Peptic ulcer
| Peptic ulcer | |
 | |
|---|---|
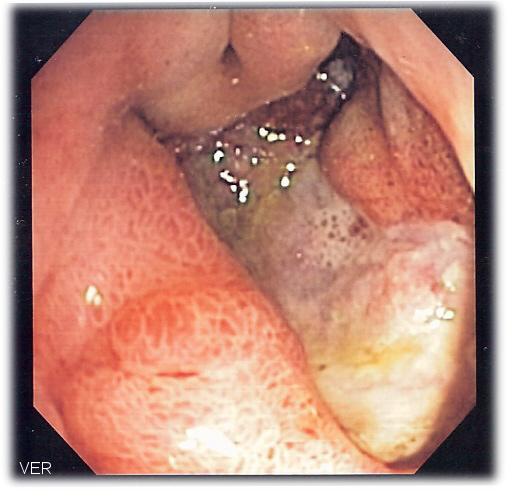
| Deep gastric ulcer | |
| ICD-10 | K25-K27 |
| ICD-9 | 531-534 |
| DiseasesDB | 9819 |
| eMedicine | med/1776 ped/2341 |
| MeSH | D010437 |
|
WikiDoc Resources for Peptic ulcer |
|
Articles |
|---|
|
Most recent articles on Peptic ulcer Most cited articles on Peptic ulcer |
|
Media |
|
Powerpoint slides on Peptic ulcer |
|
Evidence Based Medicine |
|
Clinical Trials |
|
Ongoing Trials on Peptic ulcer at Clinical Trials.gov Clinical Trials on Peptic ulcer at Google
|
|
Guidelines / Policies / Govt |
|
US National Guidelines Clearinghouse on Peptic ulcer
|
|
Books |
|
News |
|
Commentary |
|
Definitions |
|
Patient Resources / Community |
|
Patient resources on Peptic ulcer Discussion groups on Peptic ulcer Patient Handouts on Peptic ulcer Directions to Hospitals Treating Peptic ulcer Risk calculators and risk factors for Peptic ulcer
|
|
Healthcare Provider Resources |
|
Causes & Risk Factors for Peptic ulcer |
|
Continuing Medical Education (CME) |
|
International |
|
|
|
Business |
|
Experimental / Informatics |
For patient information click here
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Please Take Over This Page and Apply to be Editor-In-Chief for this topic: There can be one or more than one Editor-In-Chief. You may also apply to be an Associate Editor-In-Chief of one of the subtopics below. Please mail us [2] to indicate your interest in serving either as an Editor-In-Chief of the entire topic or as an Associate Editor-In-Chief for a subtopic. Please be sure to attach your CV and or biographical sketch.
Overview
A peptic ulcer, also known as PUD or peptic ulcer disease[1] is an ulcer of an area of the gastrointestinal tract that is usually acidic and thus extremely painful. 80% of ulcers are associated with Helicobacter pylori, a spiral-shaped bacterium that lives in the acidic environment of the stomach, however only 20% of those cases go to a doctor (for it is not a dangerous case if caught in time and can be treated with surgery). Ulcers can also be caused or worsened by drugs such as Aspirin and other NSAIDs. Contrary to general belief, more peptic ulcers arise in the duodenum (first part of the small intestine, just after the stomach) than in the stomach. About 4% of stomach ulcers are caused by a malignant tumor, so multiple biopsies are needed to make sure. Duodenal ulcers are generally benign.
Epidemiology
In Western countries the prevalence of Helicobacter pylori infections roughly matches age (i.e., 20% at age 20, 30% at age 30, 80% at age 80 etc). Prevalence is higher in third world countries. Transmission is by food, contaminated groundwater, and through human saliva (such as from kissing or sharing food utensils.)
According to Mayo Clinic, however, there is no evidence that the infection can be transmitted by kissing:
"No evidence indicates that this bacterial infection is transmitted by sharing food or kissing." (http://www.mayoclinic.org/peptic-ulcers/qanda.html))
A minority of cases of Helicobacter infection will eventually lead to an ulcer and a larger proportion of people will get non-specific discomfort, abdominal pain or gastritis.
