Electrical conduction system of the heart
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor-In-Chief: Cafer Zorkun, M.D., Ph.D. [2]
Overview
The normal electrical conduction in the heart allows the impulse that is generated by the sinoatrial node (SA node) of the heart to be propagated to (and stimulate) the myocardium (Cardiac muscle). The myocardium contracts after stimulation. It is the ordered stimulation of the myocardium that allows efficient contraction of the heart, thereby allowing blood to be pumped throughout the body.
Requirements for effective pumping
In order to maximize efficiency of contraction and cardiac output, the conduction system of the heart has:
- Substantial atrial to ventricular delay. This allows the atria to completely empty their contents into the ventricles; simultaneous contraction would cause inefficient filling and backflow. The atria are electrically isolated from the ventricles, connected only via the AV node which briefly delays the signal.
- Coordinated contraction of ventricular cells. The ventricles must maximize systolic pressure to force blood through the circulation, so all the ventricular cells must work together.
- Ventricular contraction begins at the apex of the heart, progressing upwards to eject blood into the great arteries. Contraction that squeezes blood towards the exit is more efficient than a simple squeeze from all directions. Although the ventricular stimulus originates from the AV node in the wall separating the atria and ventricles, the Bundle of His conducts the signal to the apex.
- Depolarization propagates through cardiac muscle very rapidly. Cells of the ventricles contract nearly simultaneously.
- The action potentials of cardiac muscle are unusually sustained. This prevents premature relaxation, maintaining initial contraction until the entire myocardium has had time to depolarize and contract.
- Absence of tetany. After contracting, the heart must relax to fill up again. Sustained contraction of the heart without relaxation would be fatal, and this is prevented by a temporary inactivation of certain ion channels.
Electrochemical Mechanism
