Thrombophilia medical therapy: Difference between revisions
Jump to navigation
Jump to search
No edit summary |
(update) |
||
| Line 4: | Line 4: | ||
{{CMG}} {{AE}} {{asiri}} | {{CMG}} {{AE}} {{asiri}} | ||
==Overview== | ==Overview== | ||
*The [[Thrombophilia_medical_therapy|treatment]] for thrombophilia depends on the underlying hypercoagulable state and the clinical presentation. | *The [[Thrombophilia_medical_therapy|treatment]] for thrombophilia depends on the underlying hypercoagulable state and the clinical presentation<ref name=?>DeLoughery TG. Hemostasis and Thrombosis: Springer International Publishing; 2014.</ref><ref name="pmid24421360">{{cite journal| author=Cohoon KP, Heit JA| title=Inherited and secondary thrombophilia. | journal=Circulation | year= 2014 | volume= 129 | issue= 2 | pages= 254-7 | pmid=24421360 | doi=10.1161/CIRCULATIONAHA.113.001943 | pmc=3979345 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=24421360 }} </ref><ref name="pmid11309638">{{cite journal| author=Seligsohn U, Lubetsky A| title=Genetic susceptibility to venous thrombosis. | journal=N Engl J Med | year= 2001 | volume= 344 | issue= 16 | pages= 1222-31 | pmid=11309638 | doi=10.1056/NEJM200104193441607 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=11309638 }} </ref> | ||
*Treatment should be tailored to the individual patient | *Treatment should be tailored to the individual patient | ||
** The risks and benefits, required monitoring, and costs associated with each form of anticoagulation should be discussed with the patient prior to initiation of therapy | ** The risks and benefits, required monitoring, and costs associated with each form of anticoagulation should be discussed with the patient prior to initiation of therapy | ||
*The mainstay of therapy for thrombophilia is [[anticoagulation]] with either [[warfarin]], [[Low_molecular_weight_heparin|low molecular weight heparin]], [[Direct_Xa_inhibitor|direct Xa inhibitors]], or [[Direct_thrombin_inhibitor|direct thrombin inhibitors]]. | *The mainstay of therapy for thrombophilia is [[anticoagulation]] with either [[warfarin]], [[Low_molecular_weight_heparin|low molecular weight heparin]], [[Direct_Xa_inhibitor|direct Xa inhibitors]], or [[Direct_thrombin_inhibitor|direct thrombin inhibitors]]<ref name="pmid26780738">{{cite journal| author=Streiff MB, Agnelli G, Connors JM, Crowther M, Eichinger S, Lopes R et al.