Valacyclovir
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Vignesh Ponnusamy, M.B.B.S. [2]
Disclaimer
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Valacyclovir is a nucleoside analogue DNA polymerase inhibitor that is FDA approved for the treatment of cold sores (herpes labialis), genital herpes, and herpes zoster. Common adverse reactions include headache, nausea, and abdominal pain.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Cold Sores (Herpes Labialis)
- The recommended dosage of valacyclovir hydrochloride for treatment of cold sores is 2 grams twice daily for 1 day taken 12 hours apart. Therapy should be initiated at the earliest symptom of a cold sore (e.g., tingling, itching, or burning).
Genital Herpes
- Initial Episode: The recommended dosage of valacyclovir hydrochloride for treatment of initial genital herpes is 1 gram twice daily for 10 days. Therapy was most effective when administered within 48 hours of the onset of signs and symptoms.
- Recurrent Episodes: The recommended dosage of valacyclovir hydrochloride for treatment of recurrent genital herpes is 500 mg twice daily for 3 days. Initiate treatment at the first sign or symptom of an episode.
- Suppressive Therapy: The recommended dosage of valacyclovir hydrochloride for chronic suppressive therapy of recurrent genital herpes is 1 gram once daily in patients with normal immune function. In patients with a history of 9 or fewer recurrences per year, an alternative dose is 500 mg once daily.
- In HIV-infected patients with a CD4+ cell count ≥100 cells/mm3, the recommended dosage of valacyclovir hydrochloride for chronic suppressive therapy of recurrent genital herpes is 500 mg twice daily.
- Reduction of Transmission: The recommended dosage of valacyclovir hydrochloride for reduction of transmission of genital herpes in patients with a history of 9 or fewer recurrences per year is 500 mg once daily for the source partner.
Herpes Zoster
- The recommended dosage of valacyclovir hydrochloride for treatment of herpes zoster is 1 gram 3 times daily for 7 days. Therapy should be initiated at the earliest sign or symptom of herpes zoster and is most effective when started within 48 hours of the onset of rash.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Valacyclovir in adult patients.
Non–Guideline-Supported Use
Acute retinal necrosis
- Oral valacyclovir 1 g 3 times a day.[1]
Cytomegalovirus infection; Prophylaxis - Transplantation
- Prophylaxis with valacyclovir 2000 mg orally 4 times daily for 18 weeks after bone marrow transplantation.
Genital herpes simplex, Initial and recurrent episodes - HIV infection
- Valacyclovir for 5 to 14 days.[2]
Herpes labialis - HIV infection
- Oral valacyclovir for 5 to 10 days.[2]
Herpes simplex, Non-genital
- 14-day course of valacyclovir 500 mg orally twice daily.
Herpes zoster, Shingles - HIV infection
- 7-day oral regimen of valacyclovir 1 g 3 times daily.[3]
HIV infection - Varicella
- Valacyclovir is a recommended option for uncomplicated chickenpox in adults with HIV.[2]
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
Cold Sores (Herpes Labialis)
- The recommended dosage of valacyclovir hydrochloride for the treatment of cold sores in pediatric patients ≥12 years of age is 2 grams twice daily for 1 day taken 12 hours apart. Therapy should be initiated at the earliest symptom of a cold sore (e.g., tingling, itching, or burning).
Chickenpox
- The recommended dosage of valacyclovir hydrochloride for treatment of chickenpox in immunocompetent pediatric patients 2 to <18 years of age is 20 mg/kg administered 3 times daily for 5 days. The total dose should not exceed 1 gram 3 times daily. Therapy should be initiated at the earliest sign or symptom.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Valacyclovir in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Valacyclovir in pediatric patients.
Contraindications
- Valacyclovir hydrochloride is contraindicated in patients who have had a demonstrated clinically significant hypersensitivity reaction (e.g., anaphylaxis) to valacyclovir, acyclovir, or any component of the formulation.
Warnings
Precautions
- TTP/HUS, in some cases resulting in death, has occurred in patients with advanced HIV disease and also in allogeneic bone marrow transplant and renal transplant recipients participating in clinical trials of Valacyclovir hydrochloride at doses of 8 grams per day. Treatment with Valacyclovir hydrochloride should be stopped immediately if clinical signs, symptoms, and laboratory abnormalities consistent with TTP/HUS occur.
- Acute Renal Failure
- Cases of acute renal failure have been reported in:
- Elderly patients with or without reduced renal function. Caution should be exercised when administering valacyclovir hydrochloride to geriatric patients, and dosage reduction is recommended for those with impaired renal function.
- Patients with underlying renal disease who received higher than recommended doses of valacyclovir hydrochloride for their level of renal function. Dosage reduction is recommended when administering valacyclovir hydrochloride to patients with renal impairment.
- Patients receiving other nephrotoxic drugs. Caution should be exercised when administering valacyclovir hydrochloride to patients receiving potentially nephrotoxic drugs.
- Patients without adequate hydration. Precipitation of acyclovir in renal tubules may occur when the solubility (2.5 mg/mL) is exceeded in the intratubular fluid. Adequate hydration should be maintained for all patients.
- Cases of acute renal failure have been reported in:
- In the event of acute renal failure and anuria, the patient may benefit from hemodialysis until renal function is restored.
- Central Nervous System Effects
- Central nervous system adverse reactions, including agitation, hallucinations, confusion, delirium, seizures, and encephalopathy, have been reported in both adult and pediatric patients with or without reduced renal function and in patients with underlying renal disease who received higher than recommended doses of valacyclovir hydrochloride for their level of renal function. Elderly patients are more likely to have central nervous system adverse reactions. Valacyclovir hydrochloride should be discontinued if central nervous system adverse reactions occur.
Adverse Reactions
Clinical Trials Experience
- Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared with rates in the clinical trials of another drug and may not reflect the rates observed in practice.
