WBR0322: Difference between revisions
Jump to navigation
Jump to search
No edit summary |
Sergekorjian (talk | contribs) No edit summary |
||
| Line 1: | Line 1: | ||
{{WBRQuestion | {{WBRQuestion | ||
|QuestionAuthor={{ | |QuestionAuthor={{SSK}} {{Alison}} (Reviewed by Serge Korjian) | ||
|ExamType=USMLE Step 1 | |ExamType=USMLE Step 1 | ||
|MainCategory=Immunology | |MainCategory=Immunology | ||
| Line 8: | Line 8: | ||
|MainCategory=Immunology | |MainCategory=Immunology | ||
|SubCategory=Hematology | |SubCategory=Hematology | ||
|MainCategory=Immunology | |||
|MainCategory=Immunology | |MainCategory=Immunology | ||
|MainCategory=Immunology | |MainCategory=Immunology | ||
| Line 20: | Line 21: | ||
|MainCategory=Immunology | |MainCategory=Immunology | ||
|SubCategory=Hematology | |SubCategory=Hematology | ||
|Prompt=A 67-year-old | |Prompt=A 67-year-old man presents to the physician's office with complaints of weight loss, fever, and night sweats. Following appropriate work-up,you diagnose him with acute myelogenous leukemia (AML) and start him on scheduled chemotherapy sessions. Three weeks into the treatment, you detect that patient is profoundly thrombocytopenic and requires a platelet transfusion. During the transfusion, the patient develops fever, chills, and intense flushing, but denies any itching or shortness of breath. On physical exam, you find that the patient has a temperature of 38.5 °C (101.3 °F) , heart rate of 108 bpm, respiratory rate of 18/min, and blood pressure of 128/78 mmHg. What is the most likely cause of this patient's reaction to the platelet transfusion? | ||
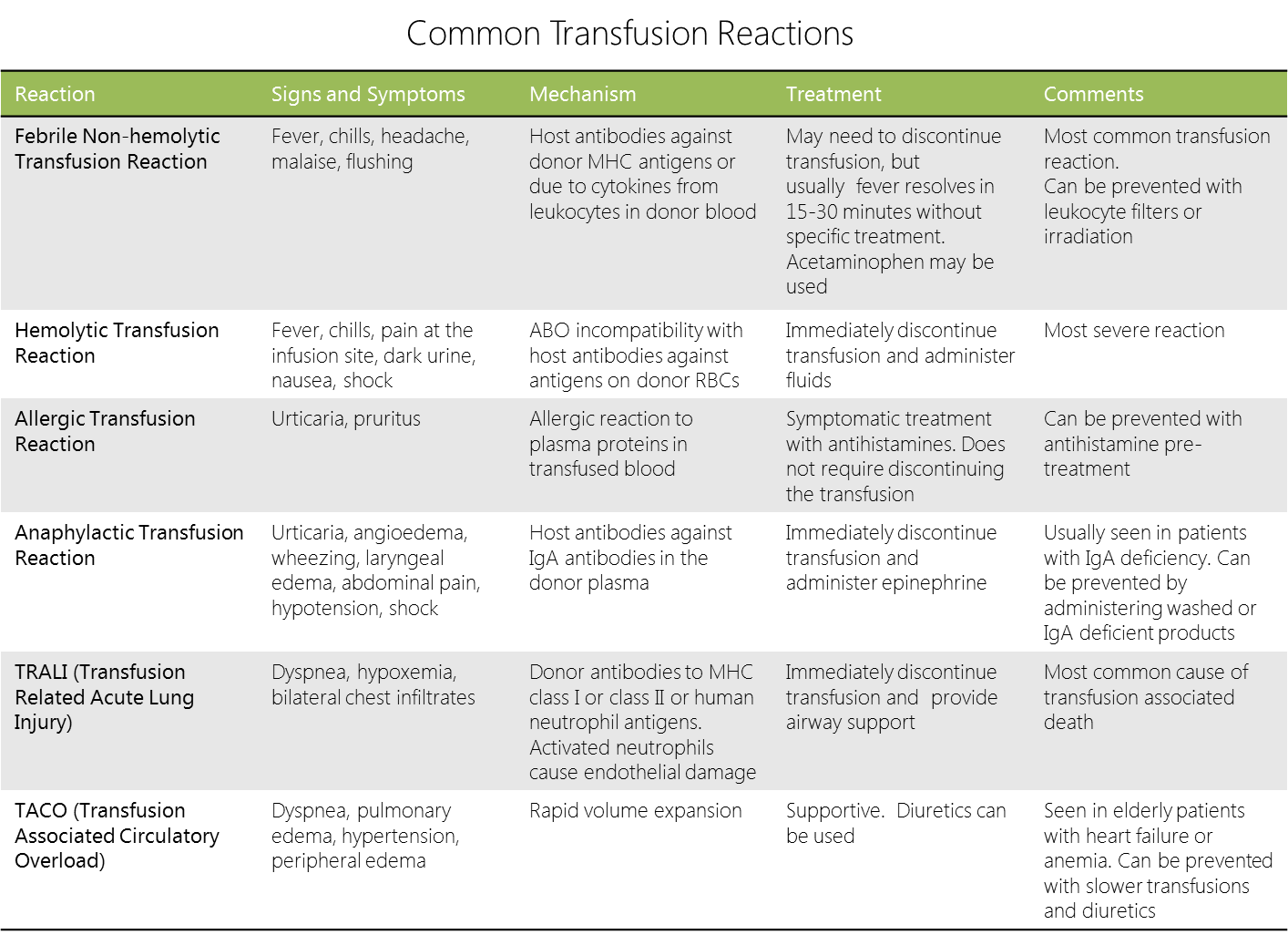
|Explanation=The patient in this scenario most likely presents with a [[febrile nonhemolytic transfusion reaction|febrile nonhemolytic transfusion reaction (FNHTR)]]. Most cases of [[FNHTR]] occur in platelet transfusions. Pathogenesis of the platelet reactions is mediated by cytokines within the product. Cytokines facilitate the reactions, while antibodies are directed against donor leukocytes and HLA antigens. In packed red blood cells, the pathophysiology is believed to be caused by the activation of recipient leukocytes against transfused erythrocytes and the subsequent release of endotoxins, causing fever that is often managed by antipyretics (such as acetaminophen). The use of acetaminophen and diphenhydramine can help minimize the risk of developing [[FNHTR]]. | |Explanation=The patient in this scenario most likely presents with a [[febrile nonhemolytic transfusion reaction|febrile nonhemolytic transfusion reaction (FNHTR)]]. Most cases of [[FNHTR]] occur in platelet transfusions. Pathogenesis of the platelet reactions is mediated by cytokines within the product. Cytokines facilitate the reactions, while antibodies are directed against donor leukocytes and HLA antigens. In packed red blood cells, the pathophysiology is believed to be caused by the activation of recipient leukocytes against transfused erythrocytes and the subsequent release of endotoxins, causing fever that is often managed by antipyretics (such as acetaminophen). The use of acetaminophen and diphenhydramine can help minimize the risk of developing [[FNHTR]]. | ||
[[File:Transfusion_reactions.png|1000px]] | |||
|AnswerA=Formation of IgG and IgA immune complexes that activate the complement pathway and release C3a and C5a | |AnswerA=Formation of IgG and IgA immune complexes that activate the complement pathway and release C3a and C5a | ||
