Chronic heart failure resident survival guide
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Ayokunle Olubaniyi, M.B,B.S [2]
| Chronic Heart Failure Resident Survival Guide Microchapters |
|---|
| Overview |
| Classification |
| Causes |
| Diagnosis |
| Treatment |
| Do's |
| Don'ts |
Overview
There are several goals in the chronic management of systolic heart failure. One goal of therapy is to improve the patient's symptoms, exercise tolerance and quality of life. Diuretics, along with regular assessment of the patient's weight, minimizes fluid accumulation and the accompanying symptoms of dyspnea and orthopnea. Another goal is to reduce hospitalization and mortality. To achieve the second goal, patients with chronic heart failure should be administered an ACE inhibitor (or ARB if they are ACE intolerant) and a beta blocker. If the patient remains symptomatic, additional therapy may include an aldosterone antagonist.
Goals of Therapy
| Goals | Therapeutic intervention |
|---|---|
| To alleviate symptoms and signs | Diuretics, morphine (no mortality benefit) |
| To reduce mortality | ACE inhibitors[1][2], ARBs, beta blockers[3], aldosterone antagonists[4], hydralazine plus isosorbide dinitrate[5], Omega-3 fatty acid[6][7], CRT[8], ICD[9] |
| To reduce hospitalization | Digoxin[10], ARBs (in HFpEF)[11] |
Classification
Based on the Stage of Heart Failure
| ACCF/AHA Stages | Description |
|---|---|
| A | At high risk for heart failure (HF) but without structural heart disease or symptoms of HF |
| B | Structural heart disease but without signs or symptoms of HF |
| C | Structural heart disease with prior or current symptoms of HF |
| D | Refractory HF requiring specialized interventions |
ACCF - American College of Cardiology Foundation; AHA - American Heart Association
Based on the Severity of Congestive Heart Failure
| NYHA classification |
Description |
|---|---|
| I | No limitation of physical activity. Ordinary physical activity does not cause symptoms of heart failure (HF) |
| II | Slight limitation of physical activity. Comfortable at rest, but ordinary physical activity results in symptoms of HF |
| III | Marked limitation of physical activity. Comfortable at rest, but less than ordinary activity causes symptoms of HF |
| IV | Unable to carry on any physical activity without symptoms of HF, or symptoms of HF at rest |
NYHA - New York Heart Association
Causes
Life Threatening Causes
Chronic heart failure is life threatening and should be treated as such irrespective of the underlying cause.
Common Causes
- Cardiotoxic drugs (e.g. NSAIDs, thiazolidinedione, and certain chemotherapy drugs)
- Concurrent infections e.g., pneumonia, viral illnesses
- Electrolyte imbalances
- Endocrine abnormalities - diabetes mellitus, thyroid disorders (hyperthyroidism, hypothyroidism)
- Excessive alcohol or illicit drug use (e.g. cocaine)
- Medication noncompliance
- Myocardial ischemia or infarction
- Noncompliance with dietary restrictions (e.g., sodium and fluid restriction)
- Progressive valvular disease (e.g. mitral regurgitation)
- Pulmonary embolus
- Uncontrolled arrhythmias
- Uncontrolled hypertension
Complete Diagnostic Approach
The algorithm below describes the diagnostic approach to a patient with chronic heart failure.[12][13][14]
Abbreviations:
ARDS: Acute respiratory distress syndrome;
BNP: B-type natriuretic peptide;
BUN: Blood urea nitrogen;
CAD: Coronary artery disease;
CBC: Complete blood count;
CCB: Calcium channel blocker;
CT: Computed tomography;
CXR: Chest x-ray;
DM: Diabetes mellitus;
EKG: Electrocardiogram;
HTN: Hypertension;
LVEF: Left ventricular ejection fraction;
LVH: Left ventricular hypertrophy;
MI: Myocardial infarction;
MRI: Magnetic resonance imaging;
NT-pro BNP: N-terminal pro-brain natriuretic peptide;
OCPs: Oral contraceptive pills;
PAWP: Pulmonary artery wedge pressure
TSH: Thyroid stimulating hormone
Characterize the symptoms: Symptoms of fluid accumulation:
