Seborrheic dermatitis
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Jesus Rosario Hernandez, M.D. [2]; Aysha Aslam, M.B.B.S[3]
Synonyms and keywords: Seborrheic eczema; Seborrhea; Cradle cap
Overview
Seborrheic eczema (also known as Seborrheic dermatitis, seborrhea) is a skin disorder affecting the scalp, face, and trunk. Seborrheic dermatitis causes flaky, itchy, red skin and temporary hair loss. It particularly affects the sebum-gland rich areas of skin. Causes of seborrheic dermatitis include Malassezia furfur (formerly known as Pityrosporum ovale) as well as genetic, environmental, hormonal, and immune-related factors. Medical therapy for seborrheic dermatitis includes antifungal agents, corticosteroids, and lithium salts.
Historical Perspective
- In 1887, seborrheic dermatitis was first described by Unna.
- In 1894, a hypothesis was made by Unna and Sabouraud that causative agents responsible for seborrheic dermatitis include yeast Malassezia, bacteria, or both as they were obtained in high quantities in cultures obtained from the affected patients.
- In 1984, Shuster discovered that seborrheic dermatitis can be treated with oral ketoconazole.[1].[2]
Classification
There is no established classification system for seborrheic dermatitis. However, it may be classified according to the anatomical location, age group, symptoms, etiology and severity.[3][4][5][6][7]
Classification by Anatomy
Seborrheic dermatitis may be classified on the basis of anatomical location into following types:[8][3][9][10]
- Localized
- Scalp: Most common presentation in infants known as cradle cap
- Face: Most commonly involves eyelids, eyebrows, and nasolabial folds
- Retroauricular
- Body folds: Commonly affects axilla, breast folds, and inguinal area
- Trunk: May be seen in severe cases and most common site of involvement is lower abdomen
- Upper Chest: Most commonly seen in adults
- Generalized: Mostly seen in infants; it is associated with Leiner's disease and children with severe immunodeficiency.[11]
Classification by Age
- Infantile: Occurs in first three months of life.
- Adults: Occurs most commonly between 30-60 years of age.
Classification by Symptomatic Presentation
- Non pruritic: Most commonly occurs in infants
- Pruritic: Most commonly occurs in older children and adults
Classification by Etiology
- Idiopathic
- Infectious
- Autoimmune / Inflammatory
Classification by Severity
- Mild to moderate disease: Occurs in immunocompetent individuals
- Severe disease: Occurs in immunocompromised individuals
Pathophysiology
The exact pathophysiology of seborrheic dermatitis remains unclear. However, several mechanisms are hypothesized to play a role in pathogenesis of seborrheic dermatitis.[12] [13][14][15][11]
Pathogenesis
Hypotheses regarding the pathogenesis of seborrheic dermatitis include:
Hypotheses related to Malassezia :
- A strong correlation between presence of the fungal yeast Malassezia and response to antifungals in patients with seborrheic dermatitis.[16]
- Malassezia is a lipophilic yeast found on the skin of both healthy individuals and seborrheic dermatitis patients. It is thought that host reaction to Malassezia or its metabolites causes an inflammatory reaction that may have a significant role in the process.[13].
- Another proposed mechanism for seborrheic dermatitis suggests that a disrupted lipid layer of Malassezia leads to an increased production of pro inflammatory cytokines such as IL-6 and IL-7, and decreased production of IL-10. [7]
- Malassezia is seen to have lipase activity, which acts on cutaneous triglycerides causing a release of unsaturated fatty acids such as arachidonic acid. These metabolites may cause abnormal proliferation and differentiation of the stratum corneum leading to signs and symptoms of seborrheic dermatitis.[17][18][19]
Other Hypotheses
- Sebaceous gland activity
- Sebum gland activity may correlate with seborrheic dermatitis.[15][20]
- Elevated levels of HLA-AW30, HLA-AW31, HLA-A32, HLA-B12 and HLA-B18 and increased levels of total serum IgA and IgG antibodies have been detected in seborrheic dermatitis patients. This implies an immune mediated pathological mechanism.[14][21][22]
- Epidermal barrier dysfunction
