Autopsy
|
WikiDoc Resources for Autopsy |
|
Articles |
|---|
|
Most recent articles on Autopsy |
|
Media |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Autopsy at Clinical Trials.gov Clinical Trials on Autopsy at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Autopsy
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Directions to Hospitals Treating Autopsy Risk calculators and risk factors for Autopsy
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Autopsy |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Overview
An autopsy, also known as a post-mortem examination, necropsy, or obduction, is a medical procedure that consists of a thorough examination of a corpse to determine the cause and manner of death and to evaluate any disease or injury that may be present. It is usually performed by a specialized medical doctor called a pathologist.
Autopsies are either performed for legal or medical purposes. A forensic autopsy is carried out when the cause of death may be a criminal matter, while a clinical or academic autopsy is performed to find the medical cause of death and is used in cases of unknown or uncertain death, or for research purposes. Autopsies can be further classified into cases where external examination suffices, and those where the body is dissected and an internal examination is conducted. Permission from next of kin may be required for internal autopsy in some cases. Once an internal autopsy is complete the body is reconstituted by sewing it back together.
Necropsy is the term for a post-mortem examination performed on an animal. The prefix 'auto-' means 'self', and so autopsy denotes the human species performing a post-mortem examination on one of its own.
Value of autopsy in medicine
Autopsies are important in clinical medicine as they often shed light on medical error and can be used to help guide continuous improvement.
A study that focused on myocardial infarction (heart attack) as a cause of death found significant errors of omission and commission,[1] i.e. a sizable number cases ascribed to myocardial infarctions (MIs) were not MIs and a significant number of non-MIs were actually MIs.
A systematic review of studies of the autopsy calculated that in about 25% of autopsies a major diagnostic error will be revealed.[2] However, this rate has decreased over time and the study projects that in a contemporary US institution, 8.4% to 24.4% of autopsies will detect major diagnostic errors.
A large meta-analysis suggested that approximately one third of death certificates are incorrect and that half of the autopsies performed produced findings that were not suspected before the person died.[3] Also, it is thought that over one fifth of unexpected findings can only be diagnosed histologically, i.e. by biopsy or autopsy, and that approximately one quarter of unexpected findings, or 5% of all findings, are major and can similarly only be diagnosed from tissue.
Value of autopsy in intensive care unit
One study found 32% major diagnositic errors (Class I and Class II) with the leading missed diagnoses being "Autopsies revealed 171 missed diagnoses, including 21 cancers, 12 strokes, 11 myocardial infarctions, 10 pulmonary emboli, and 9 endocarditis, among others".[4]
Focusing intubated patients, one study found "abdominal pathologic conditions--abscesses, bowel perforations, or infarction--were as frequent as pulmonary emboli as a cause of class I errors. While patients with abdominal pathologic conditions generally complained of abdominal pain, results of examination of the abdomen were considered unremarkable in most patients, and the symptom was not pursued".[5]
General information
The term "autopsy" derives from the Greek for "to see for oneself". "Necropsy" is from the Greek for "seeing a dead body".
There are four main types of autopsies:
- Forensic: This is done for medical-legal purposes, and is the one that is normally seen on television or in the news. This type depict an extensive methodology and tends to be complete and comprehensive. No family permission is required to complete this type of autopsy.
- Clinical/academic: This is usually performed in hospitals to for research and study purposes. For a clinical autopsy to take place a cause of death must have already been established and a death certificate completed. This usually is as comprehensive as it needs to be adequate. To complete this type of autopsy, permission from the deceased's legal next of kin is required.
- Coroner's: In Great Britain this type of autopsy encompasses cases where no medical cause of death is readily available. Cause, manner and mechanism of death are in question. Eventually, the prosectors will identify whether the cases deserve comprehensive forensic autopsy or a routine postmortem. In the United States, each state has a set of guidelines defining a "coroner's case" for autopsy, for example: hospital deaths occurring within 24 hours of admission or within 24 hours of a major surgical procedure, with any history (current or remote) of illegal drug or alcohol abuse by the deceased, patients with certain communicable diseases (HIV, hepatitis C virus, etc.), patients with any previous history of violent injury (e.g., gunshot wound many years before death). These cases may or may not be also considered "forensic" in nature. They may be done by the hospital pathologist with the legal permission of the coroner or medical examiner for that county/parish and do not require permission from the deceased's legal next of kin.