❑ Paroxysmal nocturnal dyspnea
❑ Medication history:
❑ Family history:
| |||||||||||||||||||||||||||||
Examine the patient: General appearance:
❑ Pulse
❑ Pulse oximetry
Skin:
Abdominal examination: | |||||||||||||||||||||||||||||
Order tests: Routine (Class I, level of evidence C)
❑ BNP or NT-pro BNP
❑ Chest X-ray (Class I, level of evidence C)
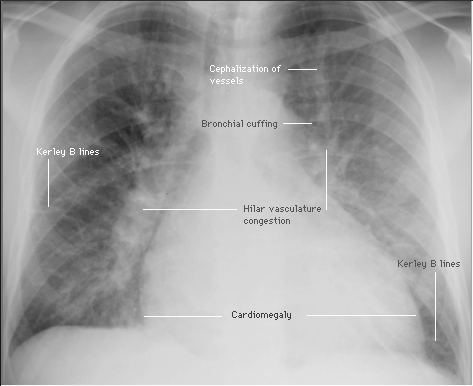 ❑ EKG
❑ 2-D echocardiography with doppler
❑ Radionuclide ventriculography or MRI
❑ Coronary angiography (in settings of ischemia) ❑ ANA, rheumatoid factor (for rheumatologic diseases) | |||||||||||||||||||||||||||||
Consider alternative diagnoses:
| |||||||||||||||||||||||||||||
Treatment
Consider admission:[17] ❑ Hypotension and/or cardiogenic shock | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Assess hemodynamic and volume status ❑ Congestion at rest e.g., narrow pulse pressure, cool extremities, hypotension | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Classify the patient based on the left ventricular ejection fraction | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Systolic heart failure LVEF ≤ 40% | Diastolic heart failure LVEF ≥ 50% | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
First step: Diuresis ❑ | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Second step: ACE Inhibition and Angiotensin Receptor Blockade ❑ | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Third step: Beta blockers ❑ | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Fourth step: Aldosterone Antagonism ❑ | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Fifth step: The Combination of Hydralazine and a Nitrate ❑ | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Sixth step: Digoxin ❑ | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Diuretic Therapy
| Evidence of volume overload | |||||||||||||||||||||
❑ Low sodium diet (<2 g daily)
Contraindications | |||||||||||||||||||||
| Symptomatic improvement? | |||||||||||||||||||||
| Yes | No | ||||||||||||||||||||
| Maintain current IV diuretic dose | Double IV diuretic dose and titrate according to patient's response or when the maximum dose is reached | ||||||||||||||||||||
| No symptomatic improvement | |||||||||||||||||||||
Add ❑ Another diuretic e.g., IV chlorothiazide or oral metolazone | Adjuvants to diuretics ❑ Low dose dopamine to preserve renal function and renal blood flow | ||||||||||||||||||||
| No symptomatic improvement (refractory edema) | |||||||||||||||||||||
| Ultrafiltration or dialysis | |||||||||||||||||||||
General measures ❑ Monitor BP, volume status, congestion ❑ Daily serum electrolytes, urea & creatinine ❑ DVT prophylaxis | |||||||||||||||||||||
Medications
| Drug Class | Drug | Daily doses, maximum daily dose |
|---|---|---|
| Loop diuretics | Furosemide | 20 to 40 mg once or twice, 600 mg max daily dose In HF patients on loop diuretic, the initial IV dose should be greater or equal to their chronic oral daily dose.[20] |
| Bumetanide | 0.5 to 1.0 mg once or twice, 10 mg | |
| Torsemide | 10 to 20 mg once, 200 mg | |
| Thiazide diuretics | Chlorothiazide | 250 to 500 mg once or twice, 1000 mg |
| Hydrochlorothiazide | 25 mg once or twice, 200 mg | |
| Metolazone | 2.5 mg once, 20 mg | |
| K+- sparing diuretic | Amiloride | 5 mg once, 20 mg |
| Spironolactone | 12.5 to 25.0 mg once, 50 mg | |
| Triamterene | 50 to 75 mg twice, 200 mg | |
| ACE inhibitors | Enalapril | 2.5 mg twice, 10 to 20 mg twice |
| Lisinopril | 2.5 to 5 mg once, 20 to 40 mg once | |
| Ramipril | 1.25 to 2.5 mg once, 10 mg once | |
| ARBs | Candesartan | 4 to 8 mg once, 32 mg once |
| Losartan | 25 to 50 mg once, 50 to 150 mg once | |
| Valsartan | 20 to 40 mg twice, 160 mg twice | |
| Beta blockers | Bisoprolol | 1.25 mg once, 10 mg once |
| Carvedilol | 3.125 mg twice, 50 mg twice | |
| Metoprolol succinate | 12.5 to 25.0 mg once, 200 mg once | |
