Topiramate: Difference between revisions
No edit summary |
No edit summary |
||
| Line 136: | Line 136: | ||
| image = 200px-Topiramate2DACS.svg.png | | image = 200px-Topiramate2DACS.svg.png | ||
| width = 200 | | width = 200 | ||
| image2 = Topiramate3Dan.gif | | image2 = 180px-Topiramate3Dan.gif | ||
| width2 = 180 | | width2 = 180 | ||
Revision as of 23:18, 28 May 2014
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Pratik Bahekar, MBBS [2]
Disclaimer
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Topiramate is a Mood Stabilizer that is FDA approved for the {{{indicationType}}} of Lennox-Gastaut syndrome (adjunct), migraine (prophylaxis), partial seizure (initial monotherapy), partial seizure(adjunct), tonic-clonic seizure, primary generalized (adjunct), tonic-clonic seizure, primary generalized (initial monotherapy). Common adverse reactions include flushing, serum bicarbonate level abnormal, loss of appetite, weight decreased, infectious disease, confusion, dizziness, impaired cognition, impaired, psychomotor performance, memory impairment, paresthesia, reduced concentration span, somnolence, feeling nervous, mood disorder, fatigue, fever.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
- Lennox-Gastaut syndrome
- Start 25 to 50 mg/day PO, increase dosage by 25 to 50 mg/day at 1-week intervals to maintenance dose of 200 to 400 mg/day in 2 divided doses.
- Migraine prophylaxis
- 100 mg/day PO administered in 2 divided doses; 25 mg in the evening for 1 week, 25 mg twice daily for 1 week, 25 mg in the morning and 50 mg in the evening for 1 week, and then 50 mg twice daily.
- Partial seizure, initial monotherapy
- 25 mg PO twice daily; second week 50 mg PO twice daily, third week 75 mg PO twice daily, fourth week 100 mg PO twice daily, fifth week 150 mg PO twice daily, sixth week (MAX dose) 200 mg PO
- Partial seizure; adjunct
- 25 to 50 mg/day PO; may increase dosage by 25 to 50 mg/day at 1-week intervals to the usual maintenance dose of 200 to 400 mg/day in 2 divided doses.
- Tonic-clonic seizure, primary generalized (adjunct)
- 25 to 50 mg/day ORALLY; may increase dosage by 25 to 50 mg/day at 1-week intervals to the usual maintenance dose of 400 mg/day in 2 divided doses.
- Tonic-clonic seizure, primary generalized (initial monotherapy).
- 25 mg PO twice daily (morning and evening); second week, 50 mg PO twice daily; third week, 75 mg PO twice daily; fourth week, 100 mg PO twice daily; fifth week, 150 mg PO twice daily; sixth week (MAX dose), 200 mg PO twice daily
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information about Off-Label Guideline-Supported Use of Topiramate in adult patients.
Non–Guideline-Supported Use
- Alcoholism
- Diabetes mellitus type 2 in obese (adjunct)
- Eating disorder.
- Essential tremor
- Obesity
There is limited information about Off-Label Non–Guideline-Supported Use of Topiramate in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
- Lennox-Gastaut syndrome
- 2 years or older for opamax(R) and Qudexy(TM) XR,
- 6 years or older for Trokendi XR(TM)
- Migraine prophylaxis
- 12 years or older for Topamax(R) only
- Partial seizure, initial monotherapy
- 2 years or older for Qudexy XR (TM)
- 10 years or older for Trokendi XR(TM),
- Partial seizure; adjunct
- 2 years or older for Topamax(R) and Qudexy(TM) XR,
- 6 years or older Trokendi XR(TM)
- Tonic-clonic seizure, primary generalized (adjunct)
- 2 years or older for Topamax(R) and Qudexy(TM) XR
- 6 years or older for Trokendi XR(TM)
- Tonic-clonic seizure, primary generalized (initial monotherapy)
- 2 years or older for Topamax(R)
- 10 years or older for Trokendi XR(TM) and Qudexy(TM) XR
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information about Off-Label Guideline-Supported Use of Topiramate in pediatric patients.
Non–Guideline-Supported Use
There is limited information about Off-Label Non–Guideline-Supported Use of Topiramate in pediatric patients.
Contraindications
There is limited information regarding Topiramate Contraindications in the drug label.
Warnings
- Acute myopia and secondary angle closure glaucoma: Untreated elevated intraocular pressure can lead to permanent visual loss. Discontinue Topiramate if it occurs
- Visual field defects: These have been reported independent of elevated intraocular pressure. Consider discontinuation of Topiramate
- Oligohydrosis and hyperthermia: Monitor decreased sweating and increased body temperature, especially in pediatric patients
- Metabolic acidosis: Measure baseline and periodic measurement of serum bicarbonate. Consider dose reduction or discontinuation of Topiramate if clinically appropriate
- Suicidal behavior and ideation: Antiepileptic drugs increase the risk of suicidal behavior or ideation
- Cognitive/neuropsychiatric: Topiramate may cause cognitive dysfunction. Use caution when operating machinery including automobiles. Depression and mood problems may occur
- Fetal toxicity: Topiramate use during pregnancy can cause cleft lip and/or palate
- Withdrawal of AEDs: Withdrawal of Topiramate should be done gradually
- Hyperammonemia and encephalopathy: Patients with inborn errors of metabolism or reduced mitochondrial activity may have an increased risk of hyperammonemia. Measure ammonia if encephalopathic symptoms occur
- Kidney stones: Avoid use with other carbonic anhydrase inhibitors, other drugs causing metabolic acidosis, or in patients on a ketogenic diet
- Hypothermia: Reported with concomitant valproic acid use
Adverse Reactions
Clinical Trials Experience
- Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice. In the topiramate study, a dose of 200 mg/day was administered to a limited number of patients; therefore, these results cannot be directly compared to immediate-release topiramate experience.
- The safety data presented below are from 249 patients with partial epilepsy on concomitant AEDs who participated in the topiramate study.
- Table 8 displays the incidence of treatment-emergent adverse reactions that occurred in ≥2% of patients and numerically greater than placebo.

- In the controlled clinical study using topiramate, 8.9% of patients who received topiramate and 4.0% who received placebo discontinued as a result of treatment-emergent adverse reactions.
Postmarketing Experience
The following adverse reactions have been identified during post-approval use of topiramate. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. The listing is alphabetized:
- Bullous skin reactions, including erythema multiforme, Stevens-Johnson syndrome, toxic epidermal necrolysis,
- Hepatic failure (including fatalities),
- Hepatitis
- Maculopathy
- Pancreatitis
- Pemphigus
Drug Interactions
- Oral Contraceptives
- The possibility of decreased contraceptive efficacy and increased breakthrough bleeding should be considered in patients taking combination oral contraceptive products with topiramate. Patients taking estrogen-containing contraceptives should be asked to report any change in their bleeding patterns. Contraceptive efficacy can be decreased even in the absence of breakthrough bleeding.
