Systemic lupus erythematosus physical examination: Difference between revisions
Tamar Sifri (talk | contribs) |
|||
| (49 intermediate revisions by 4 users not shown) | |||
| Line 2: | Line 2: | ||
{{Systemic lupus erythematosus}} | {{Systemic lupus erythematosus}} | ||
{{CMG}}; {{AE}} {{ | {{CMG}}; {{AE}} {{MIR}} | ||
==Overview== | ==Overview== | ||
In the earlier stages of the disease, patients appear well, while in the late stages of the disease, patients are clearly ill with multi-organ involvement. The patient may show a wide range of skin manifestations including [[urticaria]], [[Bullous|bullous lesions]], [[malar rash]], and scarring [[alopecia]]. The patient may develop nasal and [[oral ulcers]]. [[Arthritis]] may lead to a decreased [[range of motion]], joint effusion, and [[arthralgia]]. Neurological manifestations including [[psychosis]], [[cognitive impairment]], and [[hallucinations]], may also be present. | |||
==Physical Examination== | ==Physical Examination== | ||
===Appearance of the Patient=== | |||
* | *Patient appears well in the earlier stages of the disease | ||
* | *Patient appears ill in the late stages of the disease due to multi-organ involvement | ||
* | ===Vital Signs=== | ||
* | *[[Fever]] higher than 38 after the exclusion of [[infection]] | ||
* [[ | *[[Tachycardia]]/[[bradycardia]] depends on the accompanying complication | ||
*[[Tachypnea]]/[[bradypnea]] depends on the accompanying complication | |||
==== | === Skin<ref name="pmid25077888">{{cite journal |vauthors=Parodi A, Cozzani E |title=Cutaneous manifestations of lupus erythematosus |journal=G Ital Dermatol Venereol |volume=149 |issue=5 |pages=549–54 |year=2014 |pmid=25077888 |doi= |url=}}</ref><ref name="pmid26985173">{{cite journal |vauthors=Szczęch J, Rutka M, Samotij D, Zalewska A, Reich A |title=Clinical characteristics of cutaneous lupus erythematosus |journal=Postepy Dermatol Alergol |volume=33 |issue=1 |pages=13–7 |year=2016 |pmid=26985173 |pmc=4793050 |doi=10.5114/pdia.2014.44031 |url=}}</ref><ref name="pmid19824738">{{cite journal |vauthors=Walling HW, Sontheimer RD |title=Cutaneous lupus erythematosus: issues in diagnosis and treatment |journal=Am J Clin Dermatol |volume=10 |issue=6 |pages=365–81 |year=2009 |pmid=19824738 |doi=10.2165/11310780-000000000-00000 |url=}}</ref> === | ||
*[[Cyanosis]] | |||
**Secondary to [[respiratory]] complications | |||
*[[Jaundice]] | |||
**Secondary to [[hepatitis]] | |||
*[[Pallor]] | |||
**Secondary to [[anemia]] | |||
*Generalised [[erythema]] | |||
*[[Bruises]] | |||
**Secondary to [[thrombocytopenia]] | |||
*[[Urticaria]] | |||
*[[Bullous|Bullous lesions]] | |||
*[[Sclerodactyly]] | |||
*Skin [[Ulcerations|ulceration]] | |||
*[[Malar rash]]: the classic lupus ‘butterfly’ rash | |||
** [[Erythema|Erythematous]], elevated [[Lesions|lesion]], [[Pruritis|pruritic]] or painful, in a [[malar]] distribution, commonly precipitated by exposure to sunlight | |||
* Annular or psoriasiform skin [[lesions]] | |||
** Small, [[erythematous]], slightly scaly [[papules]] that evolve into either a psoriasiform (papulosquamous) or annular form and tend to involve shoulders, forearms, neck, and upper torso | |||
* [[Scarring]] [[chronic]] [[alopecia]] | |||
** Mostly present on face, neck, and scalp | |||
* [[Telangiectasias]] | |||
* Dyspigmentation ([[hyperpigmentation]] or [[hypopigmentation]]) of skin in [[scar]] places | |||
* Follicular plugging | |||
** Discrete, [[erythematous]], slightly infiltrated [[plaques]] covered by a well-formed adherent scale that extends into dilated [[hair follicles]] | |||
* [[Nodules]] | |||
** Can be firm (Lupus profundus) and painful | |||
* Photodistributed [[lesions]] with chronic pink indurated plaques or broad [[lesions]] that are slow to heal (more seen in lupus tumidus) | |||
* Thin hair that easily fractures (lupus hair) | |||
* Irregularly shaped raised white plaques, areas of erythema, silvery white scarred [[lesions]], and [[ulcers]] with surrounding [[erythema]] on the soft or hard palate or buccal [[mucosa]] | |||
* Periungual [[erythema]] | |||
** Dilated tortuous loops of [[capillaries]] and a prominent subcapillary venous plexus along | |||
** Involves the base of the nail and edges of the upper [[eyelid]] | |||
[[File:Systemic lupus erythematosus 055.jpg|300px]] | |||
'''For more pictures of the rash presentation in lupus, click [[Systemic lupus eryhthematosus physical examination:Gallery|here]].''' | |||
<gallery | ===HEENT=== | ||
*[[Ophthalmology]]<ref name="pmid26367085">{{cite journal |vauthors=Preble JM, Silpa-archa S, Foster CS |title=Ocular involvement in systemic lupus erythematosus |journal=Curr Opin Ophthalmol |volume=26 |issue=6 |pages=540–5 |year=2015 |pmid=26367085 |doi=10.1097/ICU.0000000000000209 |url=}}</ref><ref name="pmid25904124">{{cite journal |vauthors=Silpa-archa S, Lee JJ, Foster CS |title=Ocular manifestations in systemic lupus erythematosus |journal=Br J Ophthalmol |volume=100 |issue=1 |pages=135–41 |year=2016 |pmid=25904124 |doi=10.1136/bjophthalmol-2015-306629 |url=}}</ref> | |||
