Frontotemporal lobar degeneration
| Frontotemporal lobar degeneration | |
 | |
|---|---|
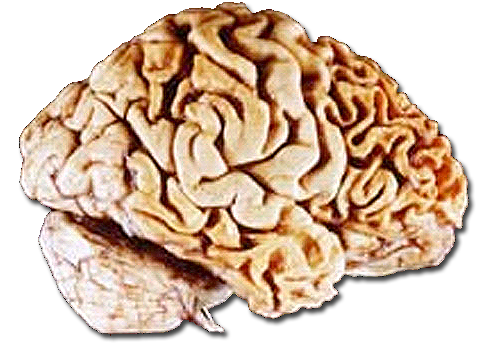
| A human brain showing frontotemporal lobar degeneration causing frontotemporal dementia. | |
| OMIM | 600274 |
| DiseasesDB | 10034 |
| MeSH | D003704 |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Kiran Singh, M.D. [2]
Synonyms and keywords: Disinhibition-dementia-parkinsonism-amyotrophy complex; ddpac; frontotemporal dementia-amyotrophic lateral sclerosis; ftd-als pallidopontonigral degeneration; ppnd FTLD; frontotemporal lobar degeneration with tau inclusions; ftld with tau inclusions; frontotemporal dementia with parkinsonism; frontotemporal lobe dementia; fldem; ftdp17; multiple system tauopathy with presenile dementia; mstd;
Overview
Frontotemporal lobar degeneration (FTLD) is a pathologic process involving degeneration of gray matter in the frontal lobe and anterior portion of the temporal lobe of the cerebrum, with sparing of the parietal and occipital lobes.
Pathophysiology
The gross finding of frontotemporal lobar degeneration is likely produced by several etiologically distinct processes, with unique genetic and histopathological findings. Accordingly, there are a number of possible histopathological findings at post-mortem:
- tau inclusions (either with Pick bodies or without)
- ubiquitin positive (tau-negative) inclusions - in the majority of cases that have this type of pathology the ubiquitinated inclusions contain a protein called TDP-43. There are three subtypes of this type of pathology. Mackenzie et al (and subsequently Davidson et al) describe the following: type 1 with intranuclear inclusions; type 2 with neurites predominantly and type 3 with cytoplasmic inclusions predominantly. It should be noted that not all ubiquitin-positive, tau negative cases stain for TDP-43 e.g. the CHMP2B cases but also other cases.
- Dementia lacking distinctive histology (DLDH) - A rare and controversial entity - new analyses have allowed many cases to be reclassified into one of the positively-defined subgroups.
Genetics
Many cases (possibly up to 50%) of FTLD are genetic rather than sporadic. Mutations in the Tau gene (on chromosome 17q21 - known as MAPT or Microtubule Associated Protein Tau) can cause FTLD and there are over 40 known mutations at present. A series of new mutations associated with FTLD has been recently described in the progranulin gene which is remarkably also on chromosome 17q21. Patients with progranulin mutations have type 1 TDP-43 positive, tau negative pathology at post-mortem. Progranulin is associated with tumorgenesis when overproduced, whereas the mutations seen in the progranulin gene associated with FTLD suggests a deficit in progranulin may be the problem. There are currently 2 other known genes that can cause FTLD: CHMP2B (on chromosome 3) which is associated with a behavioural syndrome (mainly in a large Jutland cohort); and VCP (valosin-containing protein, on chromosome 9) which is associated with the IBMPFD syndrome (inclusion body myopathy, Paget's disease and frontotemporal dementia). These 2 genes only account for a tiny proportion of cases. A locus on chromosome 9 is associated with FTD-MND (or FTD-ALS) i.e. frontotemporal dementia associated with motor neurone disease (or amyotrophic lateral sclerosis) - the hunt for this gene is currently the focus of a number of research labs around the world.
Differential Diagnosis Of Major or Mild Frontotemporal Neurocognitive Disorder
- Other neurocognitive disorders
- Other neurological conditions
- Other mental disorders and medical conditions
- The following table outlines the main findings of the diseases which must be differentiated from dementia with frontotemporal lobar degeneration as they may share common characteristics of cognitive impairment:[2][3][4][5][6][7][8][9][10][11][12][13][14][15][16][17]
| Cause of dementia | Clinical features | Associated features | Nature of progression | Histopathological findings | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Cognitive impairment | ||||||||||||||
| Recall | Recollection | Cue requirement for recall | Infirngement of thoughts | Semantic memory | Procedural memory | Working memory | Awareness | Attention | Executive functioning issues | Visuo-spatial skills | ||||
| Alzheimer's disease | +++
(Slow cognitive and functional decline with early loss of awareness) |
+++ | Not helpful | +++ | ++ | - | ++ | +++ | ++ | ++ | ++ |
|
Has the following clinical stages:
|
|
| Lewy body dementia | ++ | - | Helpful | +++ | + | + | +++ | + | +++ | +++ | +++ |
|
| |
| Frontotemporal lobar degeneration | +/- | - | Helpful | +++ | + | - | +++ | +++ | ++ | +++ | - |
|
|
|
| Vascular dementia | + (Dysexecutive syndrome) | - | Helpful | + | + | + | ++ | - | ++ | +++ | + |
|
|
|
Epidemiology and Demographics Of Major or Mild Frontotemporal Neurocognitive Disorder
Prevalence
The prevalence of major or mild frontotemporal neurocognitive disorder is 2,000-10,000 per 100,000 (2%-10%) of the overall population.[1]
Age
In the over 65 age group, FTLD is probably the fourth most common cause of dementia after Alzheimer's disease, Dementia with Lewy bodies and vascular dementia. In the below 65 age group, it is the second most common cause after Alzheimer's disease. The process of FTLD is thought to be the main cause of three clinical syndromes: frontotemporal dementia, semantic dementia, and progressive nonfluent aphasia.