- Antiepileptic Drugs
- Concomitant administration of phenytoin or carbamazepine with topiramate decreased plasma concentrations of topiramate
- Concomitant administration of valproic acid and topiramate has been associated with hyperammonemia with and without encephalopathy. Concomitant administration of topiramate with valproic acid has also been associated with hypothermia (with and without hyperammonemia) in patients who have tolerated either drug alone. It may be prudent to examine blood ammonia levels in patients in whom the onset of hypothermia has been reported.
- Numerous AEDs are substrates of the CYP enzyme system. In vitro studies indicate that topiramate does not inhibit enzyme activity for CYP1A2, CYP2A6, CYP2B6, CYP2C9, CYP2D6, CYP2E1, and CYP3A4/5 isozymes. In vitro studies indicate that immediate-release topiramate is a mild inhibitor of CYP2C19 and a mild inducer of CYP3A4. The same drug interactions can be expected with the use of topiramate.
- CNS Depressants and Alcohol
- Topiramate is a CNS depressant. Concomitant administration of topiramate with other CNS depressant drugs or alcohol can result in significant CNS depression. Concomitant use of alcohol should be avoided
- Other Carbonic Anhydrase Inhibitors
- Concomitant use of topiramate, a carbonic anhydrase inhibitor, with any other carbonic anhydrase inhibitor (e.g., zonisamide, acetazolamide or dichlorphenamide), may increase the severity of metabolic acidosis and may also increase the risk of kidney stone formation. Patients should be monitored for the appearance or worsening of metabolic acidosis when topiramate is given concomitantly with another carbonic anhydrase inhibitor
- Metformin
- Topiramate treatment can frequently cause metabolic acidosis, a condition for which the use of metformin is contraindicated. The concomitant use of topiramate and metformin is contraindicated in patients with metabolic acidosis
- Lithium
- In patients, there was an observed increase in systemic exposure of lithium following topiramate doses of up to 600 mg per day. Lithium levels should be monitored when co-administered with high-dose topiramate
Use in Specific Populations
Pregnancy
- Topiramate can cause fetal harm when administered to a pregnant woman. Data from pregnancy registries indicate that infants exposed to topiramate in utero have increased risk for cleft lip and/or cleft palate (oral clefts). When multiple species of pregnant animals received topiramate at clinically relevant doses, structural malformations, including craniofacial defects, and reduced fetal weights occurred in offspring. Topiramate should be used during pregnancy only if the potential benefit outweighs the potential risk. If this drug is used during pregnancy, or if the patient becomes pregnant while taking this drug, the patient should be informed of the potential hazard to the fetus.
- Pregnancy Registry
- Patients should be encouraged to enroll in the North American Antiepileptic Drug (NAAED) Pregnancy Registry if they become pregnant. This registry is collecting information about the safety of antiepileptic drugs during pregnancy. To enroll, patients can call the toll-free number 1-888-233-2334. Information about the North American Drug Pregnancy Registry can be found at http://www.massgeneral.org/aed/.
- Human Data
- Data from the NAAED Pregnancy Registry indicate an increased risk of oral clefts in infants exposed to topiramate monotherapy during the first trimester of pregnancy. The prevalence of oral clefts was 1.2% compared to a prevalence of 0.39% - 0.46% in infants exposed to other AEDs, and a prevalence of 0.12% in infants of mothers without epilepsy or treatment with other AEDs. For comparison, the Centers for Disease Control and Prevention (CDC) reviewed available data on oral clefts in the United States and found a similar background rate of 0.17%. The relative risk of oral clefts in topiramate-exposed pregnancies in the NAAED Pregnancy Registry was 9.6 (95% Confidence Interval=CI 3.6-25.7) as compared to the risk in a background population of untreated women. The UK Epilepsy and Pregnancy Register reported a similarly increased prevalence of oral clefts of 3.2% among infants exposed to topiramate monotherapy. The observed rate of oral clefts was 16 times higher than the background rate in the UK, which is approximately 0.2%.
- Topiramate treatment can cause metabolic acidosis [see Warnings and Precautions (5.4)]. The effect of topiramate-induced metabolic acidosis has not been studied in pregnancy; however, metabolic acidosis in pregnancy (due to other causes) can cause decreased fetal growth, decreased fetal oxygenation, and fetal death, and may affect the fetus' ability to tolerate labor. Pregnant patients should be monitored for metabolic acidosis and treated as in the nonpregnant state [see Warnings and Precautions (5.4)]. Newborns of mothers treated with topiramate should be monitored for metabolic acidosis because of transfer of topiramate to the fetus and possible occurrence of transient metabolic acidosis following birth.
- Animal Data
- Topiramate has demonstrated selective developmental toxicity, including teratogenicity, in multiple animal species at clinically relevant doses. When oral doses of 20 mg/kg, 100 mg/kg, or 500 mg/kg were administered to pregnant mice during the period of organogenesis, the incidence of fetal malformations (primarily craniofacial defects) was increased at all doses. The low dose is approximately 0.2 times the recommended human dose (RHD) 400 mg per day on a mg/m2 basis. Fetal body weights and skeletal ossification were reduced at 500 mg/kg in conjunction with decreased maternal body weight gain.
- In rat studies (oral doses of 20 mg/kg, 100 mg/kg, and 500 mg/kg or 0.2 mg/kg, 2.5 mg/kg, 30 mg/kg, and 400 mg/kg), the frequency of limb malformations (ectrodactyly, micromelia, and amelia) was increased among the offspring of dams treated with 400 mg/kg (10 times the RHD on a mg/m2 basis) or greater during the organogenesis period of pregnancy. Embryotoxicity (reduced fetal body weights, increased incidence of structural variations) was observed at doses as low as 20 mg/kg (0.5 times the RHD on a mg/m2 basis). Clinical signs of maternal toxicity were seen at 400 mg/kg and above, and maternal body weight gain was reduced during treatment with 100 mg/kg or greater.
- In rabbit studies (20 mg/kg, 60 mg/kg, and 180 mg/kg or 10 mg/kg, 35 mg/kg, and 120 mg/kg orally during organogenesis), embryo/fetal mortality was increased at 35 mg/kg (2 times the RHD on a mg/m2 basis) or greater, and teratogenic effects (primarily rib and vertebral malformations) were observed at 120 mg/kg (6 times the RHD on a mg/m2 basis). Evidence of maternal toxicity (decreased body weight gain, clinical signs, and/or mortality) was seen at 35 mg/kg and above.
- When female rats were treated during the latter part of gestation and throughout lactation (0.2 mg/kg, 4 mg/kg, 20 mg/kg, and 100 mg/kg or 2, 20, and 200 mg/kg), offspring exhibited decreased viability and delayed physical development at 200 mg/kg (5 times the RHD on a mg/m2 basis) and reductions in pre-and/or postweaning body weight gain at 2 mg/kg (0.05 times the RHD on a mg/m2 basis) and above. Maternal toxicity (decreased body weight gain, clinical signs) was evident at 100 mg/kg or greater.
