Mitral stenosis resident survival guide: Difference between revisions
No edit summary |
|||
| Line 85: | Line 85: | ||
::❑ R/S ratio in V1 = 1.0 or more | ::❑ R/S ratio in V1 = 1.0 or more | ||
::❑ S/R ratio in V6 = 1.0 or more | ::❑ S/R ratio in V6 = 1.0 or more | ||
::❑ Incomplete [[RBBB]] pattern | ::❑ Incomplete [[RBBB]] pattern | ||
::❑ ST T strain pattern in 2,3,aVF | ::❑ ST T strain pattern in leads 2,3,aVF | ||
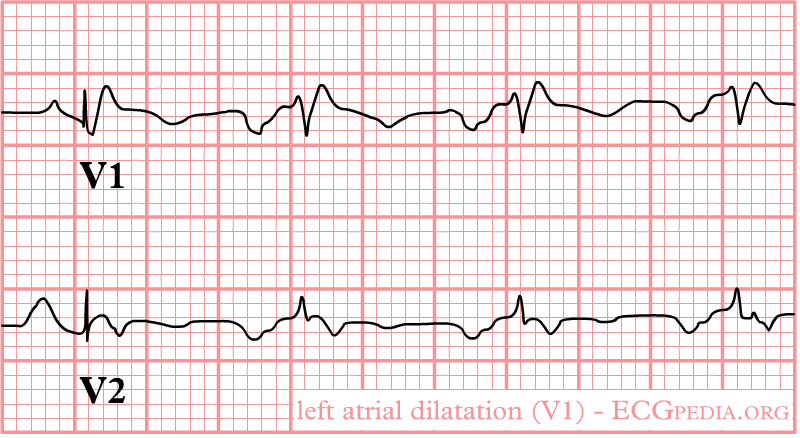
::❑ [[P pulmonale]] or [[ | ::❑ [[P pulmonale]] or [[right atrial enlargement]] or P congenitale | ||
::❑ R wave progression reversal | ::❑ R wave progression reversal | ||
::❑ Inverted [[T wave]] in the anterior precordial leads | ::❑ Inverted [[T wave]] in the anterior precordial leads | ||
Revision as of 14:34, 28 March 2014
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Twinkle Singh, M.B.B.S. [2]; Mohamed Moubarak, M.D. [3]
Synonyms and keywords: Mitral valve stenosis; narrowing of mitral valve
Overview
Mitral stenosis refers to abnormal narrowing of mitral orifice, which leads to obstruction of blood flow from left atrium to left ventricle. The most common presentations of mitral stenosis are dyspnea, orthopnea, paroxysmal nocturnal dyspnea, and peripheral edema. Mitral stenosis has a characteristic low-pitched, rumbling diastolic murmur, heard best at the apex during physical examination. The definitive therapy for mitral stenosis include percutaneous balloon valvotomy, surgical mitral valve repair, or mitral valve replacement.
Causes
Life Threatening Causes
Life-threatening causes include conditions which may result in death or permanent disability within 24 hours if left untreated.
Common Causes
Diagnosis
Shown below is an algorithm summarizing the approach to the initial evluation of mitral stenosis according to 2014 AHA/ACC guidelines for management of valvular heart disease.[2].
Abbreviations: AF: atrial fibrillation; PMBC: percutaneous mitral ballon commissurotomy; TR: tricuspid regurgitation; S1: First heart sound; P2: Pulmonary component of second heart sound; EKG: Electrocardiogram; TTE: Transthoracic echocardiography; MS: mitral stenosis
Characterize the symptoms: ❑ History of rheumatic fever | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Examine the patient:
Head:
Neck: Chest:
{{#ev:youtube|HW2pk1icYdM|250}} | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Order tests:
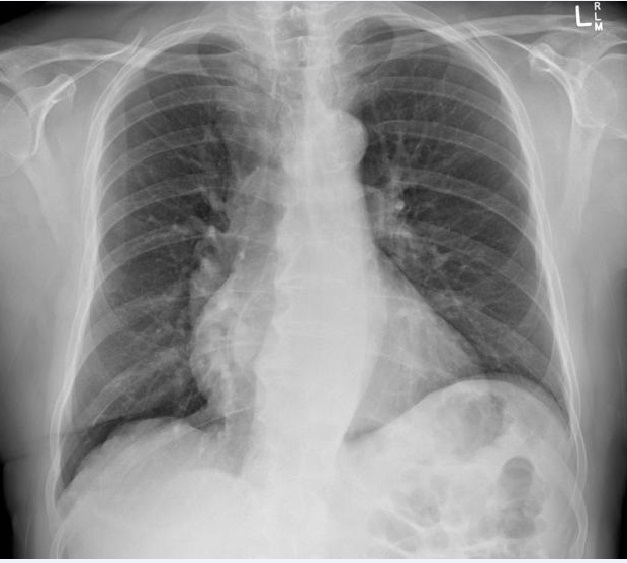
❑ Perform chest X-ray
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Consider alternative diagnosis: ❑ Myxoma
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Treatment
The filling of the left ventricle depends upon the diastole time which is limited by mitral stenosis. Therefore, slowing the heart rate is crucial in the initial management of mitral stenosis in order to improve the diastole time and consequently improve the filling of the left ventricle.