- Abnormalities in stratum corneum that may be associated with seborrheic dermatitis include:
- Neurogenic and other factors
- Patients with parkinsonism may have increase levels of α-melanocyte stimulating hormone (α-MSH) levels and seborrheic dermatitis in these patients respond to L-dopa treatment[22]
Genetics
There is no specific genetic cause for seborrheic dermatitis.[24].[25]
Associated conditions
- Parkinsonism
- Epilepsy
- Depressive mood disorder
- Traumatic brain injury
- Spinal cord injury
- HIV
- Lymphoma
- Downs syndrome
Gross Pathology
Superficial flaking and redness are characteristic findings of seborrheic dermatitis.[26]
-
Seborrheic dermatitis showing erythema on face. - By Roymishali - Own work, CC BY-SA 3.0, https://commons.wikimedia.org/w/index.php?curid=27267929
-
Upper chest showing redness and crusting. - Adapted from Dermatology Atlas.[27]
Microscopic Histopathology
Histopathological findings of seborrheic dermatitis may be categorized into the following stages: [21][28]
- Acute
- Focal mild spongiosis with superficial crust containing neutrophils.
- Edema of papillary dermis.
- Dilatation of blood vessels in superficial vascular plexus with infiltration of lymphocytes, histiocytes.
- Subacute
- Psoriasiform hyperplasia.
- Keratin showing presence of yeasts.
- Chronic
- Extensive psoriasiform hyperplasia
- Minimal spongiosis
- Follicular crusting
Causes
The cause of seborrheic dermatitis remains unknown; however, the following factors may have been implicated:
- Malassezia furfur (formerly known as Pityrosporum ovale)[29][30].[31][32][33]
- Excessive vitamin A[34]
- Lack of biotin,[35]
- pyridoxine (vitamin B6)[35][36]
- riboflavin (vitamin B2)[35]
Differentiating Seborrheic dermatitis from Other Diseases
Symptoms of seborrheic dermatitis may overlap with other skin conditions such as psoriasis, candidiasis, contact dermatitis, and atopic dermatitis. Differential diagnosis of seborrheic dermatitis may be classified into two types by age group:[37][38][39][17][40][41][28]
Differential diagnosis in Infants
- Atopic dermatitis
- Candidiasis
- Dermatophytosis
- Diaper dermatitis
- Langerhans cell histiocytosis
- Psoriasis
- Pityriasis amiantacea
- Rosacea
- Tinea capitis
- Zinc deficiency
- Vitamin B deficiency
| Disease | Rash Characteristics | Signs and Symptoms | Associated Conditions | Images |
|---|---|---|---|---|
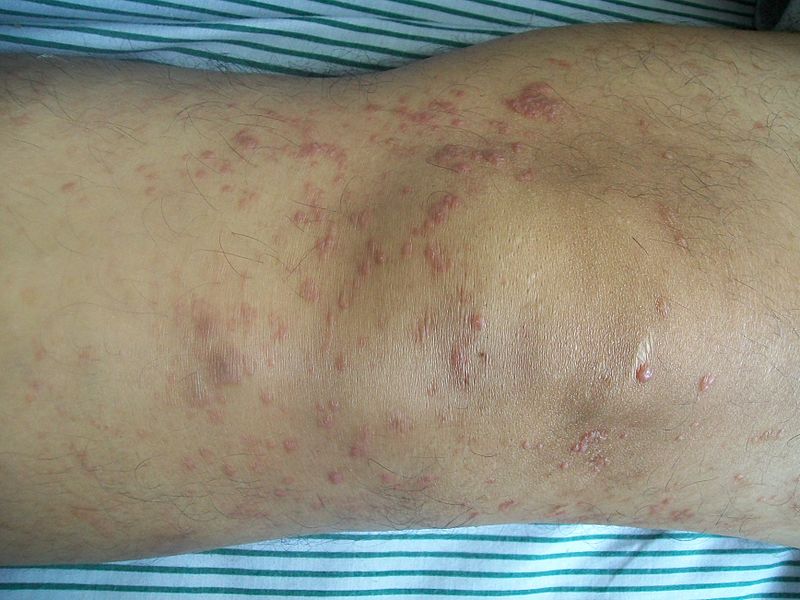
| Cutaneous T cell lymphoma/Mycosis fungoides[42] |
|
|
 | |
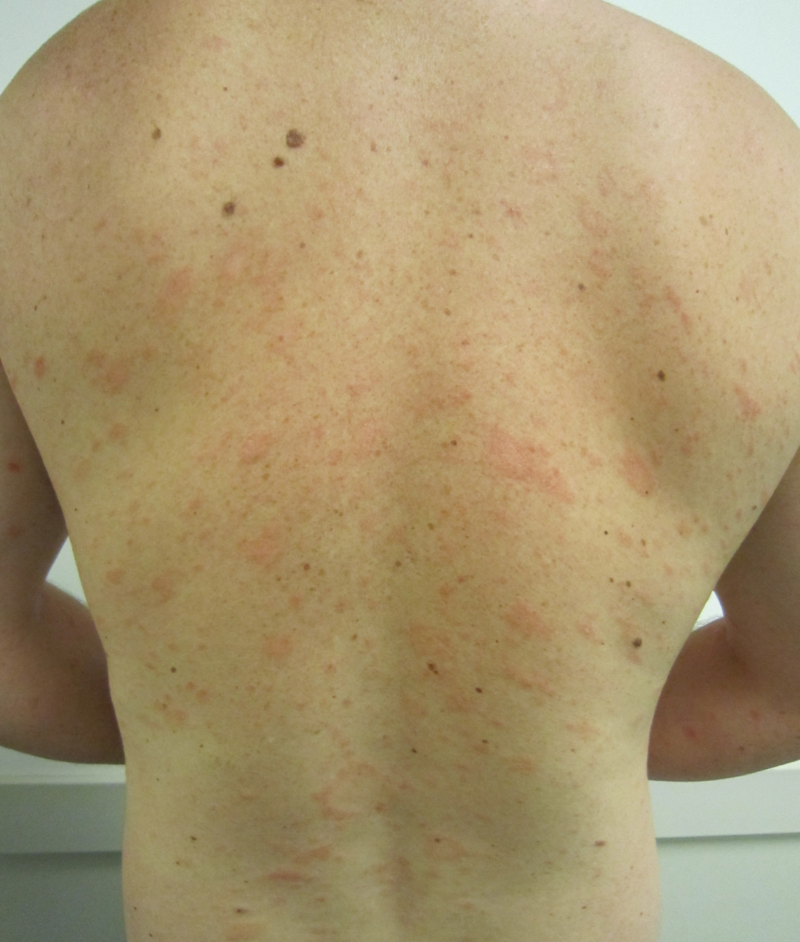
| Pityriasis rosea[43] |
|
|
 | |
| Pityriasis lichenoides chronica |
|
|
||
| Nummular dermatitis[46] |
|
|
|
|
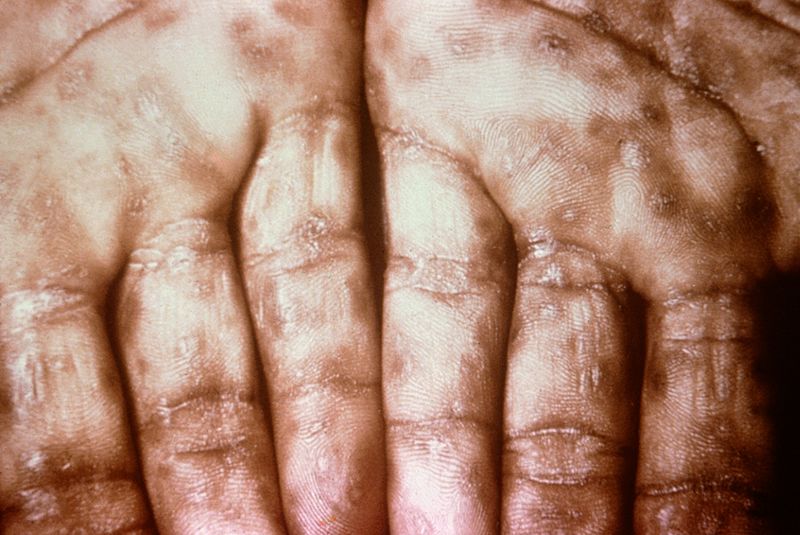
| Secondary syphilis[47] |
|
 | ||
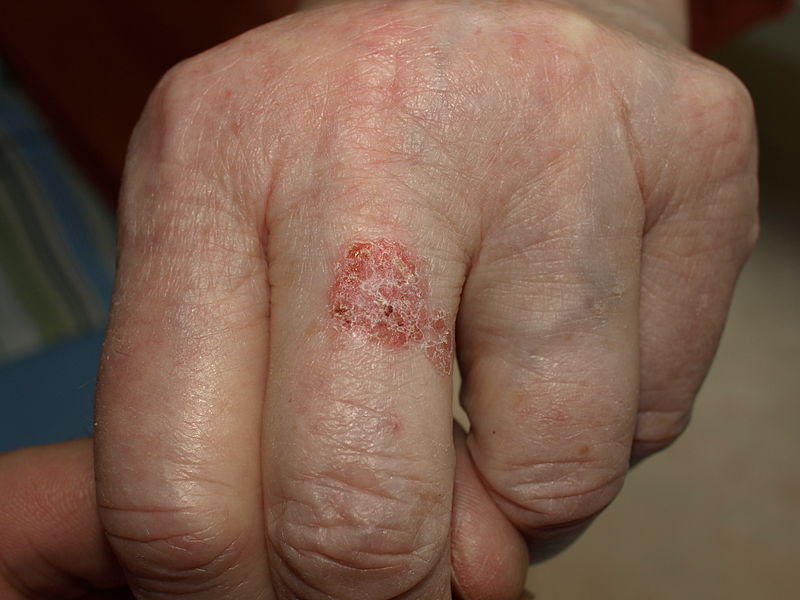
| Bowen’s disease[48] |
|
|
 | |
| Exanthematous pustulosis[50] |
|
|
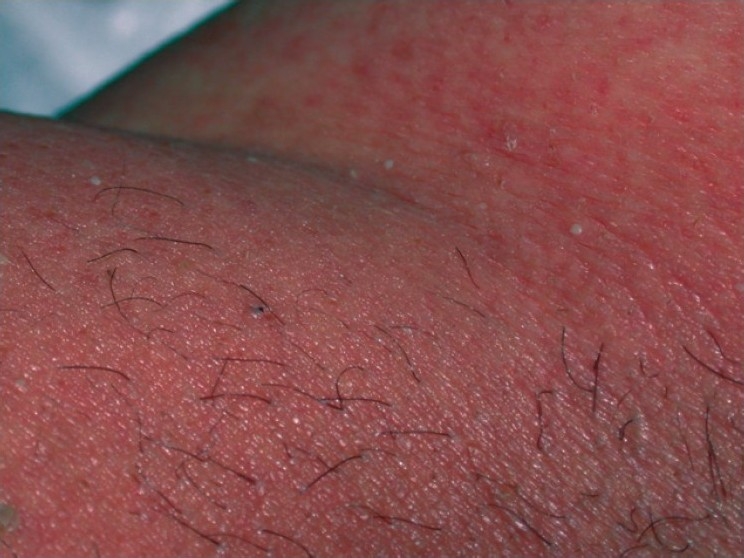 | |
| Hypertrophic lichen planus[52] |
|
|
|
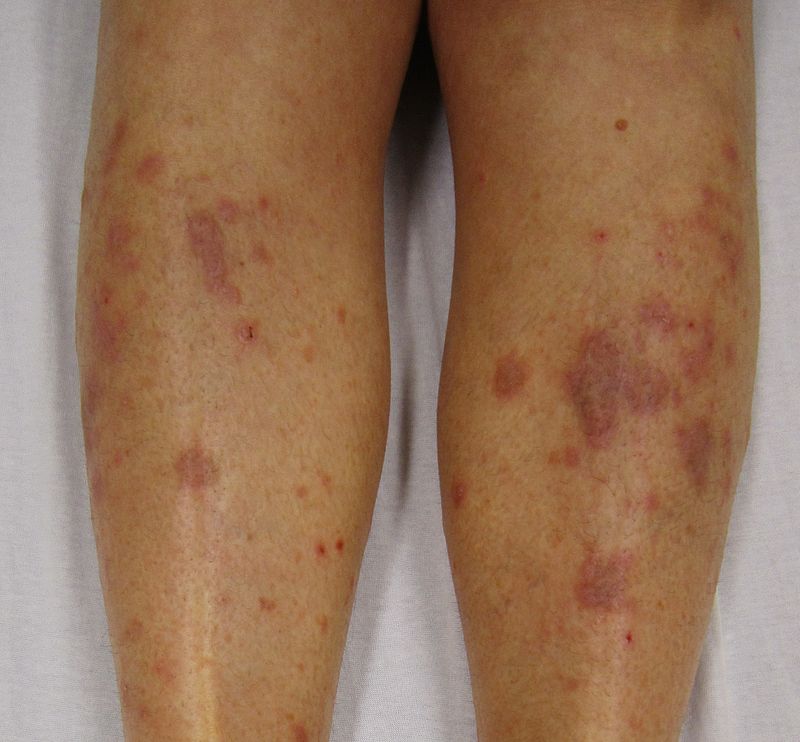 |
| Sneddon–Wilkinson disease[54] |
|
|
||
| Small plaque parapsoriasis[58] |
|
|
|
|
| Intertrigo[60] |
|
|
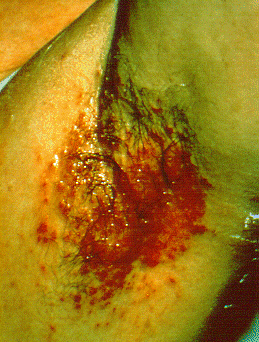 | |
| Langerhans cell histiocytosis[61] |
|
|
|
|
| Tinea manuum/pedum/capitis[65] |
|
|
|
|
| Seborrheic dermatitis |
|
|
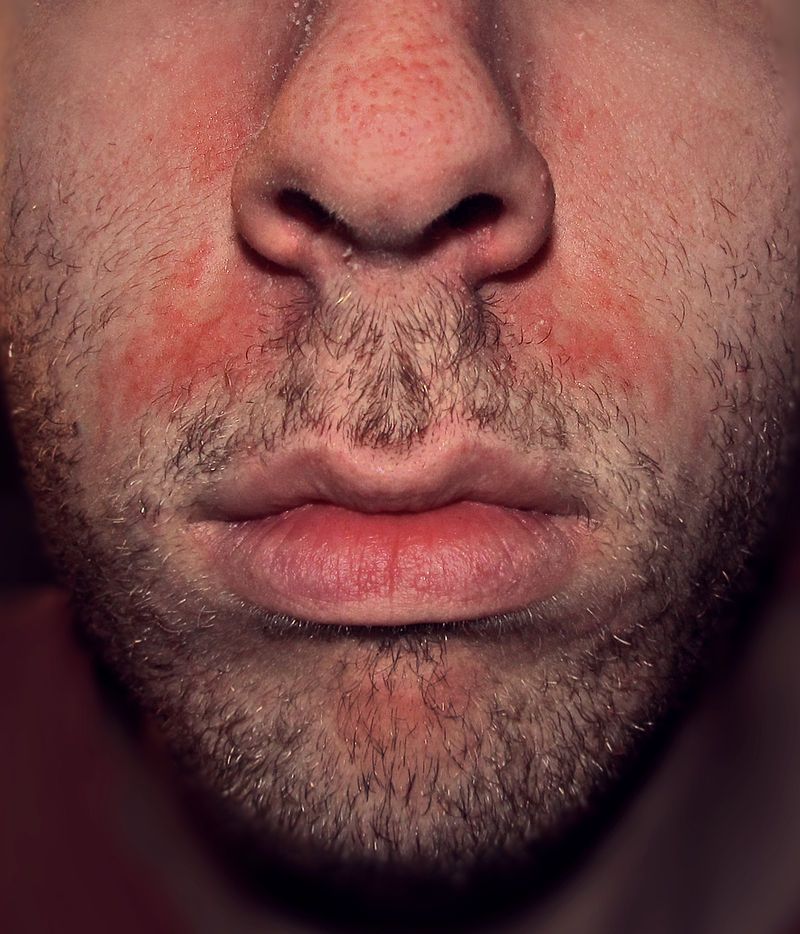 |
Differential diagnosis in Adults
- Systemic lupus erythematosus
- Candidiasis
- Erythrasma
- Contact dermatitis
- Psoriasis
- Tinea versicolor
- Tinea corporis
- Secondary syphilis
- Pemphigus foliaceus
- Rosacea
Epidemiology and Demographics
Epidemiology
Worldwide, the prevalence of seborrheic dermatitis is estimated to be 11000 cases per 100,000.[24] Prevalence of seborrheic varies among individuals based on the following factors:
- Higher reporting of mild cases
- Higher in patients with HIV with 35000 per 100,000 in early diagnosis and 85000 per 100,000 with full blown AIDS[67]
- Higher prevalence seen among those directly exposed to UV radiation[68]
Demographics
Age
Seborrheic dermatitis demonstrates a tri-modal age distribution as follows:[71][72][21]
- The first incidence peak is seen in infants around three to four months of age, which usually resolves within 12 months
- The second incidence peak is seen around puberty.