Risk Factors Of Major or Mild Frontotemporal Neurocognitive Disorder
- Genetic predisposition
- Motor neuron disease[1]
Diagnosis
Symptoms
Physical Examination
Neuro
- Ocular motility abnormalities
- Pyramidal tract dysfunction
- Frontal lobe release signs
- Perseverative vocalizations
- Bradykinesia
- Postural instability
DSM-V Diagnostic Criteria for Major Or Mild Frontotemporal Neurocognitive Disorder[1]
| “ |
AND
AND
AND
AND
Probable frontotemporal neurocognitive disorderis diagnosed if either of the following is present; otherwise, possible frontotemporal neurocognitive disorder should be diagnosed:
Possible frontotemporal neurocognitive disorderis diagnosed if there is no evidence of a genetic mutation, and neuro imaging has not been performed. |
” |
References
- ↑ 1.0 1.1 1.2 1.3 Diagnostic and statistical manual of mental disorders : DSM-5. Washington, D.C: American Psychiatric Association. 2013. ISBN 0890425558.
- ↑ Jellinger KA (2008). "The pathology of "vascular dementia": a critical update". J. Alzheimers Dis. 14 (1): 107–23. PMID 18525132.
- ↑ Murayama S (2008). "[Neuropathology of frontotemporal dementia]". Rinsho Shinkeigaku (in Japanese). 48 (11): 998. PMID 19198143.
- ↑ Hodges JR, Patterson K (1996). "Nonfluent progressive aphasia and semantic dementia: a comparative neuropsychological study". J Int Neuropsychol Soc. 2 (6): 511–24. PMID 9375155.
- ↑ Hodges JR, Patterson K, Oxbury S, Funnell E (1992). "Semantic dementia. Progressive fluent aphasia with temporal lobe atrophy". Brain. 115 ( Pt 6): 1783–806. PMID 1486461.
- ↑ "Dementia, Globalization and Contemporary Art".
- ↑ Helkala EL, Laulumaa V, Soininen H, Riekkinen PJ (1988). "Recall and recognition memory in patients with Alzheimer's and Parkinson's diseases". Ann. Neurol. 24 (2): 214–7. doi:10.1002/ana.410240207. PMID 3178177.
- ↑ Weintraub S, Wicklund AH, Salmon DP (2012). "The neuropsychological profile of Alzheimer disease". Cold Spring Harb Perspect Med. 2 (4): a006171. doi:10.1101/cshperspect.a006171. PMC 3312395. PMID 22474609.
- ↑ Goldman JG, Williams-Gray C, Barker RA, Duda JE, Galvin JE (2014). "The spectrum of cognitive impairment in Lewy body diseases". Mov. Disord. 29 (5): 608–21. doi:10.1002/mds.25866. PMC 4126402. PMID 24757110.
- ↑ Metzler-Baddeley C (2007). "A review of cognitive impairments in dementia with Lewy bodies relative to Alzheimer's disease and Parkinson's disease with dementia". Cortex. 43 (5): 583–600. PMID 17715794.
- ↑ Uversky VN (2008). "Alpha-synuclein misfolding and neurodegenerative diseases". Curr. Protein Pept. Sci. 9 (5): 507–40. PMID 18855701.
- ↑ Bennett DA, Schneider JA, Wilson RS, Bienias JL, Arnold SE (2004). "Neurofibrillary tangles mediate the association of amyloid load with clinical Alzheimer disease and level of cognitive function". Arch. Neurol. 61 (3): 378–84. doi:10.1001/archneur.61.3.378. PMID 15023815.
- ↑ Brion JP (1998). "Neurofibrillary tangles and Alzheimer's disease". Eur. Neurol. 40 (3): 130–40. PMID 9748670.
- ↑ Lee JS, Jung NY, Jang YK, Kim HJ, Seo SW, Lee J, Kim YJ, Lee JH, Kim BC, Park KW, Yoon SJ, Jeong JH, Kim SY, Kim SH, Kim EJ, Park KC, Knopman DS, Na DL (2017). "Prognosis of Patients with Behavioral Variant Frontotemporal Dementia Who have Focal Versus Diffuse Frontal Atrophy". J Clin Neurol. 13 (3): 234–242. doi:10.3988/jcn.2017.13.3.234. PMC 5532319. PMID 28748674.
- ↑ Pao WC, Dickson DW, Crook JE, Finch NA, Rademakers R, Graff-Radford NR (2011). "Hippocampal sclerosis in the elderly: genetic and pathologic findings, some mimicking Alzheimer disease clinically". Alzheimer Dis Assoc Disord. 25 (4): 364–8. doi:10.1097/WAD.0b013e31820f8f50. PMC 3107353. PMID 21346515.
- ↑ Tsolaki M, Kokarida K, Iakovidou V, Stilopoulos E, Meimaris J, Kazis A (2001). "Extrapyramidal symptoms and signs in Alzheimer's disease: prevalence and correlation with the first symptom". Am J Alzheimers Dis Other Demen. 16 (5): 268–78. doi:10.1177/153331750101600512. PMID 11603162.
- ↑ McGuinness B, Barrett SL, Craig D, Lawson J, Passmore AP (2010). "Executive functioning in Alzheimer's disease and vascular dementia". Int J Geriatr Psychiatry. 25 (6): 562–8. doi:10.1002/gps.2375. PMID 19810010.