Insulin glargine: Difference between revisions
No edit summary |
No edit summary |
||
| Line 20: | Line 20: | ||
|indication= | |indication= | ||
[[type 1 diabetes mellitus]] and [[type 2 diabetes mellitus]] | [[type 1 diabetes mellitus]] and [[type 2 diabetes mellitus]] | ||
|hasBlackBoxWarning= | |hasBlackBoxWarning= | ||
|adverseReactions= | |adverseReactions= | ||
[[hypoglycemia]], [[allergic reactions]], injection site reactions, [[lipodystrophy]], [[pruritus]], [[rash]], [[edema]] and [[weight gain]] | [[hypoglycemia]], [[allergic reactions]], injection site reactions, [[lipodystrophy]], [[pruritus]], [[rash]], [[edema]] and [[weight gain]] | ||
| Line 46: | Line 46: | ||
*Lantus is indicated to improve glycemic control in adults and pediatric patients with type 1 diabetes mellitus and in adults with type 2 diabetes mellitus. | *Lantus is indicated to improve glycemic control in adults and pediatric patients with type 1 diabetes mellitus and in adults with type 2 diabetes mellitus. | ||
* | *Important limitations of use: | ||
:*Lantus is not recommended for the treatment of diabetic ketoacidosis. intravenous short-acting insulin is the preferred treatment for this condition. | :*Lantus is not recommended for the treatment of diabetic ketoacidosis. intravenous short-acting insulin is the preferred treatment for this condition. | ||
| Line 211: | Line 211: | ||
Table 7 displays the proportion of patients experiencing severe symptomatic hypoglycemia in the Lantus and Standard Care groups in the ORIGIN Trial. | |||
: [[File:{{PAGENAME}}03.png|thumb|none|600px|This image is provided by the National Library of Medicine.]] | |||
*Retinopathy | |||
:*Retinopathy was evaluated in the LANTUS clinical studies by analysis of reported retinal adverse events and fundus photography. The numbers of retinal adverse events reported for LANTUS and NPH insulin treatment groups were similar for patients with type 1 and type 2 diabetes. | |||
:*LANTUS was compared to NPH insulin in a 5-year randomized clinical trial that evaluated the progression of retinopathy as assessed with fundus photography using a grading protocol derived from the Early Treatment Diabetic Retinopathy Scale (ETDRS). Patients had type 2 diabetes (mean age 55 yrs) with no (86%) or mild (14%) retinopathy at baseline. Mean baseline HbA1c was 8.4%. The primary outcome was progression by 3 or more steps on the ETDRS scale at study endpoint. :*Patients with pre-specified post-baseline eye procedures (pan-retinal photocoagulation for proliferative or severe nonproliferative diabetic retinopathy, local photocoagulation for new vessels, and vitrectomy for diabetic retinopathy) were also considered as 3-step progressors regardless of actual change in ETDRS score from baseline. Retinopathy graders were blinded to treatment group assignment. The results for the primary endpoint are shown in Table 8 for both the per-protocol and Intent-to-Treat populations, and indicate similarity of Lantus to NPH in the progression of diabetic retinopathy as assessed by this outcome. | |||
: [[File:{{PAGENAME}}04.png|thumb|none|600px|This image is provided by the National Library of Medicine.]] | |||
*Insulin initiation and intensification of glucose control | |||
:*Intensification or rapid improvement in glucose control has been associated with a transitory, reversible ophthalmologic refraction disorder, worsening of diabetic retinopathy, and acute painful peripheral neuropathy. However, long-term glycemic control decreases the risk of diabetic retinopathy and neuropathy. | |||
*Lipodystrophy | |||
:*Long-term use of insulin, including LANTUS, can cause lipodystrophy at the site of repeated insulin injections. Lipodystrophy includes lipohypertrophy (thickening of adipose tissue) and lipoatrophy (thinning of adipose tissue), and may affect insulin absorption. Rotate insulin injection or infusion sites within the same region to reduce the risk of lipodystrophy. [See Dosage and Administration (2.1)]. | |||
*Weight gain | |||
:*Weight gain can occur with insulin therapy, including LANTUS, and has been attributed to the anabolic effects of insulin and the decrease in glucosuria. | |||
*Peripheral Edema | |||
:*Insulin, including LANTUS, may cause sodium retention and edema, particularly if previously poor metabolic control is improved by intensified insulin therapy. | |||
*Allergic Reactions | |||
:*Local Allergy | |||
