Thyrotropin alpha
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Ammu Susheela, M.D. [2]
Disclaimer
WikiDoc MAKES NO GUARANTEE OF VALIDITY. WikiDoc is not a professional health care provider, nor is it a suitable replacement for a licensed healthcare provider. WikiDoc is intended to be an educational tool, not a tool for any form of healthcare delivery. The educational content on WikiDoc drug pages is based upon the FDA package insert, National Library of Medicine content and practice guidelines / consensus statements. WikiDoc does not promote the administration of any medication or device that is not consistent with its labeling. Please read our full disclaimer here.
Overview
Thyrotropin alpha is an hormone analog that is FDA approved for the treatment of well differentiated thyroid cancer. Common adverse reactions include nausea, vomiting, headache, paresthesia.
Adult Indications and Dosage
FDA-Labeled Indications and Dosage (Adult)
Adjunctive Diagnostic Tool for Serum Thyroglobulin Testing in Well Differentiated Thyroid Cancer
- THYROGEN® is indicated for use as an adjunctive diagnostic tool for serum thyroglobulin (Tg) testing with or without radioiodine imaging in the follow-up of patients with well-differentiated thyroid cancer who have previously undergone thyroidectomy.
Limitations of Use
- THYROGEN-stimulated Tg levels are generally lower than, and do not correlate with, Tg levels after thyroid hormone withdrawal.
- Even when THYROGEN-stimulated Tg testing is performed in combination with radioiodine imaging, there remains a risk of missing a diagnosis of thyroid cancer or of underestimating the extent of disease.
- Anti-Tg antibodies may confound the Tg assay and render Tg levels uninterpretable. Therefore, in such cases, even with a negative or low-stage THYROGEN radioiodine scan, consideration should be given to further evaluating patients.
Adjunct to Treatment for Ablation in Well Differentiated Thyroid Cancer
- THYROGEN is indicated for use as an adjunctive treatment for radioiodine ablation of thyroid tissue remnants in patients who have undergone a near-total or total thyroidectomy for well-differentiated thyroid cancer and who do not have evidence of distant metastatic thyroid cancer.
Limitations of Use
- The effect of THYROGEN on long-term thyroid cancer outcomes has not been determined. Due to the relatively small clinical experience with THYROGEN in remnant ablation, it is not possible to conclude whether long-term thyroid cancer outcomes would be equivalent after use of THYROGEN or use of thyroid hormone withholding for TSH elevation prior to remnant ablation.
Recommended Dosage
- THYROGEN should be used by physicians knowledgeable in the management of patients with thyroid cancer.
- THYROGEN is indicated as a two-injection regimen. The recommended dosage of THYROGEN is a 0.9 mg intramuscular injection to the buttock followed by a second 0.9 mg intramuscular injection to the buttock 24 hours later.
- THYROGEN should be administered intramuscularly only. THYROGEN should not be administered intravenously.
- Pretreatment with glucocorticoids should be considered for patients in whom tumor expansion may compromise vital anatomic structures.
- Routine measurement of serum TSH levels is not recommended after THYROGEN use.
Reconstitution, Preparation, and Administration of THYROGEN
- The supplied lyophilized powder must be reconstituted with Sterile Water for Injection. THYROGEN should be prepared, and administered in the following manner:
- Add 1.2 mL of Sterile Water for Injection to the vial containing the THYROGEN lyophilized powder.
- Swirl the contents of the vial until all the material is dissolved. Do not shake the solution. The reconstituted THYROGEN solution has a concentration of 0.9 mg of thyrotropin alfa per mL.
- Visually inspect the reconstituted solution for particulate matter and discoloration prior to administration. The reconstituted THYROGEN solution should be clear and colorless. Do not use if the solution has particulate matter or is cloudy or discolored.
- Withdraw 1 mL of the reconstituted THYROGEN solution (0.9 mg of thyrotropin alfa) and inject intramuscularly in the buttocks.
- The reconstituted THYROGEN solution must be injected within 3 hours unless refrigerated; if refrigerated, the reconstituted solution may be kept for up to 24 hours.
- Discard unused portions. Do not mix with other substances.
Timing of Serum Thyroglobulin Testing Following THYROGEN Administration
- For serum thyroglobulin testing, the serum sample should be obtained 72 hours after the final injection of THYROGEN.
