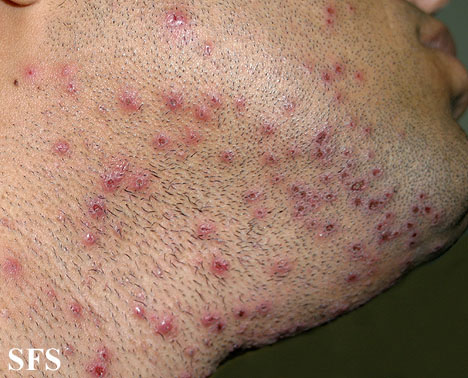
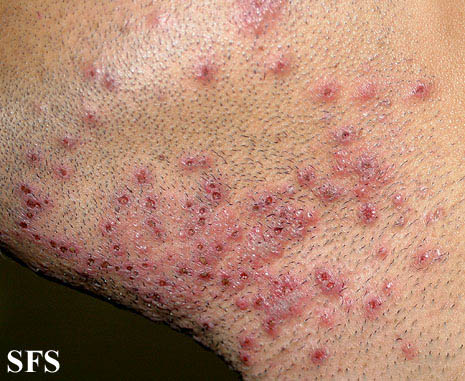
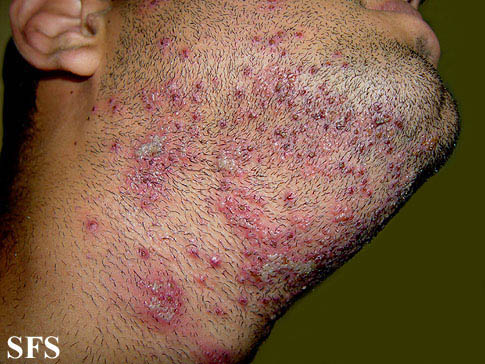
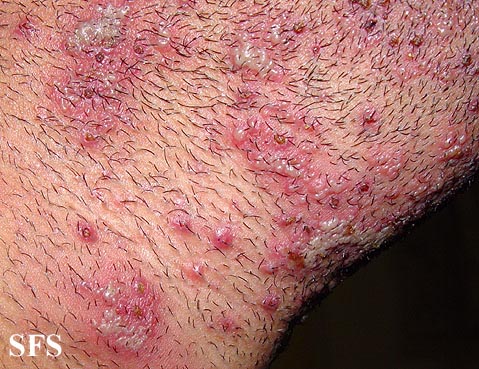
Hidradenitis suppurativa
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Jesus Rosario Hernandez, M.D. [2].
Synonyms and keywords:: Acne inversa, Velpeau's disease, Verneuil's disease.
Overview
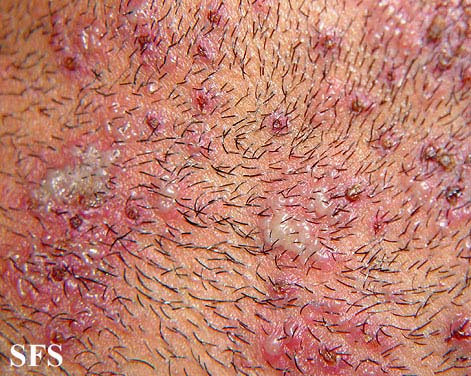
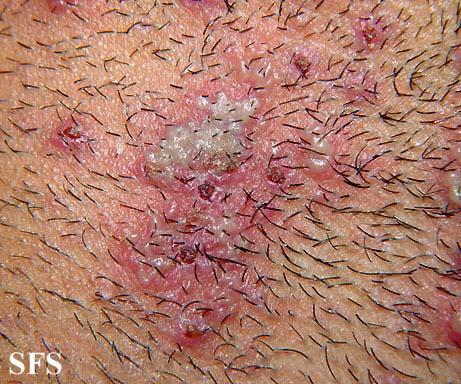
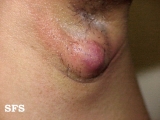
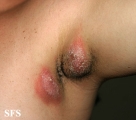
Hidradenitis suppurativa or HS is a skin disease that affects areas bearing apocrine sweat glands and hair follicles; such as the underarms, groin and buttocks. It is more commonly found in women and can be present under the breasts.
The disease manifests as clusters of chronic abscesses or boils, sometimes as large as baseballs, that are extremely painful to the touch and may persist for years with occasional to frequent periods of inflammation, culminating in drainage of pus, often leaving open wounds that will not heal. Drainage provides some relief from severe, often debilitating, pressure pain. Flare-ups may be triggered by stress, perspiration, hormonal changes (such as monthly cycles in women), humid heat, and clothing friction. Persistent lesions may lead to scarring and the formation of sinus tracts, or tunnels connecting the abscesses under the skin. At this stage, complete healing is usually not possible, and progression varies from person to person, with some experiencing remission anywhere from months to years at a time, others may worsen and require surgery in order to live comfortably. Occurrences of bacterial infections and cellulitis (deep tissue inflammation) may occur at these sites. HS pain can be difficult to manage.[1]
HS often goes undiagnosed for years because patients are too ashamed to speak with anyone.[1] When they do see a doctor, the disease is frequently misdiagnosed or prescribed treatments are ineffective, temporary and sometimes even harmful. There is no known cure nor any consistently effective treatment. Carbon dioxide laser surgery is currently considered the last resort for those who have advanced to its highest stage, where the affected areas are excised, and the skin is grafted. Surgery doesn't always alleviate the condition, however, and can be very expensive.
