Radiation injury: Difference between revisions
Ochuko Ajari (talk | contribs) |
Ochuko Ajari (talk | contribs) |
||
| Line 125: | Line 125: | ||
*Psychological effects, such as posttraumatic stress disorder | *Psychological effects, such as posttraumatic stress disorder | ||
*Possibility of increased risk of skin cancer later in life | *Possibility of increased risk of skin cancer later in life | ||
==The four stages of ARS are== | ==The four stages of ARS are== | ||
Revision as of 17:16, 1 March 2013
For patient information click here
| Radiation injury | |
 | |
|---|---|
| Radiation Hazard symbol. |
|
Radiation injury Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Radiation injury On the Web |
|
American Roentgen Ray Society Images of Radiation injury |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Cafer Zorkun, M.D., Ph.D. [2]
Table of exposure levels and symptoms
Dose-equivalents are presently stated in sieverts:
0.05–0.2 Sv (5–20 REM)
No symptoms. Potential for cancer and mutation of genetic material, according to the Linear no threshold model (LNT model): this is disputed (Note: see hormesis). A few researchers contend that low dose radiation may be beneficial. [3] [4] [5] 50 mSv is the yearly federal limit for radiation workers in the United States. In the UK the yearly limit for a classified radiation worker is 20 mSv. In Canada, the single-year maximum is 50 mSv, but the maximum 5-year dose is only 100 mSv. Company limits are usually stricter so as not to violate federal limits. [6]
0.2–0.5 Sv (20–50 REM)
No noticeable symptoms. Red blood cell count decreases temporarily.
0.5–1 Sv (50–100 REM)
Mild radiation sickness with headache and increased risk of infection due to disruption of immunity cells. Temporary male sterility is possible.
1–2 Sv (100–200 REM)
Light radiation poisoning, 10% fatality after 30 days (LD 10/30). Typical symptoms include mild to moderate nausea (50% probability at 2 Sv), with occasional vomiting, beginning 3 to 6 hours after irradiation and lasting for up to one day. This is followed by a 10 to 14 day latent phase, after which light symptoms like general illness and fatigue appear (50% probability at 2 Sv). The immune system is depressed, with convalescence extended and increased risk of infection. Temporary male sterility is common. Spontaneous abortion or stillbirth will occur in pregnant women.
2–3 Sv (200–300 REM)
Moderate radiation poisoning, 35% fatality after 30 days (LD 35/30). Nausea is common (100% at 3 Sv), with 50% risk of vomiting at 2.8 Sv. Symptoms onset at 1 to 6 hours after irradiation and last for 1 to 2 days. After that, there is a 7 to 14 day latent phase, after which the following symptoms appear: loss of hair all over the body (50% probability at 3 Sv), fatigue and general illness. There is a massive loss of leukocytes (white blood cells), greatly increasing the risk of infection. Permanent female sterility is possible. Convalescence takes one to several months.
3–4 Sv (300–400 REM)
Severe radiation poisoning, 50% fatality after 30 days (LD 50/30). Other symptoms are similar to the 2–3 Sv dose, with uncontrollable bleeding in the mouth, under the skin and in the kidneys (50% probability at 4 Sv) after the latent phase.
4–6 Sv (400–600 REM)
Acute radiation poisoning, 60% fatality after 30 days (LD 60/30). Fatality increases from 60% at 4.5 Sv to 90% at 6 Sv (unless there is intense medical care). Symptoms start half an hour to two hours after irradiation and last for up to 2 days. After that, there is a 7 to 14 day latent phase, after which generally the same symptoms appear as with 3-4 Sv irradiation, with increased intensity. Female sterility is common at this point. Convalescence takes several months to a year. The primary causes of death (in general 2 to 12 weeks after irradiation) are infections and internal bleeding.
6–10 Sv (600–1,000 REM)
Acute radiation poisoning, near 100% fatality after 14 days (LD 100/14). Survival depends on intense medical care. Bone marrow is nearly or completely destroyed, so a bone marrow transplant is required. Gastric and intestinal tissue are severely damaged. Symptoms start 15 to 30 minutes after irradiation and last for up to 2 days. Subsequently, there is a 5 to 10 day latent phase, after which the person dies of infection or internal bleeding. Recovery would take several years and probably would never be complete.
Devair Alves Ferreira received a dose of approximately 7.0 Sv (700 REM) during the Goiânia accident and survived, partially due to his fractionated exposure.