Timing for Remnant Ablation and Diagnostic Scanning Following THYROGEN Administration
- Oral radioiodine should be given 24 hours after the second injection of THYROGEN in both remnant ablation and diagnostic scanning. The activity of 131I is carefully selected at the discretion of the nuclear medicine physician.
- Diagnostic scanning should be performed 48 hours after the radioiodine administration.
Off-Label Use and Dosage (Adult)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Thyrotropin alpha in adult patients.
Non–Guideline-Supported Use
Pediatric Indications and Dosage
FDA-Labeled Indications and Dosage (Pediatric)
There is limited information regarding FDA-Labeled Use of Thyrotropin alpha in pediatric patients.
Off-Label Use and Dosage (Pediatric)
Guideline-Supported Use
There is limited information regarding Off-Label Guideline-Supported Use of Thyrotropin alpha in pediatric patients.
Non–Guideline-Supported Use
There is limited information regarding Off-Label Non–Guideline-Supported Use of Thyrotropin alpha in pediatric patients.
Contraindications
- None
Warnings
THYROGEN-induced Hyperthyroidism
- When given to patients who have substantial thyroid tissue still in situ or functional thyroid cancer metastases, THYROGEN is known to cause a transient (over 7 to 14 days) but significant rise in serum thyroid hormone concentration. There have been reports of death in non-thyroidectomized patients and in patients with distant metastatic thyroid cancer in which events leading to death occurred within 24 hours after administration of THYROGEN. Patients with residual thyroid tissue at risk for THYROGEN-induced hyperthyroidism include the elderly and those with a known history of heart disease. Hospitalization for administration of THYROGEN and post-administration observation in patients at risk should be considered.
Stroke
- There are postmarketing reports of radiologically-confirmed stroke and neurological findings suggestive of stroke unconfirmed radiologically (e.g., unilateral weakness) occurring within 72 hours (range 20 minutes to three days) of THYROGEN administration in patients without known central nervous system metastases. The majority of such patients were young women taking oral contraceptives at the time of their event or had other risk factors for stroke, such as smoking or a history of migraine headaches. The relationship between THYROGEN administration and stroke is unknown. Patients should be well-hydrated prior to treatment with THYROGEN.
Sudden Rapid Tumor Enlargement
- Sudden, rapid and painful enlargement of residual thyroid tissue or distant metastases can occur following treatment with THYROGEN. This may lead to acute symptoms, which depend on the anatomical location of the tissue. Such symptoms include acute hemiplegia, hemiparesis, and loss of vision one to three days after THYROGEN administration. Laryngeal edema, pain at the site of distant metastasis, and respiratory distress requiring tracheotomy have also been reported after THYROGEN administration.
- Pretreatment with glucocorticoids should be considered for patients in whom tumor expansion may compromise vital anatomic structures.
Adverse Reactions
Clinical Trials Experience
- Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
- The data described below reflect exposure to THYROGEN in 481 thyroid cancer patients who participated in a total of 6 clinical trials of THYROGEN: 4 trials for diagnostic use and 2 trials for ablation. In clinical trials, patients had undergone near-total thyroidectomy and had a mean age of 46.1 years. Thyroid cancer diagnosis was as follows: papillary (69.2%), follicular (12.9%), Hurthle cell (2.3%) and papillary/follicular 15.6%. Most patients received 2 intramuscular injections of 0.9 mg of THYROGEN injection given 24 hours apart.
- The safety profile of patients who have undergone thyroidectomy and received THYROGEN as adjunctive treatment for radioiodine ablation of thyroid tissue remnants for well-differentiated thyroid cancer did not differ from that of patients who received THYROGEN for diagnostic purposes.
