Dysphagia pathophysiology
|
Dysphagia Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Dysphagia pathophysiology On the Web |
|
American Roentgen Ray Society Images of Dysphagia pathophysiology |
|
Risk calculators and risk factors for Dysphagia pathophysiology |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]Associate Editor(s)-in-Chief: Feham Tariq, MD [2]
Overview
The exact pathogenesis of [disease name] is not fully understood.
OR
It is thought that [disease name] is the result of / is mediated by / is produced by / is caused by either [hypothesis 1], [hypothesis 2], or [hypothesis 3].
OR
[Pathogen name] is usually transmitted via the [transmission route] route to the human host.
OR
Following transmission/ingestion, the [pathogen] uses the [entry site] to invade the [cell name] cell.
OR
[Disease or malignancy name] arises from [cell name]s, which are [cell type] cells that are normally involved in [function of cells].
OR
The progression to [disease name] usually involves the [molecular pathway].
OR
The pathophysiology of [disease/malignancy] depends on the histological subtype.
Pathophysiology
Normal physiology of the food motility through the esophagus
- The esophagus is a part of the gastrointestinal tract which is responsible of moving the food from the mouth to the rectum.[1]
- The esophagus has anti-reflux barrier which prevents the return of the acidic contentof the stomach back to the esophagus. The anti-reflux barrier consists of the lower esophageal sphincter (LES) and the related part of the diaphragm.
- The lower esophageal sphincter is contracting smooth muscle at the end of the esophagus responsible for the food passage to the stomach. LES has high pressure tone which helps keeping it a strong barrier between the esophagus and the stomach.
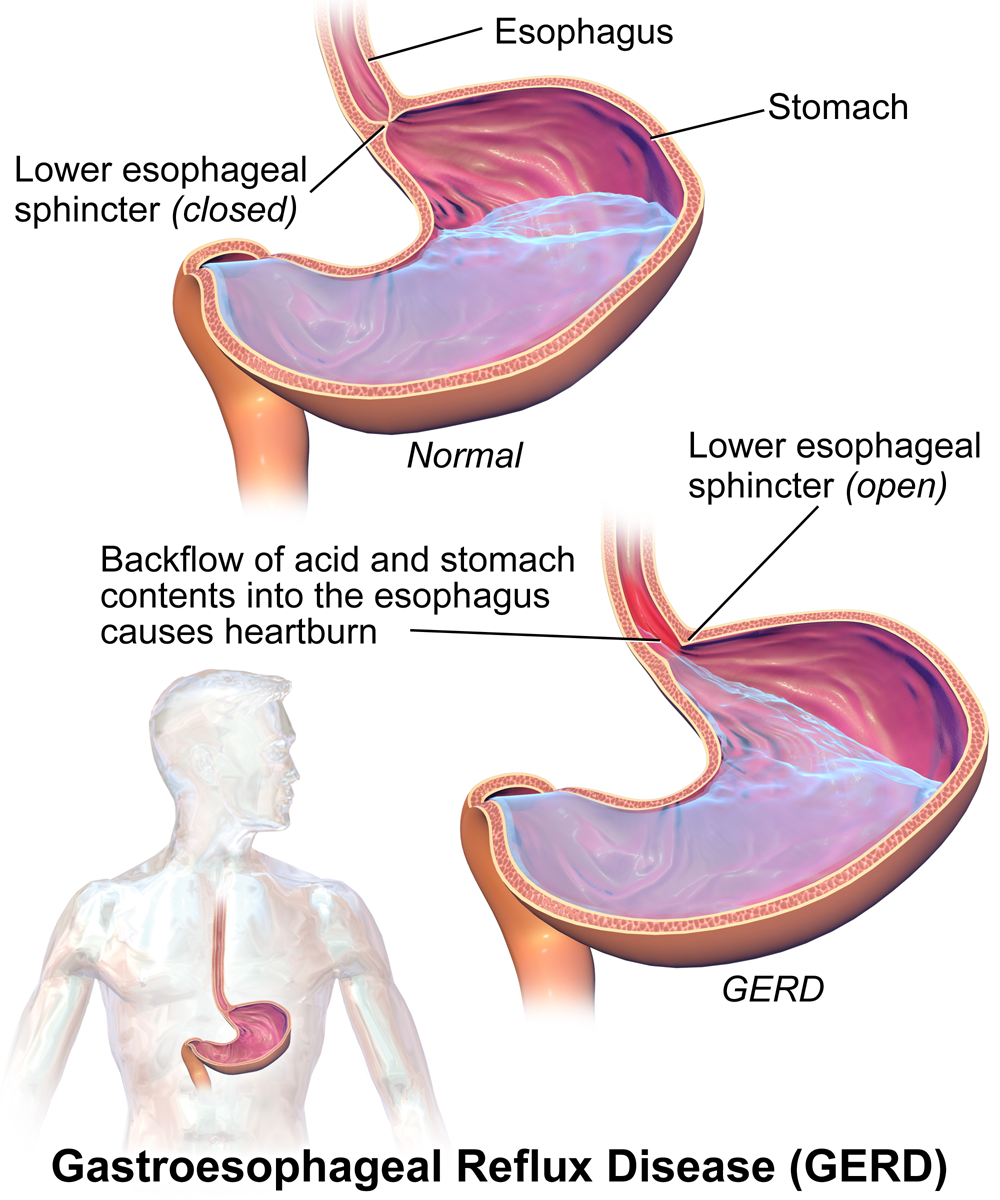
Pathogenesis of Dysphagia