- Cold Sores (Herpes Labialis): In clinical studies for the treatment of cold sores, the adverse reactions reported by patients receiving valacyclovir hydrochloride 2 grams twice daily (n = 609) or placebo (n = 609) for 1 day, respectively, included headache (14%, 10%) and dizziness (2%, 1%). The frequencies of abnormal ALT (>2 x ULN) were 1.8% for patients receiving valacyclovir hydrochloride compared with 0.8% for placebo. Other laboratory abnormalities (hemoglobin, white blood cells, alkaline phosphatase, and serum creatinine) occurred with similar frequencies in the 2 groups.
- Genital Herpes: Initial Episode: In a clinical study for the treatment of initial episodes of genital herpes, the adverse reactions reported by ≥5% of patients receiving valacyclovir hydrochloride 1 gram twice daily for 10 days (n = 318) or oral acyclovir 200 mg 5 times daily for 10 days (n = 318), respectively, included headache (13%, 10%) and nausea (6%, 6%). For the incidence of laboratory abnormalities see Table 2.
- Recurrent Episodes: In 3 clinical studies for the episodic treatment of recurrent genital herpes, the adverse reactions reported by ≥5% of patients receiving valacyclovir hydrochloride 500 mg twice daily for 3 days (n = 402), valacyclovir hydrochloride 500 mg twice daily for 5 days (n = 1,136) or placebo (n = 259), respectively, included headache (16%, 11%, 14%) and nausea (5%, 4%, 5%).
- For the incidence of laboratory abnormalities see Table 2.
- Suppressive Therapy: Suppression of Recurrent Genital Herpes in Immunocompetent Adults: In a clinical study for the suppression of recurrent genital herpes infections, the adverse reactions reported by patients receiving valacyclovir hydrochloride 1 gram once daily (n = 269), valacyclovir hydrochloride 500 mg once daily (n = 266), or placebo (n = 134), respectively, included headache (35%, 38%, 34%), nausea (11%, 11%, 8%), abdominal pain (11%, 9%, 6%), dysmenorrhea (8%, 5%, 4%), depression (7%, 5%, 5%), arthralgia (6%, 5%, 4%), vomiting (3%, 3%, 2%), and dizziness (4%, 2%, 1%). For the incidence of laboratory abnormalities see Table 2.
- Suppression of Recurrent Genital Herpes in HIV-Infected Patients: In HIV-infected patients, frequently reported adverse reactions for valacyclovir hydrochloride (500 mg twice daily; n = 194, median days on therapy = 172) and placebo (n = 99, median days on therapy = 59), respectively, included headache (13%, 8%), fatigue (8%, 5%), and rash (8%, 1%). Post-randomization laboratory abnormalities that were reported more frequently in valacyclovir subjects versus placebo included elevated alkaline phosphatase (4%, 2%), elevated ALT (14%, 10%), elevated AST (16%, 11%), decreased neutrophil counts (18%, 10%), and decreased platelet counts (3%, 0%), respectively.
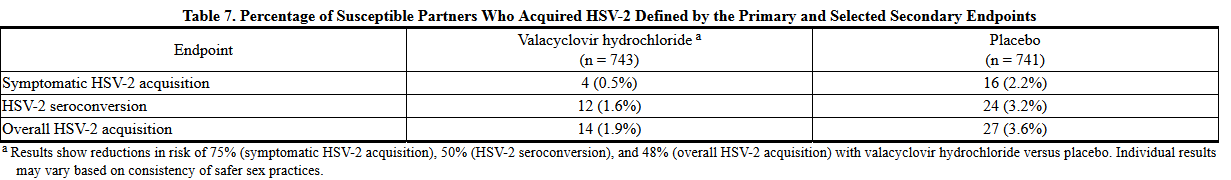
- Reduction of Transmission: In a clinical study for the reduction of transmission of genital herpes, the adverse reactions reported by patients receiving valacyclovir hydrochloride 500 mg once daily (n = 743) or placebo once daily (n = 741), respectively, included headache (29%, 26%), nasopharyngitis (16%, 15%), and upper respiratory tract infection (9%, 10%).
- Herpes Zoster: In 2 clinical studies for the treatment of herpes zoster, the adverse reactions reported by patients receiving valacyclovir hydrochloride 1 gram 3 times daily for 7 to 14 days (n = 967) or placebo (n = 195), respectively, included nausea (15%, 8%), headache (14%, 12%), vomiting (6%, 3%), dizziness (3%, 2%), and abdominal pain (3%, 2%). For the incidence of laboratory abnormalities see Table 2.
Clinical Trials Experience in Pediatric Patients
- The safety profile of valacyclovir hydrochloride has been studied in 177 pediatric patients 1 month to <18 years of age. Sixty-five of these pediatric patients, 12 to <18 years of age, received oral tablets for 1 to 2 days for treatment of cold sores. The remaining 112 pediatric patients, 1 month to <12 years of age, participated in 3 pharmacokinetic and safety studies and received valacyclovir oral suspension. Fifty-one of these 112 pediatric patients received oral suspension for 3 to 6 days. The frequency, intensity, and nature of clinical adverse reactions and laboratory abnormalities were similar to those seen in adults.
- Pediatric Patients 12 to <18 Years of Age (Cold Sores): In clinical studies for the treatment of cold sores, the adverse reactions reported by adolescent patients receiving valacyclovir hydrochloride 2 grams twice daily for 1 day, or valacyclovir hydrochloride 2 grams twice daily for 1 day followed by 1 gram twice daily for 1 day (n = 65, across both dosing groups), or placebo (n = 30), respectively, included headache (17%, 3%) and nausea (8%, 0%).
- Pediatric Patients 1 Month to <12 Years of Age: Adverse events reported in more than 1 subject across the 3 pharmacokinetic and safety studies in children 1 month to <12 years of age were diarrhea (5%), pyrexia (4%), dehydration (2%), herpes simplex (2%), and rhinorrhea (2%). No clinically meaningful changes in laboratory values were observed.
