Nipah virus encephalitis epidemiology and demographics
|
Nipah virus encephalitis Microchapters |
|
Differentiating Nipah virus encephalitis from other Diseases |
|---|
|
Diagnosis |
|
Treatment |
|
Case Studies |
|
Nipah virus encephalitis epidemiology and demographics On the Web |
|
American Roentgen Ray Society Images of Nipah virus encephalitis epidemiology and demographics |
|
FDA on Nipah virus encephalitis epidemiology and demographics |
|
CDC on Nipah virus encephalitis epidemiology and demographics |
|
Nipah virus encephalitis epidemiology and demographics in the news |
|
Blogs on Nipah virus encephalitis epidemiology and demographics |
|
Risk calculators and risk factors for Nipah virus encephalitis epidemiology and demographics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Epidemiology and Demographics
Outbreaks
Seven more outbreaks of Nipah virus have occurred since 1998, all within Bangladesh and neighbouring parts of India. The outbreak sites lie within the range of Pteropus species (Pteropus giganteus). As with Hendra virus, the timing of the outbreaks indicates a seasonal effect.
- 2001 January 31 – February 23, Siliguri, India: 66 cases with a 74% mortality rate. 75% of patients were either hospital staff or had visited one of the other patients in hospital, indicating person-to-person transmission.
- 2001 April – May, Meherpur district, Bangladesh: 13 cases with nine fatalities (69% mortality).
- 2003 January, Naogaon district, Bangladesh: 12 cases with eight fatalities (67% mortality).
- 2004 January – February, Manikganj and Rajbari provinces, Bangladesh: 42 cases with 14 fatalities (33% mortality).
- 2004 19 February – 16 April, Faridpur district, Bangladesh: 36 cases with 27 fatalities (75% mortality). Epidemiological evidence strongly suggests that this outbreak involved person-to-person transmission of Nipah virus, which had not previously been confirmed. 92% of cases involved close contact with at least one other person infected with Nipah virus. Two cases involved a single short exposure to an ill patient, including a rickshaw driver who transported a patient to hospital. In addition, at least six cases involved acute respiratory distress syndrome which has not been reported previously for Nipah virus illness in humans. This symptom is likely to have assisted human-to-human transmission through large droplet dispersal.
- 2005 January, Tangail district, Bangladesh: 12 cases with 11 fatalities (92% mortality). The virus was probably contracted from drinking date palm juice contaminated by fruit bat droppings or saliva.
- 2007 February – May, Nadia District, India: up to 50 cases with five fatalities. The outbreak site borders the Bangladesh district of Kushtia where 50 suspected cases of Nipah virus encephalitis with six fatalities occurred during April 2007.
Eleven isolated cases of Nipah virus encephalitis have also been documented in Bangladesh since 2001.
Nipah virus has been isolated from Lyle's flying fox (Pteropus lylei) in Cambodia and viral RNA found in urine and saliva from P. lylei and Horsfield's roundleaf bat (Hipposideros larvartus) in Thailand. Antibodies to henipaviruses have also been found in fruit bats (Pteropus rufus, Eidolon dupreanum) in Madagascar indicating a wide geographic distribution of the viruses. No infection of humans or other species have been observed in Cambodia, Thailand or Madagascar.
Hendra Virus
Emergence
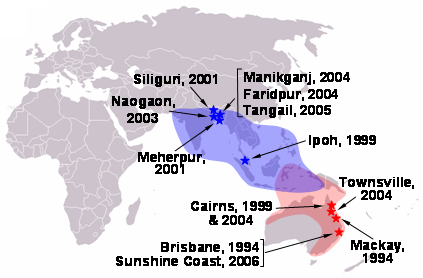
Hendra virus (originally Equine morbillivirus) was discovered in September 1994 when it caused the deaths of thirteen horses, and the prominent horse trainer Vic Rail at a training complex in Hendra, a suburb of Brisbane in Queensland, Australia.
The index case, a mare, was housed with 23 other horses after falling ill and died two days later. Subsequently, 19 of the remaining horses succumbed with 12 dying. Both the trainer and a stable hand were involved in nursing the index case and both fell ill within one week of the horse’s death with an influenza-like illness. The stable hand recovered while the trainer died of respiratory and renal failure. The source of virus was most likely frothy nasal discharge from the index case.
A second outbreak occurred in August 1994 (chronologically preceding the first outbreak) in Mackay 1000km north of Brisbane resulting in the deaths of two horses and their owner. The owner assisted in autopsies of the horses and within three weeks was admitted to hospital suffering from meningitis. He recovered, but 14 months later developed neurologic signs and died. This outbreak was diagnosed retrospectively by the presence of Hendra virus in the brain of the patient.
A survey of wildlife in the outbreak areas was conducted and identified pteropid fruit bats as the most likely source of Hendra virus with a seroprevalence of 47%. All of the other 46 species sampled were negative. Virus isolations from the reproductive tract and urine of wild bats indicated that transmission to horses may have occurred via exposure to bat urine or birthing fluids.
Outbreaks
Four more incidents, in Cairns in January 1999 and October 2004, in Townsville in December 2004 and on the Sunshine Coast in June 2006 each resulted in the death of one horse. A vet involved in autopsy of the horse from the 2004 Townsville incident developed a Hendra-related illness soon after and recovered.
The distribution of black and spectacled flying foxes covers Townsville and Cairns, and the timing of incidents indicates a seasonal pattern of outbreaks possibly related to the seasonality of fruit bat birthing. As there is no evidence of transmission to humans directly from bats, it is thought that human infection only occurs via an intermediate host.
Infection/Transmission
Where are Hendra and Nipah viruses found?
The natural reservoir for Hendra virus is thought to be flying foxes (bats of the genus Pteropus) found in Australia. The natural reservoir for Nipah virus is still under investigation, but preliminary data suggest that bats of the genus Pteropus are also the reservoirs for Nipah virus in Malaysia.
Where are the diseases found?
Hendra virus caused disease in horses in Australia, and the human infections there were due to direct exposure to tissues and secretions from infected horses. Nipah virus caused a relatively mild disease in pigs in Malaysia and Singapore. Nipah virus was transmitted to humans, cats, and dogs through close contact with infected pigs.