The pathogenesis of dysphagia can be explained on the basis of etiology. There are a number of causes of different types of dysphagia of which the most common being esophageal food impaction. The following table elaborates the mechanism of each cause.
| Cause of dysphagia | Type of food | Type of progression | Mechanism of development | Genes involved | Gross pathology findings | Microscopic findings | |
|---|---|---|---|---|---|---|---|
| Oropharyngeal dysphagia | Soilds | Liquids | Intermittent/Progressive | ||||
| •Zenker's diverticulum
•Webs |
Yes | No | Progressive | •Zenker's diverticulum:
|
Diverticulum or a sac is seen in the esophagus |
| |
| • | |||||||
| •Neoplasm | Yes | Yes | Progressive | •Neoplasm | |||
| Myogenic causes
•Myasthenia gravis •Connective tissue disorder •Myotonic dystrophy Neurogenic causes •ALS •Parkinsonism •Stroke |
Yes | Yes | Progressive | ||||
| Esophageal dysphagia | |||||||
| •Pill esophagitis
•Caustic injury •Chemotherapy |
Yes | No | |||||
| •Strictures
•Cancer |
Yes | No | Progressive | ||||
| •Rings
•Webs |
Yes | No | Intermittent | Rings:
Webs: Multiple theories have been found:
|
|||
| •Achalasia
•Diffuse esophageal spasm(DES) |
Yes | Yes | Intermittent | •Achalasia: | |||
•Diffuse esophageal spasm(DES):
|
There is a genetic association[2] | Gross thickening of muscularis propria layer and lower esophageal sphincter (LES) due to hyperplasia are characteristic findings of DES | There is degeneration of vagal fibres, inflammatory infiltration of myenteric plexus, and hyperplasia of smooth muscles are characteristic findings of DES | ||||
| •Scleroderma | Yes | Yes | Progressive | ||||
References
- ↑ Stein HJ, DeMeester TR (1992). "Outpatient physiologic testing and surgical management of foregut motility disorders". Curr Probl Surg. 29 (7): 413–555. PMID 1606845.
- ↑ Frieling T, Berges W, Borchard F, Lübke HJ, Enck P, Wienbeck M (1988). "Family occurrence of achalasia and diffuse spasm of the oesophagus". Gut. 29 (11): 1595–602. PMC 1433819. PMID 3061886.