- In a rat embryo/fetal development study with a postnatal component (0.2 mg/kg, 2.5 mg/kg, 30 mg/kg, or 400 mg/kg during organogenesis; noted above), pups exhibited delayed physical development at 400 mg/kg (10 times the RHD on a mg/m2 basis) and persistent reductions in body weight gain at 30 mg/kg (1 times the RHD on a mg/m2 basis) and higher.
- Women of Childbearing Potential
- Data from pregnancy registries indicate that infants exposed to topiramate in utero have an increased risk for cleft lip and/or cleft palate (oral clefts) Consider the benefits and risks of topiramate when prescribing this drug to women of childbearing potential, particularly when topiramate is considered for a condition not usually associated with permanent injury or death. Because of the risk of oral clefts to the fetus, which occur in the first trimester of pregnancy before many women know they are pregnant, all women of childbearing potential should be apprised of the potential hazard to the fetus from exposure to topiramate. If the decision is made to use topiramate, women who are not planning a pregnancy should use effective contraception . Women who are planning a pregnancy should be counseled regarding the relative risks and benefits of topiramate use during pregnancy, and alternative therapeutic options should be considered for these patients.
Pregnancy Category (AUS):
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Topiramate in women who are pregnant.
Labor and Delivery
Although the effect of topiramate on labor and delivery in humans has not been established, the development of topiramate-induced metabolic acidosis in the mother and/or in the fetus might affect the fetus' ability to tolerate labor
Nursing Mothers
Limited data on 5 breastfeeding infants exposed to topiramate showed infant plasma topiramate levels equal to 10-20% of the maternal plasma level. The effects of this exposure on infants are unknown. Caution should be exercised when topiramate is administered to a nursing woman.
Pediatric Use
- Seizures in Pediatric Patients 2 Years of Age and Older
- The safety and effectiveness of QUDEXY XR in pediatric patients is based on controlled trials with immediate-release topiramate
- The adverse reactions (both common and serious) in pediatric patients are similar to those seen in adults
- These include, but are not limited to:
- Oligohydrosis and hyperthermia
- Dose-related increased incidence of metabolic acidosis
- Dose-related increased incidence of hyperammonemia
- Adjunctive Treatment for Epilepsy with Partial Onset Seizures in Infants and Toddlers (1 to 24 months)
- The following pediatric use information is based on studies conducted with immediate-release topiramate.
- Safety and effectiveness in patients below the age of 2 years have not been established for the adjunctive therapy treatment of partial onset seizures, primary generalized tonic-clonic seizures, or seizures associated with Lennox-Gastaut syndrome. In a single randomized, double-blind, placebo-controlled investigational trial, the efficacy, safety, and tolerability of immediate-release topiramate oral liquid and sprinkle formulations as an adjunct to concurrent antiepileptic drug therapy in infants 1 to 24 months of age with refractory partial onset seizures, was assessed. After 20 days of double-blind treatment, immediate-release topiramate (at fixed doses of 5 mg/kg, 15 mg/kg, and 25 mg/kg per day) did not demonstrate efficacy compared with placebo in controlling seizures.
- In general, the adverse reaction profile in this population was similar to that of older pediatric patients, although results from the above controlled study, and an open-label, long-term extension study in these infants/toddlers (1 to 24 months old) suggested some adverse reactions not previously observed in older pediatric patients and adults; i.e., growth/length retardation, certain clinical laboratory abnormalities, and other adverse reactions that occurred with a greater frequency and/or greater severity than had been recognized previously from studies in older pediatric patients or adults for various indications.
- These very young pediatric patients appeared to experience an increased risk for infections (any topiramate dose 12%, placebo 0%) and of respiratory disorders (any topiramate dose 40%, placebo 16%). The following adverse reactions were observed in at least 3% of patients on immediate-release topiramate and were 3% to 7% more frequent than in patients on placebo: viral infection, bronchitis, pharyngitis, rhinitis, otitis media, upper respiratory infection, cough, and bronchospasm. A generally similar profile was observed in older children
- Immediate-release topiramate resulted in an increased incidence of patients with increased creatinine (any topiramate dose 5%, placebo 0%), BUN (any topiramate dose 3%, placebo 0%), and protein (any topiramate dose 34%, placebo 6%), and an increased incidence of decreased potassium (any topiramate dose 7%, placebo 0%). This increased frequency of abnormal values was not dose related. Creatinine was the only analyte showing a noteworthy increased incidence (topiramate 25 mg/kg/day 5%, placebo 0%) of a markedly abnormal increase. The significance of these findings is uncertain.
- Immediate-release topiramate treatment also produced a dose-related increase in the percentage of patients who had a shift from normal at baseline to high/increased (above the normal reference range) in total eosinophil count at the end of treatment. The incidence of these abnormal shifts was 6 % for placebo, 10% for 5 mg/kg/day, 9% for 15 mg/kg/day, 14% for 25 mg/kg/day, and 11% for any topiramate dose. There was a mean dose-related increase in alkaline phosphatase. The significance of these findings is uncertain.
- Treatment with immediate-release topiramate for up to 1 year was associated with reductions in Z SCORES for length, weight, and head circumference.
- In open-label, uncontrolled experience, increasing impairment of adaptive behavior was documented in behavioral testing over time in this population. There was a suggestion that this effect was dose-related. However, because of the absence of an appropriate control group, it is not known if this decrement in function was treatment related or reflects the patient's underlying disease (e.g., patients who received higher doses may have more severe underlying disease).
- In this open-label, uncontrolled study, the mortality was 37 deaths/1000 patient years. It is not possible to know whether this mortality rate is related to immediate-release topiramate treatment, because the background mortality rate for a similar, significantly refractory, young pediatric population (1 month to 24 months) with partial epilepsy is not known.
- Other Pediatric Studies
- Topiramate treatment produced a dose-related increased shift in serum creatinine from normal at baseline to an increased value at the end of 4 months treatment in adolescent patients (ages 12 years to 16 years) in a double-blind, placebo-controlled study.
- Juvenile Animal Studies
- When topiramate (30 mg/kg/day, 90 mg/kg/day or 300 mg/kg/day) was administered orally to rats during the juvenile period of development (postnatal days 12 to 50), bone growth plate thickness was reduced in males at the highest dose, which is approximately 5 to 8 times the maximum recommended pediatric dose (9 mg/kg/day) on a body surface area (mg/m2) basis.
Geriatic Use
Clinical studies of immediate-release topiramate did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently than younger subjects. Dosage adjustment is necessary for elderly with creatinine clearance less than 70 mL/min/1.73 m2. Estimate CrCl prior to dosing
Gender
Evaluation of effectiveness and safety of topiramate in clinical trials has shown no race- or gender-related effects.
Race
There is no FDA guidance on the use of Topiramate with respect to specific racial populations.
Renal Impairment
The clearance of topiramate was reduced by 42% in moderately renally impaired (creatinine clearance 30 to 69 mL/min/1.73m2) and by 54% in severely renally impaired subjects (creatinine clearance less than 30 mL/min/1.73m2) compared to normal renal function subjects (creatinine clearance greater than 70 mL/min/1.73m2). One-half the usual starting and maintenance dose is recommended in patients with moderate or severe renal impairment
Hepatic Impairment
There is no FDA guidance on the use of Topiramate in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Topiramate in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Topiramate in patients who are immunocompromised.