- The third incidence peak is seen after age 50 with the highest prevalence seen among ages 33-44 years.[73]
- Age groups showing lowest prevalence of clinical disease is seen in individuals younger than 12 years.[74]
Gender
Males are more commonly affected with seborrheic dermatitis than females.[75]
Race
- Seborrheic dermatitis is rarely seen in African Americans.
- If seborrheic dermatitis is seen in this population, it leads to high suspicion of HIV in affected individuals.[76]
Risk Factors
The most common risk factors for seborrheic dermatitis include:[77][17]
- Organ transplant recipients
- HIV/AIDS
- Malignancies such as lymphoma[78][79][80]
Neurologic and psychiatric cases
- Parkinsonism
- Depression
- Tardive dyskinesia
- Traumatic brain injury
- Epilepsy
- Facial nerve palsy
- Spinal cord injury
Genetic disorders
- Downs syndrome
- Hailey-Hailey Disease
- Cardiofaciocutaneous syndrome
- Mutation in (ZNF750) coding a zinc finger protein (C2H2)
Other risk factors
- Stress[66]
- Treatment with psoralene and UV-A
- Male gender [81]
- Obesity
- Diabetes mellitus[82]
- Seasonal changes such as low temperature and decreased humditiy[83]
- Drugs such as haloperidol deconate, lithium and chlorpromazine
Screening
There are no screening guidelines for seborrheic dermatitis.[84]
Natural History, Complications, and Prognosis
Natural History
- The symptoms of seborrheic dermatitis usually develop in the first three months in infants. It may resolve without treatment in most cases in few months and rarely presents after 12 months.[85]
- In adults, symptoms of seborrheic dermatitis usually develop in the second and third decade of life, and start with symptoms such as redness, scaling and crusting on affected areas. However, occurrence of seborrheic dermatitis is highly variable and it may present after 50 years of age.
- The course of disease is highly variable among individuals despite treatment. Some cases present with more frequent relapses than others.[71]
Complications
Common complications of seborrheic dermatitis include:[86][71][87][88][89][11]
- Temporary or permanent hair loss
- Secondary bacterial infection
- Blepharitis
- Abscess of meibomian glands
- Otitis externa
- Extensive involvement of body
Prognosis
- The prognosis of seborrheic dermatitis is excellent in infants; it is a self limited disease and usually resolves within few months after birth.
- In adults, it is a recurrent condition with no permanent cure.[90][91]
Diagnosis
There is no definitive diagnostic criteria for seborrheic dermatitis. Diagnosis of seborrheic dermatitis is primarily clinical; it is based on history and physical examination findings.[92]
History
Obtaining complete history is important in making diagnosis of seborrheic dermatitis as it will give an insight into cause and associated risk factors for the disease. In addition to symptoms of seborrheic dermatitis, patients may present with symptoms of one of the following associated conditions:[93][94][95][17] [96][97][98]
- Parkinsonism
- Epilepsy
- Depressive mood disorder
- Traumatic brain injury
- Spinal cord injury
- HIV
- Lymphoma
- Downs syndrome
- Hailey-Hailey Disease
- Diabetes mellitus
Symptoms
Symptoms of seborrheic dermatitis may be categorized according to age as follows:[24][99]
Infants
Infants usually present in the first few months of life. Symptoms can be divided into following types depending on extent of involvement.
- Localized
- Redness and flaking
- Pruritis
- Most common sites involved are scalp and face
- Other sites involved include retroauricular area, nasolabial folds, cheeks, eyebrows and eyelids
- Napkin or diaper area involvement
- Generalized
Adults
The most common symptoms of seborrheic dermatitis may be divided into two types based on extent of involvement:[24]
- Localized
- Macules, thin plaques, or red patches(scalp, face, nasolabial folds, anterior hairline, eyebrows, glabella region of the forehead, melolabial folds, ears, central chest, and genital region)
- Pruritis
- Fine scaling (mild cases)
- Redness and yellow to white crusting or scaling (severe disease)
- Redness, itching and yellow crusting of eye lashes (Blepharitis).
- Repeated itching of ear causing secondary bacterial infection resulting in fever and ear pain.