History
In 1997, the Centers for Disease Control and Prevention, with other government agencies, academic institutions, and industry, launched a national education campaign to inform health care providers and consumers about the link between H. pylori and ulcers. This campaign reinforced the news that ulcers are a curable infection, and the fact that health can be greatly improved and money saved by disseminating information about H. pylori.[2]
Helicobacter pylori was rediscovered in 1982 by two Australian scientists Robin Warren and Barry Marshall[3]. In their original paper, Warren and Marshall contended that most stomach ulcers and gastritis were caused by colonization with this bacterium, not by stress or spicy food as had been assumed before.[4]
The H. pylori hypothesis was poorly received, so in an act of self-experimentation Marshall drank a petri-dish containing a culture of organisms extracted from a patient and soon developed gastritis. His symptoms disappeared after two weeks, but he took antibiotics to kill the remaining bacteria at the urging of his wife, since halitosis is one of the symptoms of infection.[5] This experiment was published in 1984 in the Australian Medical Journal and is among the most cited articles from the journal.
In 2005, the Karolinska Institute in Stockholm awarded the Nobel Prize in Physiology or Medicine to Dr. Marshall and his long-time collaborator Dr. Warren "for their discovery of the bacterium Helicobacter pylori and its role in gastritis and peptic ulcer disease". Professor Marshall continues research related to H. pylori and runs a molecular biology lab at UWA in Perth, Western Australia.
Classification
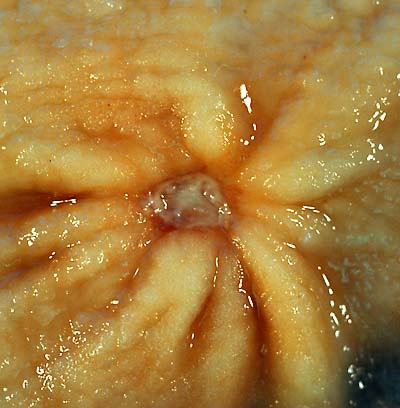
A peptic ulcer may arise at various locations:
- Stomach (called gastric ulcer)
- Duodenum (called duodenal ulcer)
- Esophagus (called esophageal ulcer)
- Meckel's diverticulum
Signs and symptoms
Symptoms of a peptic ulcer can be:
- Abdominal pain, classically epigastric with severity relating to mealtimes, after around 3 hours of taking a meal (duodenal ulcers are classically relieved by food, while gastric ulcers are exacerbated by it);
- Bloating and abdominal fullness
- Waterbrash (rush of saliva after an episode of regurgitation to dilute the acid in esophagus)
- Nausea, and lots of vomiting
- Loss of appetite and weight loss;
- Hematemesis (vomiting of blood); if the blood is just streaks, then the esophagus probably got hurt from all the vomitting.
- Melena (tarry, foul-smelling faeces due to oxidized iron from hemoglobin)
- Rarely, an ulcer can lead to a gastric or duodenal perforation. This is extremely painful and requires immediate surgery.
A history of heartburn, gastroesophageal reflux disease (GERD) and use of certain forms of medication can raise the suspicion for peptic ulcer. Medicines associated with peptic ulcer include NSAID (non-steroid anti-inflammatory drugs) that inhibit cyclooxygenase, and most glucocorticoids (e.g. dexamethasone and prednisolone).
In patients over 45 with more than 2 weeks of the above symptoms, the odds for peptic ulceration are high enough to warrant rapid investigation by EGD (see below).
The timing of the symptoms in relation to the meal may differentiate between gastric and duodenal ulcers: A gastric ulcer would give epigastric pain during the meal, as gastric acid is secreted, or after the meal, as the alkaline duodenal contents reflux into the stomach. Symptoms of duodenal ulcers would manifest mostly before the meal — when acid (production stimulated by hunger) is passed into the duodenum. However, this is not a reliable sign in clinical practice.
Stress and ulcers
Despite the finding that a bacterial infection is the cause of ulcers in 80% of cases, bacterial infection does not appear to explain all ulcers and researchers continue to look at stress as a possible cause, or at least a complication in the development of ulcers.
An expert panel convened by the Academy of Behavioral Medicine research concluded that ulcers are not purely an infectious disease and that psychological factors do play a significant role.[1] Researchers are examining how stress might promote H. pylori infection. For example, Helicobacter pylori thrives in an acidic environment, and stress has been demonstrated to cause the production of excess stomach acid.
The discovery that Helicobacter pylori is a cause of peptic ulcer has tempted many to conclude that psychological factors are unimportant. But this is dichotomised thinking. There is solid evidence that psychological stress triggers many ulcers and impairs response to treatment, while helicobacter is inadequate as a monocausal explanation as most infected people do not develop ulcers. Psychological stress probably functions most often as a cofactor with H pylori. It may act by stimulating the production of gastric acid or by promoting behavior that causes a risk to health. Unravelling the aetiology of peptic ulcer will make an important contribution to the biopsychosocial model of disease.[6]
A study of peptic ulcer patients in a Thai hospital showed that chronic stress was strongly associated with an increased risk of peptic ulcer, and a combination of chronic stress and irregular mealtimes was a significant risk factor (PMID 12948263).