| Aldosterone antagonists | Spironolactone | 12.5 to 25.0 mg once, 25 mg once or twice |
| Eplerenone | 25 mg once, 50 mg once | |
| Inotropes | Dopamine | 5 to 10 mcg/kg/min |
| Dobutamine | 2.5 to 5 mcg/kg/min | |
| Milrinone | 0.125 to 0.75 mcg/kg/min | |
| Vasodilators | Nitroglycerin | 5 to 10 mcg/min, increase dose by 5-10mcg/min every 3-5 mins as tolerated, max is 400mcg/min |
| Nitroprusside | 5 to 10 mcg/min, increase dose by 5-10mcg/min every 5 mins as tolerated, max is 400mcg/min | |
| Nesiritide | 2 mcg/kg bolus; then 0.01 mcg/kg/minute continuous infusion, maximum of 0.03 mcg/kg/minute | |
| Hydralazine and isosorbide dinitrate | Fixed-dose combination | 37.5 mg hydralazine/20 mg isosorbide dinitrate 3 times daily, 75 mg hydralazine/40 mg isosorbide dinitrate 3 times daily |
| Individual doses | Hydralazine: 25 to 50 mg 3 or 4 times daily, 300 mg daily in divided doses Isosorbide dinitrate: 20 to 30 mg 3 or 4 times daily, 120 mg daily in divided doses | |
| Digoxin | 0.125 to 0.25 mg daily |
Do's
- Ensure guideline-directed medical therapy (GDMT) - This is a term which represents the optimal medical therapy in the management of heart failure as defined by ACCF/AHA. These are primarily the class 1 recommendations. It involves the use of ACE inhibitors or (ARBs), beta blockers, aldosterone antagonists, and hydralazine/nitrate medications.
- Order an echocardiogram as soon as possible if no recent one available or if the patient's clinical status is deteriorating.
- Digitalis decreases hospitalization but not mortality. It can be beneficial in symptomatic patients with low EF.[21][22][23][24][25][26][27]
- Make sure your patient is on DVT prophylaxis unless contraindicated.[28][29]
- Daily serum electrolytes, urea nitrogen, and creatinine concentrations should be measured during the use of IV diuretics or active titration of heart failure medications.
- Schedule an early follow-up visit (within 7 to 14 days) and early telephone follow-up (within 3 days) of hospital discharge .[30][31]
Advanced heart failure refers to severe symptoms of heart failure with dyspnea and/or fatigue at rest or with minimal exertion (NYHA class III or IV). These parameters assist in identifying patients with advanced heart failure: [13]
- Repeated (≥2) hospitalizations or ED visits for HF in the past year
- Progressive deterioration in renal function (eg, rise in BUN and creatinine)
- Weight loss without other cause (eg, cardiac cachexia)
- Intolerance to ACE inhibitors due to hypotension and/or worsening renal function
- Intolerance to beta blockers due to worsening HF or hypotension
- Frequent systolic blood pressure <90 mm Hg
- Persistent dyspnea with dressing or bathing requiring rest
- Inability to walk 1 block on the level ground due to dyspnea or fatigue
- Recent need to escalate diuretics to maintain volume status, often reaching daily furosemide equivalent dose over 160 mg/d and/or use of supplemental metolazone therapy
- Progressive decline in serum sodium, usually to < 133 mEq/L
- Frequent ICD shocks
Don'ts
- Avoid the use of NSAIDs, sympathomimetics, tricyclic antidepressants, class I and III antiarrhythmics (except amiodarone), and nondihydropyridine calcium channel blockers (diltiazem, verapamil.[32][33][34][35][36][37][38]
- Don't Use parenteral inotropes in normotensive patients with acute decompensated HF without evidence of decreased organ perfusion. [39]
- Don't combine an ACEI, ARB, and aldosterone antagonist in patients with HFrEF unless otherwise indicated as this combination carries a risk of renal functions worsening and hyperkalemia.
- Avoid using statins solely for heart failure. It adds no benefit.[40][41]
References
- ↑ "Effects of enalapril on mortality in severe congestive heart failure. Results of the Cooperative North Scandinavian Enalapril Survival Study (CONSENSUS). The CONSENSUS Trial Study Group". N Engl J Med. 316 (23): 1429–35. 1987. doi:10.1056/NEJM198706043162301. PMID 2883575.