- Generalized
- Patients with HIV or other immunosupressive conditions such as malignancies usually present with more severe disease involving unusual sites such as extremities.[100][101]
Physical Examination
Physical examination may be divided into two types according to age group:
| Age | Site involved | Local Examination | Image[102] | |
|---|---|---|---|---|
| Infants | General Appearance | Infants often looks healthy with a good appetite and sleep habits. | 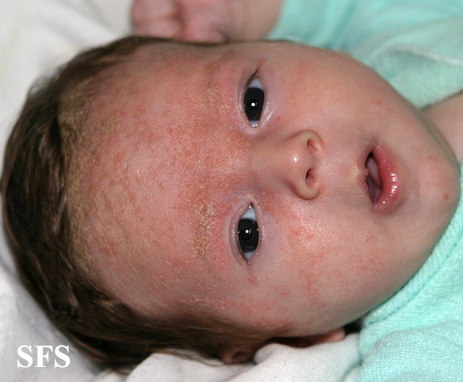
| |
| Scalp | Fine scaling in mild cases. Thick greasy scales with erythema in severe cases.[103] | 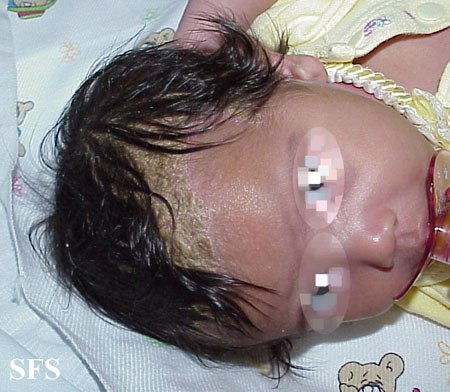
| ||
| Face | Face may present with scaly salmon colored scales. | 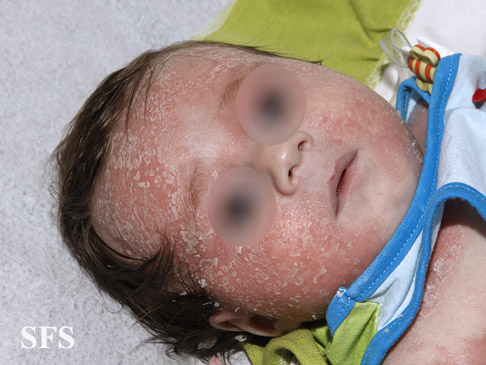
| ||
| Neck, Axillae and Body Folds | Non-scaly moist glistening appearance of lesions which tend to appear confluent.[17] | 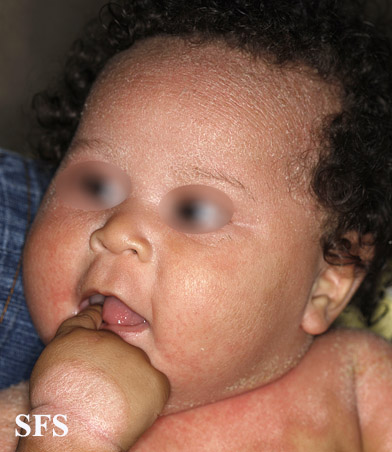
| ||
| Trunk | Trunk involvement is seen in severe cases. However, the diaper area iscommonly involved which presents with erythema and maceration of skin with edema of surrounding skin. Secondary bacterial and candidal infections are common in these cases.[104] | 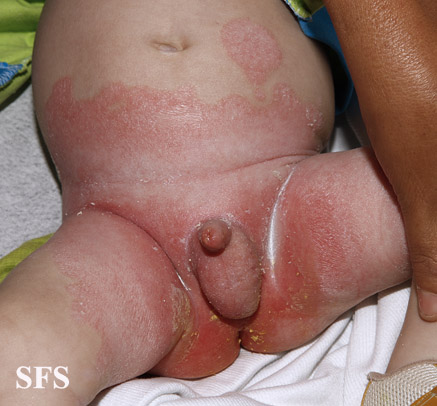
| ||
| Generalized | Most commonly seen in Leiner's disease, which is an immunosuppressive condition. It may involve unusual sites such as extremities and trunk with scaling and erythematous patches. Scaling and crusting usually spreads to involve other parts of the body with extensive peeling of skin.[105][106][107] | 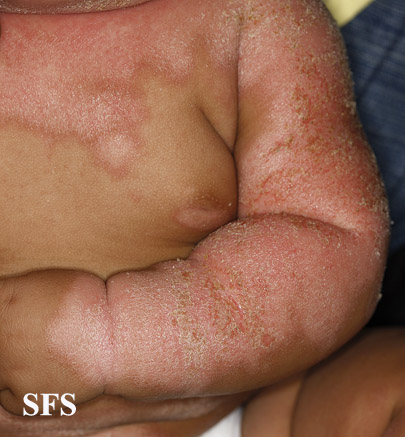
| ||
| Adults | General appearance | Adults may present with a healthy general appearance in mild cases or may present in considerable distress due to widespread involvement especially. Patients may appear ill in cases with underlying diseases associated with seborrheic dermatitis such as HIV, malignancy, or parkinsonism.[78] | 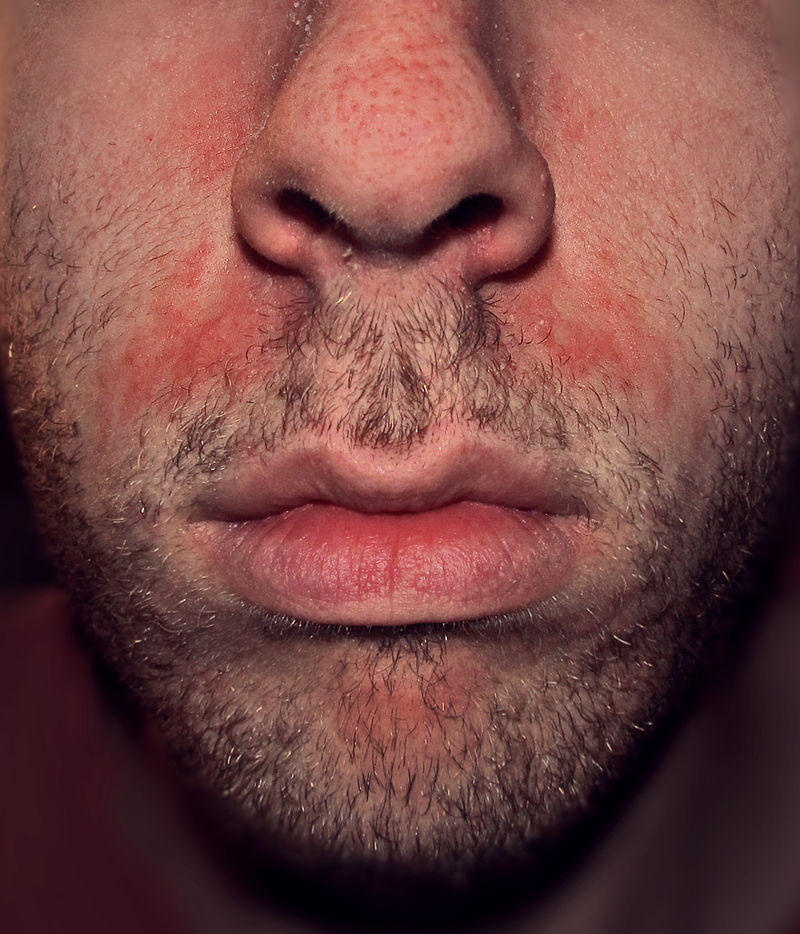
| |
| Scalp | Mild desquamation to honey coloured crusting of the scalp causing alopecia. | 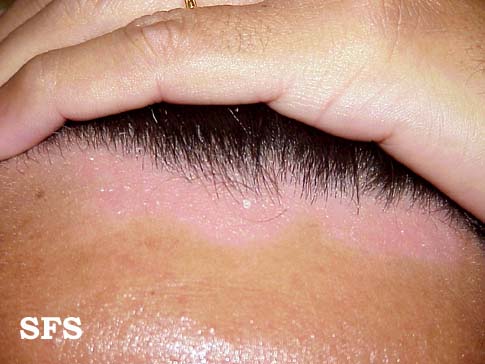
| ||
| Face/Retroauricular
areas |
May present as a "butterfly rash". Malar erythema and scaling in a symmetrical pattern . Yellowish scaling between eyelashes and eyelids causing blepharitis with honey colored crusting on free margins.[71] | 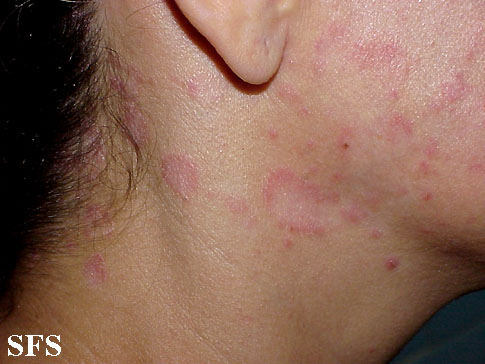
| ||
| Upper Chest | SD presents as petalloid or pityriasiform.