Postmarketing Experience
- In addition to adverse events reported from clinical trials, the following events have been identified during postmarketing use of valacyclovir hydrochloride. Because they are reported voluntarily from a population of unknown size, estimates of frequency cannot be made. These events have been chosen for inclusion due to a combination of their seriousness, frequency of reporting, or potential causal connection to valacyclovir hydrochloride.
General
Facial edema, hypertension, tachycardia.
Allergic
Acute hypersensitivity reactions including anaphylaxis, angioedema, dyspnea, pruritus, rash, and urticaria.
CNS Symptoms
Aggressive behavior; agitation; ataxia; coma; confusion; decreased consciousness; dysarthria; encephalopathy; mania; and psychosis, including auditory and visual hallucinations, seizures, tremors.
Eye
Visual abnormalities.
Gastrointestinal
Hepatobiliary Tract and Pancreas
Liver enzyme abnormalities, hepatitis.
Renal
Renal failure, renal pain (may be associated with renal failure).
Hematologic
Thrombocytopenia, aplastic anemia, leukocytoclastic vasculitis, TTP/HUS.
Skin
Erythema multiforme, rashes including photosensitivity, alopecia.
Drug Interactions
- No clinically significant drug-drug or drug-food interactions with valacyclovir hydrochloride are known.
Use in Specific Populations
Pregnancy
- Pregnancy Category B
- There are no adequate and well-controlled studies of valacyclovir hydrochloride or acyclovir in pregnant women. Based on prospective pregnancy registry data on 749 pregnancies, the overall rate of birth defects in infants exposed to acyclovir in-utero appears similar to the rate for infants in the general population. valacyclovir hydrochloride should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
- A prospective epidemiologic registry of acyclovir use during pregnancy was established in 1984 and completed in April 1999. There were 749 pregnancies followed in women exposed to systemic acyclovir during the first trimester of pregnancy resulting in 756 outcomes. The occurrence rate of birth defects approximates that found in the general population. However, the small size of the registry is insufficient to evaluate the risk for less common defects or to permit reliable or definitive conclusions regarding the safety of acyclovir in pregnant women and their developing fetuses.
- Animal reproduction studies performed at oral doses that provided up to 10 and 7 times the human plasma levels during the period of major organogenesis in rats and rabbits, respectively, revealed no evidence of teratogenicity.
- Australian Drug Evaluation Committee (ADEC) Pregnancy Category
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Valacyclovir in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Valacyclovir during labor and delivery.
Nursing Mothers
- Following oral administration of a 500 mg dose of valacyclovir hydrochloride to 5 nursing mothers, peak acyclovir concentrations (Cmax) in breast milk ranged from 0.5 to 2.3 times (median 1.4) the corresponding maternal acyclovir serum concentrations. The acyclovir breast milk AUC ranged from 1.4 to 2.6 times (median 2.2) maternal serum AUC. A 500 mg maternal dosage of valacyclovir hydrochloride twice daily would provide a nursing infant with an oral acyclovir dosage of approximately 0.6 mg/kg/day. This would result in less than 2% of the exposure obtained after administration of a standard neonatal dose of 30 mg/kg/day of intravenous acyclovir to the nursing infant. Unchanged valacyclovir was not detected in maternal serum, breast milk, or infant urine. Caution should be exercised when valacyclovir hydrochloride is administered to a nursing woman.
Pediatric Use
- Valacyclovir hydrochloride is indicated for treatment of cold sores in pediatric patients ≥12 years of age and for treatment of chickenpox in pediatric patients 2 to <18 years of age.
- The use of valacyclovir hydrochloride for treatment of cold sores is based on 2 double-blind, placebo-controlled clinical trials in healthy adults and adolescents (≥12 years of age) with a history of recurrent cold sores.
- The use of valacyclovir hydrochloride for treatment of chickenpox in pediatric patients 2 to <18 years of age is based on single-dose pharmacokinetic and multiple-dose safety data from an open-label trial with valacyclovir and supported by efficacy and safety data from 3 randomized, double-blind, placebo-controlled trials evaluating oral acyclovir in pediatric patients with chickenpox.
- The efficacy and safety of valacyclovir have not been established in pediatric patients:
- <12 years of age with cold sores
- <18 years of age with genital herpes
- <18 years of age with herpes zoster
- <2 years of age with chickenpox
- for suppressive therapy following neonatal HSV infection.
- The pharmacokinetic profile and safety of valacyclovir oral suspension in children <12 years of age were studied in 3 open-label studies. No efficacy evaluations were conducted in any of the 3 studies.
- Study 1 was a single-dose pharmacokinetic, multiple-dose safety study in 27 pediatric patients 1 to <12 years of age with clinically suspected varicella-zoster virus (VZV) infection.
- Study 2 was a single-dose pharmacokinetic and safety study in pediatric patients 1 month to <6 years of age who had an active herpes virus infection or who were at risk for herpes virus infection. Fifty-seven subjects were enrolled and received a single dose of 25 mg/kg valacyclovir oral suspension. In infants and children 3 months to <6 years of age, this dose provided comparable systemic acyclovir exposures to that from a 1 gram dose of valacyclovir in adults (historical data). In infants 1 month to <3 months of age, mean acyclovir exposures resulting from a 25 mg/kg dose were higher (Cmax: ↑30%, AUC: ↑60%) than acyclovir exposures following a 1 gram dose of valacyclovir in adults. Acyclovir is not approved for suppressive therapy in infants and children following neonatal HSV infections; therefore valacyclovir is not recommended for this indication because efficacy cannot be extrapolated from acyclovir.