**[[Nystagmus]] | |||
**Visual [[Retinal|retinal changes]] from systemic lupus erythematosus cytoid bodies, [[Retina|retinal]] [[haemorrhages]], serous exudate or [[haemorrhage]] in the [[choroid]], [[optic neuritis]] (not due to [[hypertension]], drugs or [[infection]]) | |||
**[[Cataract]] | |||
**[[Optic nerve atrophy]] | |||
**[[Icterus|Icteric sclera]] | |||
**[[Cotton wool spots]] in the [[retina]] in [[Ophthalmoscopy|ophthalmoscopic exam]] | |||
*Nasal [[ulcers]]<ref name="pmid1526055">{{cite journal |vauthors=Robson AK, Burge SM, Millard PR |title=Nasal mucosal involvement in lupus erythematosus |journal=Clin Otolaryngol Allied Sci |volume=17 |issue=4 |pages=341–3 |year=1992 |pmid=1526055 |doi= |url=}}</ref> | |||
**Mostly painless | |||
**Mostly in lower [[nasal septum]] and [[bilateral]] and parallel | |||
**Nasal perforation secondary to [[vasculitis]] may happen rarely | |||
*Oral [[ulcers]]<ref name="pmid23780804">{{cite journal |vauthors=Anyanwu CO, Ang CC, Werth VP |title=Oral mucosal involvement in bullous lupus |journal=Arthritis Rheum. |volume=65 |issue=10 |pages=2622 |year=2013 |pmid=23780804 |pmc=4333153 |doi=10.1002/art.38051 |url=}}</ref><ref name="pmid23248469">{{cite journal |vauthors=Ranginwala AM, Chalishazar MM, Panja P, Buddhdev KP, Kale HM |title=Oral discoid lupus erythematosus: A study of twenty-one cases |journal=J Oral Maxillofac Pathol |volume=16 |issue=3 |pages=368–73 |year=2012 |pmid=23248469 |pmc=3519212 |doi=10.4103/0973-029X.102487 |url=}}</ref> | |||
**Mostly painless | |||
**White plaques with areas of [[erythema]], or punched-out erosions or ulcers with surrounding [[erythema]] on the soft or hard palate or [[buccal mucosa]] | |||
===Neck<ref name="pmid19107085">{{cite journal |vauthors=Melikoglu MA, Melikoglu M |title=The clinical importance of lymphadenopathy in systemic lupus erythematosus |journal=Acta Reumatol Port |volume=33 |issue=4 |pages=402–6 |year=2008 |pmid=19107085 |doi= |url=}}</ref><ref name="pmid24722263">{{cite journal |vauthors=Sacre K, Escoubet B, Pasquet B, Chauveheid MP, Zennaro MC, Tubach F, Papo T |title=Increased arterial stiffness in systemic lupus erythematosus (SLE) patients at low risk for cardiovascular disease: a cross-sectional controlled study |journal=PLoS ONE |volume=9 |issue=4 |pages=e94511 |year=2014 |pmid=24722263 |pmc=3983200 |doi=10.1371/journal.pone.0094511 |url=}}</ref>=== | |||
*[[Jugular venous distension]] | |||
**Secondary to [[hypertension]] and cardiac complications | |||
*[[Lymphadenopathy]] | |||
** [[Lymph node|Lymph nodes]] are soft, non-tender, discrete | |||
** Usually detected in the [[cervical]], [[axillary]], and [[inguinal]] | |||
===Lungs<ref name="pmid21194884">{{cite journal |vauthors=Torre O, Harari S |title=Pleural and pulmonary involvement in systemic lupus erythematosus |journal=Presse Med |volume=40 |issue=1 Pt 2 |pages=e19–29 |year=2011 |pmid=21194884 |doi=10.1016/j.lpm.2010.11.004 |url=}}</ref><ref name="pmid26550810">{{cite journal |vauthors=Salvati F |title=[The involvement of pulmonary interstitial tissue in multisystemic lupus erythematosus: interdisciplinarity and role of the pneumologists] |language=Italian |journal=Clin Ter |volume=166 |issue=5 |pages=205–7 |year=2015 |pmid=26550810 |doi= |url=}}</ref><ref name="pmid25639532">{{cite journal |vauthors=Alamoudi OS, Attar SM |title=Pulmonary manifestations in systemic lupus erythematosus: association with disease activity |journal=Respirology |volume=20 |issue=3 |pages=474–80 |year=2015 |pmid=25639532 |pmc=4418345 |doi=10.1111/resp.12473 |url=}}</ref>=== | |||
*Fine and coarse [[crackles]] upon auscultation of the [[lung]] | |||
**May be due to [[pneumonitis]] | |||
*In case of [[pleural effusion]]: | |||
**Asymmetric [[tactile fremitus]] | |||
**Asymmetric [[chest expansion]] | |||
===Heart<ref name="pmid24790989">{{cite journal |vauthors=Mak A, Kow NY |title=Imbalance between endothelial damage and repair: a gateway to cardiovascular disease in systemic lupus erythematosus |journal=Biomed Res Int |volume=2014 |issue= |pages=178721 |year=2014 |pmid=24790989 |pmc=3984775 |doi=10.1155/2014/178721 |url=}}</ref><ref name="pmid24722263">{{cite journal |vauthors=Sacre K, Escoubet B, Pasquet B, Chauveheid MP, Zennaro MC, Tubach F, Papo T |title=Increased arterial stiffness in systemic lupus erythematosus (SLE) patients at low risk for cardiovascular disease: a cross-sectional controlled study |journal=PLoS ONE |volume=9 |issue=4 |pages=e94511 |year=2014 |pmid=24722263 |pmc=3983200 |doi=10.1371/journal.pone.0094511 |url=}}</ref><ref name="pmid23052654">{{cite journal |vauthors=Canpolat N, Kasapcopur O, Caliskan S, Gokalp S, Bor M, Tasdemir M, Sever L, Arisoy N |title=Ambulatory blood pressure and subclinical cardiovascular disease in patients with juvenile-onset systemic lupus erythematosus |journal=Pediatr. Nephrol. |volume=28 |issue=2 |pages=305–13 |year=2013 |pmid=23052654 |doi=10.1007/s00467-012-2317-3 |url=}}</ref>=== | |||
