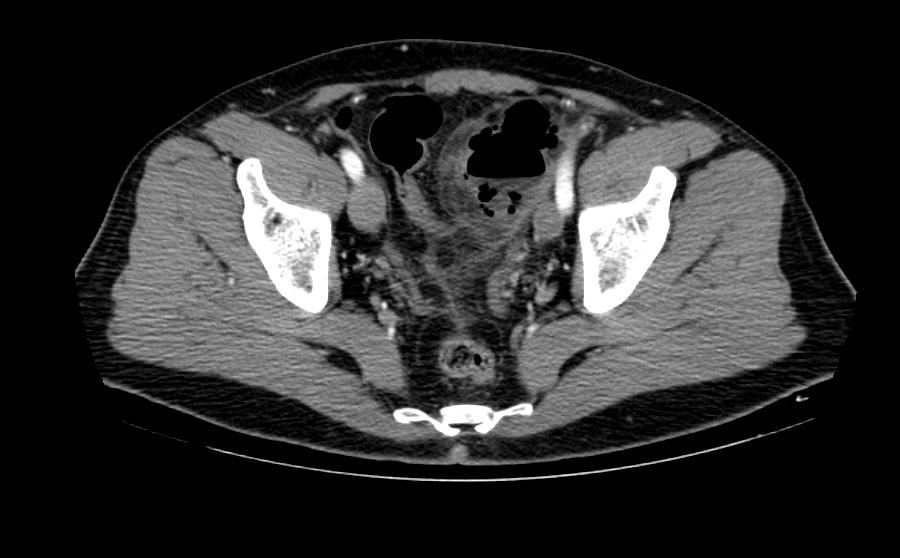
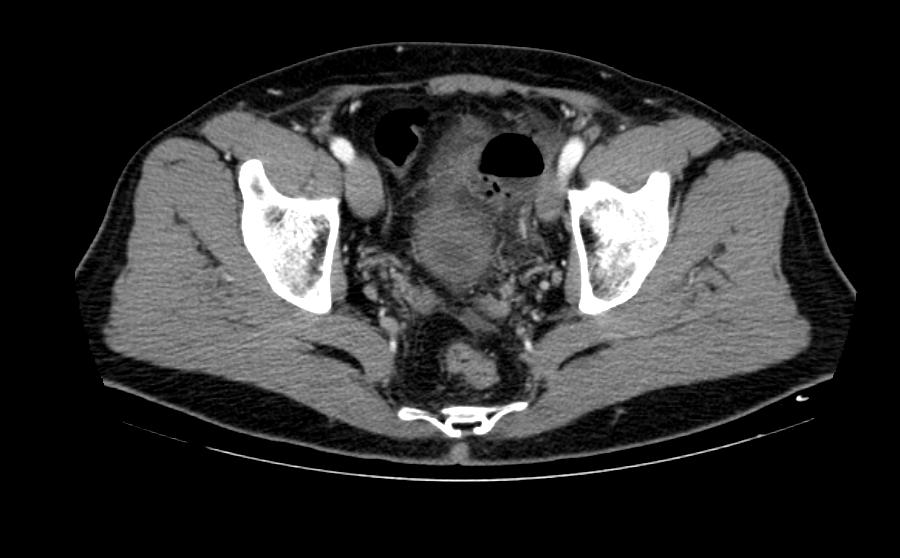
Patient #2: CT images demonstrate a diverticular abscess
References
- ↑ Schreyer AG, Layer G, German Society of Digestive and Metabolic Diseases (DGVS) as well as the German Society of General and Visceral Surgery (DGAV) in collaboration with the German Radiology Society (DRG) (2015). "S2k Guidlines for Diverticular Disease and Diverticulitis: Diagnosis, Classification, and Therapy for the Radiologist". Rofo. 187 (8): 676–84. doi:10.1055/s-0034-1399526. PMID 26019048.
- ↑ Neff CC, vanSonnenberg E (1989). "CT of diverticulitis. Diagnosis and treatment". Radiol Clin North Am. 27 (4): 743–52. PMID 2657852.
- ↑ Ambrosetti P (2016). "Acute left-sided colonic diverticulitis: clinical expressions, therapeutic insights, and role of computed tomography". Clin Exp Gastroenterol. 9: 249–57. doi:10.2147/CEG.S110428. PMC 4993273. PMID 27574459.
- ↑ Andeweg CS, Wegdam JA, Groenewoud J, van der Wilt GJ, van Goor H, Bleichrodt RP (2014). "Toward an evidence-based step-up approach in diagnosing diverticulitis". Scand J Gastroenterol. 49 (7): 775–84. doi:10.3109/00365521.2014.908475. PMID 24874087.