A study on mice showed that both long-term water-immersion-restraint stress and H. pylori infection were independently associated with the development of peptic ulcers (PMID 12465722).
Pathophysiology
Tobacco smoking, blood group, spices and other factors that were suspected to cause ulcers until late in the 20th century, are actually of relatively minor importance in the development of peptic ulcers.[7]
A major causative factor (60% of gastric and 90% of duodenal ulcers) is chronic inflammation due to Helicobacter pylori that colonizes (i.e. settles there after entering the body) the antral mucosa. The immune system is unable to clear the infection, despite the appearance of antibodies. Thus, the bacterium can cause a chronic active gastritis (type B gastritis), resulting in a defect in the regulation of gastrin production by that part of the stomach, and gastrin secretion is increased. Gastrin, in turn, stimulates the production of gastric acid by parietal cells. The acid erodes the mucosa and causes the ulcer.
Another major cause is the use of NSAIDs (see above). The gastric mucosa protects itself from gastric acid with a layer of mucus, the secretion of which is stimulated by certain prostaglandins. NSAIDs block the function of cyclooxygenase 1 (cox-1), which is essential for the production of these prostaglandins. Newer NSAIDs (celecoxib, rofecoxib) only inhibit cox-2, which is less essential in the gastric mucosa, and roughly halve the risk of NSAID-related gastric ulceration.
Glucocorticoids lead to atrophy of all epithelial tissues. Their role in ulcerogenesis is relatively small.
There is debate as to whether Stress in the psychological sense can influence the development of peptic ulcers (see Stress and ulcers above). Burns and head trauma, however, can lead to "stress ulcers", and it is reported in many patients who are on mechanical ventilation.
Smoking leads to atherosclerosis and vascular spasms, causing vascular insufficiency and promoting the development of ulcers through ischemia.
Overuse of laxatives is also known to cause peptic ulcers.
A family history is often present in duodenal ulcers, especially when blood group O is also present. Inheritance appears to be unimportant in gastric ulcers.
Gastrinomas (Zollinger-Ellison syndrome), rare gastrin-secreting tumors, cause multiple and difficult to heal ulcers.
Diagnosis
An esophagogastroduodenoscopy (EGD), a form of endoscopy, also known as a gastroscopy, is carried out on patients in whom a peptic ulcer is suspected. By direct visual identification, the location and severity of an ulcer can be described. Moreover, if no ulcer is present, EGD can often provide an alternative diagnosis.
The diagnosis of Helicobacter pylori can be by:
- Breath testing (does not require EGD);
- Direct culture from an EGD biopsy specimen;
- Direct detection of urease activity in a biopsy specimen;
- Measurement of antibody levels in blood (does not require EGD). It is still somewhat controversial whether a positive antibody without EGD is enough to warrant eradication therapy.
The possibility of other causes of ulcers, notably malignancy (gastric cancer) needs to be kept in mind. This is especially true in ulcers of the greater (large) curvature of the stomach; most are also a consequence of chronic H. pylori infection.
If a peptic ulcer perforates, air will leak from the inside of the gastrointestinal tract (which always contains some air) to the peritoneal cavity (which normally never contains air). This leads to "free gas" within the peritoneal cavity. If the patient stands erect, as when having a chest X-ray, the gas will float to a position underneath the diaphragm. Therefore, gas in the peritoneal cavity, shown on an erect chest X-ray or supine lateral abdominal X-ray, is an omen of perforated peptic ulcer disease.
Macroscopical appearance
Gastric ulcers are most often localized on the lesser curvature of the stomach. The ulcer is a round to oval parietal defect ("hole"), 2 to 4 cm diameter, with a smooth base and perpendicular borders. These borders are not elevated or irregular as in the ulcerative form of gastric cancer. Surrounding mucosa may present radial folds, as a consequence of the parietal scarring.
Microscopical appearance
A gastric peptic ulcer is a mucosal defect which penetrates the muscularis mucosae and muscularis propria, produced by acid-pepsin aggression. Ulcer margins are perpendicular and present chronic gastritis. During the active phase, the base of the ulcer shows 4 zones: inflammatory exudate, fibrinoid necrosis, granulation tissue and fibrous tissue. The fibrous base of the ulcer may contain vessels with thickened wall or with thrombosis.[8]
Differential Diagnosis
- Alcohol
- Alpha-1 Antitrypsin Deficiency
- Basophilic leukemia
- Burns
- Cerebral trauma
- Chronic debilitated conditions
- Chronic obstructive pulmonary disease
- Chronic Renal Failure
- Cigarette smoking
- Cirrhosis
- Cystic Fibrosis
- Glucosteroids
- Helicobacter pylori infection
- Hyperparathyroidism
- Incompetant gastroesophageal sphincter
- NSAIDs
- Severe systemic disease
- Zollinger-Ellison Syndrome
Treatment
Younger patients with ulcer-like symptoms are often treated with antacids or H2 antagonists before EGD is undertaken. Bismuth compounds may actually reduce or even clear organisms.