*Chest [[tenderness]] or discomfort upon palpation | |||
**May be due to [[costochondritis]] | |||
*[[Diastolic murmurs|Diastolic murmur]], or [[Systolic murmurs|systolic murmur]] >3/6 due to [[valvular disease]] | |||
*Loud second heart sound (due to [[pulmonary hypertension]]) | |||
*Loud S1-S2 due to [[cardiomegaly]] | |||
*Decrease heart sounds if associated with [[pericardial effusion]] | |||
===Abdomen<ref name="pmid20572299">{{cite journal |vauthors=Tian XP, Zhang X |title=Gastrointestinal involvement in systemic lupus erythematosus: insight into pathogenesis, diagnosis and treatment |journal=World J. Gastroenterol. |volume=16 |issue=24 |pages=2971–7 |year=2010 |pmid=20572299 |pmc=2890936 |doi= |url=}}</ref><ref name="pmid27329649">{{cite journal |vauthors=Alves SC, Fasano S, Isenberg DA |title=Autoimmune gastrointestinal complications in patients with systemic lupus erythematosus: case series and literature review |journal=Lupus |volume=25 |issue=14 |pages=1509–1519 |year=2016 |pmid=27329649 |doi=10.1177/0961203316655210 |url=}}</ref><ref name="pmid27055518">{{cite journal |vauthors=Fawzy M, Edrees A, Okasha H, El Ashmaui A, Ragab G |title=Gastrointestinal manifestations in systemic lupus erythematosus |journal=Lupus |volume=25 |issue=13 |pages=1456–1462 |year=2016 |pmid=27055518 |doi=10.1177/0961203316642308 |url=}}</ref><ref name="pmid28523968">{{cite journal |vauthors=Li Z, Xu D, Wang Z, Wang Y, Zhang S, Li M, Zeng X |title=Gastrointestinal system involvement in systemic lupus erythematosus |journal=Lupus |volume= |issue= |pages=961203317707825 |year=2017 |pmid=28523968 |doi=10.1177/0961203317707825 |url=}}</ref>=== | |||
*[[Abdominal distention]] | |||
*[[Ascites]] | |||
**Due to [[nephrotic syndrome]] | |||
*[[Abdominal pain]] | |||
**Due to [[Vasculitis|mesentric vasculitis]] | |||
*[[Hepatomegaly]] | |||
*[[Splenomegaly]] | |||
*Costo-vertebral angle tenderness | |||
===Extremities<ref name="pmid15580980">{{cite journal |vauthors=Zoma A |title=Musculoskeletal involvement in systemic lupus erythematosus |journal=Lupus |volume=13 |issue=11 |pages=851–3 |year=2004 |pmid=15580980 |doi=10.1191/0961203303lu2021oa |url=}}</ref><ref name="pmid22956550">{{cite journal |vauthors=Gabba A, Piga M, Vacca A, Porru G, Garau P, Cauli A, Mathieu A |title=Joint and tendon involvement in systemic lupus erythematosus: an ultrasound study of hands and wrists in 108 patients |journal=Rheumatology (Oxford) |volume=51 |issue=12 |pages=2278–85 |year=2012 |pmid=22956550 |doi=10.1093/rheumatology/kes226 |url=}}</ref><ref name="pmid19591780">{{cite journal |vauthors=Grossman JM |title=Lupus arthritis |journal=Best Pract Res Clin Rheumatol |volume=23 |issue=4 |pages=495–506 |year=2009 |pmid=19591780 |doi=10.1016/j.berh.2009.04.003 |url=}}</ref><ref name="pmid24862229">{{cite journal |vauthors=Zhu KK, Xu WD, Pan HF, Zhang M, Ni J, Ge FY, Ye DQ |title=The risk factors of avascular necrosis in patients with systemic lupus erythematosus: a meta-analysis |journal=Inflammation |volume=37 |issue=5 |pages=1852–64 |year=2014 |pmid=24862229 |doi=10.1007/s10753-014-9917-y |url=}}</ref><ref name="pmid23731640">{{cite journal |vauthors=Voulgari PV, Kosta P, Argyropoulou MI, Drosos AA |title=Avascular necrosis in a patient with systemic lupus erythematosus |journal=Joint Bone Spine |volume=80 |issue=6 |pages=665 |year=2013 |pmid=23731640 |doi=10.1016/j.jbspin.2013.03.018 |url=}}</ref>=== | |||
*[[Clubbing]] | |||
*[[Cyanosis]] | |||
*[[Muscle weakness|Muscle atrophy or weakness]] | |||
*[[Livedo reticularis]] | |||
**Reddish-cyanotic, reticular pattern on the skin of the arms, legs, and torso, particularly with cold exposure | |||
*[[Arthritis]] | |||
**Symmetrical | |||
**Polyarticular | |||
**Mostly involve knees, carpal joints, and joints of the fingers, especially the proximal [[interphalangeal]] (PIP) joint | |||
**Decrease range of motion in affected joints | |||
*Joints [[erythema]] | |||
**Due to [[synovitis]] | |||
*Joint effusion | |||
*Muscle [[atrophy]] | |||
*[[Fasciculations]] in the upper/lower extremity | |||
*[[Claudication]] | |||
*Loss of digit or limb | |||