Patients Undergoing Hemodialysis
Topiramate is cleared by hemodialysis at a rate that is 4 to 6 times greater than a normal individual. Accordingly, a prolonged period of dialysis may cause topiramate concentration to fall below that required to maintain an anti-seizure effect. To avoid rapid drops in topiramate plasma concentration during hemodialysis, a supplemental dose of topiramate may be required. The actual adjustment should take into account the duration of dialysis period, the clearance rate of the dialysis system being used, and the effective renal clearance of topiramate in the patient being dialyzed
Administration and Monitoring
Administration
There is limited information regarding Topiramate Administration in the drug label.
Monitoring
There is limited information regarding Topiramate Monitoring in the drug label.
IV Compatibility
There is limited information regarding the compatibility of Topiramate and IV administrations.
Overdosage
- Overdoses of topiramate resulted in signs and symptoms which included convulsions, drowsiness, speech disturbance, blurred vision, diplopia, mentation impaired, lethargy, abnormal coordination, stupor, hypotension, abdominal pain, agitation, dizziness and depression. The clinical consequences were not severe in most cases, but deaths have been reported after polydrug overdoses involving topiramate.
- Topiramate overdose has resulted in severe metabolic acidosis.
- A patient who ingested a dose between 96 g and 110 g of topiramate was admitted to hospital with coma lasting 20 to 24 hours followed by full recovery after 3 to 4 days.
- Similar signs, symptoms, and clinical consequences are expected to occur with overdosage of topiramate. Therefore, in acute topiramate overdose, if the ingestion is recent, the stomach should be emptied immediately by lavage or by induction of emesis. Activated charcoal has been shown to adsorb topiramate in vitro. Treatment should be appropriately supportive. Hemodialysis is an effective means of removing topiramate from the body.
Pharmacology
| |
| |
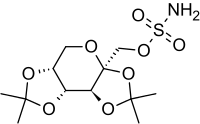
Topiramate
| |
| Systematic (IUPAC) name | |
| 2,3:4,5-Bis-O-(1-methylethylidene)-beta-D-fructopyranose sulfamate | |
| Identifiers | |
| CAS number | |
| ATC code | N03 |
| PubChem | |
| DrugBank | |
| Chemical data | |
| Formula | Template:OrganicBox atomTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox atomTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBoxTemplate:OrganicBox |
| Mol. mass | 339.363 g/mol |
| SMILES | & |
| Pharmacokinetic data | |
| Bioavailability | 80% |
| Protein binding | 13-17%; 15-41% |
| Metabolism | Hepatic (20-30%) |
| Half life | 19-25 hours |
| Excretion | Urine (70-80%) |
| Therapeutic considerations | |
| Licence data |
|
| Pregnancy cat. | |
| Legal status |
Prescription Only (S4)(AU) ?(CA) POM(UK) [[Prescription drug|Template:Unicode-only]](US) |
| Routes | Oral |
Mechanism of Action
There is limited information regarding Topiramate Mechanism of Action in the drug label.
Structure
- Topiramate, USP, is a sulfamate-substituted monosaccharide. topiramate (topiramate) extended-release capsules are available as 25 mg, 50 mg, 100 mg, 150 mg, and 200 mg capsules for oral administration as whole capsules or opened and sprinkled onto a spoonful of soft food.
- Topiramate is a white to off-white powder. Topiramate is freely soluble in polar organic solvents such as acetonitrile and acetone; and very slightly soluble to practically insoluble in non-polar organic solvents such as hexanes. Topiramate has the molecular formula C12H21NO8S and a molecular weight of 339.4. Topiramate is designated chemically as 2,3:4,5-Di-O-isopropylidene-β-D-fructopyranose sulfamate and has the following structural formula:

- Topiramate (topiramate) extended-release capsules contain beads of topiramate in a capsule. The inactive ingredients are microcrystalline cellulose, hypromellose 2910, ethylcellulose, diethyl phthalate.
- In addition, the capsule shells for all strengths contain hypromellose 2910, titanium dioxide, black iron oxide, red iron oxide and/or yellow iron oxide, black pharmaceutical ink, and white pharmaceutical ink (200 mg only).
Pharmacodynamics
There is limited information regarding Topiramate Pharmacodynamics in the drug label.
Pharmacokinetics
There is limited information regarding Topiramate Pharmacokinetics in the drug label.
Nonclinical Toxicology
- Carcinogenesis
- An increase in urinary bladder tumors was observed in mice given topiramate (20 mg/kg, 75 mg/kg, and 300 mg/kg) in the diet for 21 months. The elevated bladder tumor incidence, which was statistically significant in males and females receiving 300 mg/kg, was primarily due to the increased occurrence of a smooth muscle tumor considered histomorphologically unique to mice. Plasma exposures in mice receiving 300 mg/kg were approximately 0.5 to 1 times steady-state exposures measured in patients receiving topiramate monotherapy at the recommended human dose (RHD) of 400 mg, and 1.5 to 2 times steady-state topiramate exposures in patients receiving 400 mg of topiramate plus phenytoin. The relevance of this finding to human carcinogenic risk is uncertain.
- No evidence of carcinogenicity was seen in rats following oral administration of topiramate for 2 years at doses up to 120 mg/kg (approximately 3 times the RHD on a mg/m2 basis).
- Mutagenesis
- Topiramate did not demonstrate genotoxic potential when tested in a battery of in vitro and in vivo assays. Topiramate was not mutagenic in the Ames test or the in vitro mouse lymphoma assay; it did not increase unscheduled DNA synthesis in rat hepatocytes in vitro; and it did not increase chromosomal aberrations in human lymphocytes in vitro or in rat bone marrow in vivo.
- Impairment of Fertility
- No adverse effects on male or female fertility were observed in rats at doses up to 100 mg/kg (2.5 times the RHD on a mg/m2 basis).
Clinical Studies
- Extended-Release: Bridging Study to Demonstrate Pharmacokinetic Equivalence between Extended-Release (QUDEXY XR) and Immediate-Release Topiramate Formulations
- Although a controlled clinical trial was performed (Study 11), the basis for approval of the extended-release formulation (QUDEXY XR) included the studies described below using an immediate-release formulation [see Clinical Studies (14.2, 14.3, 14.4 and 14.5)] and the demonstration of the pharmacokinetic equivalence of QUDEXY XR to immediate-release topiramate through the analysis of concentrations and cumulative AUCs at multiple time points.
- Immediate-Release: Monotherapy Treatment in Patients with Partial Onset or Primary Generalized Tonic-Clonic Seizures
- Adults and Pediatric Patients 10 Years of Age and Older
- The effectiveness of topiramate as initial monotherapy in adults and children 10 years of age and older with partial onset or primary generalized tonic-clonic seizures was established in a multicenter, randomized, double-blind, dose-controlled, parallel-group trial (Study 1).