| title=Guidance for the treatment of deep vein thrombosis and pulmonary embolism. | journal=J Thromb Thrombolysis | year= 2016 | volume= 41 | issue= 1 | pages= 32-67 | pmid=26780738 | doi=10.1007/s11239-015-1317-0 | pmc=4715858 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=26780738 }} </ref><ref name="pmid18805965">{{cite journal| author=Martinelli I, Franchini M, Mannucci PM| title=How I treat rare venous thromboses. | journal=Blood | year= 2008 | volume= 112 | issue= 13 | pages= 4818-23 | pmid=18805965 | doi=10.1182/blood-2008-07-165969 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=18805965 }} </ref><ref name="pmid23789890">{{cite journal| author=De Stefano V, Grandone E, Martinelli I| title=Recommendations for prophylaxis of pregnancy-related venous thromboembolism in carriers of inherited thrombophilia. Comment on the 2012 ACCP guidelines. | journal=J Thromb Haemost | year= 2013 | volume= 11 | issue= 9 | pages= 1779-81 | pmid=23789890 | doi=10.1111/jth.12330 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=23789890 }} </ref> | ||
*Response to anticoagulation can be monitored clinically, or with repeat ultrasongraphy for [[Deep_vein_thrombosis|deep vein thrombosis]] or measuring [[D-dimer]] levels after treatment | *Response to anticoagulation can be monitored clinically, or with repeat ultrasongraphy for [[Deep_vein_thrombosis|deep vein thrombosis]] or measuring [[D-dimer]] levels after treatment | ||
==Medical Therapy== | ==Medical Therapy== | ||
The | *Direct oral anticoagulants, including [[Direct_Xa_inhibitor|direct Xa inhibitors]] and [[Direct_thrombin_inhibitor|direct thrombin inhibitors]], should be used for long term treatment of most patients<ref name="pmid26780738">{{cite journal| author=Streiff MB, Agnelli G, Connors JM, Crowther M, Eichinger S, Lopes R et al.| title=Guidance for the treatment of deep vein thrombosis and pulmonary embolism. | journal=J Thromb Thrombolysis | year= 2016 | volume= 41 | issue= 1 | pages= 32-67 | pmid=26780738 | doi=10.1007/s11239-015-1317-0 | pmc=4715858 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=26780738 }} </ref> | ||
:*Important exceptions include: | |||
:**Pregnancy<ref name="pmid22315276">{{cite journal| author=Bates SM, Greer IA, Middeldorp S, Veenstra DL, Prabulos AM, Vandvik PO et al.| title=VTE, thrombophilia, antithrombotic therapy, and pregnancy: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. | journal=Chest | year= 2012 | volume= 141 | issue= 2 Suppl | pages= e691S-736S | pmid=22315276 | doi=10.1378/chest.11-2300 | pmc=3278054 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=22315276 }} </ref> | |||
:**Renal insufficiency | |||