===Neuromuscular<ref name="pmid19366083">{{cite journal |vauthors=Cojocaru IM, Cojocaru M, Tănăsescu R, Burcin C, Atanasiu AN, Silosi I |title=Detection of autoantibodies to ribosome P in lupus patients with neurological involvement |journal=Rom J Intern Med |volume=46 |issue=3 |pages=239–42 |year=2008 |pmid=19366083 |doi= |url=}}</ref><ref name="pmid22594009">{{cite journal |vauthors=Madrane S, Ribi C |title=[Central neuropsychiatric involvement in systemic lupus erythematosus] |language=French |journal=Rev Med Suisse |volume=8 |issue=337 |pages=848–53 |year=2012 |pmid=22594009 |doi= |url=}}</ref><ref name="pmid7555923">{{cite journal |vauthors=Sivri A, Hasçelik Z, Celiker R, Başgöze O |title=Early detection of neurological involvement in systemic lupus erythematosus patients |journal=Electromyogr Clin Neurophysiol |volume=35 |issue=4 |pages=195–9 |year=1995 |pmid=7555923 |doi= |url=}}</ref><ref name="pmid19217587">{{cite journal |vauthors=Juncal Gallego L, Almuíña Simón C, Muíños Esparza LF, Díaz Soto R, Ramil Fraga C, Quiroga Ordóñez E |title=[Systemic lupus erythematosus with fulminant neurological involvement] |language=Spanish; Castilian |journal=An Pediatr (Barc) |volume=70 |issue=2 |pages=202–4 |year=2009 |pmid=19217587 |doi=10.1016/j.anpedi.2008.09.009 |url=}}</ref>=== | |||
*Patient is usually oriented to persons, place, and time based on the disease course | |||
*[[Cognitive impairment]] | |||
*[[Hallucination|Hallucinations]] | |||
**[[Visual hallucinations|Visual]] | |||
**[[Auditory hallucinations|Auditory]] | |||
*Memory deficit | |||
**Loose associations | |||
**Impoverished thought content | |||
**Illogical thinking | |||
**Bizarre disorganised or catatonic behaviour | |||
==Gallery== | |||
<gallery perrow="3"> | |||
Image:Systemic lupus erythematosus 052.jpg|Skin: Lupus, systemic erythematosus; Discoid skin lesion in patient with SLE. <SMALL><SMALL>''[http://www.peir.net Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.]''<ref name="Dermatology Atlas">{{Cite web | title = Dermatology Atlas | url = http://www.atlasdermatologico.com.br/}}</ref> | Image:Systemic lupus erythematosus 052.jpg|Skin: Lupus, systemic erythematosus; Discoid skin lesion in patient with SLE. <SMALL><SMALL>''[http://www.peir.net Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.]''<ref name="Dermatology Atlas">{{Cite web | title = Dermatology Atlas | url = http://www.atlasdermatologico.com.br/}}</ref> | ||
Image:Systemic lupus erythematosus 053.jpg|Skin: ulcer, necrotic; lupus anticoagulant in thigh. [http://www.peir.net Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.]''<ref name="Dermatology Atlas">{{Cite web | title = Dermatology Atlas | url = http://www.atlasdermatologico.com.br/}}</ref> | Image:Systemic lupus erythematosus 053.jpg|Skin: ulcer, necrotic; lupus anticoagulant in thigh. [http://www.peir.net Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.]''<ref name="Dermatology Atlas">{{Cite web | title = Dermatology Atlas | url = http://www.atlasdermatologico.com.br/}}</ref> | ||
| Line 28: | Line 143: | ||
======Head====== | ======Head====== | ||
<gallery> | <gallery> | ||
Image:Discoid lupus erythematosus28.jpg|Discoid lupus erythematosus. <SMALL><SMALL>''[http://www.atlasdermatologico.com.br/ Adapted from Dermatology Atlas.]''<ref name="Dermatology Atlas">{{Cite web | title = Dermatology Atlas | url = http://www.atlasdermatologico.com.br/}}</ref></SMALL></SMALL> | Image:Discoid lupus erythematosus28.jpg|500px|Discoid lupus erythematosus. <SMALL><SMALL>''[http://www.atlasdermatologico.com.br/ Adapted from Dermatology Atlas.]''<ref name="Dermatology Atlas">{{Cite web | title = Dermatology Atlas | url = http://www.atlasdermatologico.com.br/}}</ref></SMALL></SMALL> | ||
| Line 105: | Line 220: | ||
</gallery> | </gallery> | ||
=====Face===== | =====Face===== | ||
<gallery> | <gallery> | ||
Latest revision as of 19:03, 4 August 2017
|
Systemic lupus erythematosus Microchapters |
|
Differentiating Systemic lupus erythematosus from other Diseases |
|---|
|
Diagnosis |
|
Treatment |
|
Case Studies |
|
Systemic lupus erythematosus physical examination On the Web |
|
American Roentgen Ray Society Images of Systemic lupus erythematosus physical examination |
|
Systemic lupus erythematosus physical examination in the news |
|
Directions to Hospitals Treating Systemic lupus erythematosus |
|
Risk calculators and risk factors for Systemic lupus erythematosus physical examination |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Mahshid Mir, M.D. [2]
Overview
In the earlier stages of the disease, patients appear well, while in the late stages of the disease, patients are clearly ill with multi-organ involvement. The patient may show a wide range of skin manifestations including urticaria, bullous lesions, malar rash, and scarring alopecia. The patient may develop nasal and oral ulcers. Arthritis may lead to a decreased range of motion, joint effusion, and arthralgia. Neurological manifestations including psychosis, cognitive impairment, and hallucinations, may also be present.
