Hepatomegaly: Difference between revisions
| Line 133: | Line 133: | ||
{| style="border: 0px; font-size: 90%; margin: 3px;" align="center" | {| style="border: 0px; font-size: 90%; margin: 3px;" align="center" | ||
! rowspan="3" | | ! rowspan="3" |Organ system | ||
! rowspan="3" style="background:#4479BA; color: #FFFFFF;" align="center" |Disease | ! rowspan="3" style="background:#4479BA; color: #FFFFFF;" align="center" |Disease | ||
| colspan="7" rowspan="1" style="background:#4479BA; color: #FFFFFF;" align="center" |'''Clinical manifestations''' | | colspan="7" rowspan="1" style="background:#4479BA; color: #FFFFFF;" align="center" |'''Clinical manifestations''' | ||
| Line 216: | Line 216: | ||
* The risk of [[cholangiocarcinoma]] in patients with primary sclerosing cholangitis is 400 times higher than the risk in the general population. | * The risk of [[cholangiocarcinoma]] in patients with primary sclerosing cholangitis is 400 times higher than the risk in the general population. | ||
|- | |- | ||
|'''Systemic disease''' | | rowspan="2" |'''Systemic disease''' | ||
| style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Whipple's disease]] | | style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Whipple's disease]] | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="center" |Diffuse | | style="padding: 5px 5px; background: #F5F5F5;" align="center" |Diffuse | ||
| Line 243: | Line 243: | ||
* [[Arthritis]] | * [[Arthritis]] | ||
* [[Ascites]] | * [[Ascites]] | ||
|- | |||
|[[Hemochromatosis]] | |||
|RUQ | |||
|− | |||
|− | |||
|− | |||
|− | |||
|− | |||
|− | |||
| | |||
* >60% TS | |||
* >240 μg/L SF | |||
* Raised LFT <br>Hyperglycemia | |||
| | |||
* Ultrasound shows evidence of cirrhosis | |||
|Extra intestinal findings: | |||
* Hyperpigmentation | |||
* Diabetes mellitus | |||
* Arthralgia | |||
* Impotence in males | |||
* Cardiomyopathy | |||
* Atherosclerosis | |||
* Hypopituitarism | |||
* Hypothyroidism | |||
* Extrahepatic cancer | |||
* Prone to specific infections | |||
|- | |- | ||
! rowspan="3" |Hematologic causes | ! rowspan="3" |Hematologic causes | ||
| Line 305: | Line 331: | ||
! style="background:#4479BA; color: #FFFFFF;" align="center" |Comments | ! style="background:#4479BA; color: #FFFFFF;" align="center" |Comments | ||
|- | |- | ||
! | ! rowspan="2" |Cardiac causes | ||
| style="padding: 5px 5px; background: #DCDCDC;" align="center" | | | style="padding: 5px 5px; background: #DCDCDC;" align="center" |Heart failure | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="center" |Diffuse/ RLQ/LLQ | | style="padding: 5px 5px; background: #F5F5F5;" align="center" |Diffuse/ RLQ/LLQ | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="center" | − | | style="padding: 5px 5px; background: #F5F5F5;" align="center" | − | ||
| Line 316: | Line 342: | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="left" | | | style="padding: 5px 5px; background: #F5F5F5;" align="left" | | ||
* CBC | * CBC | ||
* | * Increased BNP and Pro BNP | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="left" | | | style="padding: 5px 5px; background: #F5F5F5;" align="left" | | ||
* | * Echocardiography | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="left" | | | style="padding: 5px 5px; background: #F5F5F5;" align="left" | | ||
* | * Exertional dyspnea | ||
* Chest pain | |||
* Edema | |||
|- | |- | ||
! style="padding: 5px 5px; background: #DCDCDC;" align="center" |Hepatic causes | !Constrictive pericarditis | ||
|Diffuse/ RLQ/LLQ | |||
|− | |||
|− | |||
|− | |||
|<nowiki>+</nowiki> | |||
|± | |||
|− | |||
!- | |||
| | |||
* Echocardiography | |||