:**Malignancy<ref name="pmid12853587">{{cite journal| author=Lee AY, Levine MN, Baker RI, Bowden C, Kakkar AK, Prins M et al.| title=Low-molecular-weight heparin versus a coumarin for the prevention of recurrent venous thromboembolism in patients with cancer. | journal=N Engl J Med | year= 2003 | volume= 349 | issue= 2 | pages= 146-53 | pmid=12853587 | doi=10.1056/NEJMoa025313 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=12853587 }} [http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=14711281 Review in: ACP J Club. 2004 Jan-Feb;140(1):10] [http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=14599373 Review in: J Fam Pract. 2003 Nov;52(11):843-4] </ref> | |||
*[[Low_molecular_weight_heparin|Low molecular weight heparin]] is recommended for anticoagulation for the following acquired thrombophilias: | |||
**'''Post-surgery prophylaxis'''<ref name="pmid22315265">{{cite journal| author=Falck-Ytter Y, Francis CW, Johanson NA, Curley C, Dahl OE, Schulman S et al.| title=Prevention of VTE in orthopedic surgery patients: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. | journal=Chest | year= 2012 | volume= 141 | issue= 2 Suppl | pages= e278S-325S | pmid=22315265 | doi=10.1378/chest.11-2404 | pmc=3278063 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=22315265 }} </ref><ref name="pmid11919306">{{cite journal| author=Bergqvist D, Agnelli G, Cohen AT, Eldor A, Nilsson PE, Le Moigne-Amrani A et al.| title=Duration of prophylaxis against venous thromboembolism with enoxaparin after surgery for cancer. | journal=N Engl J Med | year= 2002 | volume= 346 | issue= 13 | pages= 975-80 | pmid=11919306 | doi=10.1056/NEJMoa012385 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=11919306 }} </ref><ref name="pmid15598646">{{cite journal| author=Agnelli G| title=Prevention of venous thromboembolism in surgical patients. | journal=Circulation | year= 2004 | volume= 110 | issue= 24 Suppl 1 | pages= IV4-12 | pmid=15598646 | doi=10.1161/01.CIR.0000150639.98514.6c | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=15598646 }} </ref> | |||
***The duration of anticoagulation after surgery is variable. Most clinical trials have evaluated anticoagulation for 10-35 days | |||
***General recommendations for thrombophrophylaxis is 7-10 days for standard risk patients and 10-35 days for higher risk patients as described in the algorithims below and for patients undergoing abdominal and pelvic surgeries for gynecologic malginancies<ref name="pmid20409525">{{cite journal| author=Muntz J| title=Duration of deep vein thrombosis prophylaxis in the