Physical Examination
Appearance of the Patient
- Patient appears well in the earlier stages of the disease
- Patient appears ill in the late stages of the disease due to multi-organ involvement
Vital Signs
- Fever higher than 38 after the exclusion of infection
- Tachycardia/bradycardia depends on the accompanying complication
- Tachypnea/bradypnea depends on the accompanying complication
Skin[1][2][3]
- Cyanosis
- Secondary to respiratory complications
- Jaundice
- Secondary to hepatitis
- Pallor
- Secondary to anemia
- Generalised erythema
- Bruises
- Secondary to thrombocytopenia
- Urticaria
- Bullous lesions
- Sclerodactyly
- Skin ulceration
- Malar rash: the classic lupus ‘butterfly’ rash
- Erythematous, elevated lesion, pruritic or painful, in a malar distribution, commonly precipitated by exposure to sunlight
- Annular or psoriasiform skin lesions
- Small, erythematous, slightly scaly papules that evolve into either a psoriasiform (papulosquamous) or annular form and tend to involve shoulders, forearms, neck, and upper torso
- Scarring chronic alopecia
- Mostly present on face, neck, and scalp
- Telangiectasias
- Dyspigmentation (hyperpigmentation or hypopigmentation) of skin in scar places
- Follicular plugging
- Discrete, erythematous, slightly infiltrated plaques covered by a well-formed adherent scale that extends into dilated hair follicles
- Nodules
- Can be firm (Lupus profundus) and painful
- Photodistributed lesions with chronic pink indurated plaques or broad lesions that are slow to heal (more seen in lupus tumidus)
- Thin hair that easily fractures (lupus hair)
- Irregularly shaped raised white plaques, areas of erythema, silvery white scarred lesions, and ulcers with surrounding erythema on the soft or hard palate or buccal mucosa
- Periungual erythema
- Dilated tortuous loops of capillaries and a prominent subcapillary venous plexus along
- Involves the base of the nail and edges of the upper eyelid
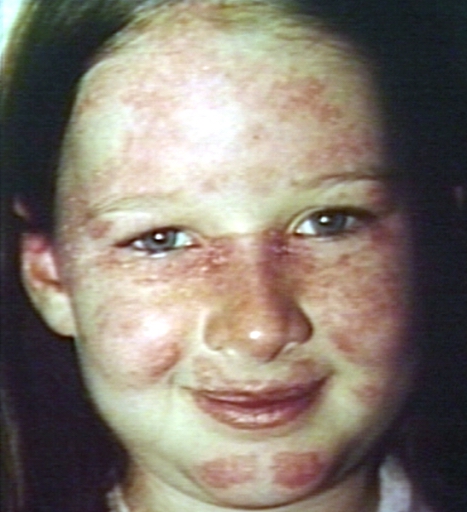 For more pictures of the rash presentation in lupus, click here.
For more pictures of the rash presentation in lupus, click here.
HEENT
- Ophthalmology[4][5]
- Nystagmus
- Visual retinal changes from systemic lupus erythematosus cytoid bodies, retinal haemorrhages, serous exudate or haemorrhage in the choroid, optic neuritis (not due to hypertension, drugs or infection)
- Cataract
- Optic nerve atrophy
- Icteric sclera
- Cotton wool spots in the retina in ophthalmoscopic exam
- Nasal ulcers[6]
- Mostly painless
- Mostly in lower nasal septum and bilateral and parallel
- Nasal perforation secondary to vasculitis may happen rarely
- Oral ulcers[7][8]
- Mostly painless
- White plaques with areas of erythema, or punched-out erosions or ulcers with surrounding erythema on the soft or hard palate or buccal mucosa
Neck[9][10]
- Jugular venous distension
- Secondary to hypertension and cardiac complications
- Lymphadenopathy
- Lymph nodes are soft, non-tender, discrete
- Usually detected in the cervical, axillary, and inguinal
Lungs[11][12][13]
- Fine and coarse crackles upon auscultation of the lung
- May be due to pneumonitis
- In case of pleural effusion:
- Asymmetric tactile fremitus
- Asymmetric chest expansion
Heart[14][10][15]
- Chest tenderness or discomfort upon palpation
- May be due to costochondritis
- Diastolic murmur, or systolic murmur >3/6 due to valvular disease
- Loud second heart sound (due to pulmonary hypertension)
- Loud S1-S2 due to cardiomegaly
- Decrease heart sounds if associated with pericardial effusion
Abdomen[16][17][18][19]
- Abdominal distention
- Ascites
- Due to nephrotic syndrome
- Abdominal pain
- Due to mesentric vasculitis
- Hepatomegaly
- Splenomegaly
- Costo-vertebral angle tenderness
Extremities[20][21][22][23][24]
- Clubbing
- Cyanosis
- Muscle atrophy or weakness
- Livedo reticularis
- Reddish-cyanotic, reticular pattern on the skin of the arms, legs, and torso, particularly with cold exposure
- Arthritis
- Symmetrical
- Polyarticular
- Mostly involve knees, carpal joints, and joints of the fingers, especially the proximal interphalangeal (PIP) joint
- Decrease range of motion in affected joints
- Joints erythema
- Due to synovitis
- Joint effusion
- Muscle atrophy
- Fasciculations in the upper/lower extremity
- Claudication
- Loss of digit or limb
Neuromuscular[25][26][27][28]
- Patient is usually oriented to persons, place, and time based on the disease course
- Cognitive impairment
- Hallucinations
- Memory deficit
- Loose associations
- Impoverished thought content
- Illogical thinking
- Bizarre disorganised or catatonic behaviour
Gallery
-
Skin: Lupus, systemic erythematosus; Discoid skin lesion in patient with SLE. Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.[29]
-
Skin: ulcer, necrotic; lupus anticoagulant in thigh. Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.[29]
-
