Skin
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [2]
- Beyond overall skin structure, refer below to: See-also.
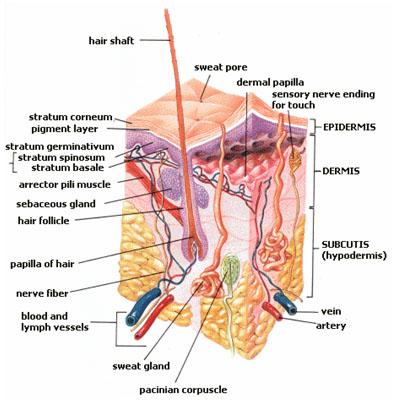
In zootomy and dermatology, skin is the largest organ of the integumentary system made up of multiple layers of epithelial tissues that guard underlying muscles and organs. [1] Skin pigmentation (see: human skin color or coloring) varies among populations, and skin type can range from dry skin to oily skin.
The adjective cutaneous literally means "of the skin" (from Latin cutis, skin).
As the interface with the surroundings, skin plays the most important role in protecting (the body) against pathogens. Its other main functions are insulation and temperature regulation, sensation, and synthesis of vitamin D and the protection of vitamin B folats.
Severely damaged skin will try to heal by forming scar tissue, often giving rise to discoloration and depigmentation of the skin.
The use of natural or synthetic cosmetics to treat the appearance of the face and condition of the skin (such as pore control and blackhead cleansing) is common among many cultures. Oily skin is caused by hormonal fluctuations in the body, which lead to a DHT sensitivity. This sensitivity means that the skin begins to lose moisture and essential fatty acids (linoleic acid in particular), causing thousands of skin cells to die, so the skin compensates for this loss of moisture by producing higher levels of oil. [2] Oily skin can be cleaned quickly with a mild solution of laundry detergent,[1] when pure bath soaps fail (see below: Hygiene). Afterward, body lotions could be used to recondition cleansed skin,[1] as would be used to treat dry skin.
Skin components
- Also see below: Skin layers, at bottom.
Skin has pigmentation, or melanin, provided by melanocytes, which absorb some of the potentially dangerous ultraviolet radiation (UV) in sunlight. It also contains DNA repair enzymes which help to reverse UV damage, and people who lack the genes for these enzymes suffer high rates of skin cancer. One form predominantly produced by UV light, malignant melanoma, is particularly invasive, causing it to spread quickly, and can often be deadly. Human skin pigmentation varies among populations in a striking manner. This has sometimes led to the classification of people(s) on the basis of skin color.
Mammalian skin often contains hairs, which in sufficient density is called fur. The hair mainly serves to augment the insulation the skin provides, but can also serve as a secondary sexual characteristic or as camouflage. On some animals, the skin is very hard and thick, and can be processed to create leather. Reptiles and fish have hard protective scales on their skin for protection, and birds have hard feathers, all made of tough β-keratins. Amphibian skin is not a strong barrier to passage of chemicals and is often subject to osmosis. A frog sitting in an anesthetic solution could quickly go to sleep.
The skin is often known as the largest organ of the human body. This applies to exterior surface, as it covers the body, appearing to have the largest surface area of all the organs. Moreover, it applies to weight, as it weighs more than any single internal organ, accounting for about 15 percent of body weight. For the average adult human, the skin has a surface area of between 1.5-2.0 square meters (8-10.8 sq.ft.), most of it is between 2-3 mm (0.10 inch) thick. The average square inch (6 cm²) of skin holds 650 sweat glands, 20 blood vessels, 60,000 melanocytes, and more than a thousand nerve endings.
Functions
Skin performs the following functions:
- Protection: an anatomical barrier between the internal and external environment in bodily defense; Langerhans cells in the skin are part of the adaptive immune system
- Sensation: contains a variety of nerve endings that react to heat and cold, touch, pressure, vibration, and tissue injury; see somatosensory system and haptics.
- Heat regulation: the skin contains a blood supply far greater than its requirements which allows precise control of energy loss by radiation, convection and conduction. Dilated blood vessels increase perfusion and heat loss while constricted vessels greatly reduce cutaneous blood flow and conserve heat. Erector pili muscles are significant in animals.
- Control of evaporation: the skin provides a relatively dry and impermeable barrier to fluid loss. Loss of this function contributes to the massive fluid loss in burns.
- Aesthetics and communication: others see our skin and can assess our mood, physical state and attractiveness.
- Storage and synthesis: acts as a storage center for lipids and water, as well as a means of synthesis of vitamin D by action of UV on certain parts of the skin.