- Virtual Autopsy: This is when the autopsy is performed entirely by medical imaging, primarily CT and MRI[6]
While dissection of human remains for medical reasons has been practised irregularly for millennia, the modern autopsy process derives from the anatomists of the Renaissance. The two great nineteenth-century medical researchers Rudolf Virchow and Carl von Rokitansky built on the Renaissance legacy to derive the two distinct autopsy techniques that still bear their names. Their demonstration of correspondences between pathological conditions in dead bodies and symptoms and illnesses in the living opened the way for a different way of thinking about disease and its treatment. In China, the office of coroner and forensic autopsy have a history nearly two thousand years old.
Forensic autopsy
A forensic autopsy is used to determine the cause of death. Forensic science involves the application of the sciences to answer questions of interest to the legal system. In United States law, deaths are placed in one of five manners:
In some jurisdictions, the Undetermined category may include deaths in absentia, such as deaths at sea and missing persons declared dead in a court of law; in others, such deaths are classified under "Other".
Following an in-depth examination of all the evidence, a medical examiner or coroner will assign a manner of death as one of the five listed above; and detail the evidence on the mechanism of the death.
Clinical autopsy
Clinical autopsies serve two major purposes. They are performed to gain more insight into pathological processes and determine what factors contributed to a patient's death. More importantly, autopsies are performed to ensure the standard of care at hospitals. Autopsies can yield insight into how patient deaths can be prevented in the future.
Within the United Kingdom, clinical autopsies can only be carried out with the consent of the family of the deceased person as opposed to a medico-legal autopsy instructed by a Coroner (England & Wales) or Procurator Fiscal (Scotland) to which the family cannot object.
The process

The body is received at a medical examiner's office or hospital in a body bag or evidence sheet. A brand new body bag is used for each body to ensure that only evidence from that body is contained within the bag. Evidence sheets are an alternate way to transport the body. An evidence sheet is a sterile sheet that the body is covered in when it is moved. If it is believed there may be any significant residue on the hands, for instance gunpowder, a separate paper sack is put around each hand and taped shut around the wrist.
There are two parts to the physical examination of the body: the external and internal examination. Toxicology, biochemical tests and/or genetic testing often supplement these and frequently assist the pathologist in assigning the cause or causes of death.
External examination
The person responsible for handling, cleaning and moving the body is often called a diener, the German word for servant. In the UK this role is performed by an Anatomical Pathology Technologist who will also assist the pathologist in eviscerating the deceased and reconstruction after the autopsy. After the body is received, it is first photographed. The examiner then notes the kind of clothes and their position on the body before they are removed. Next, any evidence such as residue, flakes of paint or other material is collected from the external surfaces of the body. Ultraviolet light may also be used to search body surfaces for any evidence not easily visible to the naked eye. Samples of hair, nails and the like are taken, and the body may also be radiographically imaged.
Once the external evidence is collected, the body is removed from the bag, undressed and any wounds present are examined. The body is then cleaned, weighed and measured in preparation for the internal examination. The scale used to weigh the body is often designed to accommodate the cart that the body is transported on; its weight is then deducted from the total weight shown to give the weight of the body.
If not already within an autopsy room, the body is transported to one and placed on a table. A general description of the body as regards race, sex, age, hair color and length, eye color and other distinguishing features (birthmarks, old scar tissue, moles, etc) is then made. A handheld voice recorder or a standard examination form is normally used to record this information. In some countries e.g. France, Germany and Canada to name but a few, an autopsy may comprise an external examination only. This concept is sometimes termed a "view and grant". The principles behind this being that the medical records, history of the deceased and circumstances of death have all indicated as to the cause and manner of death without the need for an internal examination.