10–50 Sv (1,000–5,000 REM)
Acute radiation poisoning, 100% fatality after 7 days (LD 100/7). An exposure this high leads to spontaneous symptoms after 5 to 30 minutes. After powerful fatigue and immediate nausea caused by direct activation of chemical receptors in the brain by the irradiation, there is a period of several days of comparative well-being, called the latent (or "walking ghost") phase. After that, cell death in the gastric and intestinal tissue, causing massive diarrhea, intestinal bleeding and loss of water, leads to water-electrolyte imbalance. Death sets in with delirium and coma due to breakdown of circulation. Death is currently inevitable; the only treatment that can be offered is pain therapy.
Louis Slotin was exposed to approximately 21 Sv in a critical accident on 21 May 1946, and died nine days later on 30 May.
At this dose the skin can be damaged. Here is a photo of a man who received a 10 to 20 Gy gamma whole body dose as a result of an industrial accident. He died about 10 days after the photo was taken, about 30 days after the event.
More than 50 Sv (>5,000 REM)
A worker receiving 100 Sv (10,000 REM) in an accident at Wood River, Rhode Island, USA on 24 July 1964 survived for 49 hours after exposure, and an operator receiving between 60 and 180 Sv (18,000 REM) to his upper body in an accident at Los Alamos, New Mexico, USA on 30 December 1958 survived for 36 hours; details of this accident can be found on page 16 (page 30 in the PDF version) of Los Alamos' 2000 Review of Criticality Accidents [7].
Patient Management
Diagnosis
The signs and symptoms of CRI are as follows:
- Intensely painful burn-like skin injuries (including itching, tingling, erythema, or edema) without a history of exposure to heat or caustic chemicals
- Note : Erythema will not be seen for hours to days following exposure, and its appearance is cyclic.
- Epilation
- A tendency to bleed
- Possible signs and symptoms of ARS
As mentioned previously, local injuries to the skin from acute radiation exposure evolve slowly over time, and symptoms may not manifest for days to weeks after exposure. Consider CRI in the differential diagnosis if the patient presents with a skin lesion without a history of chemical or thermal burn, insect bite, or skin disease or allergy. If the patient gives a history of possible radiation exposure (such as from a radiography source, x-ray device, or accelerator) or a history of finding and handling an unknown metallic object, note the presence of any of the following: erythema, blistering, dry or wet desquamation, epilation, ulceration.
Regarding lesions associated with CRI be aware that,
- days to weeks may pass before lesions appear;
- unless patients are symptomatic, they will not require emergency care; and
- lesions can be debilitating and life threatening after several weeks.
Medical follow-up is essential, and victims should be cautioned to avoid trauma to the involved areas.
Initial Treatment
Localized injuries should be treated symptomatically as they occur, and radiation injury experts should be consulted for detailed information. Such information can be obtained from the Radiation Emergency Assistance Center/Training Site (REAC/TS) at www.orau.gov/reacts/ or (865) 576-1005.
As with ARS, if the patient also has other trauma, wounds should be closed, burns covered, fractures reduced, surgical stabilization performed, and definitive treatment given within the first 48 hours after injury. After 48 hours, surgical interventions should be delayed until hematopoietic recovery has occurred.
A baseline CBC and differential should be taken and repeated in 24 hours. Because cutaneous radiation injury is cyclic, areas of early erythema should be noted and recorded. These areas should also be sketched and photographed, if possible, ensuring that the date and time are recorded. The following should be initiated as indicated:
- Supportive care in a clean environment (a burn unit if one is available)
- Prevention and treatment of infections
- Use of the following:
- Medications to reduce inflammation, inhibit protealysis, relieve pain, stimulate regeneration, and improve circulation
- Anticoagulant agents for widespread and deep injury
- Pain management
- Psychological support
Recommendations for Treatment by Stage
The following recommendations for treatment by stage of the illness were obtained by summarizing recommendations from Ricks et al. (226) and Gusev et al. (231), but they do not represent official recommendations of CDC.
- Prodromal Stage —Use antihistamines and topical antipruriginous preparations, which act against itch and also might prevent or attenuate initiation of the cycle that leads to the manifestation stage. Anti-inflammatory medications such as corticosteroids and topical creams, as well as slight sedatives, may prove useful.
- Latent Stage —Continue anti-inflammatory medications and sedatives. At midstage, use proteolysis inhibitors, such as Gordox®.
- Manifestation Stage —Use repeated swabs, antibiotic prophylaxis, and anti-inflammatory medications, such as Lioxasol®, to reduce bacterial, fungal, and viral infections
- Apply topical ointments containing corticosteroids along with locally acting antibiotics and vitamins.
- Stimulate regeneration of DNA by using Lioxasol® and later, when regeneration has started, biogenic drugs, such as Actovegin® and Solcoseril®.