:**As with any insulin therapy, patients taking LANTUS may experience injection site reactions, including redness, pain, itching, urticaria, edema, and inflammation. In clinical studies in adult patients, there was a higher incidence of treatment-emergent injection site pain in LANTUS-treated patients (2.7%) compared to NPH insulin-treated patients (0.7%). The reports of pain at the injection site did not result in discontinuation of therapy. | |||
:**Rotation of the injection site within a given area from one injection to the next may help to reduce or prevent these reactions. In some instances, these reactions may be related to factors other than insulin, such as irritants in a skin cleansing agent or poor injection technique. Most minor reactions to insulin usually resolve in a few days to a few weeks. | |||
:*Systemic Allergy | |||
:**Severe, life-threatening, generalized allergy, including anaphylaxis, generalized skin reactions, angioedema, bronchospasm, hypotension, and shock may occur with any insulin, including LANTUS and may be life threatening. | |||
*Antibody production | |||
:*All insulin products can elicit the formation of insulin antibodies. The presence of such insulin antibodies may increase or decrease the efficacy of insulin and may require adjustment of the insulin dose. In phase 3 clinical trials of LANTUS, increases in titers of antibodies to insulin were observed in NPH insulin and insulin glargine treatment groups with similar incidences. | |||
*Cardiovascular Safety | |||
:*The Outcome Reduction with Initial Glargine Intervention trial (i.e., ORIGIN) was an open-label, randomized, 2-by-2, factorial design study. One intervention in ORIGIN compared the effect of LANTUS to standard care on major adverse cardiovascular outcomes in 12,537 participants ≥ 50 years of age with abnormal glucose levels [i.e., impaired fasting glucose (IFG) and/or impaired glucose tolerance (IGT)] or early type 2 diabetes mellitus and established cardiovascular (i.e., CV) disease or CV risk factors at baseline. | |||
:*The objective of the trial was to demonstrate that LANTUS use could significantly lower the risk of major cardiovascular outcomes compared to standard care. Two co-primary composite cardiovascular endpoints were used in ORIGIN. The first co-primary endpoint was the time to first occurrence of a major adverse cardiovascular event defined as the composite of CV death, nonfatal myocardial infarction and nonfatal stroke. The second co-primary endpoint was the time to the first occurrence of CV death or nonfatal myocardial infarction or nonfatal stroke or revascularization procedure or hospitalization for heart failure. | |||
:*Participants were randomized to either LANTUS (N=6264) titrated to a goal fasting plasma glucose of ≤ 95 mg/dL or to standard care (N=6273). Anthropometric and disease characteristics were balanced at baseline. The mean age was 64 years and 8% of participants were 75 years of age or older. The majority of participants were male (65%). Fifty nine percent were Caucasian, 25% were Latin, 10% were Asian and 3% were Black. The median baseline BMI was 29 kg/m2. Approximately 12% of participants had abnormal glucose levels (IGT and/or IFG) at baseline and 88% had type 2 diabetes. For patients with type 2 diabetes, 59% were treated with a single oral antidiabetic drug, 23% had known diabetes but were on no antidiabetic drug and 6% were newly diagnosed during the screening procedure. The mean HbA1c (SD) at baseline was 6.5% (1.0). Fifty nine percent of participants had had a prior cardiovascular event and 39% had documented coronary artery disease or other cardiovascular risk factors. | |||
:*Vital status was available for 99.9% and 99.8% of participants randomized to LANTUS and standard care respectively at end of trial. The median duration of follow-up was 6.2 years [range: 8 days to 7.9 years]. The mean HbA1c (SD) at the end of the trial was 6.5% (1.1) and 6.8% (1.2) in the LANTUS and standard care group respectively. The median dose of LANTUS at end of trial was 0.45 U/kg. Eighty-one percent of patients randomized to LANTUS were using LANTUS at end of the study. The mean change in body weight from baseline to the last treatment visit was 2.2 kg greater in the LANTUS group than in the standard care group. | |||
:*Overall, the incidence of major adverse cardiovascular outcomes was similar between groups (see Table 9). All-cause mortality was also similar between groups. | |||
: [[File:{{PAGENAME}}05.png|thumb|none|600px|This image is provided by the National Library of Medicine.]] | |||
*Cancer | |||
:*In the ORIGIN trial, the overall incidence of cancer (all types combined) or death from cancer (Table 10) was similar between treatment groups. | |||
: [[File:{{PAGENAME}}06.png|thumb|none|600px|This image is provided by the National Library of Medicine.]] | |||