Medical therapy ❑ Consider heart rate control in MS patients with:
❑ Consider anticoagulation therapy in MS patients with:
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Shown below is an algorithm summarizing the approach to management of rheumatic mitral stenosis according to 2014 AHA/ACC guidelines for management of valvular heart disease.[2]
MVA: Mitral valve area; PMBC: Percutaneous mitral ballon commissurotomy; PCWP: Pulmonary capillary wedge pressure; ms: milliseconds; NYHA: New York Heart Association; AF: Atrial fibrillation
| ❑ Assess the presence of symptoms | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Symptomatic | Asymptomatic | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ❑ Assess the severity of mitral stenosis | ❑ Assess the severity of mitral stenosis | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Progressive ❑ MVA > 1.5 cm2 Pressure half time < 150 ms | Progressive ❑ MVA > 1.5 cm2 Pressure half time < 150 ms | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
❑ Assess if valve morphology is favorable for PMBC | ❑ Perform exercise testing | ❑ Assess if valve morphology is favorable for PMBC | ❑ Assess if the new onset AF is present | ❑ Monitor patient periodically | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Yes | No | ❑ Assess PCWP on exercise | Yes | No | No | Yes | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
❑ Proceed with PMBC | If patient is severely symptomatic (NYHA III/IV): ❑ Assess the surgical risk of patient | ❑ Proceed with PMBC | ❑ Monitor patient periodically | ❑ Assess if the valve morphology is favorable for PMBC | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Yes | No | Yes | No | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ❑ Proceed with PMBC | ❑ Proceed with mitral valve surgery | ❑ Proceed with PMBC | ❑ Monitor patient periodically | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Rheumatic Fever Prophylaxis
Shown below is the table depicting the secondary prophylaxis of rheumatic fever according to the 2014 AHA/ACC guideline for the management of valvular heart disease:[3]
| ||||||||||
| Indications | Duration of prophylaxis |
| ▸ Rheumatic fever with carditis and persistent valvular heart disease | ▸ 10 years or until the patient is 40 years (whichever is longer) |
| ▸ Rheumatic fever with carditis but no valvular heart disease | ▸ 10 years or until the patient is 21 years (whichever is longer) |
| ▸ Rheumatic fever without carditis | ▸ 5 years or until the patient is 21 years (whichever is longer) |
Do's
- Perform transesophageal echocardiography (TEE) in patients considered for PMBC to rule out left atrial thrombus and to determine mitral regurgitation severity.
- Perform exercise testing or invasive hemodynamic testing, when clinical signs and symptoms don't co-relate with echocardiographic findings.
- Perform mitral valve surgery in stage C and stage D mitral stenosis, if patient is undergoing cardiac surgery for some other indication.
- Perform mitral valve surgery in moderate mitral stenosis (mitral valve area: 1.6 - 2 cm2) if the patient is undergoing cardiac surgery for other indications.
- Perform mitral valve surgery with excision of left atrial appendage in stage C and stage D mitral stenosis patients who have had recurrent embolic events despite being on anticoagulation therapy.
- Perform TTE every 3-5 years in asymptomatic stage B MS patients and every 1-2 years in asymptomatic stage C MS patients who have mitral valve area 1-1.5 cm2 .
- Perform TTE once every year in asymptomatic stage C MS patients who have mitral valve area < 1 cm2.
- In cases of senile calcific mitral stenosis, intervention is done only when symptoms are severe and cannot be controlled with heart rate control and diuretics.
References
- ↑ Tadele, H.; Mekonnen, W.; Tefera, E. (2013). "Rheumatic mitral stenosis in Children: more accelerated course in sub-Saharan Patients". BMC Cardiovasc Disord. 13 (1): 95. doi:10.1186/1471-2261-13-95. PMID 24180350. Unknown parameter
|month=ignored (help) - ↑ 2.0 2.1 Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP, Guyton RA; et al. (2014). "2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines". Circulation. doi:10.1161/CIR.0000000000000029. PMID 24589852.
- ↑ Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP, Guyton RA; et al. (2014). "2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines". Circulation. doi:10.1161/CIR.0000000000000031. PMID 24589853.