|AnswerAExp= Anaphylactic reaction, usually occurring in patients with IgA deficiency, is caused by formation of immune complexes that activate anaphylaxins, such as C3a and C5a. Patients typically present with features characteristic of anaphylaxis, such as hypotension and shock. | |AnswerAExp=Anaphylactic reaction, usually occurring in patients with IgA deficiency, is caused by formation of immune complexes that activate anaphylaxins, such as C3a and C5a. Patients typically present with features characteristic of anaphylaxis, such as hypotension and shock. | ||
|AnswerB=Reaction caused primarily by the accumulation of cytokines in the platelet products during storage | |AnswerB=Reaction caused primarily by the accumulation of cytokines in the platelet products during storage | ||
|AnswerBExp= See explanation. | |AnswerBExp=See explanation. | ||
|AnswerC=Hypersensitivity reaction against foreign antigens on donor red blood cells | |AnswerC=Hypersensitivity reaction against foreign antigens on donor red blood cells | ||
|AnswerCExp= Acute and delayed hemolytic transfusion reactions, resulting from hypersensitivity reactions against foreign antigens on donor red blood cells, manifest in jaundice, flank pain, and hemoglobinuria. | |AnswerCExp=Acute and delayed hemolytic transfusion reactions, resulting from hypersensitivity reactions against foreign antigens on donor red blood cells, manifest in jaundice, flank pain, and hemoglobinuria. | ||
|AnswerD=Production of IgE by plasma cells following antigen exposure | |AnswerD=Production of IgE by plasma cells following antigen exposure | ||
|AnswerDExp= Following antigen exposure, allergic reaction may result from IgE production by plasma cells. The allergic reaction typically manifest with urticaria, pruritis, and wheezing. | |AnswerDExp=Following antigen exposure, allergic reaction may result from IgE production by plasma cells. The allergic reaction typically manifest with urticaria, pruritis, and wheezing. | ||
|AnswerE=Non-immune circulatory overload due to rapidly incoming transfused blood | |AnswerE=Non-immune circulatory overload due to rapidly incoming transfused blood | ||
|AnswerEExp= Transfusion-associated circulatory overload (TACO) results from the rapid transfusion of blood products. TACO is a non-immune condition, which typically causes high blood pressure, peripheral edema, dyspnea, and orthopnea. | |AnswerEExp=Transfusion-associated circulatory overload (TACO) results from the rapid transfusion of blood products. TACO is a non-immune condition, which typically causes high blood pressure, peripheral edema, dyspnea, and orthopnea. | ||
|EducationalObjectives=[[Febrile nonhemolytic transfusion reaction|Febrile nonhemolytic transfusion reaction (FNHTR)]], characterized by fever and flushing, most frequently occurs following platelet transfusions. | |||
|References=Tenorio GC, Gupte SC, Munker R. Transfusion medicine and immunohematology. in Modern Hematology - Biology and Clinical Management, 2nd ed. 2007. pp:401-432.<br> | |||
Heddle NM. Pathophysiology of febrile nonhemolytic transfusion reactions. Curr Opin Hematol. 1999; 6(6):420-6. | |||
|RightAnswer=B | |RightAnswer=B | ||
|WBRKeyword=transfusion, reaction, hemolytic, hemolysis, nonhemolytic, fever, shock, anaphylaxis, warfarin, gastrointestinal, GI, bleeding, TACO, transfusion, associated, circulatory, overload | |WBRKeyword=transfusion, reaction, hemolytic, hemolysis, nonhemolytic, fever, shock, anaphylaxis, warfarin, gastrointestinal, GI, bleeding, TACO, transfusion, associated, circulatory, overload | ||
|Approved=Yes | |Approved=Yes | ||
}} | }} | ||
Revision as of 16:20, 3 September 2014
| Author | [[PageAuthor::Serge Korjian M.D. (Reviewed by Alison Leibowitz) (Reviewed by Serge Korjian)]] |
|---|---|
| Exam Type | ExamType::USMLE Step 1 |
| Main Category | MainCategory::Immunology |
| Sub Category | SubCategory::Hematology |