<!--Postmarketing Experience--> | <!--Postmarketing Experience--> | ||
| Line 279: | Line 262: | ||
|postmarketing= | |postmarketing= | ||
*The following adverse reactions have been identified during post-approval use of LANTUS. | |||
*Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to estimate reliably their frequency or establish a causal relationship to drug exposure. | |||
*Medication errors have been reported in which other insulins, particularly short-acting insulins, have been accidentally administered instead of LANTUS [See Patient Counseling Information (17)]. To avoid medication errors between LANTUS and other insulins, patients should be instructed to always verify the insulin label before each injection. | |||
<!--Drug Interactions--> | <!--Drug Interactions--> | ||
Revision as of 15:24, 31 July 2014
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Vignesh Ponnusamy, M.B.B.S. [2]
Disclaimer
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Insulin glargine is a recombinant insulin analog that is FDA approved for the {{{indicationType}}} of type 1 diabetes mellitus and type 2 diabetes mellitus. Common adverse reactions include hypoglycemia, allergic reactions, injection site reactions, lipodystrophy, pruritus, rash, edema and weight gain.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
- Lantus is indicated to improve glycemic control in adults and pediatric patients with type 1 diabetes mellitus and in adults with type 2 diabetes mellitus.
- Important limitations of use:
- Lantus is not recommended for the treatment of diabetic ketoacidosis. intravenous short-acting insulin is the preferred treatment for this condition.
- LANTUS is a recombinant human insulin analog for once daily subcutaneous administration with potency that is approximately the same as the potency of human insulin. LANTUS exhibits a relatively constant glucose-lowering profile over 24 hours that permits once-daily dosing.
- LANTUS may be administered at any time during the day. LANTUS should be administered subcutaneously once a day at the same time every day. The dose of LANTUS must be individualized based on clinical response. Blood glucose monitoring is essential in all patients receiving insulin therapy.
- Patients adjusting the amount or timing of dosing with LANTUS, should only do so under medical supervision with appropriate glucose monitoring [see Warnings and Precautions (5.1).]
- In patients with type 1 diabetes, LANTUS must be used in regimens with short-acting insulin.
- The intended duration of activity of LANTUS is dependent on injection into subcutaneous tissue [see Clinical pharmacology (12.2)]. LANTUS should not be administered intravenously or via an insulin pump. Intravenous administration of the usual subcutaneous dose could result in severe hypoglycemia [see Warnings and Precautions (5.3)].
- As with all insulins, injection sites should be rotated within the same region (abdomen, thigh, or deltoid) from one injection to the next to reduce the risk of lipodystrophy [See Adverse Reactions (6.1)].
- In clinical studies, there was no clinically relevant difference in insulin glargine absorption after abdominal, deltoid, or thigh subcutaneous administration. As for all insulins, the rate of absorption, and consequently the onset and duration of action, may be affected by exercise and other variables, such as stress, intercurrent illness, or changes in co-administered drugs or meal patterns.
- Initiation of LANTUS therapy
- The recommended starting dose of LANTUS in patients with type 1 diabetes should be approximately one-third of the total daily insulin requirements. Short-acting, premeal insulin should be used to satisfy the remainder of the daily insulin requirements.
- The recommended starting dose of LANTUS in patients with type 2 diabetes who are not currently treated with insulin is 10 units (or 0.2 Units/kg) once daily, which should subsequently be adjusted to the patient's needs.
- The dose of LANTUS should be adjusted according to blood glucose measurements. The dosage of LANTUS should be individualized under the supervision of a healthcare provider in accordance with the needs of the patient.
- Converting to LANTUS from other insulin therapies
- If changing from a treatment regimen with an intermediate-or long-acting insulin to a regimen with LANTUS, the amount and timing of shorter-acting insulins and doses of any oral anti-diabetic drugs may need to be adjusted.
- If transferring patients from once-daily NPH insulin to once-daily LANTUS, the recommended initial LANTUS dose is the same as the dose of NPH that is being discontinued.