- Study 3 was a single-dose pharmacokinetic, multiple-dose safety study in 28 pediatric patients 1 to <12 years of age with clinically suspected HSV infection. None of the children enrolled in this study had genital herpes. Each subject was dosed with valacyclovir oral suspension, 10 mg/kg twice daily for 3 to 5 days. Acyclovir systemic exposures in pediatric patients following valacyclovir oral suspension were compared with historical acyclovir systemic exposures in immunocompetent adults receiving the solid oral dosage form of valacyclovir or acyclovir for the treatment of recurrent genital herpes. The mean projected daily acyclovir systemic exposures in pediatric patients across all age-groups (1 to <12 years of age) were lower (Cmax: ↓20%, AUC: ↓33%) compared with the acyclovir systemic exposures in adults receiving valacyclovir 500 mg twice daily, but were higher (daily AUC: ↑16%) than systemic exposures in adults receiving acyclovir 200 mg 5 times daily. Insufficient data are available to support valacyclovir for the treatment of recurrent genital herpes in this age-group because clinical information on recurrent genital herpes in young children is limited; therefore, extrapolating efficacy data from adults to this population is not possible. Moreover, valacyclovir has not been studied in children 1 to <12 years of age with recurrent genital herpes.
Geriatic Use
- Of the total number of subjects in clinical studies of valacyclovir hydrochloride, 906 were 65 and over, and 352 were 75 and over. In a clinical study of herpes zoster, the duration of pain after healing (post-herpetic neuralgia) was longer in patients 65 and older compared with younger adults. Elderly patients are more likely to have reduced renal function and require dose reduction. Elderly patients are also more likely to have renal or CNS adverse events.
Gender
There is no FDA guidance on the use of Valacyclovir with respect to specific gender populations.
Race
There is no FDA guidance on the use of Valacyclovir with respect to specific racial populations.
Renal Impairment
- Dosage reduction is recommended when administering Valacyclovir hydrochloride to patients with renal impairment.
Hepatic Impairment
There is no FDA guidance on the use of Valacyclovir in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Valacyclovir in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Valacyclovir in patients who are immunocompromised.
Administration and Monitoring
Administration
- Oral
Monitoring
There is limited information regarding Monitoring of Valacyclovir in the drug label.
IV Compatibility
There is limited information regarding IV Compatibility of Valacyclovir in the drug label.
Overdosage
Acute Overdose
Signs and Symptoms
- Caution should be exercised to prevent inadvertent overdose. Precipitation of acyclovir in renal tubules may occur when the solubility (2.5 mg/mL) is exceeded in the intratubular fluid.
Management
- In the event of acute renal failure and anuria, the patient may benefit from hemodialysis until renal function is restored.
Chronic Overdose
There is limited information regarding Chronic Overdose of Valacyclovir in the drug label.
Pharmacology
Mechanism of Action
- Valacyclovir is a nucleoside analogue DNA polymerase inhibitor. Valacyclovir hydrochloride is rapidly converted to acyclovir which has demonstrated antiviral activity against HSV types 1 (HSV-1) and 2 (HSV-2) and VZV both in cell culture and in vivo.
- The inhibitory activity of acyclovir is highly selective due to its affinity for the enzyme thymidine kinase (TK) encoded by HSV and VZV. This viral enzyme converts acyclovir into acyclovir monophosphate, a nucleotide analogue. The monophosphate is further converted into diphosphate by cellular guanylate kinase and into triphosphate by a number of cellular enzymes. In biochemical assays, acyclovir triphosphate inhibits replication of herpes viral DNA. This is accomplished in 3 ways: 1) competitive inhibition of viral DNA polymerase, 2) incorporation and termination of the growing viral DNA chain, and 3) inactivation of the viral DNA polymerase. The greater antiviral activity of acyclovir against HSV compared with VZV is due to its more efficient phosphorylation by the viral TK.
Structure
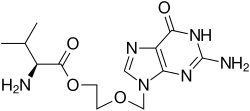
- Valacyclovir hydrochloride USP is the hydrochloride salt of the L-valyl ester of the antiviral drug acyclovir.
- Valacyclovir tablets, USP are for oral administration. Each tablet contains valacyclovir hydrochloride USP equivalent to 500 mg or 1 gram valacyclovir and the inactive ingredients croscarmellose sodium, FD&C Blue #2, hydrogenated castor oil, hypromellose, polyethylene glycol, polysorbate 80, starch (corn), and titanium dioxide.
- The chemical name of valacyclovir hydrochloride is L-valine, 2-[(2-amino-1,6-dihydro-6-oxo-9H-purin-9-yl)methoxy]ethyl ester, monohydrochloride. It has the following structural formula:
- Valacyclovir hydrochloride USP is a white to off-white powder with the molecular formula C13H20N6O4•HCl and a molecular weight of 360.80. The maximum solubility in water at 25°C is 174 mg/mL. The pkas for valacyclovir hydrochloride are 1.90, 7.47, and 9.43.
Pharmacodynamics
There is limited information regarding Pharmacodynamics of Valacyclovir in the drug label.
Pharmacokinetics
- The pharmacokinetics of valacyclovir and acyclovir after oral administration of valacyclovir hydrochloride have been investigated in 14 volunteer studies involving 283 adults and in 3 studies involving 112 pediatric subjects from 1 month to <12 years of age.
- Pharmacokinetics in Adults: Absorption and Bioavailability: After oral administration, valacyclovir hydrochloride is rapidly absorbed from the gastrointestinal tract and nearly completely converted to acyclovir and L-valine by first-pass intestinal and/or hepatic metabolism.
- The absolute bioavailability of acyclovir after administration of valacyclovir hydrochloride is 54.5% ± 9.1% as determined following a 1 gram oral dose of valacyclovir hydrochloride and a 350 mg intravenous acyclovir dose to 12 healthy volunteers. Acyclovir bioavailability from the administration of valacyclovir hydrochloride is not altered by administration with food (30 minutes after an 873 Kcal breakfast, which included 51 grams of fat).
- Acyclovir pharmacokinetic parameter estimates following administration of valacyclovir hydrochloride to healthy adult volunteers are presented in Table 3. There was a less than dose-proportional increase in acyclovir maximum concentration (Cmax) and area under the acyclovir concentration-time curve (AUC) after single-dose and multiple-dose administration (4 times daily) of valacyclovir hydrochloride from doses between 250 mg to 1 gram.
