Leprosy classification: Difference between revisions
Joao Silva (talk | contribs) |
Joao Silva (talk | contribs) |
||
| Line 4: | Line 4: | ||
==Overview== | ==Overview== | ||
Leprosy may be | Leprosy may be divided according to different systems of classification, from which two of them, the ''Ridley Jopling classification'' and the ''WHO classification'' are the most broadly used. These classifications are based on [[clinical]], [[bacteriological]] and [[histopathological]] features presented by the patient and help to identify the class of leprosy, thereby determining the [[prognosis]] and the [[Therapy|treatment]] regimen to give to that particular patient.<ref name="WalkerLockwood2007">{{cite journal|last1=Walker|first1=Stephen L.|last2=Lockwood|first2=Dina N.J.|title=Leprosy|journal=Clinics in Dermatology|volume=25|issue=2|year=2007|pages=165–172|issn=0738081X|doi=10.1016/j.clindermatol.2006.05.012}}</ref><ref name="EichelmannGonzález González2013">{{cite journal|last1=Eichelmann|first1=K.|last2=González González|first2=S.E.|last3=Salas-Alanis|first3=J.C.|last4=Ocampo-Candiani|first4=J.|title=Leprosy. An Update: Definition, Pathogenesis, Classification, Diagnosis, and Treatment|journal=Actas Dermo-Sifiliográficas (English Edition)|volume=104|issue=7|year=2013|pages=554–563|issn=15782190|doi=10.1016/j.adengl.2012.03.028}}</ref><ref name="BhatPrakash2012">{{cite journal|last1=Bhat|first1=Ramesh Marne|last2=Prakash|first2=Chaitra|title=Leprosy: An Overview of Pathophysiology|journal=Interdisciplinary Perspectives on Infectious Diseases|volume=2012|year=2012|pages=1–6|issn=1687-708X|doi=10.1155/2012/181089}}</ref> | ||
==Classification== | ==Classification== | ||
Revision as of 00:26, 3 July 2014
|
Leprosy Microchapters |
|
Diagnosis |
|---|
|
Treatment |
|
Case Studies |
|
Leprosy classification On the Web |
|
American Roentgen Ray Society Images of Leprosy classification |
|
Risk calculators and risk factors for Leprosy classification |
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: João André Alves Silva, M.D. [2]
Overview
Leprosy may be divided according to different systems of classification, from which two of them, the Ridley Jopling classification and the WHO classification are the most broadly used. These classifications are based on clinical, bacteriological and histopathological features presented by the patient and help to identify the class of leprosy, thereby determining the prognosis and the treatment regimen to give to that particular patient.[1][2][3]
Classification
There are several different approaches for classifying leprosy; however, parallels exist.
- The World Health Organization system distinguishes "paucibacillary" and "multibacillary" based upon the proliferation of bacteria[4]
- The SHAY scale provides five gradations.[5][6]
- The ICD-10, though developed by the WHO, uses Ridley-Jopling and not the WHO system. It also adds an indeterminate ("I") entry.[7]
- In MeSH, three groupings are used.
| WHO | Ridley-Jopling | ICD-10 | MeSH | Description | Lepromin test | Immune target |
|---|---|---|---|---|---|---|
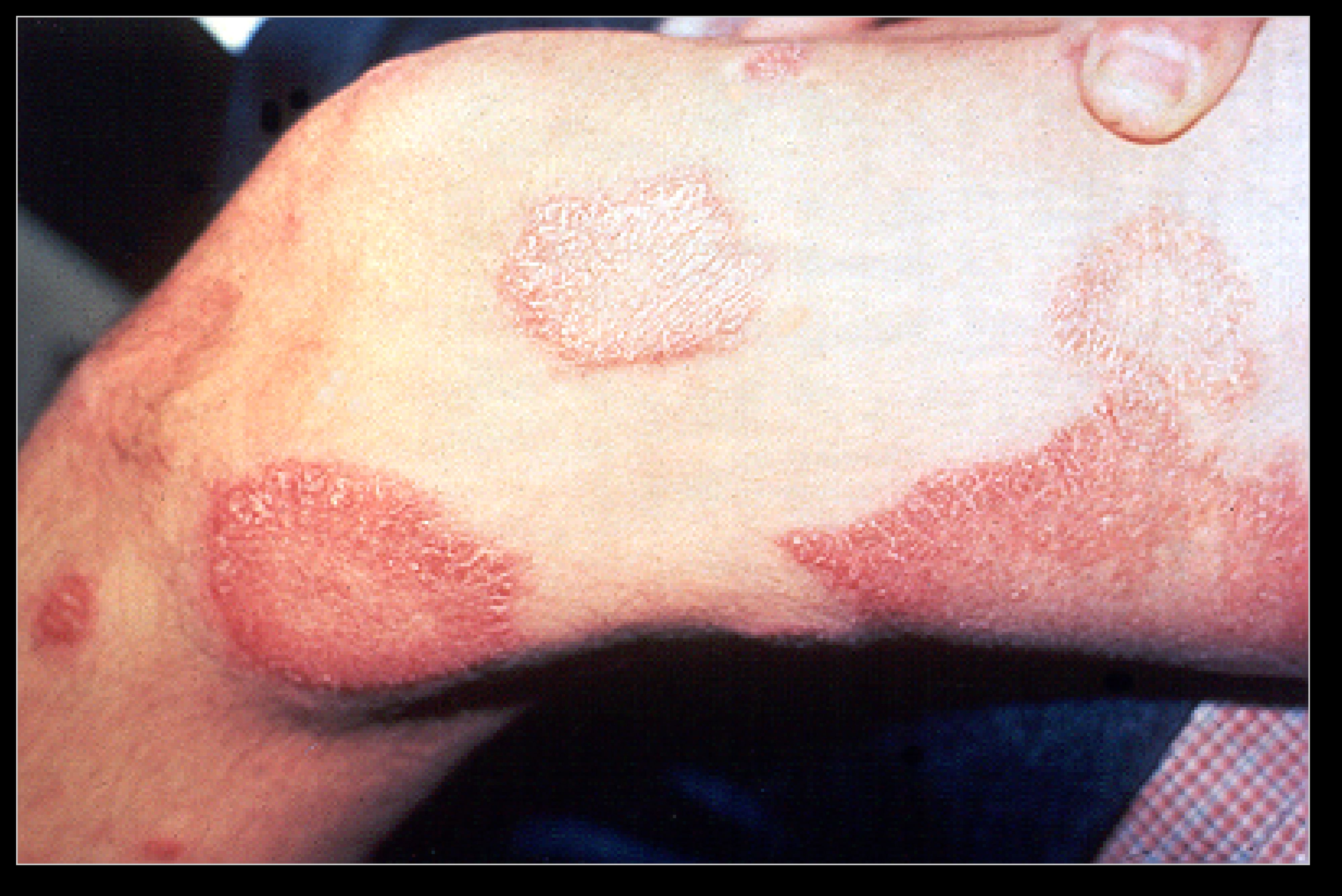
| Paucibacillary | tuberculoid ("TT"), borderline tuberculoid ("BT") | A30.1, A30.2 | Tuberculoid | It is characterized by one or more hypopigmented skin macules and anaesthetic patches, where skin sensations are lost because of damaged peripheral nerves that have been attacked by the human host's immune cells. | Positive | bacillus (Th1) |