- If transferring patients from twice-daily NPH insulin to once-daily LANTUS, the recommended initial LANTUS dose is 80% of the total NPH dose that is being discontinued. This dose reduction will lower the likelihood of hypoglycemia [see Warnings and Precautions (5.3)].
- Dosage Forms And Strengths
- LANTUS solution for injection 100 Units per mL is available as:
- 10 mL Vial (1000 Units/10 mL)
- 3 mL SoloStar® disposable insulin device (300 Units/3 mL)
- LANTUS solution for injection 100 Units per mL is available as:
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
Condition1
- Developed by:
- Class of Recommendation:
- Strength of Evidence:
- Dosing Information
- Dosage
Condition2
There is limited information regarding Off-Label Guideline-Supported Use of Insulin glargine in adult patients.
Non–Guideline-Supported Use
Condition1
- Dosing Information
- Dosage
Condition2
There is limited information regarding Off-Label Non–Guideline-Supported Use of Insulin glargine in adult patients.
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
Condition1
- Dosing Information
- Dosage
Condition2
There is limited information regarding FDA-Labeled Use of Insulin glargine in pediatric patients.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
Condition1
- Developed by:
- Class of Recommendation:
- Strength of Evidence:
- Dosing Information
- Dosage
Condition2
There is limited information regarding Off-Label Guideline-Supported Use of Insulin glargine in pediatric patients.
Non–Guideline-Supported Use
Condition1
- Dosing Information
- Dosage
Condition2
There is limited information regarding Off-Label Non–Guideline-Supported Use of Insulin glargine in pediatric patients.
Contraindications
- Condition1
Warnings
- Description
Precautions
- Description
- Hypoglycemia
- Hypoglycemia is the most common adverse reaction of insulin, including LANTUS. The risk of hypoglycemia increases with intensive glycemic control. Patients must be educated to recognize and manage hypoglycemia. Severe hypoglycemia can lead to unconsciousness or convulsions and may result in temporary or permanent impairment of brain function or death. Severe hypoglycemia requiring the assistance of another person or parenteral glucose infusion or glucagon administration has been observed in clinical trials with insulin, including trials with LANTUS.
- The timing of hypoglycemia usually reflects the time-action profile of the administered insulin formulations. Other factors such as changes in food intake (e.g., amount of food or timing of meals), exercise, and concomitant medications may also alter the risk of hypoglycemia [See Drug Interactions (7)].
- The prolonged effect of subcutaneous LANTUS may delay recovery from hypoglycemia. Patients being switched from twice daily NPH insulin to once-daily LANTUS should have their initial LANTUS dose reduced by 20% from the previous total daily NPH dose to reduce the risk of hypoglycemia.
- As with all insulins, use caution in patients with hypoglycemia unawareness and in patients who may be predisposed to hypoglycemia (e.g., the pediatric population and patients who fast or have erratic food intake). The patient's ability to concentrate and react may be impaired as a result of hypoglycemia. This may present a risk in situations where these abilities are especially important, such as driving or operating other machinery.
- Early warning symptoms of hypoglycemia may be different or less pronounced under certain conditions, such as longstanding diabetes, diabetic neuropathy, use of medications such as beta-blockers, or intensified glycemic control. These situations may result in severe hypoglycemia (and, possibly, loss of consciousness) prior to the patient's awareness of hypoglycemia.
- Hypersensitivity and allergic reactions
- Severe, life-threatening, generalized allergy, including anaphylaxis, can occur with insulin products, including LANTUS.
Adverse Reactions
Clinical Trials Experience
- Because clinical trials are conducted under widely varying designs, the adverse reaction rates reported in one clinical trial may not be easily compared to those rates reported in another clinical trial, and may not reflect the rates actually observed in clinical practice.