Petalloid: Small reddish follicular or perifollicular papules that may coalesce forming patches resembling petals of flower.
|
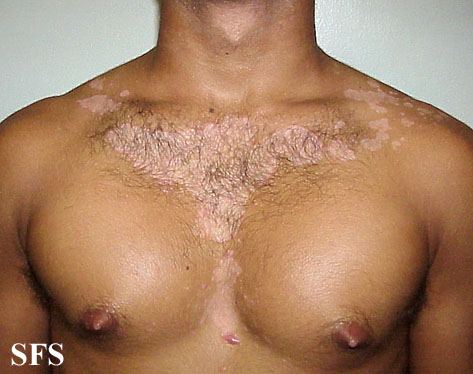
| ||
| Body Folds | Lesions usually present as moist, macerated, and erythematous lesions. May lead to fissuring and secondary infection.[17] | 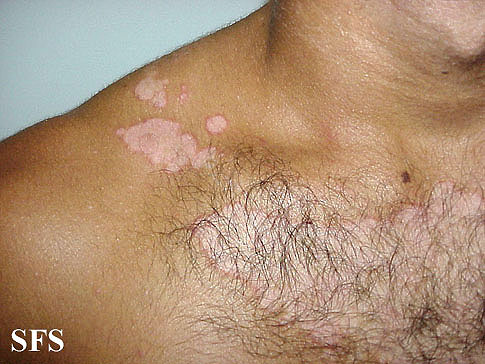
| ||
| SD of | It may present as extensive scaling and erythema involving unusual sites such as extremities and is refractory to treatment. It is usually seen in children and adults with immunosuppression such as HIV/AIDS.[108][109] | 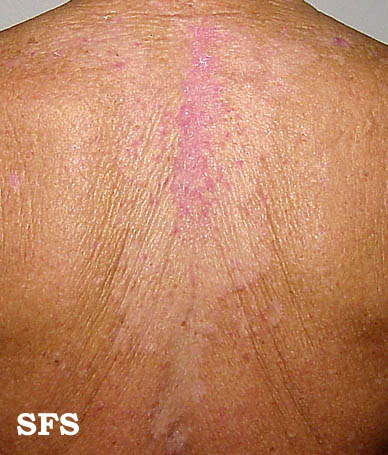
| ||
Imaging Findings
There are no imaging findings associated with seborrheic dermatitis.[41]
Other Diagnostic Studies
There are no other diagnostic studies for seborrheic dermatitis.
Treatment
The mainstay of treatment for seborrheic dermatitis is medical therapy. Depending on age and severity of symptoms the treatment may be categorized as follows:
| Severity | Acute Therapy | Maintainence Therapy | |
|---|---|---|---|
| Infants | Mild |
|
|
| Moderate to Severe |
|
| |
| Adults | Mild |
|
|
| Moderate to Severe |
|
|
The following are the preferred treatment regimens for seborrheic dermatitis:[128]
-
- Preferred regimen (1): Ketoconazole 2% in shampoo, foam, gel, or cream
- Scalp: Twice/week for clearance THEN once/week or every other week for maintenance
- Other areas: From bid to twice/week for clearance THEN from twice/week to once every other week for maintenance
- Preferred regimen (2): Bifonazole 1% in shampoo or cream
- Scalp: 3 times/week for clearance
- Other areas: qd for clearance
- Preferred regimen (3): Ciclopirox olamine (also called ciclopirox) 1.0% or 1.5% in shampoo or cream
- Scalp: Twice to 3 times/week for clearance THEN once/week or every 2 week for maintenance
- Other areas: Twice daily for clearance THEN qd for maintenance
-
- Preferred regimen (1): Hydrocortisone 1% in cream areas other than scalp qd or bid
- Preferred regimen (2): Betamethasone dipropionate 0.05% in lotion scalp and other areas qd or bid
- Preferred regimen (3): Clobetasol 17- butyrate 0.05% in cream areas other than scalp qd or bid
- Preferred regimen (4): Clobetasol dipro- pionate 0.05% in shampoo
- Scalp: Twice weekly in a short- contact fashion (up to 10 min application, then washing)
- Preferred regimen (5): Desonide 0.05% lotion bid on scalp and other areas
-
- Preferred regimen: Lithium succinate AND Zinc sulfate Oin
Plant-based treatments
The World Health Organization mentions Aloe vera gel as a yet to be scientifically proven traditional medicine treatment for Seborrhoeic dermatitis.[129]
- Arctium lappa (Burdock) oil[130]
- Chelidonium majus (Celandine)[130]
- Glycyrrhiza glabra (Licorice)[130]
- Melaleuca (Tea tree) species[130]
- Plantago (Plantain) species[130]
- Symphytum officinale (Comfrey)[130]
- Zingiber officinale (Ginger) root juice[130]treatment containing 8% Lithium succinate AND 0.05% Zinc sulfate
- Preferred regimen: Lithium gluconate 8% in gel bid on areas other than scalp
Surgery
Surgical intervention is not recommended for the management of seborrrheic dermatitis.
Prevention
Primary Prevention
There is no established method for prevention of seborrheic dermatitis.[71]
Secondary Prevention
Secondary prevention strategies following seborrheic dermatitis include:
- Using of 1% ciclopirox shampoo once or twice weekly for 4 weeks. Shampooing once weekly or once every two weeks decreases the relapse rate of seborrheic dermatitis.[115]
- Using 2% ketoconazole such as once a week or twice a week may decrease relapse of seborrheic dermatitis.[131]
- Ketoconazole 2% shampoo may have greater prophylactic effect against relapse than selenium sulfide.[71]
References
- ↑ Shuster S (1984). "The aetiology of dandruff and the mode of action of therapeutic agents". Br J Dermatol. 111 (2): 235–42. PMID 6235835.
- ↑ Low, R. Cranston, and H. W. Barber. "Discussion on the etiology of seborrhoea and seborrhoeic dermatitis." The British Medical Journal (1922): 752-757.
- ↑ 3.0 3.1 Dessinioti C, Katsambas A (2013). "Seborrheic dermatitis: etiology, risk factors, and treatments: facts and controversies". Clin Dermatol. 31 (4): 343–51. doi:10.1016/j.clindermatol.2013.01.001. PMID 23806151.
- ↑ Dessinioti, Clio, and Andreas Katsambas. "Seborrheic dermatitis: Etiology, risk factors, and treatments:: Facts and controversies." Clinics in dermatology 31.4 (2013): 343-351.
- ↑ ===Classification by Anatomical Location===Peyri, J., and M. Lleonart. "Clinical and therapeutic profile and quality of life of patients with seborrheic dermatitis." Actas Dermo-Sifiliográficas (English Edition) 98.7 (2007): 476-482.
- ↑ name="pmid6220754">Burton JL, Pye RJ (1983). "Seborrhoea is not a feature of seborrhoeic dermatitis". Br Med J (Clin Res Ed). 286 (6372): 1169–70. PMC 1547390. PMID 6220754.
- ↑ 7.0 7.1 {{cite journal| author=Thomas DS, Ingham E, Bojar RA, Holland KT| title=In vitro modulation of human keratinocyte pro- and anti-inflammatory cytokine production by the capsule of Malassezia species. | journal=FEMS Immunol Med Microbiol | year= 2008 | volume= 54 | issue= 2 | pages= 203-14 | pmid=: 18752620 | doi=10.1111/j.1574-695X.2008.00468.x | pmc= | url=http://www.ncbi.nlm.nih.gov/entrez/eutils/elink.fcgi?
- ↑ 8.0 8.1 Schwartz RA, Janusz CA, Janniger CK (2006). "Seborrheic dermatitis: an overview". Am Fam Physician. 74 (1): 125–30. PMID 16848386.
- ↑ Dessinioti, Clio, and Andreas Katsambas. "Seborrheic dermatitis: Etiology, risk factors, and treatments:: Facts and controversies." Clinics in dermatology 31.4 (2013): 343-351.
- ↑ ===Classification by Anatomical Location===Peyri, J., and M. Lleonart. "Clinical and therapeutic profile and quality of life of patients with seborrheic dermatitis." Actas Dermo-Sifiliográficas (English Edition) 98.7 (2007): 476-482.
- ↑ 11.0 11.1 11.2 Hampshire J, Violaris N (1988). "Oral and oropharyngeal malignancies: the case for early detection". Practitioner. 232 (1452): 766. PMID 3255962.
- ↑ name="pmid6220754">Burton JL, Pye RJ (1983). "Seborrhoea is not a feature of seborrhoeic dermatitis". Br Med J (Clin Res Ed). 286 (6372): 1169–70. PMC 1547390. PMID 6220754.
- ↑ 13.0 13.1 Tajima M (2001). "Seborrhoeic dermatitis and Pityrosporum (Malassezia) folliculitis: characterization of inflammatory cells and mediators in the skin by immunohistochemistry". Br J Dermatol. 144 (3): 549–56. PMID 11260013.
- ↑ Burton JL, Pye RJ (1983). "Seborrhoea is not a feature of seborrhoeic dermatitis". Br Med J (Clin Res Ed). 286 (6372): 1169–70. PMC 1547390. PMID 6220754.
- ↑ 21.0 21.1 21.2 Sampaio AL, Mameri AC, Vargas TJ, Ramos-e-Silva M, Nunes AP, Carneiro SC (2011). "Seborrheic dermatitis". An Bras Dermatol. 86 (6): 1061–71, quiz 1072-4. PMID 22281892.
- ↑ 22.0 22.1 Burton JL, Shuster S (1970). "Effect of L-dopa on seborrhoea of parkinsonism". Lancet. 2 (7662): 19–20. PMID 4193751.
- ↑ Simon M, Tazi-Ahnini R, Jonca N, Caubet C, Cork MJ, Serre G (2008). "Alterations in the desquamation-related proteolytic cleavage of corneodesmosin and other corneodesmosomal proteins in psoriatic lesional epidermis". Br J Dermatol. 159 (1): 77–85. doi:10.1111/j.1365-2133.2008.08578.x. PMID 18460028.