Patients who are taking nonsteroidal anti-inflammatories (NSAIDs) may also be prescribed a prostaglandin analogue (Misoprostol) in order to help prevent peptic ulcers, which may be a side-effect of the NSAIDs.
When H. pylori infection is present, the most effective treatments are combinations of 2 antibiotics (e.g. Erythromycin, Ampicillin, Amoxicillin, Tetracycline, Metronidazole) and 1 proton pump inhibitor (PPI). An effective combination would be Amoxicillin + Metronidazole + Pantoprazole (a PPI). In the absence of H. pylori, long-term higher dose PPIs are often used.
Treatment of H. pylori usually leads to clearing of infection, relief of symptoms and eventual healing of ulcers. Recurrence of infection can occur and retreatment may be required, if necessary with other antibiotics. Since the widespread use of PPI's in the 1990s, surgical procedures (like "highly selective vagotomy") for uncomplicated peptic ulcers became obsolete.
Perforated peptic ulcer is a surgical emergency and requires surgical repair of the perforation. Most bleeding ulcers require endoscopy urgently to stop bleeding with cauterizations or injection.
Complications
- Gastrointestinal bleeding is the commonest complication. Sudden large bleeding can be life threatening[9]. It occurs when the ulcer erodes one of the blood vessels.
- Perforation (a hole in the wall) often leads to catastrophic consequences. Erosion of the gastro-intestinal wall by the ulcer leads to spillage of stomach or intestinal content into abdominal cavity. Perforation at the anterior surface of stomach leads to acute peritonitis, initially chemical and later bacterial peritonitis. Often first sign is sudden intense abdominal pain. Posterior wall perforation leads to pancreatitis; pain in this situation often radiates to back.
- Penetration is when the ulcer continues into adjacent organs such as liver and pancreas[10].
- Scarring and swelling due to ulcers causes narrowing in the duodenum and gastric outlet obstruction. Patient often presents with severe vomiting.
References
- ↑ 1.0 1.1 "GI Consult: Perforated Peptic Ulcer". Retrieved 2007-08-26.
- ↑ Ulcer, Diagnosis and Treatment - CDC Bacterial, Mycotic Diseases
- ↑ Marshall BJ (1983). "Unidentified curved bacillus on gastric epithelium in active chronic gastritis". Lancet. 1 (8336): 1273–1275. PMID 6134060.
- ↑ Marshall BJ, Warren JR (1984). "Unidentified curved bacilli in the stomach patients with gastritis and peptic ulceration". Lancet. 1 (8390): 1311–1315. PMID 6145023.
- ↑ "Research Enterprise, The 2005 Nobel Prize in Physiology or Medicine". Retrieved 2007-08-26.
- ↑ "Stress and peptic ulcer: life beyond helicobacter". Retrieved 2007-08-26.
- ↑ For nearly 100 years, scientists and doctors thought that ulcers were caused by stress, spicy food, and alcohol. Treatment involved bed rest and a bland diet. Later, researchers added stomach acid to the list of causes and began treating ulcers with antacids. National Digestive Diseases Information Clearinghouse
- ↑ "ATLAS OF PATHOLOGY". Retrieved 2007-08-26.
- ↑ Cullen DJ, Hawkey GM, Greenwood DC; et al. (1997). "Peptic ulcer bleeding in the elderly: relative roles of Helicobacter pylori and non-steroidal anti-inflammatory drugs". Gut. 41 (4): 459–62. PMID 9391242.
- ↑ "Peptic Ulcer: Peptic Disorders: Merck Manual Home Edition". Retrieved 2007-10-10.
External links
- Pathology specimen of Gastric ulcer
- A case report and tutorial on perforated duodenal ulcer
- Causes of Peptic ulcers
Template:SIB Template:Gastroenterology
bs:Ulcerozne lezije želuca ca:Úlcera pèptica da:Mavesår de:Magengeschwür el:Έλκος it:Ulcera peptica nl:Maagzweer no:Magesår nn:Magesår sq:Ulçera në stomak simple:Peptic ulcer fi:Mahahaava sv:Magsår