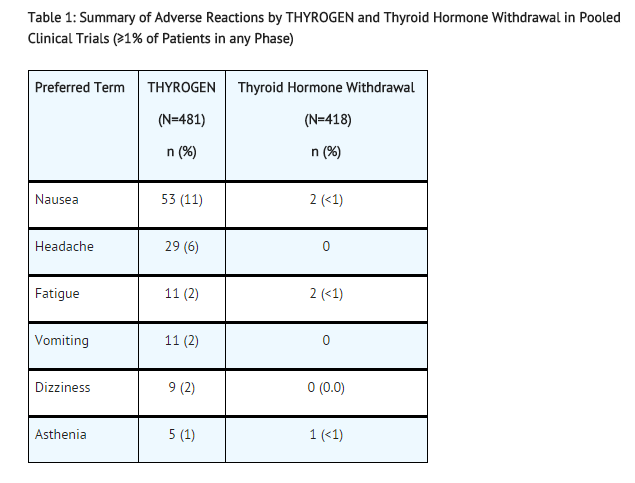
- Reactions reported in ≥ 1% of patients in the combined trials are summarized in Table 1. In some studies, an individual patient may have participated in both THYROGEN and thyroid hormone withdrawal.
- Table 1: Summary of Adverse Reactions by THYROGEN and Thyroid Hormone Withdrawal in Pooled Clinical Trials (≥1% of Patients in any Phase)
Postmarketing Experience
THYROGEN-induced Hyperthyroidism
- When given to patients who have substantial thyroid tissue still in situ or functional thyroid cancer metastases, THYROGEN is known to cause a transient (over 7 to 14 days) but significant rise in serum thyroid hormone concentration. There have been reports of death in non-thyroidectomized patients and in patients with distant metastatic thyroid cancer in which events leading to death occurred within 24 hours after administration of THYROGEN. Patients with residual thyroid tissue at risk for THYROGEN-induced hyperthyroidism include the elderly and those with a known history of heart disease. Hospitalization for administration of THYROGEN and post-administration observation in patients at risk should be considered.
Stroke
- There are postmarketing reports of radiologically-confirmed stroke and neurological findings suggestive of stroke unconfirmed radiologically (e.g., unilateral weakness) occurring within 72 hours (range 20 minutes to three days) of THYROGEN administration in patients without known central nervous system metastases. The majority of such patients were young women taking oral contraceptives at the time of their event or had other risk factors for stroke, such as smoking or a history of migraine headaches. The relationship between THYROGEN administration and stroke is unknown. Patients should be well-hydrated prior to treatment with THYROGEN.
Sudden Rapid Tumor Enlargement
- Sudden, rapid and painful enlargement of residual thyroid tissue or distant metastases can occur following treatment with THYROGEN. This may lead to acute symptoms, which depend on the anatomical location of the tissue. Such symptoms include acute hemiplegia, hemiparesis, and loss of vision one to three days after THYROGEN administration. Laryngeal edema, pain at the site of distant metastasis, and respiratory distress requiring tracheotomy have also been reported after THYROGEN administration.
- Pretreatment with glucocorticoids should be considered for patients in whom tumor expansion may compromise vital anatomic structures.
Drug Interactions
There is limited information regarding Thyrotropin alpha Drug Interactions in the drug label.
Use in Specific Populations
Pregnancy
- Animal reproduction studies have not been conducted with THYROGEN.
- It is also not known whether THYROGEN can cause fetal harm when administered to a pregnant woman or can affect reproductive capacity. THYROGEN should be given to a pregnant woman only if clearly needed.
- Australian Drug Evaluation Committee (ADEC) Pregnancy Category
There is no Australian Drug Evaluation Committee (ADEC) guidance on usage of Thyrotropin alpha in women who are pregnant.
Labor and Delivery
There is no FDA guidance on use of Thyrotropin alpha during labor and delivery.
Nursing Mothers
There is no FDA guidance on the use of Thyrotropin alpha with respect to nursing mothers.
Pediatric Use
There is no FDA guidance on the use of Thyrotropin alpha with respect to pediatric patients.
Geriatic Use
- In pooled clinical studies of THYROGEN, 60 patients (12%) were >65 years, and 421 (88%) were ≤ 65 years of age. Results from controlled trials do not indicate a difference in the safety and efficacy of THYROGEN between adult patients less than 65 years and those over 65 years of age.
Gender
There is no FDA guidance on the use of Thyrotropin alpha with respect to specific gender populations.
Race
There is no FDA guidance on the use of Thyrotropin alpha with respect to specific racial populations.
Renal Impairment
Elimination of THYROGEN is significantly slower in dialysis-dependent end stage renal disease (ESRD) patients, resulting in prolonged elevation of TSH levels.