- Study 1 was conducted in 487 patients diagnosed with epilepsy (6 to 83 years of age) who had 1 or 2 well-documented seizures during the 3-month retrospective baseline phase who then entered the study and received topiramate 25 mg per day for 7 days in an open-label fashion. Forty-nine percent of subjects had no prior AED treatment and 17% had a diagnosis of epilepsy for greater than 24 months. Any AED therapy used for temporary or emergency purposes was discontinued prior to randomization. In the double-blind phase, 470 patients were randomized to titrate up to 50 mg per day or 400 mg per day of topiramate. If the target dose could not be achieved, patients were maintained on the maximum tolerated dose. Fifty eight percent of patients achieved the maximal dose of 400 mg per day for greater than 2 weeks, and patients who did not tolerate 150 mg per day were discontinued.
- The primary efficacy assessment was a between-group comparison of time to first seizure during the double-blind phase. Comparison of the Kaplan-Meier survival curves of time to first seizure favored the topiramate 400 mg per day group over the topiramate 50 mg per day group (p=0.0002, log rank test; Figure 1). The treatment effects with respect to time to first seizure were consistent across various patient subgroups defined by age, sex, geographic region, baseline body weight, baseline seizure type, time since diagnosis, and baseline AED use.
Figure 1: Kaplan-Meier Estimates of Cumulative Rates for Time to First Seizure in Study 1

Immediate-Release: Adjunctive Therapy in Patients with Partial Onset Seizures
- Adult Patients with Partial Onset Seizures
- The effectiveness of topiramate as an adjunctive treatment for adults with partial onset seizures was established in six multicenter, randomized, double-blind, placebo-controlled trials (Studies 2, 3, 4, 5, 6, and 7), two comparing several dosages of topiramate and placebo and four comparing a single dosage with placebo, in patients with a history of partial onset seizures, with or without secondarily generalized seizures.
- Patients in these studies were permitted a maximum of two antiepileptic drugs (AEDs) in addition to topiramate tablets or placebo. In each study, patients were stabilized on optimum dosages of their concomitant AEDs during baseline phase lasting between 4 and 12 weeks. Patients who experienced a prespecified minimum number of partial onset seizures, with or without secondary generalization, during the baseline phase (12 seizures for 12-week baseline, 8 for 8-week baseline or 3 for 4-week baseline) were randomly assigned to placebo or a specified dose of topiramate tablets in addition to their other AEDs.
- Following randomization, patients began the double-blind phase of treatment. In five of the six studies, patients received active drug beginning at 100 mg per day; the dose was then increased by 100 mg or 200 mg per day increments weekly or every other week until the assigned dose was reached, unless intolerance prevented increases. In Study 7, the 25 or 50 mg per day initial doses of topiramate were followed by respective weekly increments of 25 or 50 mg per day until the target dose of 200 mg per day was reached. After titration, patients entered a 4, 8 or 12-week stabilization period. The numbers of patients randomized to each dose, and the actual mean and median doses in the stabilization period are shown in Table 10.

- Pediatric Patients Ages 2 to 16 Years with Partial Onset Seizures
- The effectiveness of topiramate as an adjunctive treatment for pediatric patients ages 2 to 16 years with partial onset seizures was established in a multicenter, randomized, double-blind, placebo-controlled trial (Study 8), comparing topiramate and placebo in patients with a history of partial onset seizures, with or without secondarily generalized seizures.
- Patients in Study 8 were permitted a maximum of two antiepileptic drugs (AEDs) in addition to topiramate tablets or placebo. In Study 8, patients were stabilized on optimum dosages of their concomitant AEDs during an 8-week baseline phase. Patients who experienced at least six partial onset seizures, with or without secondarily generalized seizures, during the baseline phase were randomly assigned to placebo or topiramate in addition to their other AEDs.
- Following randomization, patients began the double-blind phase of treatment. Patients received active drug beginning at 25 or 50 mg per day; the dose was then increased by 25 mg to 150 mg per day increments every other week until the assigned dosage of 125, 175, 225 or 400 mg per day based on patients' weight to approximate a dosage of 6 mg/kg/day per day was reached, unless intolerance prevented increases. After titration, patients entered an 8-week stabilization period.
- Immediate-Release: Adjunctive Therapy in Patients With Primary Generalized Tonic-Clonic Seizures
- The effectiveness of topiramate as an adjunctive treatment for primary generalized tonic-clonic seizures in patients 2 years old and older was established in a multicenter, randomized, double-blind, placebo-controlled trial (Study 9), comparing a single dosage of topiramate and placebo.
- Patients in Study 9 were permitted a maximum of two antiepileptic drugs (AEDs) in addition to topiramate or placebo. Patients were stabilized on optimum dosages of their concomitant AEDs during an 8-week baseline phase. Patients who experienced at least three primary generalized tonic-clonic seizures during the baseline phase were randomly assigned to placebo or topiramate in addition to their other AEDs.
- Following randomization, patients began the double-blind phase of treatment. Patients received active drug beginning at 50 mg per day for four weeks; the dose was then increased by 50 mg to 150 mg per day increments every other week until the assigned dose of 175, 225 or 400 mg per day based on patients' body weight to approximate a dosage of 6 mg/kg/day was reached, unless intolerance prevented increases. After titration, patients entered a 12-week stabilization period.
- Immediate-Release: Adjunctive Therapy in Patients With Lennox-Gastaut Syndrome
- The effectiveness of topiramate as an adjunctive treatment for seizures associated with Lennox-Gastaut syndrome was established in a multicenter, randomized, double-blind, placebo-controlled trial comparing a single dosage of topiramate with placebo in patients 2 years of age and older (Study 10).
- Patients in Study 10 were permitted a maximum of two antiepileptic drugs (AEDs) in addition to topiramate or placebo. Patients who were experiencing at least 60 seizures per month before study entry were stabilized on optimum dosages of their concomitant AEDs during a 4 week baseline phase. Following baseline, patients were randomly assigned to placebo or topiramate in addition to their other AEDs. Active drug was titrated beginning at 1 mg/kg/day for a week; the dose was then increased to 3 mg/kg/day for one week then to 6 mg/kg/day. After titration, patients entered an 8-week stabilization period. The primary measures of effectiveness were the percent reduction in drop attacks and a parental global rating of seizure severity.
- In all adjunctive topiramate trials, the reduction in seizure rate from baseline during the entire double-blind phase was measured. The median percent reductions in seizure rates and the responder rates (fraction of patients with at least a 50% reduction) by treatment group for each study are shown below in Table 11. As described above, a global improvement in seizure severity was also assessed in the Lennox-Gastaut trial.

Subset analyses of the antiepileptic efficacy of topiramate tablets in these studies showed no differences as a function of gender, race, age, baseline seizure rate, or concomitant AED.
- In clinical trials for epilepsy, daily dosages were decreased in weekly intervals by 50 mg per day to 100 mg per day in adults and over a 2- to 8-week period in children; transition was permitted to a new antiepileptic regimen when clinically indicated.