- ↑ Garg R, Yusuf S (1995). "Overview of randomized trials of angiotensin-converting enzyme inhibitors on mortality and morbidity in patients with heart failure. Collaborative Group on ACE Inhibitor Trials". JAMA. 273 (18): 1450–6. PMID 7654275.
- ↑ Foody JM, Farrell MH, Krumholz HM (2002). "beta-Blocker therapy in heart failure: scientific review". JAMA. 287 (7): 883–9. PMID 11851582.
- ↑ Zannad F, McMurray JJ, Krum H, van Veldhuisen DJ, Swedberg K, Shi H; et al. (2011). "Eplerenone in patients with systolic heart failure and mild symptoms". N Engl J Med. 364 (1): 11–21. doi:10.1056/NEJMoa1009492. PMID 21073363. Review in: J Fam Pract. 2011 Aug;60(8):482-4 Review in: Evid Based Med. 2011 Aug;16(4):121-2
- ↑ Cohn JN, Johnson G, Ziesche S, Cobb F, Francis G, Tristani F; et al. (1991). "A comparison of enalapril with hydralazine-isosorbide dinitrate in the treatment of chronic congestive heart failure". N Engl J Med. 325 (5): 303–10. doi:10.1056/NEJM199108013250502. PMID 2057035.
- ↑ Gissi-HF Investigators. Tavazzi L, Maggioni AP, Marchioli R, Barlera S, Franzosi MG; et al. (2008). "Effect of n-3 polyunsaturated fatty acids in patients with chronic heart failure (the GISSI-HF trial): a randomised, double-blind, placebo-controlled trial". Lancet. 372 (9645): 1223–30. doi:10.1016/S0140-6736(08)61239-8. PMID 18757090. Review in: Ann Intern Med. 2009 Jan 20;150(2):JC1-11
- ↑ Macchia A, Levantesi G, Franzosi MG, Geraci E, Maggioni AP, Marfisi R; et al. (2005). "Left ventricular systolic dysfunction, total mortality, and sudden death in patients with myocardial infarction treated with n-3 polyunsaturated fatty acids". Eur J Heart Fail. 7 (5): 904–9. doi:10.1016/j.ejheart.2005.04.008. PMID 16087142.
- ↑ Cleland JG, Daubert JC, Erdmann E, Freemantle N, Gras D, Kappenberger L; et al. (2005). "The effect of cardiac resynchronization on morbidity and mortality in heart failure". N Engl J Med. 352 (15): 1539–49. doi:10.1056/NEJMoa050496. PMID 15753115. Review in: ACP J Club. 2005 Sep-Oct;143(2):29
- ↑ Bardy GH, Lee KL, Mark DB, Poole JE, Packer DL, Boineau R; et al. (2005). "Amiodarone or an implantable cardioverter-defibrillator for congestive heart failure". N Engl J Med. 352 (3): 225–37. doi:10.1056/NEJMoa043399. PMID 15659722. Review in: ACP J Club. 2005 Jul-Aug;143(1):6
- ↑ Digitalis Investigation Group (1997). "The effect of digoxin on mortality and morbidity in patients with heart failure". N Engl J Med. 336 (8): 525–33. doi:10.1056/NEJM199702203360801. PMID 9036306.
- ↑ Yusuf S, Pfeffer MA, Swedberg K, Granger CB, Held P, McMurray JJ; et al. (2003). "Effects of candesartan in patients with chronic heart failure and preserved left-ventricular ejection fraction: the CHARM-Preserved Trial". Lancet. 362 (9386): 777–81. doi:10.1016/S0140-6736(03)14285-7. PMID 13678871. Review in: ACP J Club. 2004 Mar-Apr;140(2):32-3
- ↑ Yancy CW, Jessup M, Bozkurt B, Butler J, Casey DE, Drazner MH; et al. (2013). "2013 ACCF/AHA guideline for the management of heart failure: executive summary: a report of the American College of Cardiology Foundation/American Heart Association Task Force on practice guidelines". Circulation. 128 (16): 1810–52. doi:10.1161/CIR.0b013e31829e8807. PMID 23741057.
- ↑ 13.0 13.1 13.2 McMurray JJ, Adamopoulos S, Anker SD, Auricchio A, Böhm M, Dickstein K; et al. (2012). "ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure 2012: The Task Force for the Diagnosis and Treatment of Acute and Chronic Heart Failure 2012 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association (HFA) of the ESC". Eur Heart J. 33 (14): 1787–847. doi:10.1093/eurheartj/ehs104. PMID 22611136.
