Breast cancer screening
Please Take Over This Page and Apply to be Editor-In-Chief for this topic: There can be one or more than one Editor-In-Chief. You may also apply to be an Associate Editor-In-Chief of one of the subtopics below. Please mail us [1] to indicate your interest in serving either as an Editor-In-Chief of the entire topic or as an Associate Editor-In-Chief for a subtopic. Please be sure to attach your CV and or biographical sketch.
X-ray mammography
Mammography is still the modality of choice for screening of early breast cancer, since it is relatively fast, reasonably accurate, and widely available in developed countries. Breast cancers detected by mammography are usually much smaller (earlier stage) than those detected by patients or doctors as a breast lump.
Due to the high incidence of breast cancer among older women, screening is now recommended in many countries. Recommended screening methods include breast self-examination and mammography. Mammography has been estimated to reduce breast cancer-related mortality by 20-30%.[1] Routine (annual) mammography of women older than age 40 or 50 is recommended by numerous organizations as a screening method to diagnose early breast cancer and has demonstrated a protective effect in multiple clinical trials.[2] The evidence in favor of mammographic screening comes from eight randomized clinical trials from the 1960s through 1980s. Many of these trials have been criticised for methodological errors, and the results were summarized in a review article published in 1993.[3]
Improvements in mortality due to screening are hard to measure; similar difficulty exists in measuring the impact of Pap smear testing on cervical cancer, though worldwide, the impact of that test is likely enormous. Nationwide mortality due to cancer before and after the institution of a screening test is a surrogate indicator about the effectiveness of screening, and results of mammography are favorable.
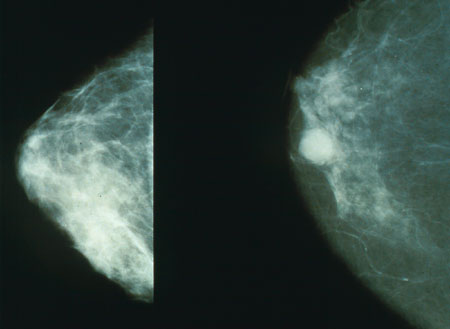
The U.S. National Cancer Institute recommends screening mammography every one to two years beginning at age 40.[4] In the UK, women are invited for screening once every three years beginning at age 50. Women with one or more first-degree relatives (mother, sister, daughter) with premenopausal breast cancer should begin screening at an earlier age. It is usually suggested to start screening at an age that is 10 years less than the age at which the relative was diagnosed with breast cancer.
A clinical practice guideline by the US Preventive Services Task Force recommended "screening mammography, with or without clinical breast examination (CBE), every 1 to 2 years for women aged 40 and older."[5] The Task Force gave a grade B recommendation.[6]
Criticisms of screening mammography
Several scientific groups however have expressed concern about the public's perceptions of the benefits of breast screening.[7] In 2001, a controversial review published in The Lancet claimed that there is no reliable evidence that screening for breast cancer reduces mortality.[8] The results of this study were widely reported in the popular press.[9]
False positives are a major problem of mammographic breast cancer screening. Data reported in the UK Million Woman Study indicates that if 134 mammograms are performed, 20 women will be called back for suspicious findings, and four biopsies will be necessary, to diagnose one cancer. Recall rates are higher in the U.S. than in the UK.[10] The contribution of mammography to the early diagnosis of cancer is controversial, and for those found with benign lesions, mammography can create a high psychological and financial cost.
Mammography in women less than 50 years old
Part of the difficulty in interpreting mammograms in younger women stems from the problem of breast density. Radiographically, a dense breast has a preponderance of glandular tissue, and younger age or estrogen hormone replacement therapy contribute to mammographic breast density. After menopause, the breast glandular tissue gradually is replaced by fatty tissue, making mammographic interpretation much more accurate. Some authors speculate that part of the contribution of estrogen hormone replacement therapy to breast cancer mortality arises from the issue of increased mammographic breast density. Breast density is an independent adverse prognostic factor on breast cancer prognosis.
A systematic review by the American College of Physicians concluded "Although few women 50 years of age or older have risks from mammography that outweigh the benefits, the evidence suggests that more women 40 to 49 years of age have such risks".[11]
Enhancements to mammography
In general, digital mammography and computer-aided mammography have increased the sensitivity of mammograms, but at the cost of more numerous false positive results.
Computer-aided diagnosis(CAD) Systems may help radiologists to evaluate X-ray images to detect breast cancer in an early stage.[citation needed] CAD is especially established in US and the Netherlands. It is used in addition to the human evaluation of the diagnostician.