It is possible that there is genetic predisposition to the disease.[2] HS is not contagious, and is not affected nor caused by good or bad hygiene. HS is often called an 'orphan illness', due to little research being conducted on the disease at this time. Because HS is considered a rare disease, its incidence rate is not well known, but has been estimated as being between 1:24 (4.1%) and 1:600 (0.2%).[3]
Other names for HS
Hidradenitis suppurativa has been referred to by multiple names in the literature, as well as in various cultures. Some of these are also used to describe different diseases, or specific instances of this disease.[1]
- Acne conglobata - not really a synonym - this is a similar process but in classic acne areas of chest and back
- Acne Inversa (AI) - a new term struggling for acceptance
- Apocrine Acne - a misnomer, out-dated, based on the disproven concept that apocrine glands are primarily involved
- Apocrinitis - another misnomer, out-dated, based on the disproven concept that apocrine glands are primarily involved
- Fox-den disease - a catchy term not used in medical literature, based on the deep fox den / burrow - like sinuses
- Hidradenitis Supportiva - a misspelling
- Pyodermia sinifica fistulans - an older term, considered archaic now, misspelled here
- Velpeau's disease - commemorating the French surgeon who first described the disease in 1833
- Verneuil's disease - recognizing the French surgeon whose name is most often associated with the disorder as a result of his 1854-1865 studies[4]
Stages
HS presents itself in three stages.[1][5]
- Solitary or multiple isolated abscess formation without scarring or sinus tracts. (A few minor sites with rare inflammation; may be mistaken for acne.)
- Recurrent abscesses, single or multiple widely separated lesions, with sinus tract formation. (Frequent inflammations restrict movement and may require minor surgery such as incision and drainage.)
- Diffuse or broad involvement across a regional area with multiple interconnected sinus tracts and abscesses. (Inflammation of sites to the size of golf balls, or sometimes baseballs; scarring develops, including subcutaneous tracts of infection - see fistula. Obviously, patients at this stage may be unable to function.)
Causes
As this disease is poorly studied, the causes are controversial and experts disagree. However, potential indicators include:
- post-pubescent
- females are more likely than males
- genetic predisposition
- plugged apocrine (sweat) gland or hair follicle
- excessive sweating
- bacterial infection
- sometimes linked with other auto-immune conditions[6]
- androgen dysfunction
- genetic disorders that alter cell structure
- stress can bring on outbreaks
- being overweight makes it worse, however this condition is not caused by obesity and weight loss will improve but not cure it.
- cigarette smoking tends to encourage outbreaks as well
The historical understanding of the disease is that there is a misfunction in either the apocrine glands[5] or hair follicles,[7] possibly triggered by a blocked gland, creating inflammation, pain, and a swollen lesion. More recent studies imply there is an autoimmune component.
HS is not caused by any bacterial infection -- any infection is secondary. Most cultures done on HS lesions come back negative for bacteria, so antibiotics should be used only when a bacterial infection has been confirmed by a physician. Hidradenitis suppurativa is not contagious.
Severe complications
Left undiscovered, undiagnosed, or untreated, the fistulas from severe stage-3 HS can lead to the development of squamous cell carcinoma in the anus or other affected areas. [8][9]
Treatments
Treatments may vary depending upon presentation and severity of the disease. Due to the poorly-studied nature of this disease, the effectiveness of the drugs and therapies listed below is not yet clear, and patients should discuss all options with their doctor or dermatologist. Nearly a quarter of patients state that nothing relieves their symptoms.[10] A list of treatments that are possible treatments for some patients is as follows.
- lifestyle
- changes in diet
- warm compresses, baths (to induce drainage)
- medication
- intralesional corticosteroid injections (to reduce inflammation)
- oral antibiotics (to treat inflammation and bacterial infection)
- isotretinoin (Accutane®), a prescription-only oral acne treatment (benefits for HS are very controversial, but it is generally considered to be ineffective)
- anti-androgen therapy
- sub-cutaneous injection or IV infusion of anti-inflammatory (anti-TNF-alpha) drugs such as infliximab (Remicade®) and etanercept[11] (Enbrel®). This use of the drugs is not currently Food and Drug Administration (FDA) approved and is somewhat controversial, and therefore may not be covered by insurance.
- Acitretin
- surgery
- incision and drainage or lancing
- wide local excision (with or without skin grafting), or laser surgery
- radiotherapy
Physical examination
Gallery
Head
References
- ↑ 1.0 1.1 1.2 1.3 "HS-USA :: What is Hidradenitis Suppurativa?".
- ↑ "Journal of Investigative Dermatology - Abstract of article: Inversa Acne (Hidradenitis Suppurativa): A Case Report and Identification of the Locus at Chromosome 1p21.1-1q25.3".
- ↑ "HS-USA :: Prevalence of Hidradenitis Suppurativa".
- ↑ Verneuil AS: Etudes sur les tumor de la peau. Arch Gen Med 1854; 94: 693.
- ↑ 5.0 5.1 "Hidradenitis suppurativa. DermNet NZ".
- ↑ "Clinical Trial: Etanercept in Hidradenitis Suppurativa".
- ↑ "HSF - What is Hidradenitis Suppurativa? What is HS?".
- ↑ Talmont, et al., 2005
- ↑ Short KA, Kalu G, Mortimer PS, Higgins EM (2005). "Vulval squamous cell carcinoma arising in chronic hidradenitis suppurativa". Clin. Exp. Dermatol. 30 (5): 481–3. doi:10.1111/j.1365-2230.2005.01875.x. PMID 16045671.
- ↑ "abscesses.org - About Hidradenitis Suppurativa".
- ↑ Cusack C, Buckley C (2006). "Etanercept: effective in the management of hidradenitis suppurativa". Br. J. Dermatol. 154 (4): 726–9. doi:10.1111/j.1365-2133.2005.07067.x. PMID 16536817.