- See main article: Cardiac action potential
Cardiac muscle has some similarities to neurons and skeletal muscle, as well as important unique properties. Like a neuron, a given myocardial cell has a negative membrane potential when at rest. Stimulation above a threshold value induces the opening of voltage-gated ion channels and a flood of cations into the cell. The positively charged ions entering the cell cause the depolarization characteristic of an action potential. Like skeletal muscle, depolarization causes the opening of voltage-gated calcium channels and release of Ca2+ from the t-tubules. This influx of calcium causes calcium-induced calcium release from the sarcoplasmic reticulum, and free Ca2+ causes muscle contraction. After a delay (the absolute refractory period), Potassium channels reopen and the resulting flow of K+ out of the cell causes repolarization to the resting state.
Note that there are important physiological differences between nodal cells and ventricular cells; the specific differences in ion channels and mechanisms of polarization give rise to unique properties of SA node cells, most importantly the spontaneous depolarizations necessary for the SA node's pacemaker activity .
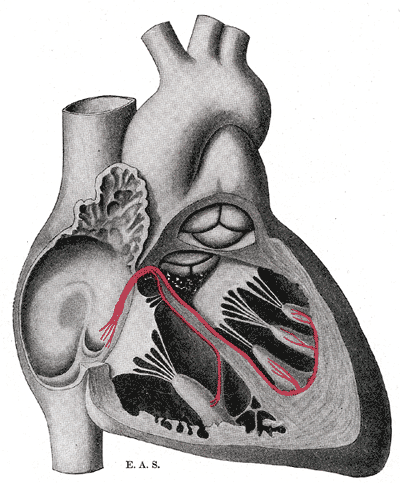
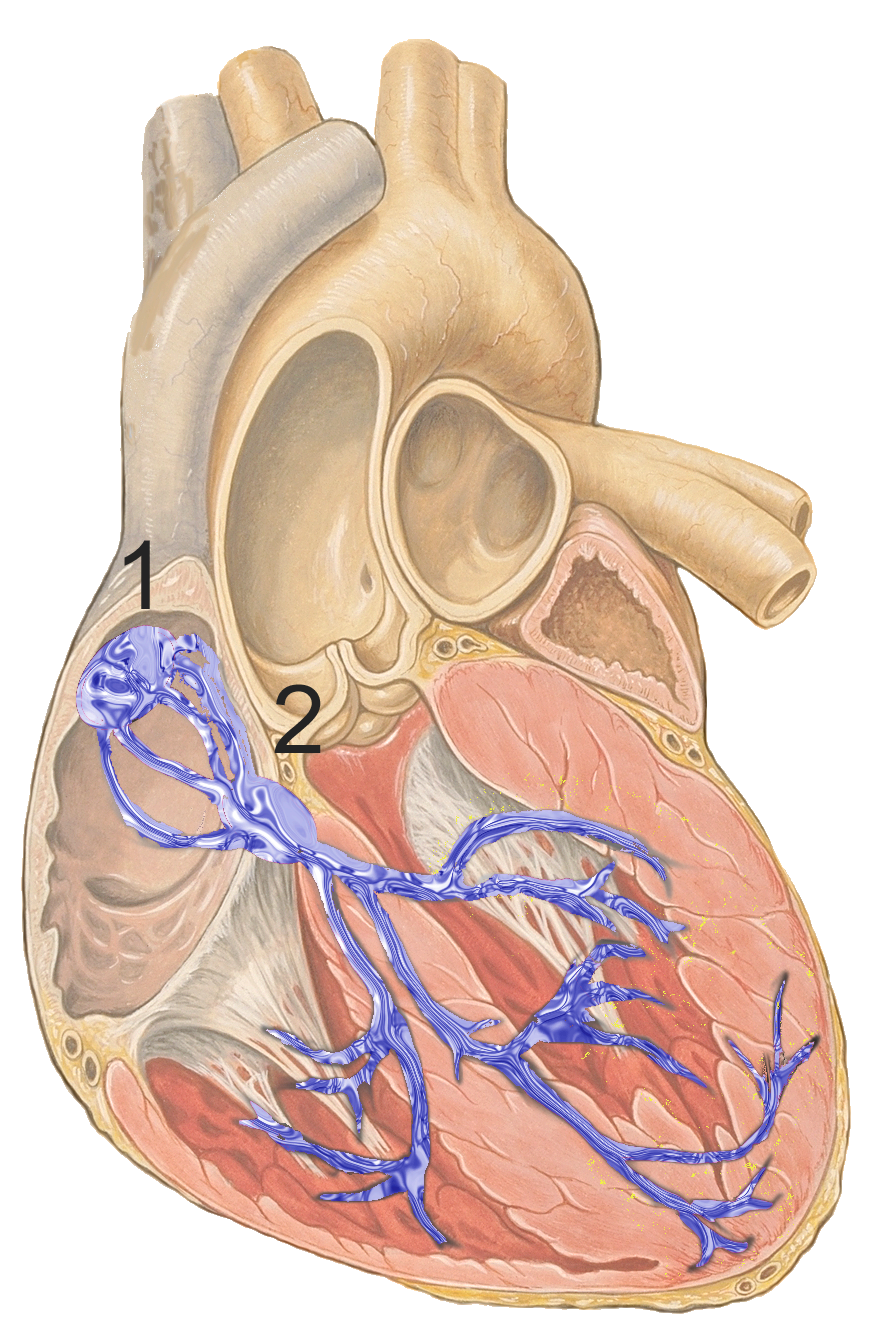
Conduction pathway
Signals arising in the SA node stimulate the atria to contract and travel to the AV node. After a delay, the stimulus is conducted through the bundle of His to the Purkinje fibers and the endocardium at the apex of the heart, then finally to the ventricular epicardium.
Microscopically, the wave of depolarization propagates to adjacent cells via gap junctions located on the intercalated disk. The heart is a syncytium: electrical impulses propagate freely between cells in every direction, so that the myocardiam functions as a single contractile unit. This property allows rapid, synchronous depolarization of the myocardium. While normally advantageous, this property can be detrimental as it potentially allows the propagation of incorrect electrical signals. These gap junctions can close to isolate damaged or dying tissue, as in a myocardial infarction.
