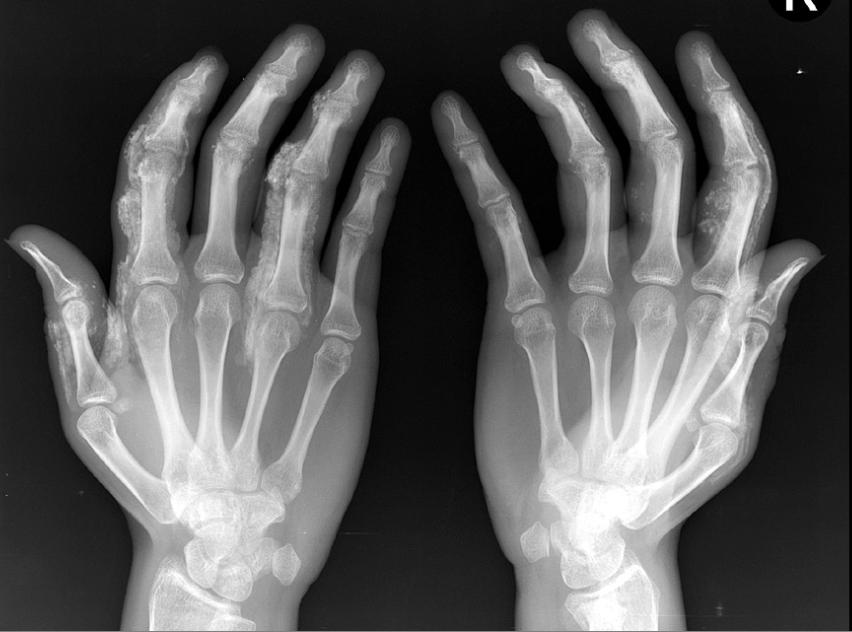
Dermatomyositis
For patient information click here
| Dermatomyositis | |
 | |
|---|---|
| X-Ray of the knee in a patient with dermatomyositis. | |
| ICD-10 | M33.0-M33.1 |
| ICD-9 | 710.3 |
| DiseasesDB | 10343 |
| MedlinePlus | 000839 |
| MeSH | D003882 |
|
Dermatomyositis Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Dermatomyositis On the Web |
|
American Roentgen Ray Society Images of Dermatomyositis |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor-In-Chief: Cafer Zorkun, M.D., Ph.D. [2]
For the heart in Dermatomyositis click here
Overview
Dermatomyositis is connective-tissue disease that is characterized by inflammation of the muscles and the skin. Its cause is unknown, but it may result from either a viral infection or an autoimmune reaction. Up to 50% of the cases may be a paraneoplastic phenomenon, indicating the presence of cancer.
X-ray findings include dystrophic calcifications in the muscles.
There is a form of this disorder that strikes children, known as juvenile dermatomyositis.
"Gottron's papules", pink patches on the knuckles, and priapism, are associated with this disorder.
Differential Diagnosis
Dermatomyositis must be differentiated from other common, lymphocyte predominant inflammatory myopathies. If present, the characteristic perifascicular atrophy makes this distinction trivial.
There is some overlap in the microscopic appearances of different inflammatory myopathies, but some helpful differences are often present.[3] The rimmed vacuoles of inclusion body myositis (IBM) are absent in dermatomyositis. Polymyositis is characterised by diffuse or patchy inflammation of the muscle fascicles, a random pattern of muscle atrophy, and T-cell predominance with T-cells seen invading otherwise viable appearing muscle fibers.[4]
Pathology
The diagnosis of dermatomyositis can be confirmed by muscle biopsy, EMG,and blood tests. It should be noted, however, that only muscle biopsy is truly diagnostic (pathognomic); liver enzymes and EMG are relatively non-specific. Liver enzymes, specificly creatine phosphokinase (CPK), are the major tool in assessing the progress of the disease and/or the efficacy of treatment. On the muscle biopsy, there are two classic microscopic findings of dermatomyositis. They are:
Dermatomyositis is associated with autoantibodies, especially anti-Jo1 antibody.[1]
Mechanism
The mechanism is conjectured to be complement-mediated damage of microscopic vessels with muscle atrophy and lymphocytic inflammation secondary to tissue ischemia.[2]
Classification
Dermatomyositis may be a type of autoimmune connective tissue disease.[3] It is related to polymyositis and inclusion body myositis.