| | |||
* Exertional dyspnea | |||
* Chest pain | |||
* Edema | |||
|- | |||
! rowspan="4" style="padding: 5px 5px; background: #DCDCDC;" align="center" |Hepatic causes | |||
| style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Hepatitis|Viral hepatitis]] | | style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Hepatitis|Viral hepatitis]] | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="center" |[[RUQ]] | | style="padding: 5px 5px; background: #F5F5F5;" align="center" |[[RUQ]] | ||
| Line 343: | Line 384: | ||
* Hep B and C transmits via blood transfusion and sexual contact. | * Hep B and C transmits via blood transfusion and sexual contact. | ||
|- | |- | ||
| style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Liver abscess]] | | style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Liver abscess]] | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="center" |RUQ | | style="padding: 5px 5px; background: #F5F5F5;" align="center" |RUQ | ||
| Line 361: | Line 401: | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="left" | | | style="padding: 5px 5px; background: #F5F5F5;" align="left" | | ||
|- | |- | ||
| style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Hepatocellular carcinoma]]/[[Metastasis]] | | style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Hepatocellular carcinoma]]/[[Metastasis]] | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="center" |RUQ | | style="padding: 5px 5px; background: #F5F5F5;" align="center" |RUQ | ||
| Line 385: | Line 424: | ||
* [[Asterixis]] | * [[Asterixis]] | ||
|- | |- | ||
| style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Budd-Chiari syndrome|Budd-Chiari syndrome]] | | style="padding: 5px 5px; background: #DCDCDC;" align="center" |[[Budd-Chiari syndrome|Budd-Chiari syndrome]] | ||
| style="padding: 5px 5px; background: #F5F5F5;" align="center" |[[RUQ]] | | style="padding: 5px 5px; background: #F5F5F5;" align="center" |[[RUQ]] | ||
| Line 417: | Line 441: | ||
*[[Total protein]] more than 2.5 g per deciliter | *[[Total protein]] more than 2.5 g per deciliter | ||
*[[White blood cells]] are usually less than 500/μL. | *[[White blood cells]] are usually less than 500/μL. | ||
|- | |- | ||
|} | |} | ||
==References== | ==References== | ||
Revision as of 21:20, 7 February 2018
| Hepatomegaly | |
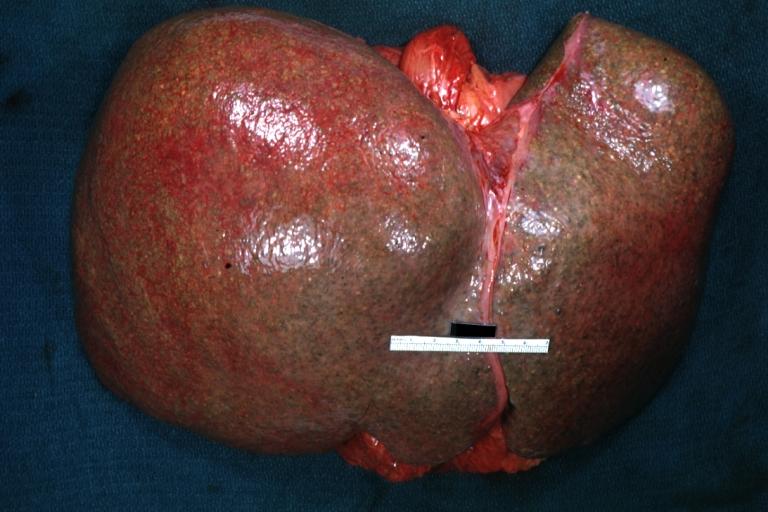 |
|---|
For patient information on this topic, click here.
|
Hepatomegaly Microchapters |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor-In-Chief: Iqra Qamar M.D.[2] Cafer Zorkun, M.D., Ph.D. [3]
Synonyms and keywords: Enlarged liver; liver enlargement
Overview
The liver is an organ present in vertebrates and some other animals. The adult human liver normally weighs between 1.4 - 1.6 kilograms (3.1 - 3.5 pounds), and it is a soft, pinkish-brown "boomerang shaped" organ. It is located on the right side of the upper abdomen below the diaphragm. The liver size increases with age and it ranges between 5 cm to 15 cm in adulthood. A normal liver is less than 16 cm in ultrasound evaluation. Hepatomegaly may be found in physical examination or during imaging studies. Imaging is more accurate in determining liver size.[1][2] In some certain conditions normal liver may be palpated as enlarged liver including thin people, during deep inspiration, right pleural effusion, and when emphysema results in hyperinflation of the chest with diaphragmatic descent and downward displacement of the liver. Common pathologic causes that may result in hepatomegaly are hepatitis, storage disorders, impaired venous outflow, infiltrative disorders, and biliary obstruction.