- There is no accumulation of acyclovir after the administration of valacyclovir at the recommended dosage regimens in adults with normal renal function.
- Distribution
- The binding of valacyclovir to human plasma proteins ranges from 13.5% to 17.9%. The binding of acyclovir to human plasma proteins ranges from 9% to 33%.
- Metabolism
- Valacyclovir is converted to acyclovir and L-valine by first-pass intestinal and/or hepatic metabolism. Acyclovir is converted to a small extent to inactive metabolites by aldehyde oxidase and by alcohol and aldehyde dehydrogenase. Neither valacyclovir nor acyclovir is metabolized by cytochrome P450 enzymes. Plasma concentrations of unconverted valacyclovir are low and transient, generally becoming non-quantifiable by 3 hours after administration. Peak plasma valacyclovir concentrations are generally less than 0.5 mcg/mL at all doses. After single-dose administration of 1 gram of valacyclovir hydrochloride, average plasma valacyclovir concentrations observed were 0.5, 0.4, and 0.8 mcg/mL in patients with hepatic dysfunction, renal insufficiency, and in healthy volunteers who received concomitant cimetidine and probenecid, respectively.
- Elimination
- The pharmacokinetic disposition of acyclovir delivered by valacyclovir is consistent with previous experience from intravenous and oral acyclovir. Following the oral administration of a single 1 gram dose of radiolabeled valacyclovir to 4 healthy subjects, 46% and 47% of administered radioactivity was recovered in urine and feces, respectively, over 96 hours. Acyclovir accounted for 89% of the radioactivity excreted in the urine. Renal clearance of acyclovir following the administration of a single 1 gram dose of valacyclovir hydrochloride to 12 healthy volunteers was approximately 255 ± 86 mL/min which represents 42% of total acyclovir apparent plasma clearance.
- The plasma elimination half-life of acyclovir typically averaged 2.5 to 3.3 hours in all studies of valacyclovir hydrochloride in volunteers with normal renal function.
- Specific Populations
- Renal Impairment: Reduction in dosage is recommended in patients with renal impairment.
- Following administration of valacyclovir hydrochloride to volunteers with ESRD, the average acyclovir half-life is approximately 14 hours. During hemodialysis, the acyclovir half-life is approximately 4 hours. Approximately one third of acyclovir in the body is removed by dialysis during a 4-hour hemodialysis session. Apparent plasma clearance of acyclovir in dialysis patients was 86.3 ± 21.3 mL/min/1.73 m2 compared with 679.16 ± 162.76 mL/min/1.73 m2 in healthy volunteers.
- Hepatic Impairment
- Administration of valacyclovir hydrochloride to patients with moderate (biopsy-proven cirrhosis) or severe (with and without ascites and biopsy-proven cirrhosis) liver disease indicated that the rate but not the extent of conversion of valacyclovir to acyclovir is reduced, and the acyclovir half-life is not affected. Dosage modification is not recommended for patients with cirrhosis.
- HIV Disease
- In 9 patients with HIV disease and CD4+ cell counts <150 cells/mm3 who received valacyclovir hydrochloride at a dosage of 1 gram 4 times daily for 30 days, the pharmacokinetics of valacyclovir and acyclovir were not different from that observed in healthy volunteers.
- Geriatrics
- After single-dose administration of 1 gram of valacyclovir hydrochloride in healthy geriatric volunteers, the half-life of acyclovir was 3.11 ± 0.51 hours, compared with 2.91 ± 0.63 hours in healthy younger adult volunteers. The pharmacokinetics of acyclovir following single- and multiple-dose oral administration of valacyclovir hydrochloride in geriatric volunteers varied with renal function. Dose reduction may be required in geriatric patients, depending on the underlying renal status of the patient.
- Pediatrics
- Acyclovir pharmacokinetics have been evaluated in a total of 98 pediatric patients (1 month to <12 years of age) following administration of the first dose of an extemporaneous oral suspension of valacyclovir. Acyclovir pharmacokinetic parameter estimates following a 20 mg/kg dose are provided in Table 4.
- Drug Interactions
- When valacyclovir hydrochloride is coadministered with antacids, cimetidine and/or probenicid, digoxin, or thiazide diuretics in patients with normal renal function, the effects are not considered to be of clinical significance (see below). Therefore, when valacyclovir hydrochloride is coadministered with these drugs in patients with normal renal function, no dosage adjustment is recommended.
- Antacids
- The pharmacokinetics of acyclovir after a single dose of valacyclovir hydrochloride (1 gram) were unchanged by coadministration of a single dose of antacids (Al3+ or Mg++).
- Cimetidine
- Acyclovir Cmax and AUC following a single dose of valacyclovir hydrochloride (1 gram) increased by 8% and 32%, respectively, after a single dose of cimetidine (800 mg).
- Cimetidine Plus Probenecid
- Acyclovir Cmax and AUC following a single dose of valacyclovir hydrochloride (1 gram) increased by 30% and 78%, respectively, after a combination of cimetidine and probenecid, primarily due to a reduction in renal clearance of acyclovir.
- Digoxin
- The pharmacokinetics of digoxin were not affected by coadministration of valacyclovir hydrochloride 1 gram 3 times daily, and the pharmacokinetics of acyclovir after a single dose of valacyclovir hydrochloride (1 gram) was unchanged by coadministration of digoxin (2 doses of 0.75 mg).
- Probenecid
- Acyclovir Cmax and AUC following a single dose of valacyclovir hydrochloride (1 gram) increased by 22% and 49%, respectively, after probenecid (1 gram).