There is a form of this disorder that strikes children, known as juvenile dermatomyositis(JDM). For the most part Juvenile dermatomyositis is the same as the adult form, but the relationship with cancer is far lower, or non-existent.
Causes
The cause is unknown, but it may result from either a viral infection or an autoimmune reaction. Some cases of dermatomyositis actually "overlap" (are combined with) another autoimmune disease such as lupus, scleroderma, or vasculitis. Because of the link between DM and autoimmune disease, doctors and patients suspecting DM may find it helpful to run an ANA - antinuclear antibody - test, which in cases of a lupus-like nature may be positive (usually from 1:160 to 1:640, with normal ranges at 1:40 and below).
Some cases of DM are a paraneoplastic phenomenon, indicating the presence of cancer.[4] In cases involving cancer, the cancer is usually pre-existent, with removal of the cancer resulting in remission of the DM. The onset of a rash in patients with pre-existing myositis requires investigation of the neoplastic possibility.
In 1988, the noted Lyme disease researcher Dr. Alan Steere observed: "Finally, the perivascular lymphoid infiltrate in clinical myositis does not differ from that seen in polymyositis or dermatomyositis. All of these histologic derangements suggest immunologic damage in response to persistence of the spirochete, however few in number.", in his article, Clinical pathologic correlations of Lyme disease by stage.
Microscopic findings
Cross sections of muscle reveal muscle fascicles with small, shrunken polygonal muscle fibers on the periphery of a fascicle surrounding central muscle fibers of normal, uniform size.
Aggregates of mature lymphocytes with small, dark nuclei and scant cytoplasm are seen surrounding vessels. Other inflammatory cells are distinctly uncommon. Immunohistochemistry can be used to demonstrate that both B- and T-cells are present in approximately equal numbers.[5] [6]
Mechanism
The mechanism is conjectured to be complement-mediated damage of microscopic vessels with muscle atrophy and lymphocytic inflammation secondary to tissue ischemia [5].
Presentation
X-ray findings sometimes include dystrophic calcifications in the muscles, and patients may or may not notice small calcium deposits under the skin. Many do not have any calcium deposits of any kind. The rash also may come and go, and may not be dependent on the severity of the muscle involvement at the time. "Gottron's papules", pink patches on the knuckles, and priapism, are associated with this disorder.
Diagnosis
History and Symptoms
The main symptoms include skin rash and symmetric proximal muscle weakness which may be accompanied by pain. The pain may resemble the type experienced after strenuous exercise. Some DM patients have little pain, while in others (esp. in JDM), the pain may be severe. It is important to remember that this condition varies from person to person in many ways.
Skin findings occur in DM but not PM and are generally present at diagnosis. Gottron's sign is an erythematous, scaly eruption occurring in symmetric fashion over the MCP and interphalangeal joints (can mimic psoriasis). Heliotrope rash (or lilac rash) [7] is a violaceous eruption on the upper eyelids, often with swelling (most specific, though uncommon). Shawl (or V-) sign is a diffuse, flat, erythematous lesion over the chest and shoulders or in a "V" over the anterior neck and chest, worsened with UV light. Erythroderma is a flat, erythematous lesion similar to the shawl sign but located in other areas, such as the malar region and the forehead. Periungual telangiectasias and erythema occur.