- Excretion: The concentration of urea is 1/130th that of urine. Excretion by sweating is at most a secondary function to temperature regulation.
- Absorption: Oxygen, nitrogen and carbon dioxide can diffuse into the epidermis in small amounts, some animals using their skin for their sole respiration organ. In addition, medicine can be administered through the skin, by ointments or by means of adhesive patch, such as the nicotine patch or iontophoresis. The skin is an important site of transport in many other organisms.
Hygiene
Unclean skin favors the development of pathogenic organisms - the dead cells that continually slough off of the epidermis mix with the secretions of the sweat and sebaceous glands and the dust found on the skin to form a filthy layer on its surface. If not washed away, the slurry of sweat and sebaceous secretions mixed with dirt and dead skin is decomposed by bacterial flora, producing a foul smell. Functions of the skin are disturbed when it is excessively dirty; it becomes more easily damaged, the release of antibacterial compounds decreases, and dirty skin is more prone to develop infections. Cosmetics should be used carefully because these may cause allergic reactions. Each season requires suitable clothing in order to facilitate the evaporation of the sweat. Sunlight, water and air play an important role in keeping the skin healthy.
The skin supports its own ecosystems of microorganisms, including yeasts and bacteria, which cannot be removed by any amount of cleaning. Estimates place the number of individual bacteria on the surface of one square inch (6.5 square cm) of human skin at 50 million though this figure varies greatly over the average 20 feet2 (1.9 m²) of human skin. Oily surfaces, such as the face, may contain over 500 million bacteria per square inch (6.5 cm²). Despite these vast quantities, all of the bacteria found on the skin's surface would fit into a volume the size of a pea.[3] In general, the microorganisms keep one another in check and are part of a healthy skin. When the balance is disturbed, there may be an overgrowth and infection, such as when antibiotics kill microbes, resulting in an overgrowth of yeast. The skin is continuous with the inner epithelial lining of the body at the orifices, each of which supports its own complement of microbes.
Oily skin is caused by over-active glands, that produce a substance called sebum, a naturally healthy skin lubricant.[1] When the skin produces excessive sebum, it becomes heavy and thick in texture. Oily skin is typified by shininess, blemishes and pimples.[1] The oily-skin type is not necessarily bad, since such skin is less prone to wrinkling, or other signs of aging,[1] because the oil helps to keep needed moisture locked into the epidermis (outermost layer of skin).
The negative aspect of the oily-skin type is that oily complexions are especially susceptible to clogged pores, blackheads, and buildup of dead skin cells on the surface of the skin.[1] Oily skin can be sallow and rough in texture and tends to have large, clearly visible pores everywhere, except around the eyes and neck.[1]
The goal of treating oily skin is to remove excess surface sebum without complete removal of skin lipids.[1] Severe degreasing treatment can foster an actual worsening of sebum secretion, which defeats the aim of the cleansing.[1] A method of cleansing oily skin is to wash with a solution of a mild synthetic detergent[1] (see: surfactant) containing no oils, waxes or other lipid agents that could aggravate the oily condition of the skin, sometimes combined with a toning lotion. Such a product removes the oily residue and debris from the skin surface. Some cleansing products have lower concentrations of hydroxy acids, which remove dead cells from the upper levels of the stratum corneum.[1] Those products should be used on a regular basis to work adequately.[1] A light moisturizer may be included in a product to counteract any drying effects of the cleanser.[1]
Aging
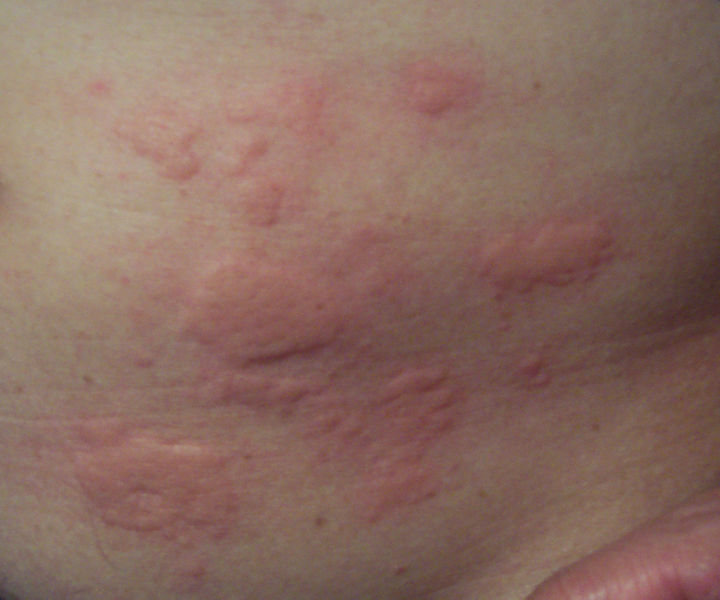
As skin ages, it becomes thinner and more easily damaged. Intensifying this effect is the decreasing ability of skin to heal itself, as a person ages and skin requires a longer time to heal in later life.