surgical patient and its relation to quality issues. | journal=Am J Surg | year= 2010 | volume= 200 | issue= 3 | pages= 413-21 | pmid=20409525 | doi=10.1016/j.amjsurg.2009.05.045 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=20409525 }} </ref> | |||
**'''Pregnancy and postpartum'''<ref name="pmid22315276">{{cite journal| author=Bates SM, Greer IA, Middeldorp S, Veenstra DL, Prabulos AM, Vandvik PO et al.| title=VTE, thrombophilia, antithrombotic therapy, and pregnancy: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. | journal=Chest | year= 2012 | volume= 141 | issue= 2 Suppl | pages= e691S-736S | pmid=22315276 | doi=10.1378/chest.11-2300 | pmc=3278054 | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=22315276 }} </ref> | |||
***Patients who develop acute thrombosis during pregnancy should be anticoagulated for the remainder of the their pregnancy and 6 weeks postpartum for a minimum of 3 months | |||
***A similar duration of anticoagulation is recommended for patients with high risk thrombophilias as described in the algorithims below | |||
**'''Malignancy'''<ref name="pmid12853587">{{cite journal| author=Lee AY, Levine MN, Baker RI, Bowden C, Kakkar AK, Prins M et al.| title=Low-molecular-weight heparin versus a coumarin for the prevention of recurrent venous thromboembolism in patients with cancer. | journal=N Engl J Med | year= 2003 | volume= 349 | issue= 2 | pages= 146-53 | pmid=12853587 | doi=10.1056/NEJMoa025313 | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=12853587 }} [http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=14711281 Review in: ACP J Club. 2004 Jan-Feb;140(1):10] [http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?dbfrom=pubmed&tool=sumsearch.org/cite&retmode=ref&cmd=prlinks&id=14599373 Review in: J Fam Pract. 2003 Nov;52(11):843-4] </ref> | |||
**Alternative agents include [[Warfarin]] and [[Fondaparinux]] | |||
'''Treatment algorithms are presented below:''' | |||
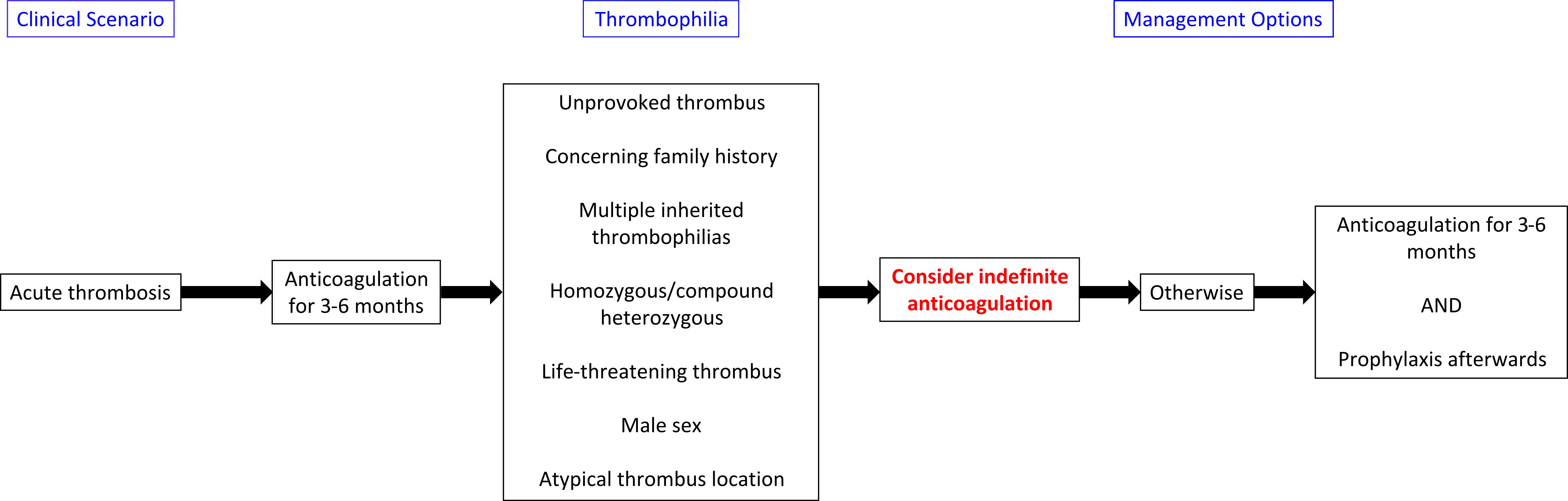
[[Image: Thrombophilia_Management_Thrombosis.jpg|thumb|center|700px|Management of acute thrombosis in patients with inherited thrombophilias]] | [[Image: Thrombophilia_Management_Thrombosis.jpg|thumb|center|700px|Management of acute thrombosis in patients with inherited thrombophilias]] | ||
| Line 18: | Line 33: | ||
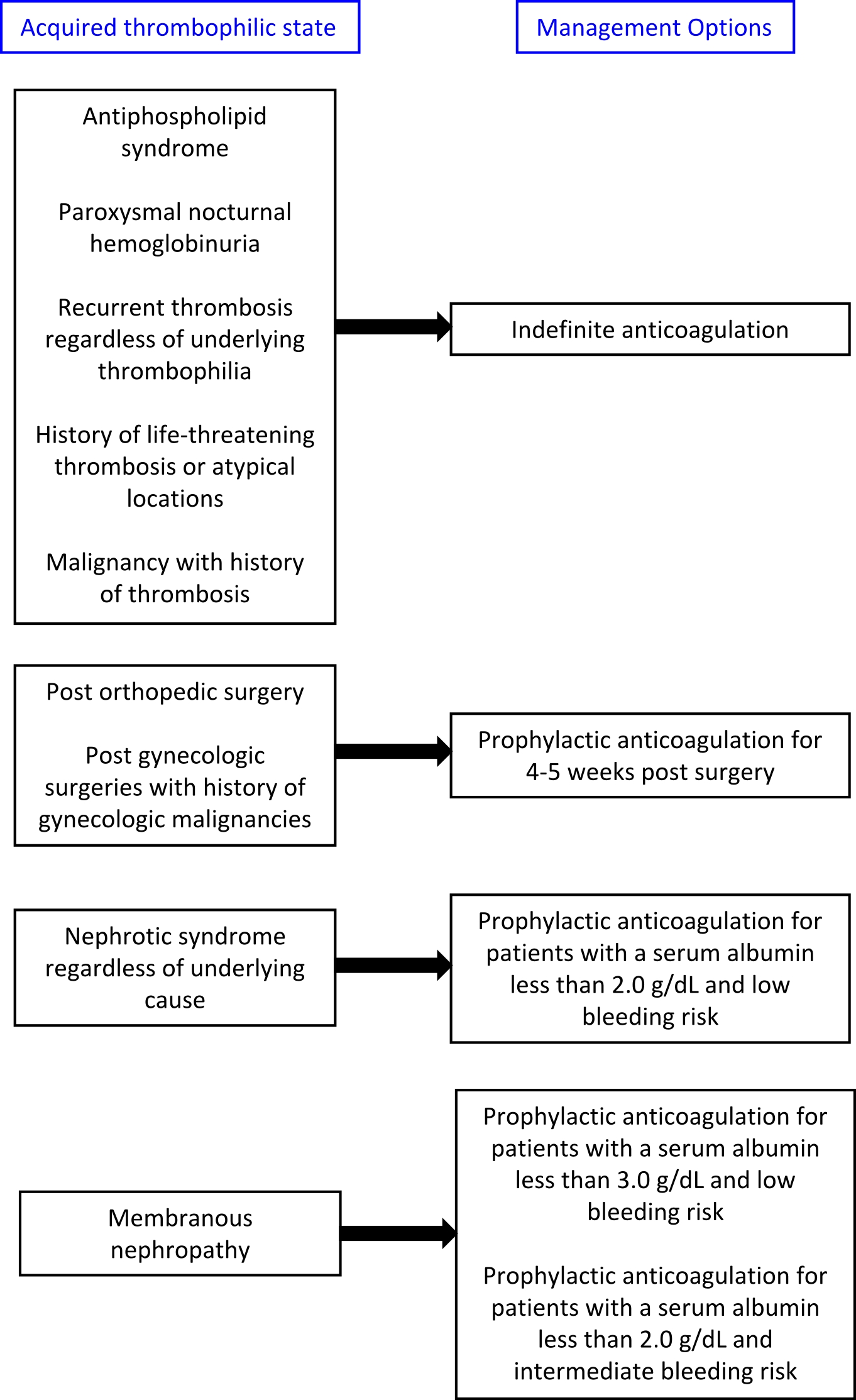
[[Image: Thrombophilia_Acquired_Management.jpg|thumb|center|500px|Management of patients with acquired thrombophilias]] | [[Image: Thrombophilia_Acquired_Management.jpg|thumb|center|500px|Management of patients with acquired thrombophilias]] | ||