Causes
Causes of hepatomegaly may be classified on the basis of etiology into hepatitis, storage disorders, impaired venous outflow, infiltrative and obstructive causes.[3][4][5][6][7][8][9][10][11][12][13][14]
| Etiology | Disease | |
|---|---|---|
| Hepatitis | Infections | Acute and chronic viral hepatitis |
| Bacterial liver abscess | ||
| Parasitic infections | ||
| Granulomatous hepatitis | ||
| Ischemia | Ischemic hepatitis ("shock liver") | |
| Toxins | Alcoholic hepatitis | |
| Steatosis | Alcoholic fatty liver disease | |
| Nonalcoholic steatohepatitis | ||
| Drugs/Medications | Drug induced liver injury (DILI) | |
| Immune mediated hepatitis | Autoimmune hepatitis | |
| Copper deposition | Wilson disease | |
| Storage disorders | Glycogen | Glycogen storage disorders |
| Diabetes mellitus | ||
| Lipid | Gaucher disease | |
| Nonalcoholic steatohepatitis | ||
| Protein | Alpha-1 antitrypsin deficiency | |
| Iron | Hemochromatosis | |
| Impaired venous outflow | Cardiac | Right heart failure |
| Constrictive pericarditis | ||
| Hepatic vein | Hepatic vein thrombosis | |
| Inferior vena cava web | ||
| Intrahepatic | Sinusoidal obstruction syndrome | |
| Peliosis hepatis | ||
| Infiltrative diseases | Benign primary liver tumors | Hemangiomas |
| Adenomas | ||
| Focal nodular hyperplasia | ||
| Malignant primary liver tumors | Hepatocellular carcinoma | |
| Cholangiocarcinoma | ||
| Fibrolamellar carcinoma | ||
| Hemangioendothelioma | ||
| Metastatic/disseminated tumors | Myeloma | |
| Lymphoma | ||
| Leukemia | ||
| Metastatic solid tumors | ||
| Biliary obstruction | Primary biliary cirrhosis | |
| Primary sclerosing cholangitis | ||
| Biliary atresia | ||
| Other | Anatomic variations | Riedel's lobe |
| Cystic liver disease | Polycystic liver disease | |
| Caroli's disease | ||
Differential diagnosis
Patients with hepatomegaly need to be differentiated from other patients presenting with similar complaints such as abdominal pain.[3][4][5][6][7][8][9][10][11][12][13][14]
Abbreviations: RUQ= Right upper quadrant of the abdomen, LUQ= Left upper quadrant, LLQ= Left lower quadrant, RLQ= Right lower quadrant, LFT= Liver function test, SIRS= Systemic inflammatory response syndrome, ERCP= Endoscopic retrograde cholangiopancreatography, IV= Intravenous, N= Normal, AMA= Anti mitochondrial antibodies, LDH= Lactate dehydrogenase, GI= Gastrointestinal, CXR= Chest X ray, IgA= Immunoglobulin A, IgG= Immunoglobulin G, IgM= Immunoglobulin M, CT= Computed tomography, PMN= Polymorphonuclear cells, ESR= Erythrocyte sedimentation rate, CRP= C-reactive protein, TS= Transferrin saturation, SF= Serum Ferritin, SMA= Superior mesenteric artery, SMV= Superior mesenteric vein, ECG= Electrocardiogram, US = Ultrasound
| Organ system | Disease | Clinical manifestations | Diagnosis | Comments | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Symptoms | Signs | ||||||||||
| Abdominal Pain | Fever | Nausea or vomiting | Jaundice | Weight loss | Hypo-
tension |
Rebound Tenderness | Lab Findings | Imaging | |||
| Pancreato-biliary disorders | Pancreatic carcinoma | Epigastric | − | + | + | + | − | − |
Skin manifestations may include: | ||
| Primary biliary cirrhosis | RUQ/Epigastric | − | − | + | − | − | − |
|
|
| |
| Primary sclerosing cholangitis | RUQ | + | − | + | − | − | − |
|
ERCP and MRCP shows
|
| |
| Systemic disease | Whipple's disease | Diffuse | ± | − | ± | + | ± | − | Endoscopy is used to confirm diagnosis.
Images used to find complications |
Extra intestinal findings: | |
| Hemochromatosis | RUQ | − | − | − | − | − | − |
|
|
Extra intestinal findings:
| |
| Hematologic causes | Myeloma | Diffuse | ± | − | − | + | ± | − |
|
− |
|
| Lymphoma | Diffuse | + | − | − | + | ± | − |
|
− | ||
| Leukemia | Diffuse | + | ± | − | + | ± | − |
|
− | ||
| Disease | Abdominal Pain | Fever | Nausea or vomiting | Jaundice | Weight loss | Hypo-
tension |
Rebound Tenderness | Lab Findings | Imaging | Comments | |
| Cardiac causes | Heart failure | Diffuse/ RLQ/LLQ | − | − | − | + | ± | − |
|
|
|
| Constrictive pericarditis | Diffuse/ RLQ/LLQ | − | − | − | + | ± | − | - |
|
| |
| Hepatic causes | Viral hepatitis | RUQ | + | + | + | + | Positive in fulminant hepatitis | + |
|
|
|
| Liver abscess | RUQ | + | + | + | + | + | ± |
|
|
||
| Hepatocellular carcinoma/Metastasis | RUQ | + | − | + | + | − | − |
|
|
Other symptoms: | |
| Budd-Chiari syndrome | RUQ | ± | − | ± | − | − | − |
|
CT scan findings:
|
Ascitic fluid examination shows:
| |
References
- ↑ Sapira JD, Williamson DL (1979). "How big is the normal liver?". Arch Intern Med. 139 (9): 971–3. PMID 475535.