- Stimulate blood supply in third or fourth week using Pentoxifylline® (contraindicated for patients with atherosclerotic heart disease).
- Puncture blisters if they are sterile, but do not remove them as long as they are intact.
- Stay alert for wound infection. Antibiotic therapy should be considered according to the individual patient's condition.
- Treat pain according to the individual patient's condition. Pain relief is very difficult and is the most demanding part of the therapeutic process.
- Debride areas of necrosis thoroughly but cautiously.
Treatment of Late Effects
After immediate treatment of radiation injury, an often long and painful process of healing will ensue. The most important concerns are the following:
- Pain management
- Fibrosis or late ulcers
Note : Use of medication to stimulate vascularization, inhibit infection, and reduce fibrosis may be effective. Examples include Pentoxifylline®, vitamin E, and interferon gamma. Otherwise, surgery may be required.
- Necrosis
- Plastic/reconstructive surgery
Note : Surgical treatment is common. It is most effective if performed early in the treatment process. Full-thickness graft and microsurgery techniques usually provide the best results.
- Psychological effects, such as posttraumatic stress disorder
- Possibility of increased risk of skin cancer later in life
The four stages of ARS are
- Prodromal stage (N-V-D stage): The classic symptoms for this stage are nausea, vomiting, as well as anorexia and possibly diarrhea (depending on dose), which occur from minutes to days following exposure. The symptoms may last (episodically) for minutes up to several days.
- Latent stage: In this stage, the patient looks and feels generally healthy for a few hours or even up to a few weeks.
- Manifest illness stage: In this stage the symptoms depend on the specific syndrome (see Table 1) and last from hours up to several months.
- Recovery or death: Most patients who do not recover will die within several months of exposure. The recovery process lasts from several weeks up to two years.
Cutaneous Radiation Syndrome (CRS)
The concept of cutaneous radiation syndrome (CRS) was introduced in recent years to describe the complex pathological syndrome that results from acute radiation exposure to the skin.
ARS usually will be accompanied by some skin damage. It is also possible to receive a damaging dose to the skin without symptoms of ARS, especially with acute exposures to beta radiation or X-rays. Sometimes this occurs when radioactive materials contaminate a patient’s skin or clothes.
When the basal cell layer of the skin is damaged by radiation, inflammation, erythema, and dry or moist desquamation can occur. Also, hair follicles may be damaged, causing epilation. Within a few hours after irradiation, a transient and inconsistent erythema (associated with itching) can occur. Then, a latent phase may occur and last from a few days up to several weeks, when intense reddening, blistering, and ulceration of the irradiated site are visible. In most cases, healing occurs by regenerative means; however, very large skin doses can cause permanent hair loss, damaged sebaceous and sweat glands, atrophy, fibrosis, decreased or increased skin pigmentation, and ulceration or necrosis of the exposed tissue. Patient Management
Triage: If radiation exposure is suspected:
- Secure ABCs (airway, breathing, circulation) and physiologic monitoring (blood pressure, blood gases, electrolyte and urine output) as appropriate.
- Treat major trauma, burns and respiratory injury if evident.
- In addition to the blood samples required to address the trauma, obtain blood samples for CBC (complete blood count), with attention to lymphocyte count, and HLA (human leukocyte antigen) typing prior to any initial transfusion and at periodic intervals following transfusion.
- Treat contamination as needed.
- If exposure occurred within 8 to 12 hours, repeat CBC, with attention to lymphocyte count, 2 or 3 more times (approximately every 2 to 3 hours) to assess lymphocyte depletion.
Diagnosis
The diagnosis of ARS can be difficult to make because ARS causes no unique disease. Also, depending on the dose, the prodromal stage may not occur for hours or days after exposure, or the patient may already be in the latent stage by the time they receive treatment, in which case the patient may appear and feel well when first assessed.
If a patient received more than 0.05 Gy (5 rads) and three or four CBCs are taken within 8 to 12 hours of the exposure, a quick estimate of the dose can be made (see Ricks, et. al. for details). If these initial blood counts are not taken, the dose can still be estimated by using CBC results over the first few days. It would be best to have radiation dosimetrists conduct the dose assessment, if possible.
If a patient is known to have been or suspected of having been exposed to a large radiation dose, draw blood for CBC analysis with special attention to the lymphocyte count, every 2 to 3 hours during the first 8 hours after exposure (and every 4 to 6 hours for the next 2 days). Observe the patient during this time for symptoms and consult with radiation experts before ruling out ARS.