- ↑ 24.0 24.1 24.2 24.3 Dill FJ, Schertzer M, Sandercock J, Tischler B, Wood S (1987). "Inverted tandem duplication generates a duplication deficiency of chromosome 8p". Clin Genet. 32 (2): 109–13. PMID 2888552.
- ↑ Birnbaum RY, Zvulunov A, Hallel-Halevy D, Cagnano E, Finer G, Ofir R; et al. (2006). "Seborrhea-like dermatitis with psoriasiform elements caused by a mutation in ZNF750, encoding a putative C2H2 zinc finger protein". Nat Genet. 38 (7): 749–51. doi:10.1038/ng1813. PMID 16751772.
- ↑ Warner, Ronald R., et al. "Dandruff has an altered stratum corneum ultrastructure that is improved with zinc pyrithione shampoo." Journal of the American Academy of Dermatology 45.6 (2001): 897-903.
- ↑ "Dermatology Atlas".
- ↑ 28.0 28.1 Druet P, Burtin P (1967). "[On the detection in renal cancers of an antigen not found in normal human kidney]". Eur J Cancer. 3 (3): 237–8. PMID 4318061.
- ↑ Hay R, Graham-Brown R (1997). "Dandruff and seborrheic dermatitis: causes and management". Clin Exp Dermatol. 22 (1): 3–6. doi:10.1046/j.1365-2230.1997.d01-231.x. PMID 9330043.
- ↑ Nowicki R (2006). "[Modern management of dandruff]". Pol Merkur Lekarski. 20 (115): 121–4. PMID 16617752.
- ↑ Am Fam Physician 2000;61:2703-10,2713-4
- ↑ Janniger C, Schwartz R (1995). "Seborrheic dermatitis". Am Fam Physician. 52 (1): 149–55, 159–60. PMID 7604759.
- ↑ Parry M, Sharpe G (1998). "Seborrheic dermatitis is not caused by an altered immune response to Malassezia yeast". Br J Dermatol. 139 (2): 254–63. doi:10.1046/j.1365-2133.1998.02362.x. PMID 9767239.
- ↑ "MedlinePlus Medical Encyclopedia: Hypervitaminosis A". www.nlm.nih.gov. Retrieved 2008-03-19.
- ↑ 35.0 35.1 35.2 "Seborrheic Dermatitis: An Overview - July 1, 2006 -- American Family Physician". www.aafp.org. Retrieved 2008-03-19.
- ↑ "eMedicine - Nutritional Neuropathy : Article by R Andrew Sewell". www.emedicine.com. Retrieved 2008-03-19.
- ↑ Naldi, Luigi, and Alfredo Rebora. "Seborrheic dermatitis." New England Journal of Medicine 360.4 (2009): 387-396.
- ↑ Braun-Falco O, Heilgemeir GP, Lincke-Plewig H (1979). "[Histological differential diagnosis of psoriasis vulgaris and seborrheic eczema of the scalp]". Hautarzt. 30 (9): 478–83. PMID 161301.
- ↑ Rosina P, Zamperetti MR, Giovannini A, Girolomoni G (2007). "Videocapillaroscopy in the differential diagnosis between psoriasis and seborrheic dermatitis of the scalp". Dermatology. 214 (1): 21–4. doi:10.1159/000096908. PMID 17191043.
- ↑ Schwartz, Robert A., Christopher A. Janusz, and Camila K. Janniger. "Seborrheic dermatitis: an overview." Am Fam Physician 74.1 (2006): 125-130.
- ↑ 41.0 41.1 Clark GW, Pope SM, Jaboori KA (2015). "Diagnosis and treatment of seborrheic dermatitis". Am Fam Physician. 91 (3): 185–90. PMID 25822272.
- ↑ "Mycosis Fungoides and the Sézary Syndrome Treatment (PDQ®)—Patient Version - National Cancer Institute".
- ↑ Mahajan K, Relhan V, Relhan AK, Garg VK (2016). "Pityriasis Rosea: An Update on Etiopathogenesis and Management of Difficult Aspects". Indian J Dermatol. 61 (4): 375–84. doi:10.4103/0019-5154.185699. PMC 4966395. PMID 27512182.
- ↑ Prantsidis A, Rigopoulos D, Papatheodorou G, Menounos P, Gregoriou S, Alexiou-Mousatou I, Katsambas A (2009). "Detection of human herpesvirus 8 in the skin of patients with pityriasis rosea". Acta Derm. Venereol. 89 (6): 604–6. doi:10.2340/00015555-0703. PMID 19997691.
- ↑ Smith KJ, Nelson A, Skelton H, Yeager J, Wagner KF (1997). "Pityriasis lichenoides et varioliformis acuta in HIV-1+ patients: a marker of early stage disease. The Military Medical Consortium for the Advancement of Retroviral Research (MMCARR)". Int. J. Dermatol. 36 (2): 104–9. PMID 9109005.
- ↑ Jiamton S, Tangjaturonrusamee C, Kulthanan K (2013). "Clinical features and aggravating factors in nummular eczema in Thais". Asian Pac. J. Allergy Immunol. 31 (1): 36–42. PMID 23517392.
- ↑ "STD Facts - Syphilis".
- ↑ Neagu TP, Ţigliş M, Botezatu D, Enache V, Cobilinschi CO, Vâlcea-Precup MS, GrinŢescu IM (2017). "Clinical, histological and therapeutic features of Bowen's disease". Rom J Morphol Embryol. 58 (1): 33–40. PMID 28523295.
- ↑ Murao K, Yoshioka R, Kubo Y (2014). "Human papillomavirus infection in Bowen disease: negative p53 expression, not p16(INK4a) overexpression, is correlated with human papillomavirus-associated Bowen disease". J. Dermatol. 41 (10): 878–84. doi:10.1111/1346-8138.12613. PMID 25201325.
- ↑ Szatkowski J, Schwartz RA (2015). "Acute generalized exanthematous pustulosis (AGEP): A review and update". J. Am. Acad. Dermatol. 73 (5): 843–8. doi:10.1016/j.jaad.2015.07.017. PMID 26354880.
- ↑ Schmid S, Kuechler PC, Britschgi M, Steiner UC, Yawalkar N, Limat A, Baltensperger K, Braathen L, Pichler WJ (2002). "Acute generalized exanthematous pustulosis: role of cytotoxic T cells in pustule formation". Am. J. Pathol. 161 (6): 2079–86. doi:10.1016/S0002-9440(10)64486-0. PMC 1850901. PMID 12466124.
- ↑ Ankad BS, Beergouder SL (2016). "Hypertrophic lichen planus versus prurigo nodularis: a dermoscopic perspective". Dermatol Pract Concept. 6 (2): 9–15. doi:10.5826/dpc.0602a03. PMC 4866621. PMID 27222766.
- ↑ Shengyuan L, Songpo Y, Wen W, Wenjing T, Haitao Z, Binyou W (2009). "Hepatitis C virus and lichen planus: a reciprocal association determined by a meta-analysis". Arch Dermatol. 145 (9): 1040–7. doi:10.1001/archdermatol.2009.200. PMID 19770446.
- ↑ Lutz ME, Daoud MS, McEvoy MT, Gibson LE (1998). "Subcorneal pustular dermatosis: a clinical study of ten patients". Cutis. 61 (4): 203–8. PMID 9564592.
- ↑ Kasha EE, Epinette WW (1988). "Subcorneal pustular dermatosis (Sneddon-Wilkinson disease) in association with a monoclonal IgA gammopathy: a report and review of the literature". J. Am. Acad. Dermatol. 19 (5 Pt 1): 854–8. PMID 3056995.
- ↑ Delaporte E, Colombel JF, Nguyen-Mailfer C, Piette F, Cortot A, Bergoend H (1992). "Subcorneal pustular dermatosis in a patient with Crohn's disease". Acta Derm. Venereol. 72 (4): 301–2. PMID 1357895.
- ↑ Sauder MB, Glassman SJ (2013). "Palmoplantar subcorneal pustular dermatosis following adalimumab therapy for rheumatoid arthritis". Int. J. Dermatol. 52 (5): 624–8. doi:10.1111/j.1365-4632.2012.05707.x. PMID 23489057.
- ↑ Lambert WC, Everett MA (1981). "The nosology of parapsoriasis". J. Am. Acad. Dermatol. 5 (4): 373–95. PMID 7026622.
- ↑ Väkevä L, Sarna S, Vaalasti A, Pukkala E, Kariniemi AL, Ranki A (2005). "A retrospective study of the probability of the evolution of parapsoriasis en plaques into mycosis fungoides". Acta Derm. Venereol. 85 (4): 318–23. doi:10.1080/00015550510030087. PMID 16191852.
- ↑ Janniger CK, Schwartz RA, Szepietowski JC, Reich A (2005). "Intertrigo and common secondary skin infections". Am Fam Physician. 72 (5): 833–8. PMID 16156342.