Skin: lupus, erythematosus, subacute; Papulosquamous diseases. Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.[29]
-
Skin: lupus, erythematosus; Papulosquamous diseases. Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.[29]
-
Skin: lupus, erythematosus; papulosquamous diseases. Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.[29]
Discoid Lupus Erythematosus
Head
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
Face
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
-
Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]
Lupus Erythematosus-Systemic
Face
-
Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]
-
Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]
-
Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]
-
Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]
Extremity
-
Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]
-
Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]
-
Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]
Trunk
-
Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]
Lupus Erythematosus Chronicus Disseminatus Superficialis
-
Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]
Lupus Erythematosus Chronicus Verrucous
-
Lupus Erythematosus Chronicus Verrucous. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus Chronicus Verrucous. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus Chronicus Verrucous. Adapted from Dermatology Atlas.[29]
Lupus Erythematosus Profundus
-
Lupus Erythematosus Profundu. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus Profundu. Adapted from Dermatology Atlas.[29]
Lupus Erythematosus-Subacute Cutaneous Lupus Erythematosus
-
Lupus Erythematosus-Subacute Cutaneous Lupus Erythematosus. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus-Subacute Cutaneous Lupus Erythematosus. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus-Subacute Cutaneous Lupus Erythematosus. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus-Subacute Cutaneous Lupus Erythematosus. Adapted from Dermatology Atlas.[29]
-
Lupus Erythematosus-Subacute Cutaneous Lupus Erythematosus. Adapted from Dermatology Atlas.[29]
Lupus Vulgaris
-
Lupus Vulgaris. Adapted from Dermatology Atlas.[29]
-
Lupus Vulgaris. Adapted from Dermatology Atlas.[29]
References
- ↑ Parodi A, Cozzani E (2014). "Cutaneous manifestations of lupus erythematosus". G Ital Dermatol Venereol. 149 (5): 549–54. PMID 25077888.
- ↑ Szczęch J, Rutka M, Samotij D, Zalewska A, Reich A (2016). "Clinical characteristics of cutaneous lupus erythematosus". Postepy Dermatol Alergol. 33 (1): 13–7. doi:10.5114/pdia.2014.44031. PMC 4793050. PMID 26985173.
- ↑ Walling HW, Sontheimer RD (2009). "Cutaneous lupus erythematosus: issues in diagnosis and treatment". Am J Clin Dermatol. 10 (6): 365–81. doi:10.2165/11310780-000000000-00000. PMID 19824738.
- ↑ Preble JM, Silpa-archa S, Foster CS (2015). "Ocular involvement in systemic lupus erythematosus". Curr Opin Ophthalmol. 26 (6): 540–5. doi:10.1097/ICU.0000000000000209. PMID 26367085.
- ↑ Silpa-archa S, Lee JJ, Foster CS (2016). "Ocular manifestations in systemic lupus erythematosus". Br J Ophthalmol. 100 (1): 135–41. doi:10.1136/bjophthalmol-2015-306629. PMID 25904124.
- ↑ Robson AK, Burge SM, Millard PR (1992). "Nasal mucosal involvement in lupus erythematosus". Clin Otolaryngol Allied Sci. 17 (4): 341–3. PMID 1526055.
- ↑ Anyanwu CO, Ang CC, Werth VP (2013). "Oral mucosal involvement in bullous lupus". Arthritis Rheum. 65 (10): 2622. doi:10.1002/art.38051. PMC 4333153. PMID 23780804.
- ↑ Ranginwala AM, Chalishazar MM, Panja P, Buddhdev KP, Kale HM (2012). "Oral discoid lupus erythematosus: A study of twenty-one cases". J Oral Maxillofac Pathol. 16 (3): 368–73. doi:10.4103/0973-029X.102487. PMC 3519212. PMID 23248469.
- ↑ Melikoglu MA, Melikoglu M (2008). "The clinical importance of lymphadenopathy in systemic lupus erythematosus". Acta Reumatol Port. 33 (4): 402–6. PMID 19107085.
- ↑ 10.0 10.1 Sacre K, Escoubet B, Pasquet B, Chauveheid MP, Zennaro MC, Tubach F, Papo T (2014). "Increased arterial stiffness in systemic lupus erythematosus (SLE) patients at low risk for cardiovascular disease: a cross-sectional controlled study". PLoS ONE. 9 (4): e94511. doi:10.1371/journal.pone.0094511. PMC 3983200. PMID 24722263.
- ↑ Torre O, Harari S (2011). "Pleural and pulmonary involvement in systemic lupus erythematosus". Presse Med. 40 (1 Pt 2): e19–29. doi:10.1016/j.lpm.2010.11.004. PMID 21194884.
- ↑ Salvati F (2015). "[The involvement of pulmonary interstitial tissue in multisystemic lupus erythematosus: interdisciplinarity and role of the pneumologists]". Clin Ter (in Italian). 166 (5): 205–7. PMID 26550810.
- ↑ Alamoudi OS, Attar SM (2015). "Pulmonary manifestations in systemic lupus erythematosus: association with disease activity". Respirology. 20 (3): 474–80. doi:10.1111/resp.12473. PMC 4418345. PMID 25639532.