Breast MRI
Magnetic resonance imaging (MRI) has been shown to detect cancers not visible on mammograms, but has long been regarded to have disadvantages. For example, although it is 27-36% more sensitive, it is less specific than mammography.[12] As a result, MRI studies will have more false positives (up to 5%), which may have undesirable financial and psychological costs. It is also a relatively expensive procedure, and one which requires the intravenous injection of a chemical agent to be effective. Proposed indications for using MRI for screening include:[13]
- Strong family history of breast cancer
- Patients with BRCA-1 or BRCA-2 oncogene mutations
- Evaluation of women with breast implants
- History of previous lumpectomy or breast biopsy surgeries
- Axillary metastasis with an unknown primary tumor
- Very dense or scarred breast tissue
However, two studies published in 2007 demonstrated the strengths of MRI-based screening:
- In March 2007, an article published in the New England Journal of Medicine demonstrated that in 3.1% of patients with breast cancer, whose contralateral breast was clinically and mammographically tumor-free, MRI could detect breast cancer. Sensitivity for detection of breast cancer in this study was 91%, specificity 88%.[14]
- In August 2007, an article published in The Lancet compared MRI breast cancer screening to conventional mammographic screening in 7,319 women. MRI screening was highly more sensitive (97% in the MRI group vs. 56% in the mammography group) in recognizing early high-grade Ductal Carcinoma in situ (DCIS), the most important precursor of invasive carcinoma. Despite the high sensitivity, MRI screening had a positive predictive value of 52%, which is totally accepted for cancer screening tests.[15] The author of a comment published in the same issue of The Lancet concludes that "MRI outperforms mammography in tumour detection and diagnosis."[16]
Breast ultrasound
Ultrasound alone is not usually employed as a screening tool but it is a useful additional tool for the characterization of palpable tumours and directing image-guided biopsies. U-Systems is a US-based company that is selling a breast-cancer detection system using ultrasound that is fully-automated. Using an ultrasound allows a look at dense breast tissue which is not possible with digital mammmography. It is closely correlated with the digital mammography. The other significant advantage over digital mammography is that it is a pain-free procedure.
Breast self-exam
Breast self-examination was widely discussed in the 1990s as a useful modality for detecting breast cancer at an earlier stage of presentation. A large clinical trial in China reduced enthusiasm for breast self-exam. In the trial, reported in the Journal of the National Cancer Institute first in 1997 and updated in 2002, 132,979 female Chinese factory workers were taught by nurses at their factories to perform monthly breast self-exam, while 133,085 other workers were not taught self-exam. The women taught self-exam tended to detect more breast nodules, but their breast cancer mortality rate was no different from that of women in the control group. In other words, women taught breast self-exam were mostly likely to detect benign breast disease, but were just as likely to die of breast cancer.[17] An editorial in the Journal of the National Cancer Institute reported in 2002, "Routinely Teaching Breast Self-Examination is Dead. What Does This Mean?"[18]
BRCA testing
A clinical practice guideline by the US Preventive Services Task Force :[5]
- "recommends against routine referral for genetic counseling or routine breast cancer susceptibility gene (BRCA) testing for women whose family history is not associated with an increased risk for deleterious mutations in breast cancer susceptibility gene 1 (BRCA1) or breast cancer susceptibility gene 2 (BRCA2)" The Task Force gave a grade D recommendation.[6]
- "recommends that women whose family history is associated with an increased risk for deleterious mutations in BRCA1 or BRCA2 genes be referred for genetic counseling and evaluation for BRCA testing." The Task Force gave a grade B recommendation.[6]
The Task Force noted that about 2% of women have family histories that indicate increased risk as defined by:
- For non–Ashkenazi Jewish women, any of the following:
- "2 first-degree relatives with breast cancer, 1 of whom received the diagnosis at age 50 years or younger"
- "3 or more first- or second-degree relatives with breast cancer regardless of age at diagnosis"
- "both breast and ovarian cancer among first- and second- degree relatives"
- "a first-degree relative with bilateral breast cancer"
- "a combination of 2 or more first- or second-degree relatives with ovarian cancer regardless of age at diagnosis"
- "a first- or second-degree relative with both breast and ovarian cancer at any age"
- "a history of breast cancer in a male relative."
- "For women of Ashkenazi Jewish heritage, an increased-risk family history includes any first-degree relative (or 2 second-degree relatives on the same side of the family) with breast or ovarian cancer."