- ↑ Hunt SA, Abraham WT, Chin MH, Feldman AM, Francis GS, Ganiats TG; et al. (2009). "2009 Focused update incorporated into the ACC/AHA 2005 Guidelines for the Diagnosis and Management of Heart Failure in Adults A Report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines Developed in Collaboration With the International Society for Heart and Lung Transplantation". J Am Coll Cardiol. 53 (15): e1–e90. doi:10.1016/j.jacc.2008.11.013. PMID 19358937.
- ↑ Perna, ER.; Macín, SM.; Parras, JI.; Pantich, R.; Farías, EF.; Badaracco, JR.; Jantus, E.; Medina, F.; Brizuela, M. (2002). "Cardiac troponin T levels are associated with poor short- and long-term prognosis in patients with acute cardiogenic pulmonary edema". Am Heart J. 143 (5): 814–20. PMID 12040342. Unknown parameter
|month=ignored (help) - ↑ Fuat A, Murphy JJ, Hungin AP, Curry J, Mehrzad AA, Hetherington A; et al. (2006). "The diagnostic accuracy and utility of a B-type natriuretic peptide test in a community population of patients with suspected heart failure". Br J Gen Pract. 56 (526): 327–33. PMC 1837840. PMID 16638247.
- ↑ Lindenfeld J, Albert NM, Boehmer JP, Collins SP, Ezekowitz JA, Givertz MM, Katz SD, Klapholz M, Moser DK, Rogers JG, Starling RC, Stevenson WG, Tang WH, Teerlink JR, Walsh MN (2010). "HFSA 2010 Comprehensive Heart Failure Practice Guideline". Journal of Cardiac Failure. 16 (6): e1–194. doi:10.1016/j.cardfail.2010.04.004. PMID 20610207. Retrieved 2013-04-29. Unknown parameter
|month=ignored (help) - ↑ Gheorghiade M, Gattis WA, O'Connor CM, Adams KF, Elkayam U, Barbagelata A; et al. (2004). "Effects of tolvaptan, a vasopressin antagonist, in patients hospitalized with worsening heart failure: a randomized controlled trial". JAMA. 291 (16): 1963–71. doi:10.1001/jama.291.16.1963. PMID 15113814.
- ↑ Udelson JE, Smith WB, Hendrix GH, Painchaud CA, Ghazzi M, Thomas I; et al. (2001). "Acute hemodynamic effects of conivaptan, a dual V(1A) and V(2) vasopressin receptor antagonist, in patients with advanced heart failure". Circulation. 104 (20): 2417–23. PMID 11705818.
- ↑ Felker GM, Lee KL, Bull DA, Redfield MM, Stevenson LW, Goldsmith SR, LeWinter MM, Deswal A, Rouleau JL, Ofili EO, Anstrom KJ, Hernandez AF, McNulty SE, Velazquez EJ, Kfoury AG, Chen HH, Givertz MM, Semigran MJ, Bart BA, Mascette AM, Braunwald E, O'Connor CM (2011). "Diuretic strategies in patients with acute decompensated heart failure". The New England Journal of Medicine. 364 (9): 797–805. doi:10.1056/NEJMoa1005419. PMC 3412356. PMID 21366472. Retrieved 2013-04-30. Unknown parameter
|month=ignored (help) - ↑ The Captopril-Digoxin Multicenter Research Group. Comparative effects of therapy with captopril and digoxin in patients with mild to moderate heart failure. JAMA. 1988;259:539–44.
- ↑ Dobbs SM, Kenyon WI, Dobbs RJ. Maintenance digoxin after an episode of heart failure: placebo-controlled trial in outpatients. Br Med J. 1977;1:749–52
- ↑ Lee DC, Johnson RA, Bingham JB, et al. Heart failure in outpatients: a randomized trial of digoxin versus placebo. N Engl J Med. 1982;306: 699–705.
- ↑ Guyatt GH, Sullivan MJ, Fallen EL, et al. A controlled trial of digoxin in congestive heart failure. Am J Cardiol. 1988;61:371–5.
- ↑ . DiBianco R, Shabetai R, Kostuk W, et al. A comparison of oral milrinone, digoxin, and their combination in the treatment of patients with chronic heart failure. N Engl J Med. 1989;320:677–83.
- ↑ Uretsky BF, Young JB, Shahidi FE, et al., for the PROVED Investigative Group. Randomized study assessing the effect of digoxin withdrawal in patients with mild to moderate chronic congestive heart failure: results of the PROVED trial. J Am Coll Cardiol. 1993;22:955–62.