- ↑ Mak A, Kow NY (2014). "Imbalance between endothelial damage and repair: a gateway to cardiovascular disease in systemic lupus erythematosus". Biomed Res Int. 2014: 178721. doi:10.1155/2014/178721. PMC 3984775. PMID 24790989.
- ↑ Canpolat N, Kasapcopur O, Caliskan S, Gokalp S, Bor M, Tasdemir M, Sever L, Arisoy N (2013). "Ambulatory blood pressure and subclinical cardiovascular disease in patients with juvenile-onset systemic lupus erythematosus". Pediatr. Nephrol. 28 (2): 305–13. doi:10.1007/s00467-012-2317-3. PMID 23052654.
- ↑ Tian XP, Zhang X (2010). "Gastrointestinal involvement in systemic lupus erythematosus: insight into pathogenesis, diagnosis and treatment". World J. Gastroenterol. 16 (24): 2971–7. PMC 2890936. PMID 20572299.
- ↑ Alves SC, Fasano S, Isenberg DA (2016). "Autoimmune gastrointestinal complications in patients with systemic lupus erythematosus: case series and literature review". Lupus. 25 (14): 1509–1519. doi:10.1177/0961203316655210. PMID 27329649.
- ↑ Fawzy M, Edrees A, Okasha H, El Ashmaui A, Ragab G (2016). "Gastrointestinal manifestations in systemic lupus erythematosus". Lupus. 25 (13): 1456–1462. doi:10.1177/0961203316642308. PMID 27055518.
- ↑ Li Z, Xu D, Wang Z, Wang Y, Zhang S, Li M, Zeng X (2017). "Gastrointestinal system involvement in systemic lupus erythematosus". Lupus: 961203317707825. doi:10.1177/0961203317707825. PMID 28523968.
- ↑ Zoma A (2004). "Musculoskeletal involvement in systemic lupus erythematosus". Lupus. 13 (11): 851–3. doi:10.1191/0961203303lu2021oa. PMID 15580980.
- ↑ Gabba A, Piga M, Vacca A, Porru G, Garau P, Cauli A, Mathieu A (2012). "Joint and tendon involvement in systemic lupus erythematosus: an ultrasound study of hands and wrists in 108 patients". Rheumatology (Oxford). 51 (12): 2278–85. doi:10.1093/rheumatology/kes226. PMID 22956550.
- ↑ Grossman JM (2009). "Lupus arthritis". Best Pract Res Clin Rheumatol. 23 (4): 495–506. doi:10.1016/j.berh.2009.04.003. PMID 19591780.
- ↑ Zhu KK, Xu WD, Pan HF, Zhang M, Ni J, Ge FY, Ye DQ (2014). "The risk factors of avascular necrosis in patients with systemic lupus erythematosus: a meta-analysis". Inflammation. 37 (5): 1852–64. doi:10.1007/s10753-014-9917-y. PMID 24862229.
- ↑ Voulgari PV, Kosta P, Argyropoulou MI, Drosos AA (2013). "Avascular necrosis in a patient with systemic lupus erythematosus". Joint Bone Spine. 80 (6): 665. doi:10.1016/j.jbspin.2013.03.018. PMID 23731640.
- ↑ Cojocaru IM, Cojocaru M, Tănăsescu R, Burcin C, Atanasiu AN, Silosi I (2008). "Detection of autoantibodies to ribosome P in lupus patients with neurological involvement". Rom J Intern Med. 46 (3): 239–42. PMID 19366083.
- ↑ Madrane S, Ribi C (2012). "[Central neuropsychiatric involvement in systemic lupus erythematosus]". Rev Med Suisse (in French). 8 (337): 848–53. PMID 22594009.
- ↑ Sivri A, Hasçelik Z, Celiker R, Başgöze O (1995). "Early detection of neurological involvement in systemic lupus erythematosus patients". Electromyogr Clin Neurophysiol. 35 (4): 195–9. PMID 7555923.
- ↑ Juncal Gallego L, Almuíña Simón C, Muíños Esparza LF, Díaz Soto R, Ramil Fraga C, Quiroga Ordóñez E (2009). "[Systemic lupus erythematosus with fulminant neurological involvement]". An Pediatr (Barc) (in Spanish; Castilian). 70 (2): 202–4. doi:10.1016/j.anpedi.2008.09.009. PMID 19217587.
- ↑ 29.00 29.01 29.02 29.03 29.04 29.05 29.06 29.07 29.08 29.09 29.10 29.11 29.12 29.13 29.14 29.15 29.16 29.17 29.18 29.19 29.20 29.21 29.22 29.23 29.24 29.25 29.26 29.27 29.28 29.29 29.30 29.31 29.32 29.33 29.34 29.35 29.36 29.37 29.38 29.39 29.40 29.41 29.42 29.43 29.44 29.45 29.46 29.47 29.48 29.49 29.50 29.51 29.52 29.53 29.54 29.55 29.56 29.57 29.58 29.59 29.60 29.61 29.62 29.63 29.64 29.65 29.66 29.67 29.68 29.69 29.70 29.71 29.72 29.73 29.74 29.75 29.76 29.77 "Dermatology Atlas".
