Heart failure resident survival guide
For acute heart failure prevention click here.
Editor-In-Chief: C. Michael Gibson, M.S., M.D. [1]; Associate Editor(s)-in-Chief: Mahmoud Sakr, M.D. [2]; Ayokunle Olubaniyi, M.B,B.S [3]; Rim Halaby, M.D. [4]
| Acute Heart Failure Resident Survival Guide Microchapters |
|---|
| Overview |
| Classification |
| Causes |
| FIRE |
| Diagnosis |
| Treatment
Stage A and B |
| Do's |
| Don'ts |
Overview
Heart failure is a complex syndrome characterized by inadequate blood ejection or impaired ventricular filling, leading to the inability of the heart to pump blood to meet the metabolic demands of the body. Heart failure is a clinical syndrome for which the diagnosis relies mainly on symptoms and physical examination findings. The main symptoms and signs of heart failure are dyspnea, volume overload (leading to pulmonary edema and/or peripheral edema), fatigue, and exercise intolerance. Acute decompensated heart failure (ADHF) is a life-threatening condition that can occur in the setting of a new onset heart failure or worsening of an existing chronic heart failure. Symptoms of ADHF may include dyspnea secondary to pulmonary edema, peripheral edema, hypotension, and impaired end organ perfusion that can manifest by worsening renal function, altered mental status, and cold clammy extremities. The mainstays of treatment of ADHF are 1) oxygen therapy to improve hypoxia, 2) diuresis to reduce both preload and intravascular volume, and 3) vasodilators to reduce afterload. The goals of treatment for chronic heart failure are to relieve symptoms, decrease hospitalization rate, and decrease morbidity and mortality. Treatment of heart failure includes identification and management of precipitating factors, lifestyle changes, pharmacological therapy, and devices.
Classification
Classification by Severity of Congestive Heart Failure
Shown below is a table comparing American College of Cardiology Foundation/American Heart Association (ACCF/AHA) stages to New York Heart Association (NYHA) classification of severity of heart failure.[1]
| ACCF/AHA Stages | New York Heart Association (NYHA) Classification | ||
| Stage | Interpretation | Class | Interpretation |
| A | At high risk for heart failure (HF) but without structural heart disease or symptoms of HF | - | - |
| B | Structural heart disease but without signs or symptoms of HF | I | No limitation of physical activity. Ordinary physical activity does not cause symptoms of HF |
| C | Structural heart disease with prior or current symptoms of HF | I | No limitation of physical activity. Ordinary physical activity does not cause symptoms of HF |
| II | Slight limitation of physical activity. Comfortable at rest, but ordinary physical activity results in symptoms of HF | ||
| III | Marked limitation of physical activity. Comfortable at rest, but less than ordinary activity causes symptoms of HF | ||
| IV | Unable to carry on any physical activity without symptoms of HF, or symptoms of HF at rest | ||
| D | Refractory HF requiring specialized interventions | IV | Unable to carry on any physical activity without symptoms of HF, or symptoms of HF at rest |
Classification by Other Factors
Left Ventricular Ejection Fraction (LVEF)
- Heart failure with reduced ejection fraction (HFrEF) or systolic heart failure: ejection fraction (EF) ≤40%
- Heart failure with preserved ejection fraction (HFpEF) or diastolic heart failure: EF ≥50%
- Borderline HFpEF: EF between 41 to 49%
- Improved HFpEF: EF >40% following a HFrEF
Cardiac Output
- Low cardiac output
- High stroke volume with/without cardiac output
Left vs. Right Sided
- Left sided: Pulmonary edema
- Right sided: Peripheral edema, elevated jugular venous pressure, hepatomegaly
Backwards vs. Forward
- Backwards: Congestion, elevated filling pressure
- Forwards: Low systemic perfusion
Causes
Life Threatening Causes
Acute decompensated heart failure is life threatening and should be treated as such irrespective of the underlying cause.