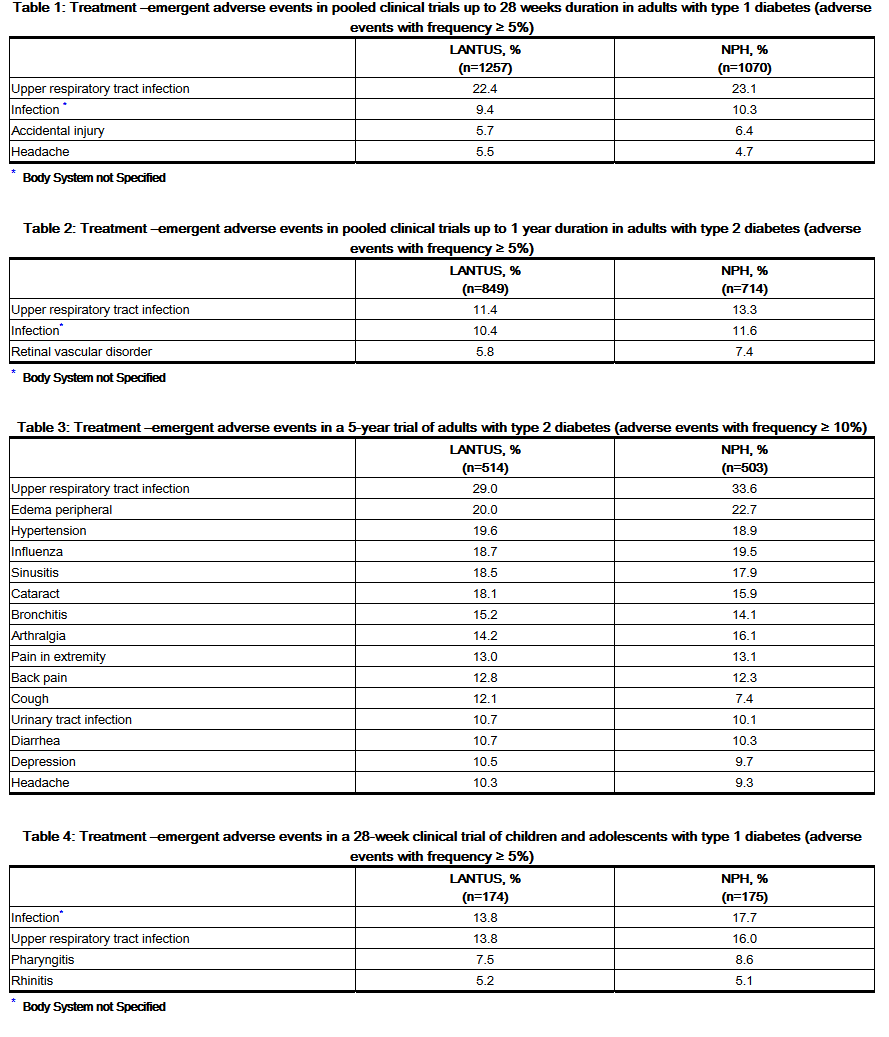
- The frequencies of treatment-emergent adverse events during LANTUS clinical trials in patients with type 1 diabetes mellitus and type 2 diabetes mellitus are listed in the tables below.
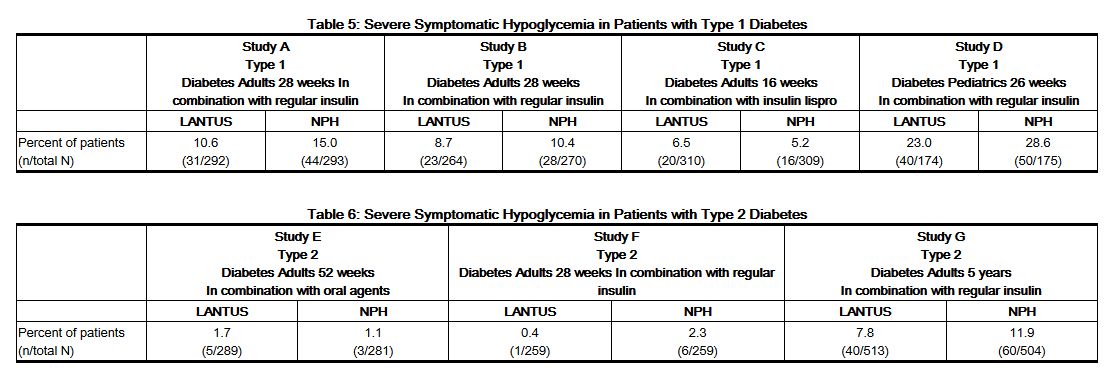
- Severe Hypoglycemia
- Hypoglycemia is the most commonly observed adverse reaction in patients using insulin, including LANTUS [See Warnings and Precautions (5.3)]. Tables 5, and 6 and 7 summarize the incidence of severe hypoglycemia in the LANTUS individual clinical trials. Severe symptomatic hypoglycemia was defined as an event with symptoms consistent with hypoglycemia requiring the assistance of another person and associated with either a blood glucose below 50 mg/dL (≤56 mg/dL in the 5-year trial and ≤36 mg/dL in the ORIGIN trial) or prompt recovery after oral carbohydrate, intravenous glucose or glucagon administration.