Internal examination
If not already in place, a plastic or rubber brick called a "body block" is placed under the back of the body, causing the arms and neck to fall backward whilst stretching and pushing the chest upward to make it easier to cut open. This gives the prosector, a pathologist or assistant, maximum exposure to the trunk. After this is done, the internal examination begins. The internal examination consists of inspecting the internal organs of the body for evidence of trauma or other indications of the cause of death. For the internal examination there are a number of different approaches available:
- a large and deep Y-shaped incision can be made from behind each ear and running down the sides of the neck, meeting at the breastbone. This is the approach most often used in forensic autopsies so as to allow maximum exposure of the neck structures for later detailed examination. This could prove essential in cases of suspected strangulation
- a T-shaped incision made from the tips of both shoulder, in a horizontal line across the region of the collar bones to meet at the sternum (breastbone) in the middle. This initial cut is used more often to produce a more aesthetic finish to the body when it is re-constituted as stitching marks will not be as apparent as with a Y-shaped incision
- a single vertical cut is made from the middle of the neck (in the region of the 'adam's apple' on a male body)
In all of the above cases the cut then extends all the way down to the pubic bone (making a deviation to the left side of the navel).
Bleeding from the cuts is minimal, or non-existent, due to the fact that the pull of gravity is producing the only blood pressure at this point, related directly to the complete lack of cardiac functionality. However, in certain cases there is anecdotal evidence to prove that bleeding can be quite profuse, especially in cases of drowning.
An electric saw dubbed a "Stryker saw" after a common manufacturer of the tool, is most often used to open the chest cavity. However, in some cases, due to the large amount of dust created when the bone is cut by the saw, shears are used to open the chest cavity. It is also possible to utilise a simple scalpel blade. The prosector uses the tool to saw through the ribs on the lateral sides of the chest cavity to allow the sternum and attached ribs to be lifted as one chest plate; this is done so that the heart and lungs can be seen in situ and that the heart, in particular the pericardial sac is not damaged or disturbed from opening. A scalpel is used to remove any soft tissue that is still attached to the posterior side of the chest plate. Now the lungs and the heart are exposed. The chest plate is set aside and will be eventually replaced at the end of the autopsy.
At this stage the organs are exposed. Usually, the organs are removed in a systematic fashion. Making a decision as to what order the organs are to be removed will depend highly on the case in question. Organs can be removed in several ways: The first is the en masse technique of letulle whereby all the organs are removed as one large mass. The second is the en bloc method of Ghon. The most popular in the UK is a modified version of this method which is divided into four groups of organs. Although these are the two predominant evisceration techniques in the UK variations on these are widespread.
One method is described here: The pericardial sac is opened to view the heart. Blood for chemical analysis may be removed from the inferior vena cava or the pulmonary veins. Before removing the heart, the pulmonary artery is opened in order to search for a blood clot. The heart can then be removed by cutting the inferior vena cava, the pulmonary veins, the aorta and pulmonary artery, and the superior vena cava. This method leaves the aortic arch intact, which will make things easier for the embalmer. The left lung is then easily accessible and can be removed by cutting the bronchus, artery, and vein at the hilum. The right lung can then be similarly removed. The abdominal organs can be removed one by one after first examining their relationships and vessels.
Some pathologists, however, prefer to remove the organs all in one "block". Then a series of cuts, along the vertebral column, are made so that the organs can be detached and pulled out in one piece for further inspection and sampling. During autopsies of infants, this method is used almost all of the time. The various organs are examined, weighed and tissue samples in the form of slices are taken. Even major blood vessels are cut open and inspected at this stage. Next the stomach and intestinal contents are examined and weighed. This could be useful to find the cause and time of death, due to the natural passage of food through the bowel during digestion. The more area empty, the longer the deceased had gone without a meal before death.