Hepatic Impairment
There is no FDA guidance on the use of Thyrotropin alpha in patients with hepatic impairment.
Females of Reproductive Potential and Males
There is no FDA guidance on the use of Thyrotropin alpha in women of reproductive potentials and males.
Immunocompromised Patients
There is no FDA guidance one the use of Thyrotropin alpha in patients who are immunocompromised.
Administration and Monitoring
Administration
Monitoring
There is limited information regarding Monitoring of Thyrotropin alpha in the drug label.
IV Compatibility
There is limited information regarding IV Compatibility of Thyrotropin alpha in the drug label.
Overdosage
- In clinical trials of THYROGEN, three patients experienced symptoms after receiving THYROGEN doses higher than those recommended. Two patients had nausea after a 2.7 mg IM dose (3 times the recommended dose), and in one of these patients, the event was accompanied by weakness, dizziness and headache.
- Another patient experienced nausea, vomiting and hot flashes after a 3.6 mg IM dose (4 times the recommended dose). There is no specific therapy for THYROGEN overdose. Supportive care is recommended.
Pharmacology
There is limited information regarding Thyrotropin alpha Pharmacology in the drug label.
Mechanism of Action
- Thyrotropin (TSH) is a pituitary hormone that stimulates the thyroid gland to produce thyroid hormone. Binding of thyrotropin alfa to TSH receptors on normal thyroid epithelial cells or on well-differentiated thyroid cancer tissue stimulates iodine uptake and organification, and synthesis and secretion of thyroglobulin (Tg), triiodothyronine (T3) and thyroxine (T4).
- The effect of thyroid stimulating hormone activation of thyroid cells is to increase uptake of radioiodine to allow scan detection or radioiodine killing of thyroid cells. TSH activation also leads to the release of thyroglobulin by thyroid cells. Thyroglobulin functions as a tumor marker which is detected in blood specimens.
Structure
- Each vial of THYROGEN contains 1.1 mg thyrotropin alfa, 36 mg Mannitol, 5.1 mg Sodium Phosphate, and 2.4 mg Sodium Chloride.
- THYROGEN (thyrotropin alfa for injection) contains recombinant human thyroid stimulating hormone (TSH). Thyrotropin alfa is synthesized in a genetically modified Chinese hamster ovary cell line.
- Thyrotropin alfa is a heterodimeric glycoprotein comprised of two non-covalently linked subunits, an alpha subunit of 92 amino acid residues containing two N-linked glycosylation sites and a beta subunit of 118 residues containing one N-linked glycosylation site. The amino acid sequence of thyrotropin alfa is identical to that of human pituitary TSH.
- Both thyrotropin alfa and naturally occurring human pituitary TSH are synthesized as a mixture of glycosylation variants. Unlike pituitary TSH, which is secreted as a mixture of sialylated and sulfated forms, thyrotropin alfa is sialylated but not sulfated. The biological activity of thyrotropin alfa is determined by a cell-based bioassay. In this assay, cells expressing a functional TSH receptor and a cAMP-responsive element coupled to a heterologous reporter gene, luciferase, enable the measurement of thyrotropin alfa activity by measuring the luciferase response. The specific activity of thyrotropin alfa is determined relative to an internal Genzyme reference standard that was calibrated against the World Health Organization (WHO) human TSH reference standard.
Pharmacodynamics
There is limited information regarding Pharmacodynamics of Thyrotropin alpha in the drug label.
Pharmacokinetics
- The pharmacokinetics of THYROGEN were studied in 16 patients with well-differentiated thyroid cancer given a single 0.9 mg IM dose. Mean peak serum TSH concentrations of 116 ± 38 mU/L were reached between 3 and 24 hours after injection (median of 10 hours). The mean apparent elimination half-life was 25 ± 10 hours. The organ(s) of TSH clearance in man have not been identified, but studies of pituitary-derived TSH suggest the involvement of the liver and kidneys.
Nonclinical Toxicology
Carcinogenesis, Mutagenesis, Impairment of Fertility
- Long-term toxicity studies in animals have not been performed with THYROGEN to evaluate the carcinogenic potential of the drug. THYROGEN was not mutagenic in the bacterial reverse mutation assay. Studies have not been performed with THYROGEN to evaluate the effects on fertility.