- The proportion of patients experiencing severe symptomatic hypoglycemia in the LANTUS clinical trials [See Clinical Studies (14)] in adults with type 1 diabetes and type 2 diabetes were comparable for all treatment regimens (see Tables 5 and 6). In the pediatric phase 3 clinical trial, children and adolescents with type 1 diabetes had a higher incidence of severe symptomatic hypoglycemia in the two treatment groups compared to the adult trials with type 1 diabetes.
Table 7 displays the proportion of patients experiencing severe symptomatic hypoglycemia in the Lantus and Standard Care groups in the ORIGIN Trial.
- Retinopathy
- Retinopathy was evaluated in the LANTUS clinical studies by analysis of reported retinal adverse events and fundus photography. The numbers of retinal adverse events reported for LANTUS and NPH insulin treatment groups were similar for patients with type 1 and type 2 diabetes.
- LANTUS was compared to NPH insulin in a 5-year randomized clinical trial that evaluated the progression of retinopathy as assessed with fundus photography using a grading protocol derived from the Early Treatment Diabetic Retinopathy Scale (ETDRS). Patients had type 2 diabetes (mean age 55 yrs) with no (86%) or mild (14%) retinopathy at baseline. Mean baseline HbA1c was 8.4%. The primary outcome was progression by 3 or more steps on the ETDRS scale at study endpoint. :*Patients with pre-specified post-baseline eye procedures (pan-retinal photocoagulation for proliferative or severe nonproliferative diabetic retinopathy, local photocoagulation for new vessels, and vitrectomy for diabetic retinopathy) were also considered as 3-step progressors regardless of actual change in ETDRS score from baseline. Retinopathy graders were blinded to treatment group assignment. The results for the primary endpoint are shown in Table 8 for both the per-protocol and Intent-to-Treat populations, and indicate similarity of Lantus to NPH in the progression of diabetic retinopathy as assessed by this outcome.
- Insulin initiation and intensification of glucose control
- Intensification or rapid improvement in glucose control has been associated with a transitory, reversible ophthalmologic refraction disorder, worsening of diabetic retinopathy, and acute painful peripheral neuropathy. However, long-term glycemic control decreases the risk of diabetic retinopathy and neuropathy.
- Lipodystrophy
- Long-term use of insulin, including LANTUS, can cause lipodystrophy at the site of repeated insulin injections. Lipodystrophy includes lipohypertrophy (thickening of adipose tissue) and lipoatrophy (thinning of adipose tissue), and may affect insulin absorption. Rotate insulin injection or infusion sites within the same region to reduce the risk of lipodystrophy. [See Dosage and Administration (2.1)].
- Weight gain
- Weight gain can occur with insulin therapy, including LANTUS, and has been attributed to the anabolic effects of insulin and the decrease in glucosuria.
- Peripheral Edema
- Insulin, including LANTUS, may cause sodium retention and edema, particularly if previously poor metabolic control is improved by intensified insulin therapy.
- Allergic Reactions
- Local Allergy
- As with any insulin therapy, patients taking LANTUS may experience injection site reactions, including redness, pain, itching, urticaria, edema, and inflammation. In clinical studies in adult patients, there was a higher incidence of treatment-emergent injection site pain in LANTUS-treated patients (2.7%) compared to NPH insulin-treated patients (0.7%). The reports of pain at the injection site did not result in discontinuation of therapy.
- Rotation of the injection site within a given area from one injection to the next may help to reduce or prevent these reactions. In some instances, these reactions may be related to factors other than insulin, such as irritants in a skin cleansing agent or poor injection technique. Most minor reactions to insulin usually resolve in a few days to a few weeks.
- Local Allergy
- Systemic Allergy
- Severe, life-threatening, generalized allergy, including anaphylaxis, generalized skin reactions, angioedema, bronchospasm, hypotension, and shock may occur with any insulin, including LANTUS and may be life threatening.