- Thiazide Diuretics
Microbiology
- Antiviral Activities
- The quantitative relationship between the cell culture susceptibility of herpes viruses to antivirals and the clinical response to therapy has not been established in humans, and virus sensitivity testing has not been standardized. Sensitivity testing results, expressed as the concentration of drug required to inhibit by 50% the growth of virus in cell culture (EC50), vary greatly depending upon a number of factors. Using plaque-reduction assays, the EC50 values against herpes simplex virus isolates range from 0.09 to 60 μM (0.02 to 13.5 mcg/mL) for HSV-1 and from 0.04 to 44 μM (0.01 to 9.9 mcg/mL) for HSV-2. The EC50 values for acyclovir against most laboratory strains and clinical isolates of VZV range from 0.53 to 48 μM (0.12 to 10.8 mcg/mL). Acyclovir also demonstrates activity against the Oka vaccine strain of VZV with a mean EC50 of 6 μM (1.35 mcg/mL).
- Resistance
- Resistance of HSV and VZV to acyclovir can result from qualitative and quantitative changes in the viral TK and/or DNA polymerase. Clinical isolates of VZV with reduced susceptibility to acyclovir have been recovered from patients with AIDS. In these cases, TK-deficient mutants of VZV have been recovered.
- Resistance of HSV and VZV to acyclovir occurs by the same mechanisms. While most of the acyclovir-resistant mutants isolated thus far from immunocompromised patients have been found to be TK-deficient mutants, other mutants involving the viral TK gene (TK partial and TK altered) and DNA polymerase have also been isolated. TK-negative mutants may cause severe disease in immunocompromised patients. The possibility of viral resistance to valacyclovir (and therefore, to acyclovir) should be considered in patients who show poor clinical response during therapy.
Nonclinical Toxicology
- The data presented below include references to the steady-state acyclovir AUC observed in humans treated with 1 gram valacyclovir hydrochloride given orally 3 times a day to treat herpes zoster. Plasma drug concentrations in animal studies are expressed as multiples of human exposure to acyclovir.
- Valacyclovir was noncarcinogenic in lifetime carcinogenicity bioassays at single daily doses (gavage) of valacyclovir giving plasma acyclovir concentrations equivalent to human levels in the mouse bioassay and 1.4 to 2.3 times human levels in the rat bioassay. There was no significant difference in the incidence of tumors between treated and control animals, nor did valacyclovir shorten the latency of tumors.
- Valacyclovir was tested in 5 genetic toxicity assays. An Ames assay was negative in the absence or presence of metabolic activation. Also negative were an in vitro cytogenetic study with human lymphocytes and a rat cytogenetic study.
- In the mouse lymphoma assay, valacyclovir was not mutagenic in the absence of metabolic activation. In the presence of metabolic activation (76% to 88% conversion to acyclovir), valacyclovir was mutagenic.
- Valacyclovir was mutagenic in a mouse micronucleus assay.
- Valacyclovir did not impair fertility or reproduction in rats at 6 times human plasma levels.
Clinical Studies
Cold Sores (Herpes Labialis)
- Two double-blind, placebo-controlled clinical trials were conducted in 1,856 healthy adults and adolescents (≥12 years old) with a history of recurrent cold sores. Patients self-initiated therapy at the earliest symptoms and prior to any signs of a cold sore. The majority of patients initiated treatment within 2 hours of onset of symptoms. Patients were randomized to valacyclovir hydrochloride 2 grams twice daily on Day 1 followed by placebo on Day 2, valacyclovir hydrochloride 2 grams twice daily on Day 1 followed by 1 gram twice daily on Day 2, or placebo on Days 1 and 2.
- The mean duration of cold sore episodes was about 1 day shorter in treated subjects as compared with placebo. The 2 day regimen did not offer additional benefit over the 1-day regimen.
- No significant difference was observed between subjects receiving valacyclovir hydrochloride or placebo in the prevention of progression of cold sore lesions beyond the papular stage.
Genital Herpes Infections
- Initial Episode: Six hundred forty-three immunocompetent adults with first-episode genital herpes who presented within 72 hours of symptom onset were randomized in a double-blind trial to receive 10 days of valacyclovir hydrochloride 1 gram twice daily (n = 323) or oral acyclovir 200 mg 5 times a day (n = 320). For both treatment groups: the median time to lesion healing was 9 days, the median time to cessation of pain was 5 days, the median time to cessation of viral shedding was 3 days.
- Recurrent Episodes: Three double-blind trials (2 of them placebo-controlled) in immunocompetent adults with recurrent genital herpes were conducted. Patients self-initiated therapy within 24 hours of the first sign or symptom of a recurrent genital herpes episode.
- In 1 study, patients were randomized to receive 5 days of treatment with either valacyclovir hydrochloride 500 mg twice daily (n = 360) or placebo (n = 259). The median time to lesion healing was 4 days in the group receiving valacyclovir hydrochloride 500 mg versus 6 days in the placebo group, and the median time to cessation of viral shedding in patients with at least 1 positive culture (42% of the overall study population) was 2 days in the group receiving valacyclovir hydrochloride 500 mg versus 4 days in the placebo group. The median time to cessation of pain was 3 days in the group receiving valacyclovir hydrochloride 500 mg versus 4 days in the placebo group. Results supporting efficacy were replicated in a second trial.
- In a third study, patients were randomized to receive valacyclovir hydrochloride 500 mg twice daily for 5 days (n = 398) or valacyclovir hydrochloride 500 mg twice daily for 3 days (and matching placebo twice daily for 2 additional days) (n = 402). The median time to lesion healing was about 4½ days in both treatment groups. The median time to cessation of pain was about 3 days in both treatment groups.
- Suppressive Therapy: Two clinical studies were conducted, one in immunocompetent adults and one in HIV-infected adults.
- A double-blind, 12-month, placebo- and active-controlled study enrolled immunocompetent adults with a history of 6 or more recurrences per year. Outcomes for the overall study population are shown in Table 5.
- Subjects with 9 or fewer recurrences per year showed comparable results with valacyclovir hydrochloride 500 mg once daily.