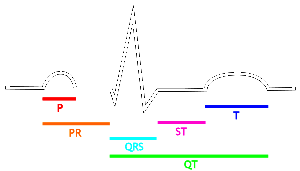
Depolarization and the ECG
- See also: Electrocardiogram
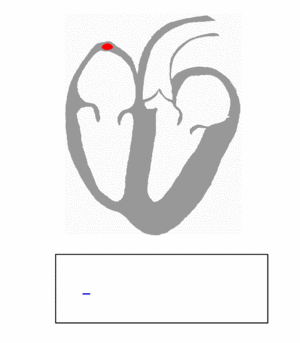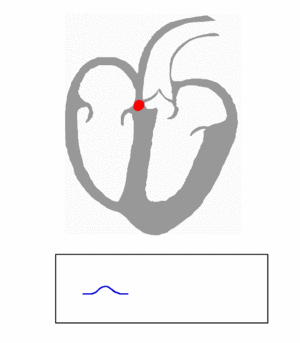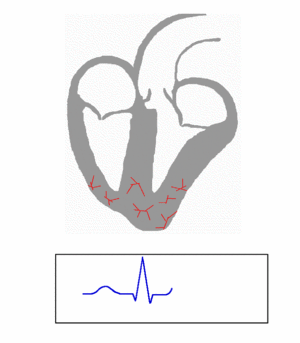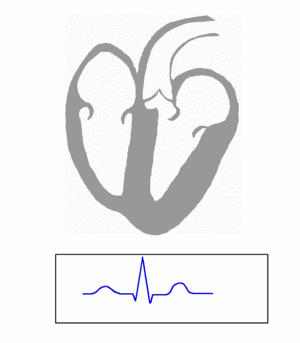
SA node: P wave
Under normal conditions, electrical activity is spontaneously generated by the SA node, the physiological pacemaker. This electrical impulse is propagated throughout the right and left atria, stimulating the myocardium of the atria to contract. The conduction of the electrical impulse throughout the atria is seen on the ECG as the P wave.
As the electrical activity is spreading throughout the atria, it travels via specialized pathways, known as internodal tracts, from the SA node to the AV node.
AV node/Bundles: PR interval
The AV node functions as a critical delay in the conduction system. Without this delay, the atria and ventricles would contract at the same time, and blood wouldn't flow effectively from the atria to the ventricles. The delay in the AV node forms much of the PR segment on the ECG. And part of atrial repolarization can be represented by PR segment.
The distal portion of the AV node is known as the Bundle of His. The Bundle of His splits into two branches in the interventricular septum, the left bundle branch and the right bundle branch. The left bundle branch activates the left ventricle, while the right bundle branch activates the right ventricle. The left bundle branch is short, splitting into the left anterior fascicle and the left posterior fascicle. The left posterior fascicle is relatively short and broad, with dual blood supply, making it particularly resistant to ischemic damage.
Purkinje fibers/ventricular myocardium: QRS complex
The two bundle branches taper out to produce numerous Purkinje fibers, which stimulate individual groups of myocardial cells to contract.
The spread of electrical activity through the ventricular myocardium produces the QRS complex on the ECG.
Ventricular repolarization: T wave
The last event of the cycle is the repolarization of the ventricles.
Normal Sinus Rhythm and Junctional Rhythms
An impulse (action potential) that originates from the SA node at a rate of 60 - 100 beats/minute (bpm) is known as normal sinus rhythm. If SA nodal impulses occur at a rate less than 60 bpm, the heart rhythm is known as sinus bradycardia. If SA nodal impulse occur at a rate exceeding 100 bpm, the consequent rapid heart rate is sinus tachycardia. Sinus bradycardia may not always be indicative of disease. Trained athletes, for example, often have heart rates < 60 bpm when not exercising. If the SA node fails to initialize the AV Junction can take over as the main pacemaker of the heart. The AV Junction "surrounds" the AV node (the AV node is not able to initialize its own impulses) and has a regular rate of 40 to 60 bpm. These "Junctional" rhythms are characterized by a missing or inverted P Wave. If both the SA node and the AV Junction fail to initialize the electrical impulse, the ventricles can fire the electrical impulses themselves at a rate of 20 to 40 bpm and will have a QRS complex of greater than 0.12 seconds.
See also
- Bradycardia
- Cardiac pacemaker
- Electrocardiogram (ECG)
- Tachycardia
- Circle map -- simplified mathematical model of the beating heart.