Human parainfluenza viruses
|
Human parainfluenza viruses Microchapters |
|
Differentiating Human parainfluenza viruses from other Diseases |
|---|
|
Diagnosis |
|
Treatment |
|
Case Studies |
|
Human parainfluenza viruses On the Web |
|
American Roentgen Ray Society Images of Human parainfluenza viruses |
|
Directions to Hospitals Treating Human parainfluenza viruses |
|
Risk calculators and risk factors for Human parainfluenza viruses |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]
Clinical features
Human parainfluenza viruses (HPIVs) are second to respiratory syncytial virus (RSV) as a common cause of lower respiratory tract disease in young children. Similar to RSV, HPIVs can cause repeated infections throughout life, usually manifested by an upper respiratory tract illness (e.g., a cold and/or sore throat). HPIVs can also cause serious lower respiratory tract disease with repeat infection (e.g., pneumonia, bronchitis, and bronchiolitis), especially among the elderly, and among patients with compromised immune systems.
The viruses
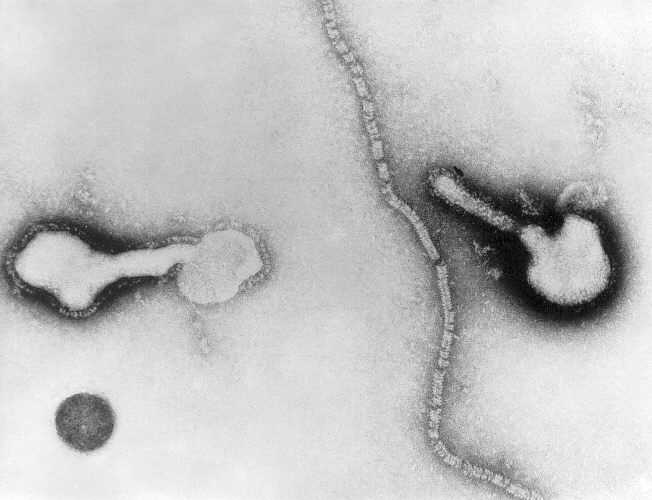
HPIVs are negative-sense, single-stranded RNA viruses that possess fusion and hemagglutinin-neuraminidase glycoprotein "spikes" on their surface. There are four serotypes types of HPIV (1 through 4) and two subtypes (4a and 4b). The virion varies in size (average diameter between 150 and 300 nm) and shape, is unstable in the environment (surviving a few hours on environmental surfaces), and is readily inactivated with soap and water.
Types
The four serotypes include:
- Human parainfluenza virus type 1: HPIV-1 (most common cause of croup; also other upper and lower respiratory tract illnesses typical)
- Human parainfluenza virus type 2: HPIV-2 (causes croup and other upper and lower respiratory tract illnesses)
- Human parainfluenza virus type 3: HPIV-3 (associated with bronchiolitis and pneumonia)
- Human parainfluenza virus type 4: HPIV-4 (includes subtypes 4a and 4b)
Diagnosis
Infection with HPIVs can be confirmed in two ways: 1) by isolation and identification of the virus in cell culture or by direct detection of the virus in respiratory secretions (usually, collected within one week of onset of symptoms) using immunofluorescence, enzyme immunoassay, or polymerase chin reaction assay, and 2) by demonstration of a significant rise in specific IgG antibodies between appropriately collected paired serum specimens or specific IgM antibodies in a single serum specimen.
Prevention
No vaccine is currently available to protect against infection caused by any of the HPIVs; however, researchers are developing vaccines against HPIV-1 and -3 infections. Passively acquired maternal antibodies may play a role in protection from HPIV types 1 and 2 in the first few months of life, highlighting the importance of breast-feeding. Strict attention to infection-control practices should decrease or prevent spread of infection. Frequent handwashing and not sharing items such as cups, glasses, and utensils with an infected person should decrease the spread of virus to others. Excluding children with colds or other respiratory illnesses (without fever) who are well enough to attend child care or school settings will probably not decrease the spread of HPIVs, because the viruses are often spread in the early stages of illness. In a hospital setting, spread of HPIVs can and should be prevented by strict attention to contact precautions, such as handwashing and wearing of protective gowns and gloves.
References
- American Academy of Pediatrics. Parainfluenza Viral Infections. In: Peter G, ed. 1997 Red Book: Report of the Committee on Infectious Diseases. 24th ed. Elk Grove Village, IL: American Academy of Pediatrics; 1997: 379.
- Collins PL, Chanock RM, McIntosh K. Parainfluenza viruses. In: Fields BN, Knipe DM, Howley PM, eds. Fields Virology. 3rd ed. Philadelphia: Lippincott-Raven; 1995: 1205-41.
- Glezen WP, Denny FW. Parainfluenza Viruses In: Evans A, Kaslow R, eds. Viral Infections in Humans: epidemiology and control. 4th ed. New York: Plenum; 1997:551-67.