- In a second study, 293 HIV-infected adults on stable antiretroviral therapy with a history of 4 or more recurrences of ano-genital herpes per year were randomized to receive either valacyclovir hydrochloride 500 mg twice daily (n = 194) or matching placebo (n = 99) for 6 months. The median duration of recurrent genital herpes in enrolled subjects was 8 years, and the median number of recurrences in the year prior to enrollment was 5. Overall, the median prestudy HIV-1 RNA was 2.6 log10 copies/mL. Among patients who received valacyclovir hydrochloride, the prestudy median CD4+ cell count was 336 cells/mm3; 11% had <100 cells/mm3, 16% had 100 to 199 cells/mm3, 42% had 200 to 499 cells/mm3, and 31% had ≥500 cells/mm3. Outcomes for the overall study population are shown in Table 6.
- Reduction of Transmission of Genital Herpes: A double-blind, placebo-controlled study to assess transmission of genital herpes was conducted in 1,484 monogamous, heterosexual, immunocompetent adult couples. The couples were discordant for HSV-2 infection. The source partner had a history of 9 or fewer genital herpes episodes per year. Both partners were counseled on safer sex practices and were advised to use condoms throughout the study period. Source partners were randomized to treatment with either valacyclovir hydrochloride 500 mg once daily or placebo once daily for 8 months. The primary efficacy endpoint was symptomatic acquisition of HSV-2 in susceptible partners. Overall HSV-2 acquisition was defined as symptomatic HSV-2 acquisition and/or HSV-2 seroconversion in susceptible partners. The efficacy results are summarized in Table 7.
Herpes Zoster
- Two randomized double-blind clinical trials in immunocompetent adults with localized herpes zoster were conducted. Valacyclovir hydrochloride was compared with placebo in patients less than 50 years of age, and with oral acyclovir in patients greater than 50 years of age. All patients were treated within 72 hours of appearance of zoster rash. In patients less than 50 years of age, the median time to cessation of new lesion formation was 2 days for those treated with valacyclovir hydrochloride compared with 3 days for those treated with placebo. In patients greater than 50 years of age, the median time to cessation of new lesions was 3 days in patients treated with either valacyclovir hydrochloride or oral acyclovir. In patients less than 50 years of age, no difference was found with respect to the duration of pain after healing (post-herpetic neuralgia) between the recipients of valacyclovir hydrochloride and placebo. In patients greater than 50 years of age, among the 83% who reported pain after healing (post-herpetic neuralgia), the median duration of pain after healing [95% confidence interval] in days was: 40 [31, 51], 43 [36, 55], and 59 [41, 77] for 7-day valacyclovir hydrochloride, 14-day valacyclovir hydrochloride, and 7-day oral acyclovir, respectively.
Chickenpox
- The use of valacyclovir hydrochloride for treatment of chickenpox in pediatric patients 2 to <18 years of age is based on single-dose pharmacokinetic and multiple-dose safety data from an open-label trial with valacyclovir and supported by safety and extrapolated efficacy data from 3 randomized, double-blind, placebo-controlled trials evaluating oral acyclovir in pediatric patients.
- The single-dose pharmacokinetic and multiple-dose safety study enrolled 27 pediatric patients 1 to <12 years of age with clinically suspected VZV infection. Each subject was dosed with valacyclovir oral suspension, 20 mg/kg 3 times daily for 5 days. Acyclovir systemic exposures in pediatric patients following valacyclovir oral suspension were compared with historical acyclovir systemic exposures in immunocompetent adults receiving the solid oral dosage form of valacyclovir or acyclovir for the treatment of herpes zoster. The mean projected daily acyclovir exposures in pediatric patients across all age-groups (1 to <12 years of age) were lower (Cmax: ↓13%, AUC: ↓30%) than the mean daily historical exposures in adults receiving valacyclovir 1 gram 3 times daily, but were higher (daily AUC: ↑50%) than the mean daily historical exposures in adults receiving acyclovir 800 mg 5 times daily. The projected daily exposures in pediatric patients were greater (daily AUC approximately 100% greater) than the exposures seen in immunocompetent pediatric patients receiving acyclovir 20 mg/kg 4 times daily for the treatment of chickenpox. Based on the pharmacokinetic and safety data from this study and the safety and extrapolated efficacy data from the acyclovir studies, oral valacyclovir 20 mg/kg 3 times a day for 5 days (not to exceed 1 gram 3 times daily) is recommended for the treatment of chickenpox in pediatric patients 2 to <18 years of age. Because the efficacy and safety of acyclovir for the treatment of chickenpox in children <2 years of age have not been established, efficacy data cannot be extrapolated to support valacyclovir treatment in children <2 years of age with chickenpox. Valacyclovir is also not recommended for the treatment of herpes zoster in children because safety data up to 7 days' duration are not available.
How Supplied
- Valacyclovir tablets, USP (blue, film-coated, capsule-shaped, biconvex tablets) containing valacyclovir hydrochloride equivalent to 500 mg valacyclovir and debossed with "CIPLA" on one side and "153" on the other side.
- Bottle of 30 (NDC 69097-153-02).
- Bottle of 90 (NDC 69097-153-05).
- Bottle of 500 (NDC 69097-153-12).
- Valacyclovir tablets, USP (blue, film-coated, capsule-shaped, biconvex tablets), with a partial scorebar on both sides) containing valacyclovir hydrochloride equivalent to 1 gram valacyclovir and debossed with "CIPLA"on one side and "154" on the other side.
- Bottle of 30 (NDC 69097-154-02).
- Bottle of 90 (NDC 69097-154-05).
- Bottle of 500 (NDC 69097-154-12).
- Storage
- Store at 20°C to 25°C (68°F to 77°F). Dispense in a well-closed container as defined in the USP.
Storage
There is limited information regarding Valacyclovir Storage in the drug label.