Skin sagging is caused by the fall in elasticity. Ageing skin also receives less blood flow and lower gland activity.
Disease
In medicine, the branch concerned with the skin is called dermatology. The skin is subject to constant attack from without, and so can be afflicted by numerous ailments, such as these:
Tumors:
- Benign tumors of the skin such as Squamous cell papilloma
- Skin cancer
Others:
- Rashes
- Blisters
- Acne
- Keratosis pilaris
- Fungal infections such as athlete's foot
- Microbial infections.
- Calcinosis cutis
- Ring worm
- Sunburn
- Keloid
- Scabies
There are several other skin diseases as well.
Variability in skin tone
Individuals with ancestors from different parts of the world can have highly visible differences in skin pigmentation. Individuals with African ancestry (black people) tend towards darker skin, while those of Northern European descent (white people) have paler skin. Between these extremes are individuals of Asian, South-East Asian, Native American, Middle Eastern, Polynesian and Melanesian descent.
The skin of black people has more variation in color from one part of the body to another than does the skin of other racial groups, particularly the palms of the hands and soles of the feet. Part of this is the result of the variations in the thickness of the skin or different parts of the body. The thicker the skin, the more layers of cell with melanin in them, and the darker the color.[4] In addition, these parts of the body do not have melanin-producing cells.
Darker skin hinders UV A rays from penetrating. Since vitamin B folats are degraded by UV A and vitamin D is synthesised different skin tones are more likely to produce different vitamin deficiencies.
Animal skin products
Skins and hides from different animals are used for clothing, bags and other consumer products, usually in the form of leather, but also furs, rawhide, snakeskin and hagfish. Skin can also be used to make products such as gelatin and glue. See also wool.
Skin layers
Skin is composed of three primary layers: the epidermis, which provides waterproofing and serves as a barrier to infection; the dermis, which serves as a location for the appendages of skin; and the hypodermis (subcutaneous adipose layer), which is called the basement membrane.
Epidermis
Epidermis, "epi" coming from the Greek meaning "over" or "upon", is the outermost layer of the skin. It forms the waterproof, protective wrap over the body's surface and is made up of stratified squamous epithelium with an underlying basal lamina.
The outermost epidermis consists of stratified squamous epithelium with an underlying connective tissue section, or dermis, and a hypodermis, or basement membrane. The epidermis contains no blood vessels, and cells in the deepest layers are nourished by diffusion from blood capillaries extending to the upper layers of the dermis. The main type of cells which make up the epidermis are keratinocytes, with melanocytes and Langerhans cells also present. The epidermis can be further subdivided into the following strata (beginning with the outermost layer): corneum, lucidum (only in palms of hands and bottoms of feet), granulosum, spinosum, basale. Cells are formed through mitosis at the basale layer. The daughter cells, (see cell division) move up the strata changing shape and composition as they die due to isolation from their blood source. The cytoplasm is released and the protein keratin is inserted. They eventually reach the corneum and slough off (desquamation). This process is called keratinization and takes place within about 30 days. This keratinized layer of skin is responsible for keeping water in the body and keeping other harmful chemicals and pathogens out, making skin a natural barrier to infection.

Optical Coherence Tomography tomogram of fingertip, depicting stratum corneum (~500µm thick) with stratum disjunctum on top and stratum lucidum (connection to stratum spinosum) in the middle. At the bottom superficial parts of the dermis. Sweatducts are clearly visible.
Components
The epidermis contains no blood vessels, and is nourished by diffusion from the dermis. The main type of cells which make up the epidermis are keratinocytes, melanocytes, Langerhans cells and Merkels cells.
Layers
Epidermis is divided into several layers where cells are formed through mitosis at the innermost layers. They move up the strata changing shape and composition as they differentiate and become filled with keratin. They eventually reach the top layer called stratum corneum and become sloughed off, or desquamated. This process is called keratinization and takes place within weeks. The outermost layer of Epidermis consists of 25 to 30 layers of dead cells.