If no radiation exposure is initially suspected, you may consider ARS in the differential diagnosis if a history exists of nausea and vomiting that is unexplained by other causes. Other indications are bleeding, epilation, or white blood count (WBC) and platelet counts abnormally low a few days or weeks after unexplained nausea and vomiting. Again, consider CBC and chromosome analysis and consultation with radiation experts to confirm diagnosis.
Initial Treatment and Diagnostic Evaluation
Treat vomiting, and repeat CBC analysis, with special attention to the lymphocyte count, every 2 to 3 hours for the first 8 to 12 hours following exposure (and every 4 to 6 hours for the following 2 or 3 days). Sequential changes in absolute lymphocyte counts over time are demonstrated below in the Andrews Lymphocyte Nomogram (see Figure 1). Precisely record all clinical symptoms, particularly nausea, vomiting, diarrhea, and itching, reddening or blistering of the skin. Be sure to include time of onset.
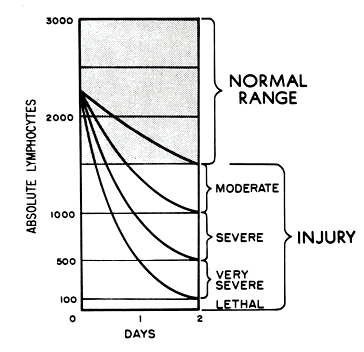
Note and record areas of erythema. If possible, take color photographs of suspected radiation skin damage. Consider tissue, blood typing, and initiating viral prophylaxis. Promptly consult with radiation, hematology, and radiotherapy experts about dosimetry, prognosis, and treatment options. Call the Radiation Emergency Assistance Center/Training Site (REAC/TS) at (865) 576-3131 (M-F, 8 am to 4:30 am EST) or (865) 576-1005 (after hours) to record the incident in the Radiation Accident Registry System.
After consultation, begin the following (as indicated):
- supportive care in a clean environment (if available, the use of a burn unit may be quite effective)
- prevention and treatment of infections
- stimulation of hematopoiesis by use of growth factors
- stem cell transfusions or platelet transfusions (if platelet count is too low)
- psychological support
- careful observation for erythema (document locations), hair loss, skin injury, mucositis, parotitis, weight loss, or fever
- confirmation of initial dose estimate using chromosome aberration cytogenetic bioassay when possible. Although resource intensive, this is the best method of dose assessment following acute exposures.
- consultation with experts in radiation accident management.
Source
References
- Berger ME, O’Hare FM Jr, Ricks RC, editors. The Medical Basis for Radiation Accident Preparedness: The Clinical Care of Victims. REAC/TS Conference on the Medical Basis for Radiation Accident Preparedness. New York : Parthenon Publishing; 2002.
- Gusev IA , Guskova AK , Mettler FA Jr, editors. Medical Management of Radiation Accidents, 2 nd ed., New York : CRC Press, Inc.; 2001.
- Jarrett DG. Medical Management of Radiological Casualties Handbook, 1 st ed. Bethesda , Maryland : Armed Forces Radiobiology Research Institute (AFRRI); 1999.
- LaTorre TE. Primer of Medical Radiobiology, 2 nd ed. Chicago : Year Book Medical Publishers, Inc.; 1989.
- National Council on Radiation Protection and Measurements (NCRP). Management of Terrorist Events Involving Radioactive Material, NCRP Report No. 138. Bethesda , Maryland : NCRP; 2001.
- Prasad KN. Handbook of Radiobiology, 2 nd ed. New York : CRC Press, Inc.; 1995.
Additional Resources
- Michihiko Hachiya, Hiroshima Diary (Chapel Hill: University of North Carolina, 1955), ISBN 0-8078-4547-7.
- John Hersey, Hiroshima (New York: Vintage, 1946, 1985 new chapter), ISBN 0-679-72103-7.
- Ibuse Masuji, Black Rain (1969) ISBN 0-87011-364-X
- Ernest J. Sternglass, Secret Fallout: low-level radiation from Hiroshima to Three-Mile Island (1981) ISBN 0-07-061242-0 (online)
- Norman Solomon, Harvey Wasserman Killing Our Own: The Disaster of America's Experience with Atomic Radiation, 1945-1982, New York: Dell, 1982. ISBN 0-385-28537-X, ISBN 0-385-28536-1, ISBN 0-440-04567-3 (online)
- George N. Hamawy, A Brief Introduction to Radiation Safety (Tucson, Arizona: Wheatmark, 2007), ISBN 1587368935
External links
- Radiation accidents with multi-organ failure in the United States
- List of radiation accidents and other events causing radiation casualties
- The critical accident in Sarov, International Atomic Energy Agency
- The Center for Disease Control's fact sheet on Acute Radiation Syndrome
- Therac-25 computerized radiation therapy machine accidents