- Systemic Allergy
- Antibody production
- All insulin products can elicit the formation of insulin antibodies. The presence of such insulin antibodies may increase or decrease the efficacy of insulin and may require adjustment of the insulin dose. In phase 3 clinical trials of LANTUS, increases in titers of antibodies to insulin were observed in NPH insulin and insulin glargine treatment groups with similar incidences.
- Cardiovascular Safety
- The Outcome Reduction with Initial Glargine Intervention trial (i.e., ORIGIN) was an open-label, randomized, 2-by-2, factorial design study. One intervention in ORIGIN compared the effect of LANTUS to standard care on major adverse cardiovascular outcomes in 12,537 participants ≥ 50 years of age with abnormal glucose levels [i.e., impaired fasting glucose (IFG) and/or impaired glucose tolerance (IGT)] or early type 2 diabetes mellitus and established cardiovascular (i.e., CV) disease or CV risk factors at baseline.
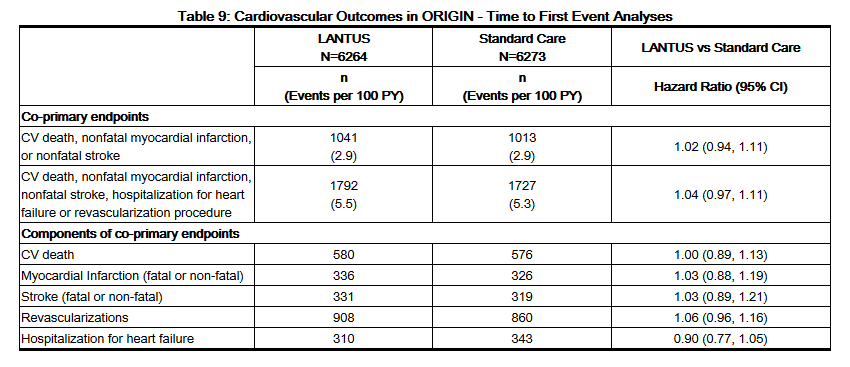
- The objective of the trial was to demonstrate that LANTUS use could significantly lower the risk of major cardiovascular outcomes compared to standard care. Two co-primary composite cardiovascular endpoints were used in ORIGIN. The first co-primary endpoint was the time to first occurrence of a major adverse cardiovascular event defined as the composite of CV death, nonfatal myocardial infarction and nonfatal stroke. The second co-primary endpoint was the time to the first occurrence of CV death or nonfatal myocardial infarction or nonfatal stroke or revascularization procedure or hospitalization for heart failure.
- Participants were randomized to either LANTUS (N=6264) titrated to a goal fasting plasma glucose of ≤ 95 mg/dL or to standard care (N=6273). Anthropometric and disease characteristics were balanced at baseline. The mean age was 64 years and 8% of participants were 75 years of age or older. The majority of participants were male (65%). Fifty nine percent were Caucasian, 25% were Latin, 10% were Asian and 3% were Black. The median baseline BMI was 29 kg/m2. Approximately 12% of participants had abnormal glucose levels (IGT and/or IFG) at baseline and 88% had type 2 diabetes. For patients with type 2 diabetes, 59% were treated with a single oral antidiabetic drug, 23% had known diabetes but were on no antidiabetic drug and 6% were newly diagnosed during the screening procedure. The mean HbA1c (SD) at baseline was 6.5% (1.0). Fifty nine percent of participants had had a prior cardiovascular event and 39% had documented coronary artery disease or other cardiovascular risk factors.
- Vital status was available for 99.9% and 99.8% of participants randomized to LANTUS and standard care respectively at end of trial. The median duration of follow-up was 6.2 years [range: 8 days to 7.9 years]. The mean HbA1c (SD) at the end of the trial was 6.5% (1.1) and 6.8% (1.2) in the LANTUS and standard care group respectively. The median dose of LANTUS at end of trial was 0.45 U/kg. Eighty-one percent of patients randomized to LANTUS were using LANTUS at end of the study. The mean change in body weight from baseline to the last treatment visit was 2.2 kg greater in the LANTUS group than in the standard care group.
- Overall, the incidence of major adverse cardiovascular outcomes was similar between groups (see Table 9). All-cause mortality was also similar between groups.