| Prompt | [[Prompt::A 67-year-old man presents to the physician's office with complaints of weight loss, fever, and night sweats. Following appropriate work-up,you diagnose him with acute myelogenous leukemia (AML) and start him on scheduled chemotherapy sessions. Three weeks into the treatment, you detect that patient is profoundly thrombocytopenic and requires a platelet transfusion. During the transfusion, the patient develops fever, chills, and intense flushing, but denies any itching or shortness of breath. On physical exam, you find that the patient has a temperature of 38.5 °C (101.3 °F) , heart rate of 108 bpm, respiratory rate of 18/min, and blood pressure of 128/78 mmHg. What is the most likely cause of this patient's reaction to the platelet transfusion?]] |
| Answer A | AnswerA::Formation of IgG and IgA immune complexes that activate the complement pathway and release C3a and C5a |
| Answer A Explanation | [[AnswerAExp::Anaphylactic reaction, usually occurring in patients with IgA deficiency, is caused by formation of immune complexes that activate anaphylaxins, such as C3a and C5a. Patients typically present with features characteristic of anaphylaxis, such as hypotension and shock.]] |
| Answer B | AnswerB::Reaction caused primarily by the accumulation of cytokines in the platelet products during storage |
| Answer B Explanation | AnswerBExp::See explanation. |
| Answer C | AnswerC::Hypersensitivity reaction against foreign antigens on donor red blood cells |
| Answer C Explanation | AnswerCExp::Acute and delayed hemolytic transfusion reactions, resulting from hypersensitivity reactions against foreign antigens on donor red blood cells, manifest in jaundice, flank pain, and hemoglobinuria. |
| Answer D | AnswerD::Production of IgE by plasma cells following antigen exposure |
| Answer D Explanation | AnswerDExp::Following antigen exposure, allergic reaction may result from IgE production by plasma cells. The allergic reaction typically manifest with urticaria, pruritis, and wheezing. |
| Answer E | AnswerE::Non-immune circulatory overload due to rapidly incoming transfused blood |
| Answer E Explanation | AnswerEExp::Transfusion-associated circulatory overload (TACO) results from the rapid transfusion of blood products. TACO is a non-immune condition, which typically causes high blood pressure, peripheral edema, dyspnea, and orthopnea. |
| Right Answer | RightAnswer::B |
| Explanation | [[Explanation::The patient in this scenario most likely presents with a febrile nonhemolytic transfusion reaction (FNHTR). Most cases of FNHTR occur in platelet transfusions. Pathogenesis of the platelet reactions is mediated by cytokines within the product. Cytokines facilitate the reactions, while antibodies are directed against donor leukocytes and HLA antigens. In packed red blood cells, the pathophysiology is believed to be caused by the activation of recipient leukocytes against transfused erythrocytes and the subsequent release of endotoxins, causing fever that is often managed by antipyretics (such as acetaminophen). The use of acetaminophen and diphenhydramine can help minimize the risk of developing FNHTR.
|
| Approved | Approved::Yes |
| Keyword | WBRKeyword::transfusion, WBRKeyword::reaction, WBRKeyword::hemolytic, WBRKeyword::hemolysis, WBRKeyword::nonhemolytic, WBRKeyword::fever, WBRKeyword::shock, WBRKeyword::anaphylaxis, WBRKeyword::warfarin, WBRKeyword::gastrointestinal, WBRKeyword::GI, WBRKeyword::bleeding, WBRKeyword::TACO, WBRKeyword::transfusion, WBRKeyword::associated, WBRKeyword::circulatory, WBRKeyword::overload |
| Linked Question | Linked:: |
| Order in Linked Questions | LinkedOrder:: |