Images
Drug Images
{{#ask: Page Name::Valacyclovir |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel


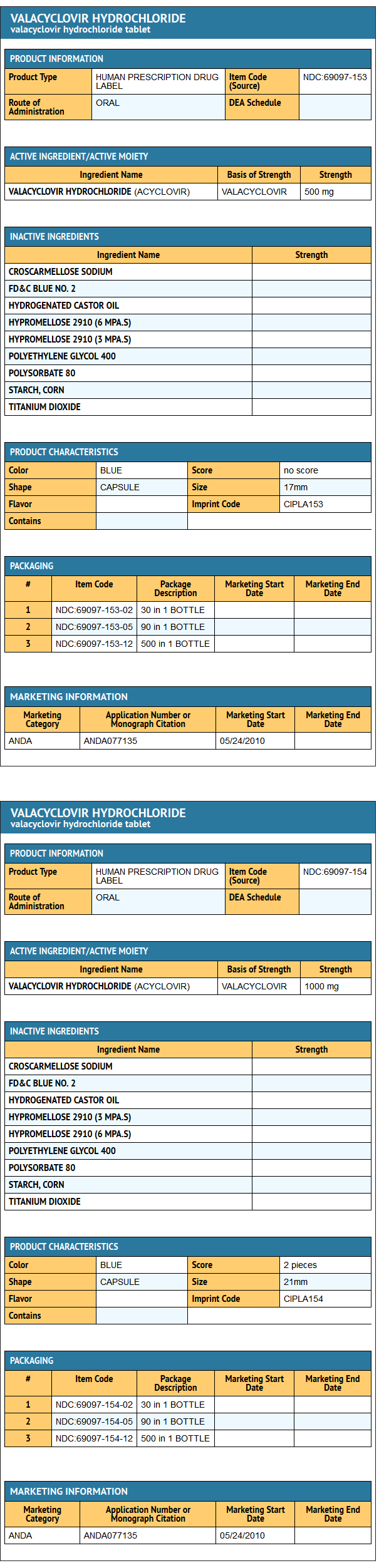
{{#ask: Label Page::Valacyclovir |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
- Importance of Adequate Hydration
- Patients should be advised to maintain adequate hydration.
- Cold Sores (Herpes Labialis)
- Patients should be advised to initiate treatment at the earliest symptom of a cold sore (e.g., tingling, itching, or burning). There are no data on the effectiveness of treatment initiated after the development of clinical signs of a cold sore (e.g., papule, vesicle, or ulcer). Patients should be instructed that treatment for cold sores should not exceed 1 day (2 doses) and that their doses should be taken about 12 hours apart. Patients should be informed that valacyclovir hydrochloride is not a cure for cold sores.
- Genital Herpes
- Patients should be informed that valacyclovir hydrochloride is not a cure for genital herpes. Because genital herpes is a sexually transmitted disease, patients should avoid contact with lesions or intercourse when lesions and/or symptoms are present to avoid infecting partners. Genital herpes is frequently transmitted in the absence of symptoms through asymptomatic viral shedding. Therefore, patients should be counseled to use safer sex practices in combination with suppressive therapy with valacyclovir hydrochloride. Sex partners of infected persons should be advised that they might be infected even if they have no symptoms. Type-specific serologic testing of asymptomatic partners of persons with genital herpes can determine whether risk for HSV-2 acquisition exists.
- Valacyclovir hydrochloride has not been shown to reduce transmission of sexually transmitted infections other than HSV-2.
- If medical management of a genital herpes recurrence is indicated, patients should be advised to initiate therapy at the first sign or symptom of an episode.
- There are no data on the effectiveness of treatment initiated more than 72 hours after the onset of signs and symptoms of a first episode of genital herpes or more than 24 hours after the onset of signs and symptoms of a recurrent episode.
- There are no data on the safety or effectiveness of chronic suppressive therapy of more than 1 year's duration in otherwise healthy patients. There are no data on the safety or effectiveness of chronic suppressive therapy of more than 6 months' duration in HIV-infected patients.
- Herpes Zoster
- There are no data on treatment initiated more than 72 hours after onset of the zoster rash. Patients should be advised to initiate treatment as soon as possible after a diagnosis of herpes zoster.
- Chickenpox
- Patients should be advised to initiate treatment at the earliest sign or symptom of chickenpox.
Precautions with Alcohol
- Alcohol-Valacyclovir interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
- VALACYCLOVIR HYDROCHLORIDE®[4]
Look-Alike Drug Names
- Valtrex® — Keflex®[5]
- valacyclovir® — valganciclovir®[5]
- Valtrex® — Valcyte®[5]
Drug Shortage Status
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
- ↑ Aslanides IM, De Souza S, Wong DT, Giavedoni LR, Altomare F, Detorakis ET; et al. (2002). "Oral valacyclovir in the treatment of acute retinal necrosis syndrome". Retina. 22 (3): 352–4. PMID 12055471.
- ↑ 2.0 2.1 2.2 Kaplan JE, Benson C, Holmes KK, Brooks JT, Pau A, Masur H; et al. (2009). "Guidelines for prevention and treatment of opportunistic infections in HIV-infected adults and adolescents: recommendations from CDC, the National Institutes of Health, and the HIV Medicine Association of the Infectious Diseases Society of America". MMWR Recomm Rep. 58 (RR-4): 1–207, quiz CE1-4. PMID 19357635.
- ↑ Arora A, Mendoza N, Brantley J, Yates B, Dix L, Tyring S (2008). "Double-blind study comparing 2 dosages of valacyclovir hydrochloride for the treatment of uncomplicated herpes zoster in immunocompromised patients 18 years of age and older". J Infect Dis. 197 (9): 1289–95. doi:10.1086/586903. PMID 18422441.
- ↑ "VALACYCLOVIR HYDROCHLORIDE- valacyclovir hydrochloride tablet".
- ↑ 5.0 5.1 5.2 "http://www.ismp.org". External link in
|title=(help)
{