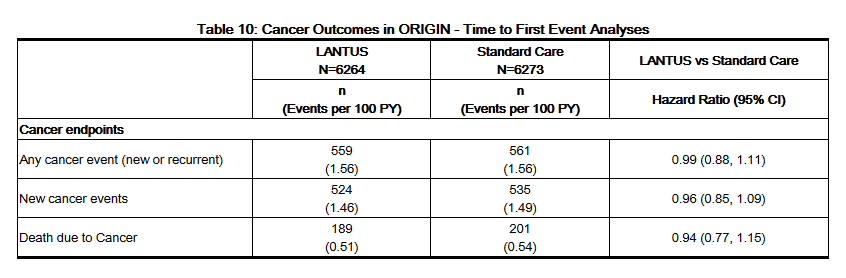
- Cancer
- In the ORIGIN trial, the overall incidence of cancer (all types combined) or death from cancer (Table 10) was similar between treatment groups.
Postmarketing Experience
- The following adverse reactions have been identified during post-approval use of LANTUS.
- Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to estimate reliably their frequency or establish a causal relationship to drug exposure.
- Medication errors have been reported in which other insulins, particularly short-acting insulins, have been accidentally administered instead of LANTUS [See Patient Counseling Information (17)]. To avoid medication errors between LANTUS and other insulins, patients should be instructed to always verify the insulin label before each injection.
Drug Interactions
- Drug
- Description
Use in Specific Populations
Pregnancy
- Pregnancy Category
- Australian Drug Evaluation Committee (ADEC) Pregnancy Category
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Insulin glargine in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Insulin glargine during labor and delivery.
Nursing Mothers
There is no FDA guidance on the use of Insulin glargine with respect to nursing mothers.
Pediatric Use
There is no FDA guidance on the use of Insulin glargine with respect to pediatric patients.
Geriatic Use
There is no FDA guidance on the use of Insulin glargine with respect to geriatric patients.
Gender
There is no FDA guidance on the use of Insulin glargine with respect to specific gender populations.
Race
There is no FDA guidance on the use of Insulin glargine with respect to specific racial populations.
Renal Impairment
There is no FDA guidance on the use of Insulin glargine in patients with renal impairment.
Hepatic Impairment
There is no FDA guidance on the use of Insulin glargine in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Insulin glargine in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Insulin glargine in patients who are immunocompromised.
Administration and Monitoring
Administration
- Oral
- Intravenous
Monitoring
There is limited information regarding Monitoring of Insulin glargine in the drug label.
- Description
IV Compatibility
There is limited information regarding IV Compatibility of Insulin glargine in the drug label.
Overdosage
Acute Overdose
Signs and Symptoms
- Description
Management
- Description
Chronic Overdose
There is limited information regarding Chronic Overdose of Insulin glargine in the drug label.
Pharmacology
There is limited information regarding Insulin glargine Pharmacology in the drug label.
Mechanism of Action
Structure
Pharmacodynamics
There is limited information regarding Pharmacodynamics of Insulin glargine in the drug label.
Pharmacokinetics
There is limited information regarding Pharmacokinetics of Insulin glargine in the drug label.
Nonclinical Toxicology
There is limited information regarding Nonclinical Toxicology of Insulin glargine in the drug label.
Clinical Studies
There is limited information regarding Clinical Studies of Insulin glargine in the drug label.
How Supplied
Storage
There is limited information regarding Insulin glargine Storage in the drug label.
Images
Drug Images
{{#ask: Page Name::Insulin glargine |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Insulin glargine |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
There is limited information regarding Patient Counseling Information of Insulin glargine in the drug label.
Precautions with Alcohol
- Alcohol-Insulin glargine interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
- ®[1]
Look-Alike Drug Names
- A® — B®[2]
Drug Shortage Status
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
- ↑ Empty citation (help)
- ↑ "http://www.ismp.org". External link in
|title=(help)
{{#subobject:
|Page Name=Insulin glargine |Pill Name=No image.jpg |Drug Name= |Pill Ingred=|+sep=; |Pill Imprint= |Pill Dosage= |Pill Color=|+sep=; |Pill Shape= |Pill Size (mm)= |Pill Scoring= |Pill Image= |Drug Author= |NDC=
}}
{{#subobject:
|Label Page=Insulin glargine |Label Name=Insulin glargine11.png
}}
{{#subobject:
|Label Page=Insulin glargine |Label Name=Insulin glargine11.png
}}