==References== | ==References== | ||
{{reflist|2}} | {{reflist|2}} | ||
Revision as of 03:14, 18 July 2016
|
Thrombophilia Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Thrombophilia medical therapy On the Web |
|
American Roentgen Ray Society Images of Thrombophilia medical therapy |
|
Risk calculators and risk factors for Thrombophilia medical therapy |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1] Associate Editor(s)-in-Chief: Asiri Ediriwickrema, M.D., M.H.S. [2]
Overview
- The treatment for thrombophilia depends on the underlying hypercoagulable state and the clinical presentation[1][2][3]
- Treatment should be tailored to the individual patient
- The risks and benefits, required monitoring, and costs associated with each form of anticoagulation should be discussed with the patient prior to initiation of therapy
- The mainstay of therapy for thrombophilia is anticoagulation with either warfarin, low molecular weight heparin, direct Xa inhibitors, or direct thrombin inhibitors[4][5][6]
- Response to anticoagulation can be monitored clinically, or with repeat ultrasongraphy for deep vein thrombosis or measuring D-dimer levels after treatment
Medical Therapy
- Direct oral anticoagulants, including direct Xa inhibitors and direct thrombin inhibitors, should be used for long term treatment of most patients[4]
- Low molecular weight heparin is recommended for anticoagulation for the following acquired thrombophilias:
- Post-surgery prophylaxis[9][10][11]
- The duration of anticoagulation after surgery is variable. Most clinical trials have evaluated anticoagulation for 10-35 days
- General recommendations for thrombophrophylaxis is 7-10 days for standard risk patients and 10-35 days for higher risk patients as described in the algorithims below and for patients undergoing abdominal and pelvic surgeries for gynecologic malginancies[12]
- Pregnancy and postpartum[7]
- Patients who develop acute thrombosis during pregnancy should be anticoagulated for the remainder of the their pregnancy and 6 weeks postpartum for a minimum of 3 months
- A similar duration of anticoagulation is recommended for patients with high risk thrombophilias as described in the algorithims below
- Malignancy[8]
- Alternative agents include Warfarin and Fondaparinux
- Post-surgery prophylaxis[9][10][11]
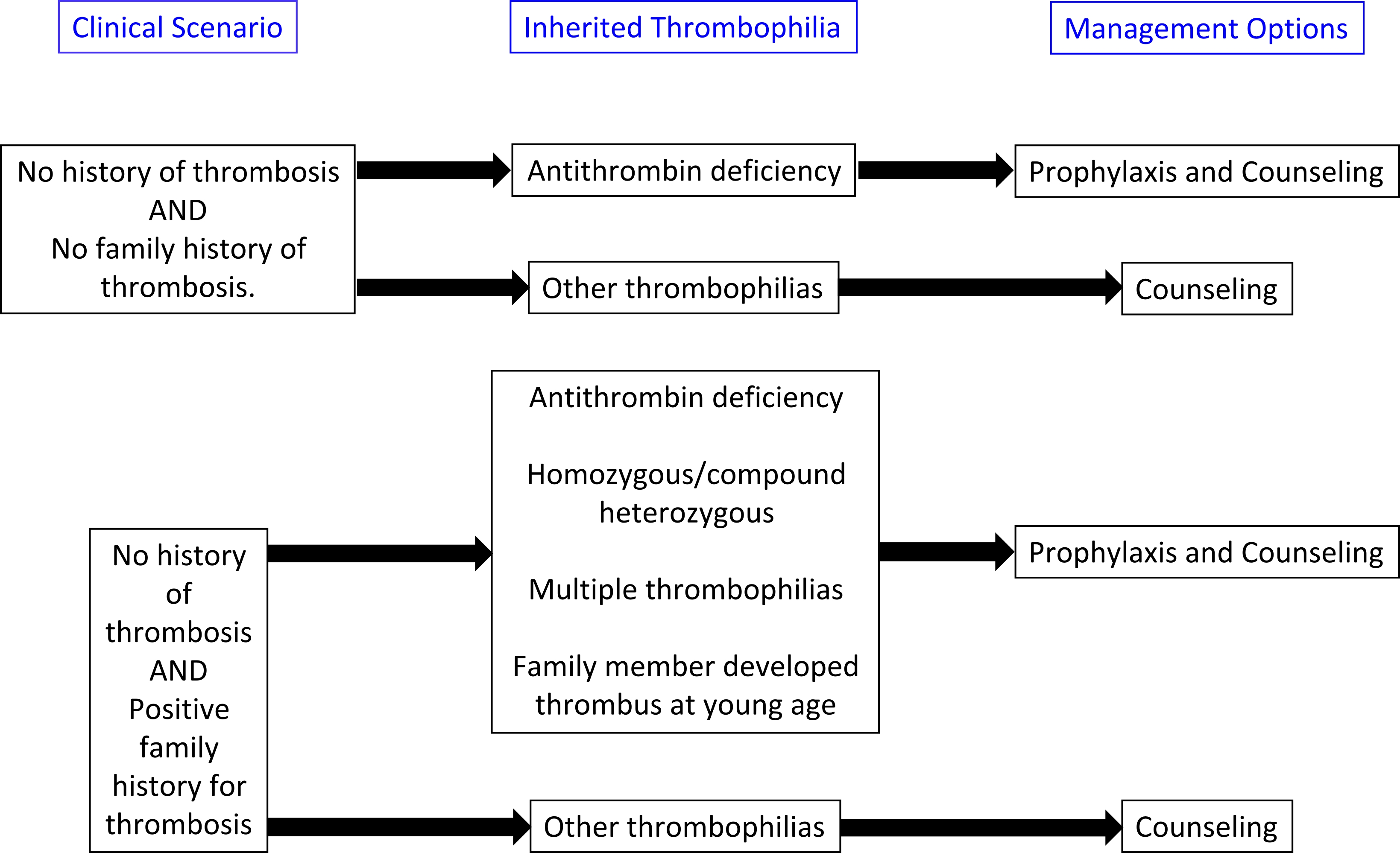
Treatment algorithms are presented below:
References
- ↑ DeLoughery TG. Hemostasis and Thrombosis: Springer International Publishing; 2014.