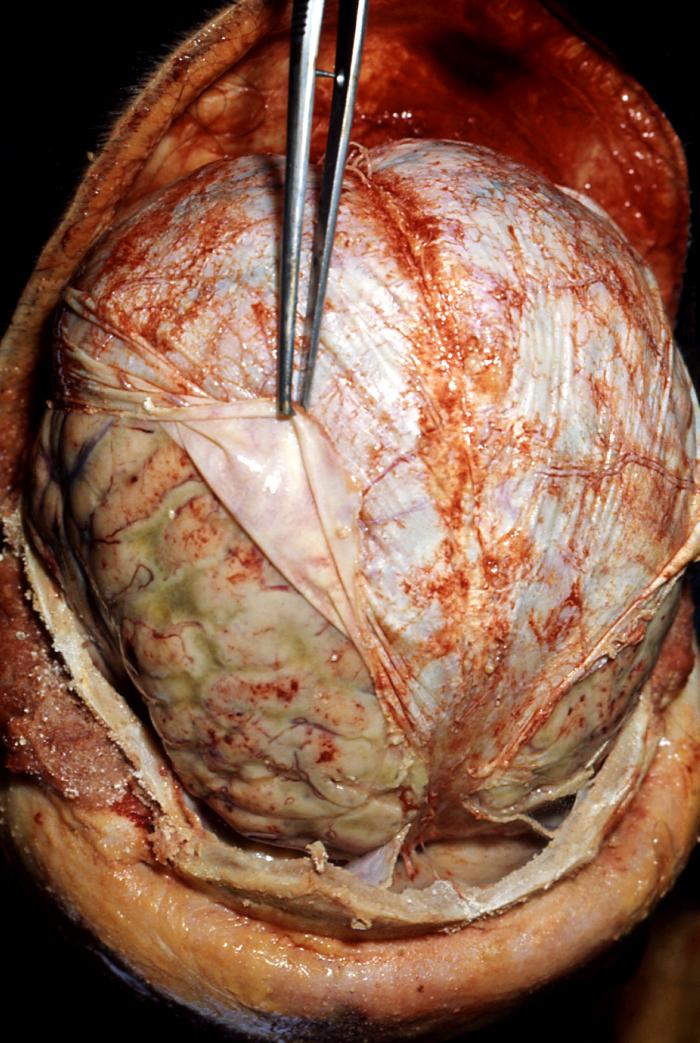
The body block that was used earlier to elevate the chest cavity is now used to elevate the head. To examine the brain, a cut is made from behind one ear, over the crown of the head, to a point behind the other ear. When the autopsy is completed, the incision can be neatly sewn up and is not noticed when the head is resting on a pillow in an open casket funeral. The scalp is pulled away from the skull in two flaps with the front flap going over the face and the rear flap over the back of the neck. The skull is then cut with an electric saw to create a "cap" that can be pulled off, exposing the brain. The brain is then observed in situ. Then the brain's connection to the spinal cord is severed, and the brain is then lifted out of the skull for further examination. If the brain needs to be preserved before being inspected, it is contained in a large container of formalin (15 percent solution of formaldehyde gas in buffered water) for at least two but preferably four weeks. This not only preserves the brain, but also makes it firmer allowing easier handling without corrupting the tissue.
Reconstitution of the body
An important component of the autopsy is the reconstitution of the body such that it can be viewed, if desired, by relatives of the deceased following the procedure. After the examination, the body has an open and empty chest cavity with chest flaps open on both sides, the top of the skull is missing, and the skull flaps are pulled over the face and neck. It is unusual to examine the face, arms, hands or legs internally. In the UK, following the Human Tissue Act 2004 all organs and tissue must be returned to the body unless permission is given by the family to retain any tissue for further investigation. Normally the internal body cavity is lined with cotton wool or an appropriate material, the organs are then placed into a plastic bag to prevent leakage and returned to the body cavity. The chest flaps are then closed and sewn back together and the skull cap is sewed back in place. Then the body may be wrapped in a shroud and it is common for relatives of the deceased to not be able to tell the procedure has been done when the deceased is viewed in a funeral parlor after embalming.
Other information
The principal aim of an autopsy is to determine the cause of death, the state of health of the person before he or she died, and whether any medical diagnosis and treatment before death was appropriate.