- Extended-Release: Adjunctive Therapy in Adult Patients with Partial Onset Seizures with QUDEXY XR (Study 11)
- The effectiveness of QUDEXY XR as an adjunctive treatment for adults (18 to 75 years of age) was evaluated in Study 11, a randomized, international, multi-center, double-blind, parallel-group, placebo-controlled trial in patients with a history of partial onset seizures, with or without secondary generalization.
- Patients with partial onset seizures on a stable dose of 1 to 3 AEDs entered into an 8 week baseline period. Patients who experienced at least 8 partial onset seizures, with or without secondary generalization, and no more than 21 consecutive seizure free days during the 8 week baseline phase were randomly assigned to placebo or QUDEXY XR administered once daily in addition to their concomitant AEDs. Following randomization, 249 patients began the double-blind treatment phase, which consisted of an initial 3 week titration period :*Followed by an 8 week maintenance period. During the titration period, patients received QUDEXY XR or placebo beginning at 50 mg once daily; the dose was increased at weekly intervals by 50 mg once daily, or the placebo equivalent, until a final dose of 200 mg once daily was achieved. Patients than entered the maintenance period at the assigned dose of 200 mg once daily, or its placebo equivalent.
- The percent reduction in the frequency of partial-onset seizure, baseline period compared to the treatment phase, was the primary endpoint. Data was analyzed by the Wilcoxon rank-sum test, with the criteria of statistical significance of p<0.05. The results of the analysis are presented in Table 12. The median percent reduction in seizure rate was 39.5% in patients taking QUDEXY XR (N=124) and 21.7% in patients taking placebo (N=125). This difference was statistically significant.

- Figure 2 shows the change from baseline during titration plus maintenance (11 weeks) in partial-onset seizure frequency by category for patients treated with QUDEXY XR and placebo. Patients in whom the seizure frequency increased are shown as "worse." Patients in whom the seizure frequency decreased are shown in four categories of reduction in seizure frequency.

How Supplied
- 25 mg: light pink and grey capsules, printed with "UPSHER-SMITH" on the cap in black ink and "25 mg" on the body in black ink. 25 mg capsules are available in the following package configurations:
- Bottle of 30 count with desiccant (NDC 0245-1071-30)
- Bottle of 90 count with desiccant (NDC 0245-1071-90)
- Bottle of 500 count with desiccant (NDC 0245-1071-15)
- 50 mg: golden yellow and grey capsules, printed with "UPSHER-SMITH" on the cap in black ink and "50 mg" on the body in black ink. 50 mg capsules are available in the following package configurations:
- Bottle of 30 count with desiccant (NDC 0245-1072-30)
- Bottle of 90 count with desiccant (NDC 0245-1072-90)
- Bottle of 500 count with desiccant (NDC 0245-1072-15)
- 100 mg: reddish brown and grey capsules, printed with "UPSHER-SMITH" on the cap in black ink and "100 mg" on the body in black ink. 100 mg capsules are available in the following package configurations:
- Bottle of 30 count with desiccant (NDC 0245-1074-30)
- Bottle of 90 count with desiccant (NDC 0245-1074-90)
- Bottle of 500 count with desiccant (NDC 0245-1074-15)
- 150 mg: pale yellow and grey capsules, printed with "UPSHER-SMITH" on the cap in black ink and "150 mg" on the body in black ink. 150 mg capsules are available in the following package configurations:
- Bottle of 30 count with desiccant (NDC 0245-1075-30)
- Bottle of 90 count with desiccant (NDC 0245-1075-90)
- Bottle of 500 count with desiccant (NDC 0245-1075-15)
- 200 mg: brown and grey capsules, printed with "UPSHER-SMITH" on the cap in white ink and "200 mg" on the body in black ink. 200 mg capsules are available in the following package configurations:
- Bottle of 30 count with desiccant (NDC 0245-1073-30)
- Bottle of 90 count with desiccant (NDC 0245-1073-90)
- Bottle of 500 count with desiccant (NDC 0245-1073-15)
Storage
Topiramate extended-release capsules should be stored in a tightly-closed container at 20 to 25°C (68 to 77°F). Excursions permitted 15 to 30°C (59 to 86°F) [see USP Controlled Room Temperature]. Protect from moisture.
Images
Drug Images
{{#ask: Page Name::Topiramate |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Topiramate |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
Advise patients and caregivers to read the FDA-approved patient labeling (Medication Guide).
- Administration Instructions
- Instruct patients to take QUDEXY XR only as prescribed.
- Counsel patients to swallow QUDEXY XR capsules whole or carefully open and sprinkle the entire contents on a spoonful of soft food. This drug/food mixture should be swallowed immediately and not chewed. Do not store drug/food mixture for future use.
- Eye Disorders
- Advise patients taking QUDEXY XR to seek immediate medical attention if they experience blurred vision, visual disturbances or periorbital pain.
- Oligohydrosis and Hyperthermia
- Counsel patients, especially pediatric patients, that QUDEXY XR can cause decreased sweating and increased body temperature, especially in hot weather, and they should seek immediate medical attention if this is noticed
- Metabolic Acidosis
- Warn patients about the potentially significant risk for metabolic acidosis that may be asymptomatic and may be associated with adverse effects on kidneys (e.g., kidney stones, nephrocalcinosis), bones (e.g., osteoporosis, osteomalacia, and/or rickets in children), and growth (e.g., growth delay/retardation) in pediatric patients, and on the fetus.
- Suicidal Behavior and Ideation
- Counsel patients, their caregivers, and families that AEDs, including QUDEXY XR, may increase the risk of suicidal thoughts and behavior and they should be advised of the need to be alert for the emergence or worsening of the signs and symptoms of depression, any unusual changes in mood or behavior or the emergence of suicidal thoughts, behavior or thoughts about self-harm. Behaviors of concern should be reported immediately to healthcare providers.
- Interference with Cognitive and Motor Performance
- Warn patients about the potential for somnolence, dizziness, confusion, difficulty concentrating, visual effects and advise them not to drive or operate machinery until they have gained sufficient experience on QUDEXY XR to gauge whether it adversely affects their mental performance, motor performance, and/or vision.
- Advise patients that even when taking QUDEXY XR, or other anticonvulsants, some patients with epilepsy will continue to have unpredictable seizures. Therefore, counsel all patients taking QUDEXY XR for epilepsy to exercise appropriate caution when engaging in any activities where loss of consciousness could result in serious danger to themselves or those around them (including swimming, driving a car, climbing in high places, etc.). Some patients with refractory epilepsy will need to avoid such activities altogether. Physicians should discuss the appropriate level of caution with their patients, before patients with epilepsy engage in such activities.
- Fetal Toxicity
- Counsel pregnant women and women of childbearing potential that use of topiramate during pregnancy can cause fetal harm, including an increased risk for cleft lip and/or cleft palate (oral clefts), which occur early in pregnancy before many women know they are pregnant. There may also be risks to the fetus from chronic metabolic acidosis with use of QUDEXY XR during pregnancy.
- When appropriate, prescribers should counsel pregnant women and women of childbearing potential about alternative therapeutic options. This is particularly important when QUDEXY XR use is considered for a condition not usually associated with permanent injury or death. Advise women of childbearing potential who are not planning a pregnancy to use effective contraception while using topiramate, keeping in mind that there is a potential for decreased contraceptive efficacy when using estrogen-containing birth control with topiramate.