- ↑ Packer M, Gheorghiade M, Young JB, et al. Withdrawal of digoxin from patients with chronic heart failure treated with angiotensin-convertingenzyme inhibitors. RADIANCE Study. N Engl J Med. 1993;329:1–7.
- ↑ Alikhan R, Cohen AT, Combe S, Samama MM, Desjardins L, Eldor A; et al. (2003). "Prevention of venous thromboembolism in medical patients with enoxaparin: a subgroup analysis of the MEDENOX study". Blood Coagul Fibrinolysis. 14 (4): 341–6. PMID 12945875.
- ↑ Guyatt GH, Akl EA, Crowther M, Gutterman DD, Schuünemann HJ, American College of Chest Physicians Antithrombotic Therapy and Prevention of Thrombosis Panel (2012). "Executive summary: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest. 141 (2 Suppl): 7S–47S. doi:10.1378/chest.1412S3. PMC 3278060. PMID 22315257.
- ↑ Krumholz HM, Chen YT, Wang Y, Vaccarino V, Radford MJ, Horwitz RI (2000). "Predictors of readmission among elderly survivors of admission with heart failure". Am Heart J. 139 (1 Pt 1): 72–7. PMID 10618565.
- ↑ Hernandez AF, Greiner MA, Fonarow GC, Hammill BG, Heidenreich PA, Yancy CW; et al. (2010). "Relationship between early physician follow-up and 30-day readmission among Medicare beneficiaries hospitalized for heart failure". JAMA. 303 (17): 1716–22. doi:10.1001/jama.2010.533. PMID 20442387.
- ↑ Heerdink ER, Leufkens HG, Herings RM, et al. NSAIDs associated with increased risk of congestive heart failure in elderly patients taking diuretics. Arch Intern Med. 1998;158:1108–12.
- ↑ . Herchuelz A, Derenne F, Deger F, et al. Interaction between nonsteroidal anti-inflammatory drugs and loop diuretics: modulation by sodiumbalance. J Pharmacol Exp Ther. 1989;248:1175–81.
- ↑ Gottlieb SS, Robinson S, Krichten CM, et al. Renal response to indomethacin in congestive heart failure secondary to ischemic or idiopathic dilated cardiomyopathy. Am J Cardiol. 1992;70:890–3
- ↑ Bank AJ, Kubo SH, Rector TS, et al. Local forearm vasodilation with intra-arterial administration of enalaprilat in humans. Clin Pharmacol Ther. 1991;50:314–21.
- ↑ The Cardiac Arrhythmia Suppression Trial (CAST) Investigators. Preliminary report: effect of encainide and flecainide on mortality in a randomized trial of arrhythmia suppression after myocardial infarction. N Engl J Med. 1989;321:406–12.
- ↑ The Cardiac Arrhythmia Suppression Trial II Investigators. Effect of the antiarrhythmic agent moricizine on survival after myocardial infarction. N Engl J Med. 1992;327:227–33.
- ↑ Pratt CM, Eaton T, Francis M, et al. The inverse relationship between baseline left ventricular ejection fraction and outcome of antiarrhythmic therapy: a dangerous imbalance in the risk-benefit ratio. Am Heart J. 1989;118:433–40.
- ↑ Cuffe MS, Califf RM, Adams KF, Benza R, Bourge R, Colucci WS, Massie BM, O'Connor CM, Pina I, Quigg R, Silver MA, Gheorghiade M (2002). "Short-term intravenous milrinone for acute exacerbation of chronic heart failure: a randomized controlled trial". JAMA : the Journal of the American Medical Association. 287 (12): 1541–7. PMID 11911756. Retrieved 2012-04-06. Unknown parameter
|month=ignored (help) - ↑ Horwich TB, MacLellan WR, Fonarow GC (2004). "Statin therapy is associated with improved survival in ischemic and non-ischemic heart failure". J Am Coll Cardiol. 43 (4): 642–8. doi:10.1016/j.jacc.2003.07.049. PMID 14975476.
- ↑ Gissi-HF Investigators. Tavazzi L, Maggioni AP, Marchioli R, Barlera S, Franzosi MG; et al. (2008). "Effect of rosuvastatin in patients with chronic heart failure (the GISSI-HF trial): a randomised, double-blind, placebo-controlled trial". Lancet. 372 (9645): 1231–9. doi:10.1016/S0140-6736(08)61240-4. PMID 18757089.