In most Western countries the number of autopsies performed in hospitals has been decreasing every year since 1955. Critics, including pathologist and former JAMA editor George Lundberg, have charged that the reduction in autopsies is negatively affecting the care delivered in hospitals, because when mistakes result in death, they are often not investigated and lessons learned.
When a person has given permission in advance of their death, autopsies may also be carried out for the purposes of teaching or medical research.
An autopsy is frequently performed in cases of sudden death, where a doctor is not able to write a death certificate, or when death is believed to be due to an unnatural cause. These examinations are performed under a legal authority (Medical Examiner or Coroner or Procurator Fiscal) and do not require the consent of relatives of the deceased. The most extreme example is the examination of murder victims, especially when medical examiners are looking for signs of death or the murder method, such as bullet wounds and exit points, signs of strangulation, or traces of poison.
See also
- Forensic science
- Disposal of human corpses
- Pathology
- John Tonge Centre
- Gunther von Hagens
References
- ↑ Ravakhah K (2006). "Death certificates are not reliable: revivification of the autopsy". South. Med. J. 99 (7): 728–33. PMID 16866055.
- ↑ Shojania KG, Burton EC, McDonald KM, Goldman L (2003). "Changes in rates of autopsy-detected diagnostic errors over time: a systematic review". JAMA. 289 (21): 2849–56. doi:10.1001/jama.289.21.2849. PMID 12783916.
- ↑ Roulson J, Benbow EW, Hasleton PS (2005). "Discrepancies between clinical and autopsy diagnosis and the value of post mortem histology; a meta-analysis and review". Histopathology. 47 (6): 551–9. doi:10.1111/j.1365-2559.2005.02243.x. PMID 16324191.
- ↑ Combes A, Mokhtari M, Couvelard A; et al. (2004). "Clinical and autopsy diagnoses in the intensive care unit: a prospective study". Arch. Intern. Med. 164 (4): 389–92. doi:10.1001/archinte.164.4.389. PMID 14980989.
- ↑ Papadakis MA, Mangione CM, Lee KK, Kristof M (1991). "Treatable abdominal pathologic conditions and unsuspected malignant neoplasms at autopsy in veterans who received mechanical ventilation". JAMA. 265 (7): 885–7. PMID 1992186.
- ↑ Heston T. Can we skip the autopsy?. Retrieved 24-Feb-2012.
External links
- Autopsy - Autopsy - Who gets autopsied?, Autopsy permission, Autopsy technique
- Autopsy - a detailed description by a pathologist complete with cartoon figures.
- The Virtual Autopsy - a site from the University of Leicester were one examines the patient, looks at the (medical) history and gets a try at the diagnosis.
- HBO's Autopsy - a series on HBO about forensics and autopsies.
- BBC News - Controversial Autopsy goes ahead - news story about Prof. Gunther von Hagens performing the first public autopsy in the UK in 170 years.
- How Stuff Works - Autopsies
- Autopsies - Forensic
- President Abraham Lincoln's Autopsy.
- www.autopsyvideo.com- This site offers autopsy documentaries, one produced with the aid of The LA County Coroner's Office.
- Autopsy of a Murder - An interactive exploration of a murder scene and the science involved in a criminalistic investigation: autopsy and laboratory expertise. Produced by the Montreal Science Centre for its namesake exhibition.
- Prevention of Infection during autopsy It lists the risk factors and prevention strategies during post mortem examination.
- [2] - The official organisation for Anatomical Pathology Technologists in the UK
Template:Pathology Template:Death
bs:Autopsija bg:Аутопсия de:Leichenschau cs:Pitva el:Νεκροψία eu:Autopsia gl:Autopsia id:Otopsi iu:ᑐᖁᖓᔪᒥᒃ ᖃᐅᔨᓴᕐᓂᖅ/tuqungajumik qaujisarniq it:Autopsia he:נתיחה שלאחר המוות nl:Autopsie no:Obduksjon sk:Pitva sr:Аутопсија fi:Ruumiinavaus sv:Obduktion yi:פאלמעסונג