References
- ↑ Elwood J, Cox B, Richardson A. "The effectiveness of breast cancer screening by mammography in younger women". Online J Curr Clin Trials. Doc No 32: [23, 227 words, 195 paragraphs]. PMID 8305999.
- ↑ Fletcher S, Black W, Harris R, Rimer B, Shapiro S (1993). "Report of the International Workshop on Screening for Breast Cancer". J Natl Cancer Inst. 85 (20): 1644–56. PMID 8105098.
- ↑ Fletcher SW, Black W, Harris R, Rimer BK, Shapiro S (1993). "Report of the International Workshop on Screening for Breast Cancer". J. Natl. Cancer Inst. 85 (20): 1644–56. PMID 8105098.
|access-date=requires|url=(help) - ↑ "NCI Statement on Mammography Screening - National Cancer Institute". Retrieved 2007-09-11.
- ↑ 5.0 5.1 "Screening for breast cancer: recommendations and rationale". Ann. Intern. Med. 137 (5 Part 1): 344–6. 2002. PMID 12204019.
- ↑ 6.0 6.1 6.2
- ↑ "Women 'misjudge screening benefits'". BBC. Monday, 15 October, 2001. Retrieved 2007-04-04. Check date values in:
|date=(help) - ↑ Olsen O, Gøtzsche P (2001). "Cochrane review on screening for breast cancer with mammography". Lancet. 358 (9290): 1340–2. PMID 11684218.
- ↑ "New concerns over breast screening". BBC. Thursday, 18 October, 2001. Retrieved 2007-04-04. Check date values in:
|date=(help) - ↑ Smith-Bindman R, Ballard-Barbash R, Miglioretti DL, Patnick J, Kerlikowske K (2005). "Comparing the performance of mammography screening in the USA and the UK". Journal of medical screening. 12 (1): 50–4. doi:10.1258/0969141053279130. PMID 15814020.
- ↑ Armstrong K, Moye E, Williams S, Berlin JA, Reynolds EE (2007). "Screening mammography in women 40 to 49 years of age: a systematic review for the American College of Physicians". Ann. Intern. Med. 146 (7): 516–26. PMID 17404354.
- ↑ Hrung J, Sonnad S, Schwartz J, Langlotz C (1999). "Accuracy of MR imaging in the work-up of suspicious breast lesions: a diagnostic meta-analysis". Acad Radiol. 6 (7): 387–97. PMID 10410164.
- ↑ Morrow M (2004). "Magnetic resonance imaging in breast cancer: one step forward, two steps back?". JAMA. 292 (22): 2779–80. PMID 15585740.
- ↑ Lehman CD, Gatsonis C, Kuhl CK, Hendrick RE, Pisano ED, Hanna L, Peacock S, Smazal SF, Maki DD, Julian TB, DePeri ER, Bluemke DA, Schnall MD (2007). "MRI evaluation of the contralateral breast in women with recently diagnosed breast cancer". N Engl J Med. 356 (13): 1295–1303. PMID 17392300.
- ↑ Kuhl CK, Schrading S, Bieling HB, Wardelmann E, Leutner CC, Koenig R, Kuhn W, Schild HH (2007). "MRI for diagnosis of pure ductal carcinoma in situ: a prospective observational study". The Lancet. 370 (9586): 485–492. PMID.
- ↑ Boetes C, Mann RM (2007). "Ductal carcinoma in situ and breast MRI". The Lancet. 370 (9586): 459–460. PMID.
- ↑ Thomas DB, Gao DL, Ray RM; et al. (2002). "Randomized trial of breast self-examination in Shanghai: final results". J. Natl. Cancer Inst. 94 (19): 1445–57. PMID 12359854.
- ↑ Harris R, Kinsinger LS (2002). "Routinely teaching breast self-examination is dead. What does this mean?". J. Natl. Cancer Inst. 94 (19): 1420–1. PMID 12359843.
External links
|
Breast Cancer Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Breast cancer screening On the Web |
|
American Roentgen Ray Society Images of Breast cancer screening |
|
Risk calculators and risk factors for Breast cancer screening |
- Pages with reference errors
- CS1 maint: Multiple names: authors list
- Pages using citations with accessdate and no URL
- CS1 errors: dates
- CS1 maint: Explicit use of et al.
- All articles with unsourced statements
- Articles with unsourced statements from September 2007
- Articles with invalid date parameter in template
- Oncology
- Types of cancer
- Breast
- Hereditary cancers