- ↑ Satter EK, High WA (2008). "Langerhans cell histiocytosis: a review of the current recommendations of the Histiocyte Society". Pediatr Dermatol. 25 (3): 291–5. doi:10.1111/j.1525-1470.2008.00669.x. PMID 18577030.
- ↑ Stull MA, Kransdorf MJ, Devaney KO (1992). "Langerhans cell histiocytosis of bone". Radiographics. 12 (4): 801–23. doi:10.1148/radiographics.12.4.1636041. PMID 1636041.
- ↑ Sholl LM, Hornick JL, Pinkus JL, Pinkus GS, Padera RF (2007). "Immunohistochemical analysis of langerin in langerhans cell histiocytosis and pulmonary inflammatory and infectious diseases". Am. J. Surg. Pathol. 31 (6): 947–52. doi:10.1097/01.pas.0000249443.82971.bb. PMID 17527085.
- ↑ Grois N, Pötschger U, Prosch H, Minkov M, Arico M, Braier J, Henter JI, Janka-Schaub G, Ladisch S, Ritter J, Steiner M, Unger E, Gadner H (2006). "Risk factors for diabetes insipidus in langerhans cell histiocytosis". Pediatr Blood Cancer. 46 (2): 228–33. doi:10.1002/pbc.20425. PMID 16047354.
- ↑ Al Hasan M, Fitzgerald SM, Saoudian M, Krishnaswamy G (2004). "Dermatology for the practicing allergist: Tinea pedis and its complications". Clin Mol Allergy. 2 (1): 5. doi:10.1186/1476-7961-2-5. PMC 419368. PMID 15050029.
- ↑ 66.0 66.1 Misery L, Touboul S, Vinçot C, Dutray S, Rolland-Jacob G, Consoli SG, Farcet Y, Feton-Danou N, Cardinaud F, Callot V, De La Chapelle C, Pomey-Rey D, Consoli SM (2007). "[Stress and seborrheic dermatitis]". Ann Dermatol Venereol (in French). 134 (11): 833–7. PMID 18033062.
- ↑ 67.0 67.1 Gupta AK, Bluhm R (2004). "Seborrheic dermatitis". J Eur Acad Dermatol Venereol. 18 (1): 13–26, quiz 19-20. PMID 14678527.
- ↑ Moehrle M, Dennenmoser B, Schlagenhauff B, Thomma S, Garbe C (2000). "High prevalence of seborrhoeic dermatitis on the face and scalp in mountain guides". Dermatology. 201 (2): 146–7. doi:18458 Check
|doi=value (help). PMID 11053918. - ↑ Naldi, Luigi, and Alfredo Rebora. "Seborrheic dermatitis." New England Journal of Medicine 360.4 (2009): 387-396
- ↑ Denton, C. P., et al. "Scleroderma (systemic sclerosis)." Fitzpatrick’s Dermatology in General Medicine. 7th ed. New York, NY: McGraw-Hill Medical Publishing Division (2008): 1553-1562
- ↑ 71.0 71.1 71.2 71.3 71.4 71.5 71.6 Okochi T, Seike H, Saeki K, Sumikawa K, Yamamoto T, Higashino K (1987). "A novel alkaline phosphatase isozyme in human adipose tissue". Clin Chim Acta. 162 (1): 19–27. PMID 3100109.
- ↑ Sachdeva M, Kaur S, Nagpal M, Dewan SP (2002). "Cutaneous lesions in new born". Indian J Dermatol Venereol Leprol. 68 (6): 334–7. PMID 17656992.
- ↑ Naldi, Luigi, and Alfredo Rebora. "Seborrheic dermatitis." New England Journal of Medicine 360.4 (2009): 387-396.
- ↑ Naldi, Luigi, and Alfredo Rebora. "Seborrheic dermatitis." New England Journal of Medicine 360.4 (2009): 387-396.
- ↑ name="pmid12956195">Gupta AK, Bluhm R, Cooper EA, Summerbell RC, Batra R (2003). "Seborrheic dermatitis". Dermatol Clin. 21 (3): 401–12. PMID 12956195.
- ↑ Mahé, Antoine, et al. "Predictive value of seborrheic dermatitis and other common dermatoses for HIV infection in Bamako, Mali." Journal of the American Academy of Dermatology 34.6 (1996):
- ↑ Hastings GB, Leathar DS, Scott AC (1988). "Scottish attitudes to AIDS". Br Med J (Clin Res Ed). 296 (6627): 991–2. PMC 2545449. PMID 3129121.
- ↑ 78.0 78.1 Dunic I, Vesic S, Jevtovic DJ (2004). "Oral candidiasis and seborrheic dermatitis in HIV-infected patients on highly active antiretroviral therapy". HIV Med. 5 (1): 50–4. PMID 14731170.
- ↑ Soldatov IuN, Glushko AV (1974). "[Spontaneous rupture of the epigastric arteries simulating acute abdomen]". Klin Khir (11): 61–2. PMID 4280471.
- ↑ Özcan D, Seçkin D, Ada S, Haberal M (2013). "Mucocutaneous disorders in renal transplant recipients receiving sirolimus-based immunosuppressive therapy: a prospective, case-control study". Clin Transplant. 27 (5): 742–8. doi:10.1111/ctr.12215. PMID 23991694 : 23991694 Check
|pmid=value (help). - ↑ Baran, Robert, and Howard Maibach, eds. Textbook of cosmetic dermatology. CRC Press, 2010.
- ↑ Dowlati, Bijan, et al. "Insulin quantification in patients with seborrheic dermatitis." Archives of dermatology 134.8 (1998): 1043-1045.
- ↑ Banerjee S, Gangopadhyay DN, Jana S, Chanda M (2010). "Seasonal variation in pediatric dermatoses". Indian J Dermatol. 55 (1): 44–6. doi:10.4103/0019-5154.60351. PMC 2856373. PMID 20418977.
- ↑ US preventive service task force.seborrheic dermatitis. http://www.uspreventiveservicestaskforce.org/accessed on August16, 2016
- ↑ Tedder JM (1989). "New Zealand Society of Physiotherapists, court of appeal and ACC". N Z Med J. 102 (875): 483. PMID 2528704.
- ↑ Gorman CR, White SW (2005). "Rosaceiform dermatitis as a complication of treatment of facial seborrheic dermatitis with 1% pimecrolimus cream". Arch Dermatol. 141 (9): 1168. doi:10.1001/archderm.141.9.1168. PMID 16172323.
- ↑ Guin JD (2004). "Eyelid dermatitis: a report of 215 patients". Contact Dermatitis. 50 (2): 87–90. doi:10.1111/j.0105-1873.2004.00311.x. PMID 15128319.
- ↑ Ooi ET, Tidman MJ (2014). "Improving the management of seborrhoeic dermatitis". Practitioner. 258 (1768): 23–6, 3. PMID 24689165.
- ↑ Ross, Elizabeth K., Colombina Vincenzi, and Antonella Tosti. "Videodermoscopy in the evaluation of hair and scalp disorders." Journal of the American Academy of Dermatology 55.5 (2006): 799-806.
- ↑ Foley P, Zuo Y, Plunkett A, Merlin K, Marks R (2003). "The frequency of common skin conditions in preschool-aged children in Australia: seborrheic dermatitis and pityriasis capitis (cradle cap)". Arch Dermatol. 139 (3): 318–22. PMID 12622623.
- ↑ Forrestel AK, Kovarik CL, Mosam A, Gupta D, Maurer TA, Micheletti RG (2016). "Diffuse HIV-associated seborrheic dermatitis - a case series". Int J STD AIDS. doi:10.1177/0956462416641816. PMID 27013615.
- ↑ Schwartz, Robert A., Christopher A. Janusz, and Camila K. Janniger. "Seborrheic dermatitis: an overview." Am Fam Physician 74.1 (2006): 125-130
- ↑ Tsao BP, Aldo-Benson MA (1985). "Macrophage-derived soluble factors mediate suppression induced by 2,4-dinitrophenyl-conjugated mouse IgG in hybridoma cells". Cell Immunol. 91 (2): 362–74. PMID 3995588.
- ↑ Rola-Pleszczynski M (1985). "Differential effects of leukotriene B4 on T4+ and T8+ lymphocyte phenotype and immunoregulatory functions". J Immunol. 135 (2): 1357–60. PMID 2861228.
- ↑ Borda LJ, Wikramanayake TC. Seborrheic Dermatitis and Dandruff: A Comprehensive Review. Journal of clinical and investigative dermatology. 2015;3(2):10.13188/2373-1044.1000019.
- ↑ Muñoz-Pérez MA, Rodriguez-Pichardo A, Camacho F, Colmenero MA (1998). "Dermatological findings correlated with CD4 lymphocyte counts in a prospective 3 year study of 1161 patients with human immunodeficiency virus disease predominantly acquired through intravenous drug abuse". Br J Dermatol. 139 (1): 33–9. PMID 9764146.