Mechanic's hands (also in PM) refers to rough, cracked skin at the tips and lateral aspects of the fingers forming irregular dirty-appearing lines that resemble those seen in a laborer (this is also associated with the anti-synthetase syndrome).See: sclerodactyly. Psoriaform changes in the scalp can occur. Centripetal flagellate erythema comprises linear, violaceous streaks on the trunk (possibly caused by itching pruritic skin). Calcinosis cutis (deposition of calcium in the skin) is usually seen in juvenile DM, not adult DM. Dysphagia (difficulty swallowing) is another feature, occurring in as much as 33% of cases.
Physical Examination

Diagnostic Findings
Patient #1
Patient #2
Treatment
There is no cure for dermatomyositis, but the symptoms can be treated. Options include medication, physical therapy, exercise, heat therapy (including microwave and ultrasound), orthotics and assistive devices, and rest. The standard treatment for dermatomyositis is a corticosteroid drug, given either in pill form or intravenously.
Immunosuppressant drugs, such as azathioprine and methotrexate, may reduce inflammation in people who do not respond well to prednisone.
Periodic treatment using intravenous immunoglobulin can also improve recovery. Other immunosuppressive agents used to treat the inflammation associated with dermatomyositis include cyclosporine A, cyclophosphamide, and tacrolimus.
Physical therapy is usually recommended to prevent muscle atrophy and to regain muscle strength and range of motion. Many individuals with dermatomyositis may need a topical ointment, such as topical corticosteroids, for their skin disorder. They should wear a high-protection sunscreen and protective clothing. Surgery may be required to remove calcium deposits that cause nerve pain and recurrent infections.
- Prednisolone
- Methotrexate
- Mycophenolate (CellCept / Myfortic)
- Intravenous immunoglobulin
- Azathioprine
- Cyclophosphamide
- Rituximab[9]
Prognosis
Most cases of dermatomyositis respond to therapy. The disease is usually more severe and resistant to therapy in individuals with cardiac or pulmonary problems.
References
- ↑ Ghirardello, A (2006). "Clinical implications of autoantibody screening in patients with autoimmune myositis". Autoimmunity. 39 (3): 217–221. doi:10.1080/08916930600622645. PMID 16769655. Unknown parameter
|coauthors=ignored (help); Unknown parameter|month=ignored (help) - ↑ Benveniste, O (2004). "Pathogenesis of primary inflammatory myopathies". Presse Médicale. 33 (20): 1444–1450. doi:10.1016/S0755-4982(04)98952-X. PMID 15611679. Unknown parameter
|coauthors=ignored (help); Unknown parameter|month=ignored (help) - ↑ "Polymyositis and Dermatomyositis: Autoimmune Disorders of Connective Tissue: Merck Manual Home Edition".
- ↑ Scheinfeld NS (2006). "Ulcerative paraneoplastic dermatomyositis secondary to metastatic breast cancer". Skinmed. 5 (2): 94–6. doi:10.1111/j.1540-9740.2006.03637.x. PMID 16603844.
- ↑ Benveniste O, Squier W, Boyer O, Hilton-Jones D, Herson S. Presse Med. 2004 Nov 20;33(20):1444-50. PMID: 15611679
- ↑ Nirmalananthan N, Holton JL, Hanna MG. Is it really myositis? A consideration of the differential diagnosis. Curr Opin Rheumatol. 2004 Nov;16(6):684-91.
- ↑ Page 151 in: Mitchell, Richard Sheppard; Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson (2007). Robbins Basic Pathology. Philadelphia: Saunders. ISBN 1-4160-2973-7. 8th edition.
- ↑ http://picasaweb.google.com/mcmumbi/USMLEIIImages/photo#5089143195781344626
- ↑ Scheinfeld N (2006). "A review of rituximab in cutaneous medicine". Dermatol. Online J. 12 (1): 3. PMID 16638371.
External links
- Dermatomyositis at Medline-Plus
- Goldminer: Dermatomyositis
- The American College of Rheumatology's patient education page on myopathy
- Illustration of Gottron's papules
- Polymyositis and Dermatomyositis Discussion group
- The Myositis Association
Template:Muscular Dystrophy
Template:Diseases of the musculoskeletal system and connective tissue