- ↑ Cohoon KP, Heit JA (2014). "Inherited and secondary thrombophilia". Circulation. 129 (2): 254–7. doi:10.1161/CIRCULATIONAHA.113.001943. PMC 3979345. PMID 24421360.
- ↑ Seligsohn U, Lubetsky A (2001). "Genetic susceptibility to venous thrombosis". N Engl J Med. 344 (16): 1222–31. doi:10.1056/NEJM200104193441607. PMID 11309638.
- ↑ 4.0 4.1 Streiff MB, Agnelli G, Connors JM, Crowther M, Eichinger S, Lopes R; et al. (2016). "Guidance for the treatment of deep vein thrombosis and pulmonary embolism". J Thromb Thrombolysis. 41 (1): 32–67. doi:10.1007/s11239-015-1317-0. PMC 4715858. PMID 26780738.
- ↑ Martinelli I, Franchini M, Mannucci PM (2008). "How I treat rare venous thromboses". Blood. 112 (13): 4818–23. doi:10.1182/blood-2008-07-165969. PMID 18805965.
- ↑ De Stefano V, Grandone E, Martinelli I (2013). "Recommendations for prophylaxis of pregnancy-related venous thromboembolism in carriers of inherited thrombophilia. Comment on the 2012 ACCP guidelines". J Thromb Haemost. 11 (9): 1779–81. doi:10.1111/jth.12330. PMID 23789890.
- ↑ 7.0 7.1 Bates SM, Greer IA, Middeldorp S, Veenstra DL, Prabulos AM, Vandvik PO; et al. (2012). "VTE, thrombophilia, antithrombotic therapy, and pregnancy: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest. 141 (2 Suppl): e691S–736S. doi:10.1378/chest.11-2300. PMC 3278054. PMID 22315276.
- ↑ 8.0 8.1 Lee AY, Levine MN, Baker RI, Bowden C, Kakkar AK, Prins M; et al. (2003). "Low-molecular-weight heparin versus a coumarin for the prevention of recurrent venous thromboembolism in patients with cancer". N Engl J Med. 349 (2): 146–53. doi:10.1056/NEJMoa025313. PMID 12853587. Review in: ACP J Club. 2004 Jan-Feb;140(1):10 Review in: J Fam Pract. 2003 Nov;52(11):843-4
- ↑ Falck-Ytter Y, Francis CW, Johanson NA, Curley C, Dahl OE, Schulman S; et al. (2012). "Prevention of VTE in orthopedic surgery patients: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest. 141 (2 Suppl): e278S–325S. doi:10.1378/chest.11-2404. PMC 3278063. PMID 22315265.
- ↑ Bergqvist D, Agnelli G, Cohen AT, Eldor A, Nilsson PE, Le Moigne-Amrani A; et al. (2002). "Duration of prophylaxis against venous thromboembolism with enoxaparin after surgery for cancer". N Engl J Med. 346 (13): 975–80. doi:10.1056/NEJMoa012385. PMID 11919306.
- ↑ Agnelli G (2004). "Prevention of venous thromboembolism in surgical patients". Circulation. 110 (24 Suppl 1): IV4–12. doi:10.1161/01.CIR.0000150639.98514.6c. PMID 15598646.
- ↑ Muntz J (2010). "Duration of deep vein thrombosis prophylaxis in the surgical patient and its relation to quality issues". Am J Surg. 200 (3): 413–21. doi:10.1016/j.amjsurg.2009.05.045. PMID 20409525.