Animal Pharmacology and/or Toxicology
- Four toxicology studies, two in rodents and two in primates, have been conducted using both single and repeated daily injections of thyrotropin alfa. In a single-dose study utilizing male and female rats bolus injections were given at levels up to 7.14 IU/kg (equivalent to 50 times the expected single human dose). There were no effects, either gross or microscopic, in this study which could be attributed to the administration of thyrotropin alfa. In a repeated-dose study, rats were given thyrotropin alfa in the form of 5 daily intramuscular injections at levels up to 1.43 IU/kg (equivalent to 10 times the expected single human dose) without dose-related toxic effects observed.
- A single-dose study in male and female cynomolgus monkeys used single intramuscular injections of thyrotropin alfa at levels equivalent to the expected dose and 0.25 and 4 times the expected single human dose. There were no changes that were regarded as indicative of an adverse or toxic response to thyrotropin alfa. Cynomolgus monkeys were also administered thyrotropin alfa as three consecutive daily bolus intramuscular injections at levels extending to 4 times the dose in humans. There were no changes that are considered to indicate an adverse or toxic response to thyrotropin alfa.
Clinical Studies
Clinical Trials of THYROGEN as an Adjunctive Diagnostic Tool
- Two prospective, randomized phase 3 clinical trials were conducted in patients with well-differentiated thyroid cancer to compare 131I whole body scans obtained after THYROGEN injection to 131I whole body scans after thyroid hormone withdrawal. A cross-over, non-blinded design was used in both trials. Oral radioiodine was given 24 hours after the second injection of THYROGEN, and scanning was done 48 hours after the radioiodine administration. Each patient was scanned first following THYROGEN and then scanned after thyroid hormone withdrawal. In both studies, the primary endpoint was the rate of concordant scans (scan findings in agreement in a given patient using each preparation method).
- Study 1 (n=127) compared the diagnostic scanning following a THYROGEN regimen of 0.9 mg IM daily on two consecutive days to thyroid hormone withdrawal. In addition to body scans, Study 2 (n=229) also compared thyroglobulin (Tg) levels obtained after THYROGEN to those at baseline and to those after thyroid hormone withdrawal. All Tg testing was performed in a central laboratory using a radioimmunoassay (RIA) with a functional sensitivity of 2.5 ng/mL. Patients who were included in the Tg analysis were those who had undergone total or near-total thyroidectomy with or without 131I ablation, had < 1% uptake in the thyroid bed on a scan after thyroid hormone withdrawal, and did not have detectable anti-Tg antibodies. The maximum THYROGEN Tg value was obtained 72 hours after the final THYROGEN injection, and this value was used in the analysis.
Diagnostic Radioiodine Whole Body Scan Results
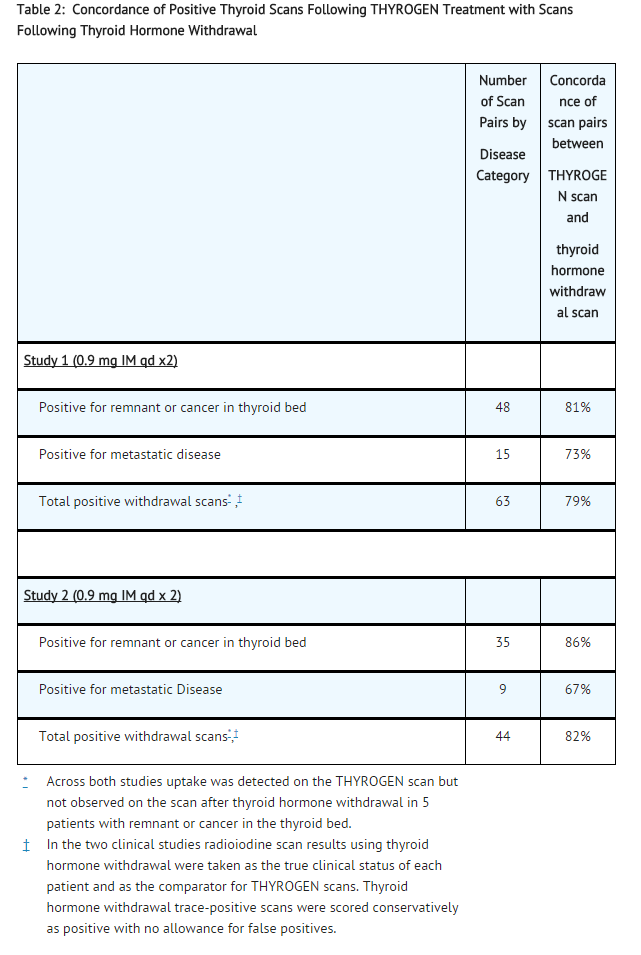
- Study 1 enrolled 127 patients, 71% were female and 29% male, and mean age was 44 years. The study included the following forms of differentiated thyroid cancer: papillary cancer (88%), follicular cancer (9%), and Hurthle cell (2%). Study results are displayed in Table 2.