- ↑ Bilgili SG, Akdeniz N, Karadag AS, Akbayram S, Calka O, Ozkol HU (2011). "Mucocutaneous disorders in children with down syndrome: case-controlled study". Genet Couns. 22 (4): 385–92. PMID 22303799.
- ↑ Baş Y, Seçkin HY, Kalkan G, Takci Z, Çitil R, Önder Y; et al. (2016). "Prevalence and related factors of psoriasis and seborrheic dermatitis: a community-based study". Turk J Med Sci. 46 (2): 303–9. doi:10.3906/sag-1406-51. PMID 27511489.
- ↑ Sarkar R, Garg VK (2010). "Erythroderma in children". Indian J Dermatol Venereol Leprol. 76 (4): 341–7. doi:10.4103/0378-6323.66576. PMID 20657113.
- ↑ 100.0 100.1 Soeprono FF, Schinella RA, Cockerell CJ, Comite SL (1986). "Seborrheic-like dermatitis of acquired immunodeficiency syndrome. A clinicopathologic study". J Am Acad Dermatol. 14 (2 Pt 1): 242–8. PMID 2936776.
- ↑ Mathes BM, Douglass MC (1985). "Seborrheic dermatitis in patients with acquired immunodeficiency syndrome". J Am Acad Dermatol. 13 (6): 947–51. PMID 2934444.
- ↑ Dermatology Atlas. Seborrheic dermatitis(2016) http://www.atlasdermatologico.com.br/disease.jsf?diseaseId=424 Accessed on Aug22, 2016
- ↑ Borda, Luis J., and Tongyu C. Wikramanayake. "Seborrheic Dermatitis and Dandruff: A Comprehensive Review." Journal of clinical and investigative dermatology 3.2 (2015).
- ↑ Tüzün Y, Wolf R, Bağlam S, Engin B (2015). "Diaper (napkin) dermatitis: A fold (intertriginous) dermatosis". Clin Dermatol. 33 (4): 477–82. doi:10.1016/j.clindermatol.2015.04.012. PMID 26051065.
- ↑ Fischer HG, Hartmann U, Becker R, Kommans B, Mader A, Hollmann W (1992). "The excretion of 17-ketosteroids and 17-hydroxycorticosteroids in night urine of elite rowers during altitude training". Int J Sports Med. 13 (1): 15–20. doi:10.1055/s-2007-1021227. PMID 1544726.
- ↑ Sonea MJ, Moroz BE, Reece ER (1987). "Leiner's disease associated with diminished third component of complement". Pediatr Dermatol. 4 (2): 105–7. PMID 2958789.
- ↑ Evans DI, Holzel A, MacFarlane H (1977). "Yeast opsonization defect and immunoglobulin deficiency in severe infantile dermatitis (Leiner's disease)". Arch Dis Child. 52 (9): 691–5. PMC 1544726. PMID 144462.
- ↑ Bukvić, Mokos Z., et al. "Seborrheic dermatitis: an update." Acta dermatovenerologica Croatica: ADC 20.2 (2011): 98-104.
- ↑ Mathes, Barbara M., and Margaret C. Douglass. "Seborrheic dermatitis in patients with acquired immunodeficiency syndrome." Journal of the American Academy of Dermatology 13.6 (1985): 947-951.
- ↑ Foley, Peter, et al. "The frequency of common skin conditions in preschool-age children in Australia: atopic dermatitis." Archives of dermatology 137.3 (2001): 293-300.
- ↑ Yasuda G, Sun L, Umemura S, Pettinger WA, Jeffries WB (1991). "Characterization of prazosin-sensitive alpha 2 B-adrenoceptors expressed by cultured rat IMCD cells". Am J Physiol. 261 (5 Pt 2): F760–6. PMID 1719824.
- ↑ Wannanukul S, Chiabunkana J (2004). "Comparative study of 2% [[ketoconazole]] cream and 1% hydrocortisone cream in the treatment of infantile seborrheic dermatitis". J Med Assoc Thai. 87 Suppl 2: S68–71. PMID 16083165. URL–wikilink conflict (help)
- ↑ Reygagne P, Poncet M, Sidou F, Soto P (2007). "Clobetasol propionate shampoo 0.05% in the treatment of seborrheic dermatitis of the scalp: results of a pilot study". Cutis. 79 (5): 397–403. PMID 17569404.
- ↑ Peter RU, Richarz-Barthauer U (1995). "Successful treatment and prophylaxis of scalp seborrhoeic dermatitis and dandruff with 2% ketoconazole shampoo: results of a multicentre, double-blind, placebo-controlled trial". Br J Dermatol. 132 (3): 441–5. PMID 7718463.
- ↑ 115.0 115.1 Shuster S, Meynadier J, Kerl H, Nolting S (2005). "Treatment and prophylaxis of seborrheic dermatitis of the scalp with antipityrosporal 1% ciclopirox shampoo". Arch Dermatol. 141 (1): 47–52. doi:10.1001/archderm.141.1.47. PMID 15655141.
- ↑ 116.0 116.1 Kastarinen H, Oksanen T, Okokon EO, Kiviniemi VV, Airola K, Jyrkkä J; et al. (2014). "Topical anti-inflammatory agents for seborrhoeic dermatitis of the face or scalp". Cochrane Database Syst Rev (5): CD009446. doi:10.1002/14651858.CD009446.pub2. PMID 24838779.
- ↑ Faergemann, J. "Pharmacology and Treatment Seborrhoeic dermatitis and Pityrosporumorbiculare: treatment of seborrhoeic dermatitis of the scalp with miconazole‐hydrocortisone (Daktacort), miconazole and hydrocortisone." British journal of dermatology 114.6 (1986): 695-700.
- ↑ Ballanger F, Tenaud I, Volteau C, Khammari A, Dréno B (2008). "Anti-inflammatory effects of lithium gluconate on keratinocytes: a possible explanation for efficiency in seborrhoeic dermatitis". Arch Dermatol Res. 300 (5): 215–23. doi:10.1007/s00403-007-0824-z. PMID 18330588.
- ↑ Dreno B, Moyse D (2002). "Lithium gluconate in the treatment of seborrhoeic dermatitis: a multicenter, randomised, double-blind study versus placebo". Eur J Dermatol. 12 (6): 549–52. PMID 12459525.
- ↑ "A double-blind, placebo-controlled, multicenter trial of lithium succinate ointment in the treatment of seborrheic dermatitis. Efalith Multicenter Trial Group". J Am Acad Dermatol. 26 (3 Pt 2): 452–7. 1992. PMID 1532964.
- ↑ Zisova LG (2009). "Treatment of Malassezia species associated seborrheic blepharitis with fluconazole". Folia Med (Plovdiv). 51 (3): 57–9. PMID 19957565.
- ↑ Young Jr, A. W. "Seborrhea in the geriatric patient: incidence, implication, management." Geriatrics 24.3 (1969): 144-150.
- ↑ Gupta, Aditya K., Karyn Nicol, and Roma Batra. "Role of antifungal agents in the treatment of seborrheic dermatitis." American journal of clinical dermatology 5.6 (2004): 417-422.
- ↑ Shin, Hyoseung, et al. "Clinical efficacies of topical agents for the treatment of seborrheic dermatitis of the scalp: a comparative study." The Journal of dermatology 36.3 (2009): 131-137.
- ↑ Braza TJ, DiCarlo JB, Soon SL, McCall CO (2003). "Tacrolimus 0.1% ointment for seborrhoeic dermatitis: an open-label pilot study". Br J Dermatol. 148 (6): 1242–4. PMID 12828755.
- ↑ Collins, Chris D., and Chad Hivnor. "Seborrheic dermatitis." management 41 (1988): 182-186.
- ↑ Geißler, Sabine E., Silke Michelsen, and Gerd Plewig. "Very low dose isotretinoin is effective in controlling seborrhea." JDDG: Journal der Deutschen Dermatologischen Gesellschaft 1.12 (2003): 952-958.
- ↑ Stevens DL, Bisno AL, Chambers HF, Dellinger EP, Goldstein EJ, Gorbach SL; et al. (2014). "Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the infectious diseases society of America". Clin Infect Dis. 59 (2): 147–59. doi:10.1093/cid/ciu296. PMID 24947530.
- ↑ "WHO Monographs on Selected Medicinal Plants - Volume 1: Aloe Vera Gel". www.who.int. Retrieved 2008-03-18.
- ↑ 130.0 130.1 130.2 130.3 130.4 130.5 130.6 "The Green Pharmacy: New Discoveries ... - Google Book Search". books.google.com. Retrieved 2008-03-19.
- ↑ Piérard-Franchimont C, Piérard GE, Arrese JE, De Doncker P (2001). "Effect of ketoconazole 1% and 2% shampoos on severe dandruff and seborrhoeic dermatitis: clinical, squamometric and mycological assessments". Dermatology. 202 (2): 171–6. doi:51628 Check
|doi=value (help). PMID 11306850.