- Encourage pregnant women using topiramate to enroll in the North American Antiepileptic Drug (NAAED) Pregnancy Registry. The registry is collecting information about the safety of antiepileptic drugs during pregnancy. To enroll, patients can call the toll-free number, 1-888-233-2334. Information about the North American Drug Pregnancy Registry can be found at http://www.massgeneral.org/aed/
- Hyperammonemia and Encephalopathy
- Warn patients about the possible development of hyperammonemia with or without encephalopathy. Although hyperammonemia may be asymptomatic, clinical symptoms of hyperammonemic encephalopathy often include acute alterations in level of consciousness and/or cognitive function with lethargy or vomiting. This hyperammonemia and encephalopathy can develop with topiramate treatment alone or with topiramate treatment with concomitant valproic acid (VPA). Patients should be instructed to contact their physician if they develop unexplained lethargy, vomiting, or changes in mental status.
- Kidney Stones
- Instruct patients, particularly those with predisposing factors, to maintain an adequate fluid intake in order to minimize the risk of kidney stone formation.
- Hypothermia
- Counsel patients that QUDEXY XR can cause a reduction in body temperature, which can lead to alterations in mental status. If they note such changes, they should call their health care professional and measure their body temperature. Patients taking concomitant valproic acid should be specifically counseled on this potential adverse reaction.
- Paresthesia
- Counsel patients that they may experience tingling in the arms and legs. If this symptom occurs, they should consult with their physician.
Distributed by UPSHER-SMITH LABORATORIES, INC. Maple Grove, MN 55369 Revised: 3/2014 Qudexy is a trademark of Upsher-Smith Laboratories. MEDICATION GUIDE QUDEXY™ XR (cue-DEKS-ee ex-arr) (topiramate) Extended-Release Capsules Read this Medication Guide before you start taking QUDEXY XR and each time you get a refill. There may be new information. This information does not take the place of talking to your healthcare provider about your medical condition or treatment. If you have any questions about QUDEXY XR, talk to your healthcare provider or pharmacist.
- What is the most important information I should know about QUDEXY XR?
- QUDEXY XR may cause eye problems. Serious eye problems include:
- Any sudden decrease in vision with or without eye pain and redness,
- A blockage of fluid in the eye causing increased pressure in the eye (secondary angle closure glaucoma).
- These eye problems can lead to permanent loss of vision if not treated. You should call your healthcare provider right away if you have any new eye symptoms, including any new problems with your vision.
- QUDEXY XR may cause decreased sweating and increased body temperature (fever). People, especially children, should be watched for signs of decreased sweating and fever, especially in hot temperatures. Some people may need to be hospitalized for this condition. If a high fever, a fever that does not go away, or decreased sweating develops, call your healthcare provider right away.
- QUDEXY XR can increase the level of acid in your blood (metabolic acidosis). If left untreated, metabolic acidosis can cause brittle or soft bones (osteoporosis, osteomalacia, osteopenia), kidney stones, can slow the rate of growth in children, and may possibly harm your baby if you are pregnant. Metabolic acidosis can happen with or without symptoms. Sometimes people with metabolic acidosis will:
- Feel tired
- Not feel hungry (loss of appetite)
- Feel changes in heartbeat
- Have trouble thinking clearly
- Your healthcare provider should do a blood test to measure the level of acid in your blood before and during your treatment with QUDEXY XR.
- If you are pregnant, you should talk to your healthcare provider about whether you have metabolic acidosis.
- Like other antiepileptic drugs, QUDEXY XR may cause suicidal thoughts or actions in a very small number of people, about 1 in 500.
- Call a healthcare provider right away if you have any of these symptoms, especially if they are new, worse, or worry you:
- Thoughts about suicide or dying
- Attempts to commit suicide
- New or worse depression
- New or worse anxiety
- Feeling agitated or restless
- Panic attacks
- Trouble sleeping (insomnia)
- New or worse irritability
- Acting aggressive, being angry, or violent
- Acting on dangerous impulses
- An extreme increase in activity and talking (mania)
- Other unusual changes in behavior or mood
- Do not stop QUDEXY XR without first talking to a healthcare provider.
- Stopping QUDEXY XR suddenly can cause serious problems.
- Suicidal thoughts or actions can be caused by things other than medicines. If you have suicidal thoughts or actions, your healthcare provider may check for other causes.
- How can I watch for early symptoms of suicidal thoughts and actions?
- Pay attention to any changes, especially sudden changes, in mood, behaviors, thoughts, or feelings.
- Keep all follow-up visits with your healthcare provider as scheduled.
- Call your healthcare provider between visits as needed, especially if you are worried about symptoms.
- QUDEXY XR can harm your unborn baby.
- If you take QUDEXY XR during pregnancy, your baby has a higher risk for birth defects called cleft lip and cleft palate. :*These defects can begin early in pregnancy, even before you know you are pregnant.
- Cleft lip and cleft palate may happen even in children born to women who are not taking any medicines and do not have other risk factors.
- There may be other medicines to treat your condition that have a lower chance of birth defects.
- All women of childbearing age should talk to their healthcare providers about using other possible treatments instead of QUDEXY XR. If the decision is made to use QUDEXY XR, you should use effective birth control (contraception) unless you are planning to become pregnant. You should talk to your healthcare provider about the best kind of birth control to use while you are taking QUDEXY XR.
- Tell your healthcare provider right away if you become pregnant while taking QUDEXY XR. You and your healthcare provider should decide if you will continue to take QUDEXY XR while you are pregnant.
- Metabolic acidosis may have harmful effects on your baby. Talk to your healthcare provider if QUDEXY XR has caused metabolic acidosis during your pregnancy.
- Pregnancy Registry: If you become pregnant while taking QUDEXY XR, talk to your healthcare provider about registering with the North American Antiepileptic Drug Pregnancy Registry. You can enroll in this registry by calling 1-888-233-2334. The purpose of this registry is to collect information about the safety of QUDEXY XR and other antiepileptic drugs during pregnancy.
- What is QUDEXY XR?
- QUDEXY XR is a prescription medicine used:
- To treat certain types of seizures (partial onset seizures and primary generalized tonic-clonic seizures) in adults and children 10 years of age and older,
- With other medicines to treat certain types of seizures (partial onset seizures, primary generalized tonic-clonic seizures, and seizures associated with Lennox-Gastaut syndrome) in adults and children 2 years of age and older.
- Who should not take QUDEXY XR?
- Do not take QUDEXY XR if you have been told you have a problem with your blood called metabolic acidosis and are taking a medicine called metformin at the same time.
- What should I tell my healthcare provider before taking QUDEXY XR?