![Skin: Lupus, systemic erythematosus; Discoid skin lesion in patient with SLE. Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.[29]](/images/d/d6/Systemic_lupus_erythematosus_052.jpg)
![Skin: ulcer, necrotic; lupus anticoagulant in thigh. Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.[29]](/images/c/cd/Systemic_lupus_erythematosus_053.jpg)
![Skin: lupus, erythematosus, subacute; Papulosquamous diseases. Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.[29]](/images/2/26/Systemic_lupus_erythematosus_054.jpg)
![Skin: lupus, erythematosus; papulosquamous diseases. Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.[29]](/images/2/25/Systemic_lupus_erythematosus_056.jpg)
![Skin: discoid lupus, face. Image courtesy of Professor Peter Anderson DVM PhD and published with permission © PEIR, University of Alabama at Birmingham, Department of Pathology.[29]](/images/e/e9/Systemic_lupus_erythematosus_057.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/a/a7/Discoid_lupus_erythematosus28.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/d/d7/Discoid_lupus_erythematosus27.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/f/fe/Discoid_lupus_erythematosus26.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/f/fd/Discoid_lupus_erythematosus17.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/b/b5/Discoid_lupus_erythematosus16.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/d/d4/Discoid_lupus_erythematosus03.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/0/02/Discoid_lupus_erythematosus43.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/b/b5/Discoid_lupus_erythematosus34.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/1/1e/Discoid_lupus_erythematosus38.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/4/44/Discoid_lupus_erythematosus37.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/8/82/Discoid_lupus_erythematosus36.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/8/8b/Discoid_lupus_erythematosus35.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/0/04/Discoid_lupus_erythematosus32.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/a/a9/Discoid_lupus_erythematosus29.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/d/d0/Discoid_lupus_erythematosus30.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/8/8b/Discoid_lupus_erythematosus33.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/2/26/Discoid_lupus_erythematosus31.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/b/ba/Discoid_lupus_erythematosus42.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/b/b5/Discoid_lupus_erythematosus41.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/0/03/Discoid_lupus_erythematosus40.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/2/29/Discoid_lupus_erythematosus39.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/6/67/Discoid_lupus_erythematosus01.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/f/ff/Discoid_lupus_erythematosus02.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/f/f9/Discoid_lupus_erythematosus05.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/f/f9/Discoid_lupus_erythematosus06.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/d/d1/Discoid_lupus_erythematosus07.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/8/86/Discoid_lupus_erythematosus08.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/b/bd/Discoid_lupus_erythematosus09.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/f/fa/Discoid_lupus_erythematosus10.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/2/29/Discoid_lupus_erythematosus11.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/b/b9/Discoid_lupus_erythematosus12.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/d/d3/Discoid_lupus_erythematosus13.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/d/da/Discoid_lupus_erythematosus14.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/2/27/Discoid_lupus_erythematosus15.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/a/af/Discoid_lupus_erythematosus18.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/c/cd/Discoid_lupus_erythematosus20.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/1/12/Discoid_lupus_erythematosus21.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/c/ca/Discoid_lupus_erythematosus22.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/c/c7/Discoid_lupus_erythematosus23.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/5/55/Discoid_lupus_erythematosus24.jpg)
![Discoid lupus erythematosus. Adapted from Dermatology Atlas.[29]](/images/8/8c/Discoid_lupus_erythematosus25.jpg)
![Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]](/images/f/f0/Lupus_erythematosus-systemic01.jpg)
![Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]](/images/1/12/Lupus_erythematosus-systemic02.jpg)
![Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]](/images/6/6a/Lupus_erythematosus-systemic03.jpg)
![Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]](/images/2/25/Lupus_erythematosus-systemic04.jpg)
![Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]](/images/0/09/Lupus_erythematosus-systemic05.jpg)
![Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]](/images/0/09/Lupus_erythematosus-systemic06.jpg)
![Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]](/images/e/e7/Lupus_erythematosus-systemic07.jpg)
![Lupus erythematosus-systemic. Adapted from Dermatology Atlas.[29]](/images/7/72/Lupus_erythematosus-systemic08.jpg)
![Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]](/images/f/f0/L4091.jpg)
![Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]](/images/5/57/L4092.jpg)
![Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]](/images/0/0f/L4094.jpg)
![Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]](/images/5/5c/L4098.jpg)
![Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]](/images/a/ab/L4099.jpg)
![Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]](/images/d/d4/L4100.jpg)
![Lupus Erythematosus Chronicus Disseminatus Superficialis. Adapted from Dermatology Atlas.[29]](/images/8/8f/L4101.jpg)
![Lupus Erythematosus Chronicus Verrucous. Adapted from Dermatology Atlas.[29]](/images/3/37/L4110.jpg)
![Lupus Erythematosus Chronicus Verrucous. Adapted from Dermatology Atlas.[29]](/images/e/e0/L4103.jpg)
![Lupus Erythematosus Profundu. Adapted from Dermatology Atlas.[29]](/images/3/39/L4119.jpg)
![Lupus Erythematosus Profundu. Adapted from Dermatology Atlas.[29]](/images/a/ae/8835.jpg)
![Lupus Erythematosus-Subacute Cutaneous Lupus Erythematosus. Adapted from Dermatology Atlas.[29]](/images/e/e7/L4122.jpg)
![Lupus Erythematosus-Subacute Cutaneous Lupus Erythematosus. Adapted from Dermatology Atlas.[29]](/images/3/3c/L4123.jpg)
![Lupus Erythematosus-Subacute Cutaneous Lupus Erythematosus. Adapted from Dermatology Atlas.[29]](/images/e/e9/L4121.jpg)
![Lupus Erythematosus-Subacute Cutaneous Lupus Erythematosus. Adapted from Dermatology Atlas.[29]](/images/a/a1/L4126.jpg)
![Lupus Erythematosus-Subacute Cutaneous Lupus Erythematosus. Adapted from Dermatology Atlas.[29]](/images/a/a8/L4127.jpg)
![Lupus Vulgaris. Adapted from Dermatology Atlas.[29]](/images/5/59/L4142.jpg)
![Lupus Vulgaris. Adapted from Dermatology Atlas.[29]](/images/5/57/L4146.jpg)