- In Study 2, patients with differentiated thyroid cancer who had been thyroidectomized (n = 229) were randomized into one of two THYROGEN treatment regimens: THYROGEN 0.9 mg IM daily on two consecutive days (n = 117), and THYROGEN 0.9 mg IM daily on days 1, 4 and 7 (n = 112). Each patient was scanned first using THYROGEN, then scanned using thyroid hormone withdrawal. The group receiving the THYROGEN 0.9 mg IM x 2 regimen was 63% female/27% male, had a mean age 44 years, and generally had low-stage papillary or follicular cancer (AJCC/TNM Stage I 61%, Stage II 19%, Stage III 14%, Stage IV 5%). The group receiving the THYROGEN 0.9 mg IM x 3 regimen was 66% female/34% male, had a mean age 50 years, and generally had low-stage papillary or follicular cancer (AJCC/TNM Stage I 50%, Stage II 20%, Stage III 20%, Stage IV 9%). The amount of radioiodine used for scanning was 4 mCi ± 10%, and scanning times were lengthened in some patients to capture adequate images (30 minute scans, or 140,000 counts). Scan pairs were assessed by blinded readers. Study results are presented in Table 2.
- Across the two clinical studies, and scoring all false positives in favor of thyroid hormone withdrawal, the majority of positive scans using THYROGEN and thyroid hormone withdrawal were concordant. The THYROGEN scan failed to detect remnant and/or cancer localized to the thyroid bed in 17% (14/83) of patients in whom it was detected by a scan after thyroid hormone withdrawal. In addition, the THYROGEN scan failed to detect metastatic disease in 29% (7/24) of patients in whom it was detected by a scan after thyroid hormone withdrawal.
Thyroglobulin (Tg) Results
- THYROGEN Tg Testing Alone and in Combination with Diagnostic Whole Body Scanning: Comparison with Results after Thyroid Hormone Withdrawal
- In anti-Tg antibody negative patients with a thyroid remnant or cancer (as defined by a withdrawal Tg ≥ 2.5 ng/mL or a positive scan [after thyroid hormone withdrawal or after radioiodine therapy]), the THYROGEN Tg was positive (≥ 2.5 ng/mL) in 69% (40/58) of patients after 2 doses of THYROGEN.
- In these same patients, adding the whole body scan increased the detection rate of thyroid remnant or cancer to 84% (49/58) of patients after 2 doses of THYROGEN.
- Among patients with metastatic disease confirmed by a post-treatment scan or by lymph node biopsy (35 patients), THYROGEN Tg was positive (≥ 2.5 ng/mL) in all 35 patients, while Tg on thyroid hormone suppressive therapy was positive ( ≥ 2.5 ng/mL) in 79% of these patients.
- As with thyroid hormone withdrawal, the intra-patient reproducibility of THYROGEN testing with regard to both Tg stimulation and radioiodine imaging has not been studied.