| Multibacillary | midborderline or borderline ("BB") | A30.3 | Borderline | Borderline leprosy is of intermediate severity and is the most common form. Skin lesions resemble tuberculoid leprosy but are more numerous and irregular; large patches may affect a whole limb, and peripheral nerve involvement with weakness and loss of sensation is common. This type is unstable and may become more like lepromatous leprosy or may undergo a reversal reaction, becoming more like the tuberculoid form. | ||
| Multibacillary | borderline lepromatous ("BL"), and lepromatous ("LL") | A30.4, A30.5 | Lepromatous | It is associated with symmetric skin lesions, nodules, plaques, thickened dermis, and frequent involvement of the nasal mucosa resulting in nasal congestion and epistaxis (nose bleeds), but, typically, detectable nerve damage is late. | Negative | plasmid inside bacillus (Th2) |
Hansen's disease may also be divided into the following types:[8]
- Early and indeterminate leprosy
- Tuberculoid leprosy
- Borderline tuberculoid leprosy
- Borderline leprosy
- Borderline lepromatous leprosy
- Lepromatous leprosy
- Histoid leprosy
- Diffuse leprosy of Lucio and Latapí
Contrary to popular belief, Hansen's bacillus does not cause rotting of the flesh; rather, a long investigation by Paul Brand yielded that insensitivity in the limbs extremities was the reason why unfelt wounds or lesions, however minute, lead to undetected deterioration of the tissues, the lack of pain not triggering an immediate response as in a fully functioning body. Recently, leprosy has also emerged as a problem in HIV patients on antiretroviral drugs.[9]
References
- ↑ Walker, Stephen L.; Lockwood, Dina N.J. (2007). "Leprosy". Clinics in Dermatology. 25 (2): 165–172. doi:10.1016/j.clindermatol.2006.05.012. ISSN 0738-081X.
- ↑ Eichelmann, K.; González González, S.E.; Salas-Alanis, J.C.; Ocampo-Candiani, J. (2013). "Leprosy. An Update: Definition, Pathogenesis, Classification, Diagnosis, and Treatment". Actas Dermo-Sifiliográficas (English Edition). 104 (7): 554–563. doi:10.1016/j.adengl.2012.03.028. ISSN 1578-2190.
- ↑ Bhat, Ramesh Marne; Prakash, Chaitra (2012). "Leprosy: An Overview of Pathophysiology". Interdisciplinary Perspectives on Infectious Diseases. 2012: 1–6. doi:10.1155/2012/181089. ISSN 1687-708X.
- ↑ Smith DS (2008-08-19). "Leprosy: Overview". eMedicine Infectious Diseases. Retrieved 2010-02-01.
- ↑ Singh N, Manucha V, Bhattacharya SN, Arora VK, Bhatia A (2004). "Pitfalls in the cytological classification of borderline leprosy in the Ridley-Jopling scale". Diagn. Cytopathol. 30 (6): 386–8. doi:10.1002/dc.20012. PMID 15176024. Unknown parameter
|month=ignored (help) - ↑ Ridley DS, Jopling WH (1966). "Classification of leprosy according to immunity. A five-group system". Int. J. Lepr. Other Mycobact. Dis. 34 (3): 255–73. PMID 5950347.
- ↑ "What Is Leprosy?" THE MEDICAL NEWS | from News-Medical.Net - Latest Medical News and Research from Around the World. Web. 20 Nov. 2010. <http://www.news-medical.net/health/What-is-Leprosy.aspx>.
- ↑ James, William D.; Berger, Timothy G.; et al. (2006). Andrews' Diseases of the Skin: clinical Dermatology. Saunders Elsevier. ISBN 0-7216-2921-0.
- ↑ McNeil Jr DG (2006-10-24). "Worrisome New Link: AIDS Drugs and Leprosy". New York Times. Retrieved 2007-05-07.