- Before taking QUDEXY XR, tell your healthcare provider about all of your medical conditions, including if you:
- Have or have had depression, mood problems or suicidal thoughts or behavior
- Have kidney problems, kidney stones or are getting kidney dialysis
- Have a history of metabolic acidosis (too much acid in the blood)
- Have liver problems
- Have weak, brittle or soft bones (osteomalacia, osteoporosis, osteopenia, or decreased bone density)
- Have lung or breathing problems
- Have eye problems, especially glaucoma
- Have diarrhea
- Have a growth problem
- Are on a diet high in fat and low in carbohydrates, which is called a ketogenic diet
- Are having surgery
- Are pregnant or plan to become pregnant
- Are breastfeeding. QUDEXY XR passes into your breast milk. It is not known if the QUDEXY XR that passes into breast milk can harm your baby. Talk to your healthcare provider about the best way to feed your baby if you take QUDEXY XR.
- Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. QUDEXY XR and other medicines may affect each other causing side effects.
- Especially tell your healthcare provider if you take:
- Metformin (such as GLUCOPHAGE®)
- Valproic acid (such as DEPAKENE® or DEPAKOTE®)
- Any medicines that impair or decrease your thinking, concentration, or muscle coordination
- Birth control pills. QUDEXY XR may make your birth control pills less effective. Tell your healthcare provider if your menstrual bleeding changes while you are taking birth control pills and QUDEXY XR.
- Medicines used to prevent seizures
- Any other carbonic anhydrase inhibitors like QUDEXY XR (such as zonisamide, acetazolamide, or dichlorphenamide).
- Ask your healthcare provider if you are not sure if your medicine is listed above.
- Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist each time you get a new medicine. Do not start a new medicine without talking with your healthcare provider.
- How should I take QUDEXY XR?
- Take QUDEXY XR exactly as your healthcare provider tells you to.
- Your healthcare provider may change your dose. Do not change your dose without talking to your healthcare provider.
- QUDEXY XR capsules may be swallowed whole or, if you cannot swallow the capsule whole, you may carefully open the :*QUDEXY XR capsule and sprinkle the medicine on a spoonful of soft food like applesauce.
- Swallow the food and medicine mixture right away. Do not store the food and medicine mixture to use later.
- Drink fluids right after eating the food and medicine mixture to make sure it is all swallowed.
- Do not crush or chew the food and medicine mixture before swallowing.
- Do not crush or chew QUDEXY XR capsules before swallowing.
- QUDEXY XR can be taken before, during, or after a meal. Drink plenty of fluids during the day. This may help prevent kidney stones while taking QUDEXY XR.
- If you take too much QUDEXY XR, call your healthcare provider or poison control center right away or go to the nearest emergency room.
- If you miss a single dose of QUDEXY XR, take it as soon as you can. Do not double your dose. If you have missed more than one dose, you should call your healthcare provider for advice.
- Do not stop taking QUDEXY XR without talking to your healthcare provider. Stopping QUDEXY XR suddenly may cause serious problems. If you have epilepsy and you stop taking QUDEXY XR suddenly, you may have seizures that do not stop. Your healthcare provider will tell you how to stop taking QUDEXY XR slowly.
- Your healthcare provider may do blood tests while you take QUDEXY XR.
- What should I avoid while taking QUDEXY XR?
- Do not drink alcohol while taking QUDEXY XR. QUDEXY XR and alcohol can cause serious side effects such as severe sleepiness and dizziness and an increase in seizures.
:*Do not drive a car or operate heavy machinery until you know how QUDEXY XR affects you. QUDEXY XR can slow your thinking and motor skills, and may affect vision.
- What are the possible side effects of QUDEXY XR?
- QUDEXY XR may cause serious side effects including:
- See "What is the most important information I should know about QUDEXY XR?"
- High blood ammonia levels. High ammonia in the blood can affect your mental activities, slow your alertness, make you feel tired, or cause vomiting. This has happened when QUDEXY XR is taken with a medicine called valproic acid (DEPAKENE® and DEPAKOTE®).
- Kidney stones. Drink plenty of fluids when taking QUDEXY XR to decrease your chances of getting kidney stones.
- Low body temperature. Taking QUDEXY XR when you are also taking valproic acid cause a drop in body temperature to less than 95ºF, feeling tired, confusion, or coma.
- Effects on thinking and alertness. QUDEXY XR may affect how you think, and cause confusion, problems with concentration, attention, memory, or speech. QUDEXY XR may cause depression or mood problems, tiredness, and sleepiness.
- Dizziness or loss of muscle coordination.
- Call your healthcare provider right away if you have any of the symptoms above. The most common side effects of QUDEXY XR include:
- Tingling of the arms and legs (paresthesia)
- Irregular movement of eyes (nystagmus)
- Not feeling hungry
- Nausea or indigestion
- A change in the way foods taste
- Diarrhea
- Weight loss
- Nervousness
- 8Upper respiratory tract infection
- Tell your healthcare provider about any side effect that bothers you or that does not go away.
- These are not all the possible side effects of QUDEXY XR. For more information, ask your healthcare provider or pharmacist.
- Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
- You may also report side effects to UPSHER-SMITH LABORATORIES, INC. at 1-855-899-9180.
- How should I store QUDEXY XR?
- Store QUDEXY XR capsules at room temperature between 68°F to 77°F (20°C to 25°C).
- Keep QUDEXY XR in a tightly closed container.
- Keep QUDEXY XR dry and away from moisture.
- Keep QUDEXY XR and all medicines out of the reach of children.
- General information about the safe and effective use of QUDEXY XR:
- Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use QUDEXY XR for a condition for which it was not prescribed. Do not give QUDEXY XR to other people, even if they have the same symptoms that you have. It may harm them.
- This Medication Guide summarizes the most important information about QUDEXY XR. If you would like more information, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about QUDEXY XR that is written for health professionals.
- For more information, go to www.upsher-smith.com or call UPSHER-SMITH LABORATORIES, INC. at 1-888-650-3789.
What are the ingredients in QUDEXY XR?
- Active ingredient: topiramate
- Inactive ingredients: microcrystalline cellulose, hypromellose 2910, ethylcellulose, diethyl phthalate, titanium dioxide, black iron oxide, red iron oxide and/or yellow iron oxide, black pharmaceutical ink, and white pharmaceutical ink (200 mg only).
- This Medication Guide has been approved by the U.S. Food and Drug Administration.
Distributed by UPSHER-SMITH LABORATORIES, INC. Maple Grove, MN 55369 Issued: 3/2014 Qudexy is a trademark of Upsher-Smith Laboratories. All other marks are owned by their respective owners.
Precautions with Alcohol
Alcohol-Topiramate interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
There is limited information regarding Topiramate Brand Names in the drug label.
Look-Alike Drug Names
There is limited information regarding Topiramate Look-Alike Drug Names in the drug label.
Drug Shortage Status
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
{{#subobject:
|Label Page=Topiramate |Label Name=Topi16.PNG
}}
{{#subobject:
|Label Page=Topiramate |Label Name=Topi17.PNG
}}
{{#subobject:
|Label Page=Topiramate |Label Name=Topi18.PNG
}}
{{#subobject:
|Label Page=Topiramate |Label Name=Topi19.PNG
}}
{{#subobject:
|Label Page=Topiramate |Label Name=Topi20.PNG
}}