- ↑ Niederau C, Sonnenberg A, Müller JE, Erckenbrecht JF, Scholten T, Fritsch WP (1983). "Sonographic measurements of the normal liver, spleen, pancreas, and portal vein". Radiology. 149 (2): 537–40. doi:10.1148/radiology.149.2.6622701. PMID 6622701.
- ↑ 3.0 3.1 Wolf AD, Lavine JE (2000). "Hepatomegaly in neonates and children". Pediatr Rev. 21 (9): 303–10. PMID 10970452.
- ↑ 4.0 4.1 Chau TN, Lai ST, Tse C, Ng TK, Leung VK, Lim W, Ng MH (2006). "Epidemiology and clinical features of sporadic hepatitis E as compared with hepatitis A". Am. J. Gastroenterol. 101 (2): 292–6. doi:10.1111/j.1572-0241.2006.00416.x. PMID 16454833.
- ↑ 5.0 5.1 Bernstein DL, Hülkova H, Bialer MG, Desnick RJ (2013). "Cholesteryl ester storage disease: review of the findings in 135 reported patients with an underdiagnosed disease". J. Hepatol. 58 (6): 1230–43. doi:10.1016/j.jhep.2013.02.014. PMID 23485521.
- ↑ 6.0 6.1 Torbenson M, Chen YY, Brunt E, Cummings OW, Gottfried M, Jakate S, Liu YC, Yeh MM, Ferrell L (2006). "Glycogenic hepatopathy: an underrecognized hepatic complication of diabetes mellitus". Am. J. Surg. Pathol. 30 (4): 508–13. PMID 16625098.
- ↑ 7.0 7.1 Chatila R, West AB (1996). "Hepatomegaly and abnormal liver tests due to glycogenosis in adults with diabetes". Medicine (Baltimore). 75 (6): 327–33. PMID 8982149.
- ↑ 8.0 8.1 Mukewar S, Sharma A, Lackore KA, Enders FT, Torbenson MS, Kamath PS, Roberts LR, Kudva YC (2017). "Clinical, Biochemical, and Histopathology Features of Patients With Glycogenic Hepatopathy". Clin. Gastroenterol. Hepatol. 15 (6): 927–933. doi:10.1016/j.cgh.2016.11.038. PMID 28043933.
- ↑ 9.0 9.1 Charrow J, Andersson HC, Kaplan P, Kolodny EH, Mistry P, Pastores G, Rosenbloom BE, Scott CR, Wappner RS, Weinreb NJ, Zimran A (2000). "The Gaucher registry: demographics and disease characteristics of 1698 patients with Gaucher disease". Arch. Intern. Med. 160 (18): 2835–43. PMID 11025794.
- ↑ 10.0 10.1 Drebber U, Kasper HU, Ratering J, Wedemeyer I, Schirmacher P, Dienes HP, Odenthal M (2008). "Hepatic granulomas: histological and molecular pathological approach to differential diagnosis--a study of 442 cases". Liver Int. 28 (6): 828–34. doi:10.1111/j.1478-3231.2008.01695.x. PMID 18312287.
- ↑ 11.0 11.1 Park MA, Mueller PS, Kyle RA, Larson DR, Plevak MF, Gertz MA (2003). "Primary (AL) hepatic amyloidosis: clinical features and natural history in 98 patients". Medicine (Baltimore). 82 (5): 291–8. doi:10.1097/01.md.0000091183.93122.c7. PMID 14530778.
- ↑ 12.0 12.1 Cooke CB, Krenacs L, Stetler-Stevenson M, Greiner TC, Raffeld M, Kingma DW, Abruzzo L, Frantz C, Kaviani M, Jaffe ES (1996). "Hepatosplenic T-cell lymphoma: a distinct clinicopathologic entity of cytotoxic gamma delta T-cell origin". Blood. 88 (11): 4265–74. PMID 8943863.
- ↑ 13.0 13.1 Long RG, Scheuer PJ, Sherlock S (1977). "Presentation and course of asymptomatic primary biliary cirrhosis". Gastroenterology. 72 (6): 1204–7. PMID 870368.
- ↑ 14.0 14.1 "EASL Clinical Practice Guidelines: management of cholestatic liver diseases". J. Hepatol. 51 (2): 237–67. 2009. doi:10.1016/j.jhep.2009.04.009. PMID 19501929.