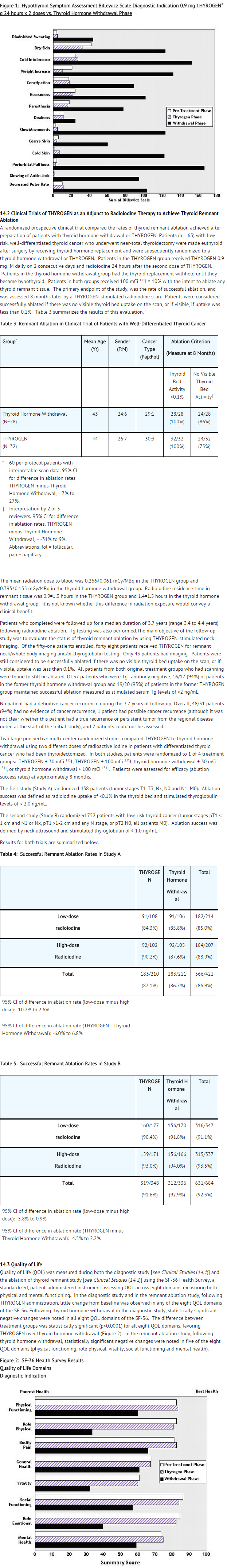
Hypothyroid Signs and Symptoms
- THYROGEN administration was not associated with the signs and symptoms of hypothyroidism that accompanied thyroid hormone withdrawal as measured by the Billewicz scale. Statistically significant worsening in all signs and symptoms were observed during the hypothyroid phase (p<0.01)
How Supplied
- THYROGEN (thyrotropin alfa for injection) is supplied as a sterile, non-pyrogenic, lyophilized product. It is available either in a two-vial kit or a four-vial kit. The two-vial kit contains two 1.1 mg vials of THYROGEN. The four-vial kit contains two 1.1 mg vials of THYROGEN, as well as two 10 mL vials of Sterile Water for Injection, USP.
- NDC 58468-1849-4 (4-vial kit)
- NDC 58468-0030-2 (2-vial kit)
- THYROGEN is for intramuscular injection to the buttock. The lyophilized powder should be reconstituted immediately prior to use with 1.2 mL of Sterile Water for Injection, USP. Each vial of THYROGEN and each vial of diluent, if provided, is intended for single use.
- THYROGEN should be stored at 2-8ºC (36-46ºF)
Storage
- If necessary, the reconstituted solution can be stored for up to 24 hours at a temperature between 2ºC and 8ºC, while avoiding microbial contamination.
- Protect from light.
Images
Drug Images
{{#ask: Page Name::Thyrotropin alpha |?Pill Name |?Drug Name |?Pill Ingred |?Pill Imprint |?Pill Dosage |?Pill Color |?Pill Shape |?Pill Size (mm) |?Pill Scoring |?NDC |?Drug Author |format=template |template=DrugPageImages |mainlabel=- |sort=Pill Name }}
Package and Label Display Panel
{{#ask: Label Page::Thyrotropin alpha |?Label Name |format=template |template=DrugLabelImages |mainlabel=- |sort=Label Page }}
Patient Counseling Information
If necessary, the reconstituted solution can be stored for up to 24 hours at a temperature between 2ºC and 8ºC, while avoiding microbial contamination.
Protect from light.
Precautions with Alcohol
- Alcohol-Thyrotropin alpha interaction has not been established. Talk to your doctor about the effects of taking alcohol with this medication.
Brand Names
- THYROGEN ®[2]
Look-Alike Drug Names
There is limited information regarding Thyrotropin alpha Look-Alike Drug Names in the drug label.
Drug Shortage Status
Price
References
The contents of this FDA label are provided by the National Library of Medicine.
- ↑ Silva MN, Rubió IG, Romão R, Gebrin EM, Buchpiguel C, Tomimori E; et al. (2004). "Administration of a single dose of recombinant human thyrotrophin enhances the efficacy of radioiodine treatment of large compressive multinodular goitres". Clin Endocrinol (Oxf). 60 (3): 300–8. PMID 15008994 PMID: 15008994 Check
|pmid=value (help). - ↑ "THYROGEN- thyrotropin alfa injection, powder, for solution".
{{#subobject:
|Label Page=Thyrotropin alpha |Label Name=Thyr 04.jpg
}}
{{#subobject:
|Label Page=Thyrotropin alpha |Label Name=Thro 05.jpg
}}
{{#subobject:
|Label Page=Thyrotropin alpha |Label Name=DailyMed - THYROGEN- thyrotropin alfa injection, powder, for solution THYROGEN- thyrotropin alfa .png
}}