Sublayers
Epidermis is divided into the following 5 sublayers or strata:
- Stratum corneum
- Stratum lucidum
- Stratum granulosum
- Stratum spinosum
- Stratum germinativum (also called "stratum basale")
Mnemonics that are good for remembering the layers of the skin (using "stratum basale" instead of "stratum germinativum"):
- "Cher Likes Getting Skin Botoxed" (from superficial to deep)
- "Before signing, get legal counsel" (from deep to superficial)
- "Before Sex Get Latex Condoms (from deep to superficial)
Blood capillaries are found beneath the epidermis, and are linked to an arteriole and a venule. Arterial shunt vessels may bypass the network in ears, the nose and fingertips.
Dermis
The dermis is the layer of skin beneath the epidermis that consists of connective tissue and cushions the body from stress and strain. The dermis is tightly connected to the epidermis by a basement membrane. It also harbors many nerve endings that provide the sense of touch and heat. It contains the hair follicles, sweat glands, sebaceous glands, apocrine glands, lymphatic vessels and blood vessels. The blood vessels in the dermis provide nourishment and waste removal to its own cells as well as the Stratum basale of the epidermis.
Structure
The dermis is structurally divided into two areas: a superficial area adjacent to the epidermis, called the papillary region, and a deep thicker area known as the reticular region.
Papillary region
The papillary region is composed of loose areolar connective tissue. It is named for its fingerlike projections called papillae, that extend toward the epidermis. The papillae provide the dermis with a "bumpy" surface that interdigitates with the epidermis, strengthening the connection between the two layers of skin.
In the palms, fingers, soles, and toes, the influence of the papillae projecting into the epidermis forms contours in the skin's surface. These are called friction ridges, because they help the hand or foot to grasp by increasing friction. Friction ridges occur in patterns (see: fingerprint) that are genetically determined and are therefore unique to the individual, making it possible to use fingerprints or footprints as a means of identification.
Reticular region
The reticular region lies deep in the papillary region and is usually much thicker. It is composed of dense irregular connective tissue, and receives its name from the dense concentration of collagenous, elastic, and reticular fibers that weave throughout it. These protein fibers give the dermis its properties of strength, extensibility, and elasticity.
Also located within the reticular region are the roots of the hair, sebaceous glands, sweat glands, receptors, nails, and blood vessels.
Tattoo ink is injected into the dermis. Stretch marks from pregnancy are also located in the dermis.
The hypodermis is not part of the skin, and lies below the dermis. Its purpose is to attach the skin to underlying bone and muscle as well as supplying it with blood vessels and nerves. It consists of loose connective tissue and elastin. The main cell types are fibroblasts, macrophages and adipocytes (the hypodermis contains 50% of body fat). Fat serves as padding and insulation for the body.
Microorganisms like Staphylococcus epidermidis colonize the skin surface. These microorganisms serve as ecoorgan. The density of skin flora depends on region of the skin. The disinfected skin surface gets recolonized from bacteria residing in the deeper areas of the hair follicle, gut and urogenital openings.
See also
Related topics (in alphabetical order):
- Acid mantle
- Callus - thick area of skin
- Cosmetic surgery
- Cutaneous structure development
- Diseases - list of skin diseases
- Dermatology - branch of medicine
- Fingerprint - skin on fingertips
- Hair - including hair follicles in skin
- Skin color
- Hyperpigmentation - about excess skin color
- Meissner's corpuscle
- Nails - fingernails or toenails
- Pacinian corpuscle
- Polyphenol antioxidant
- Sweat - description of perspiration
- Superficial fascia
References
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 "Skin care" (analysis), Health-Cares.net, 2007, webpage: HCcare.
- ↑ "Why Me, Why Now?" SkinMed.co.uk, 2007, webpage: [1].
- ↑ Theodor Rosebury. Life on Man: Secker & Warburg, 1969 ISBN 0-670-42793-4
- ↑ Smith, Wilma and Burns, Catherine. (1999) "Managing the hair and skin of African American pediatric patients." Journal of Pediatric Health Care 13(2):72-8.
External links
Template:Integumentary system Template:Human anatomical features
af:Vel ar:جلد bg:Кожа ca:Pell cs:Kůže cy:Croen da:Hud de:Haut et:Nahk eo:Haŭto fa:پوست gl:Pel hr:Koža id:Kulit is:Húð it:Pelle he:עור lv:Āda lt:Oda ln:Lomposo mk:Кожа ms:Kulit nl:Huid no:Hud nrm:Pé (la) pam:Balat scn:Peddi simple:Skin sk:Koža sl:Koža sr:Кожа su:Kulit fi:Iho sv:Hud th:ผิวหนัง tl:Balat