Common Causes
- Acute coronary syndrome
- Acute kidney injury
- Acute severe myocarditis
- Cardiac arrhythmias
- Cardiomyopathy
- Cardiotoxic agents - alcohol, cocaine
- Decompensation of an underlying chronic heart failure
- Hypertensive crisis
- Pulmonary embolus
- Systemic Inflammatory response syndrome
- Valvular heart disease
Click here for the complete list of causes.
FIRE: Focused Initial Rapid Evaluation
A Focused Initial Rapid Evaluation (FIRE) should be performed to identify patients of severe acute decompensated heart failure in need of immediate intervention.[1]
Boxes in red signify that an urgent management is needed.
Abbreviations:
BU: Blood urea nitrogen;
COPD: Chronic obstructive pulmonary disease;
D5W: 5% dextrose solution in water ;
HF: Heart failure;
IV: Intravenous;
MAP: Mean arterial pressure;
Na: Sodium;
NSAID: Non steroidal anti-inflammatory drug;
SBP: Systolic blood pressure;
S3: Third heart sound;
Identify cardinal findings that increase the pretest probability of acute decompensated heart failure ❑ Dyspnea | |||||||||||||||||
Does the patient have any of the following findings that require hospitalization and urgent management? ❑ Severe decompendated HF:
❑ Dyspnea at rest manifested by tachypnea or oxygen saturation <90% | |||||||||||||||||
Yes | No | ||||||||||||||||
Admit to to a level of care that allows for constant ECG monitoring given the risk of arrhythmia | |||||||||||||||||
Initial stabilization: Assess congestion and perfusion: Identify precipitating factor and treat accordingly:
❑ COPD Treat congestion and optimize volume status:
❑ Low sodium diet (<2 g daily)
❑ Consider low dose dopamine infusion for improved diuresis and renal blood flow (IIb-B) Venodilators
Treat low perfusion:
Invasive hemodynamic monitoring: VTE prevention: Chronic medical therapy:
❑ DO NOT INITIATE ACE INHIBITORS during an acute decompensation Monitor laboratory tests: Management of hyponatremia:
❑ Optimization of chronic home medications | |||||||||||||||||
Complete Diagnostic Approach
A complete diagnostic approach should be carried out after a focused initial rapid evaluation is conducted and following initiation of any urgent intervention.[1][2]
Abbreviations:
ANA: Antinuclear antibody;
ARDS: Acute respiratory distress syndrome;
BNP: B-type natriuretic peptide;
BUN: Blood urea nitrogen;
CAD: Coronary artery disease;
CBC: Complete blood count;
CCB: Calcium channel blocker;
CHF: Congestive heart failure;
CT: Computed tomography;
CXR: Chest X-ray;
DM: Diabetes mellitus;
ECG: Electrocardiogram;
JVP: Jugular venous pressure;
HF: Heart failure;
HTN: Hypertension;
LVEF: Left ventricular ejection fraction;
LVH: Left ventricular hypertrophy;
MI: Myocardial infarction;
MRI: Magnetic resonance imaging;
NT-pro BNP: N-terminal pro-brain natriuretic peptide;
OCPs: Oral contraceptive pills;
PAWP: Pulmonary artery wedge pressure;
SBP: Systolic blood pressure;
S1: First heart sound;
S3: Third heart sound;
TSH: Thyroid stimulating hormone
Characterize the symptoms: Symptoms of left-sided fluid accumulation:
❑ Paroxysmal nocturnal dyspnea Obtain a detailed history:
❑ Medication history
❑ Family history
Determine the NYHA classification based on symptoms: | |||||||||||||||||||||||||||||||||
Examine the patient: General appearance: Vitals: ❑ Pulse
❑ Pulse oximetry (maintain oxygen sat ≥ 94% unless COPD) Weight: Skin Neck examination: Respiratory examination Cardiovascular examination
Abdominal examination Extremity examination Neurological examination Determine status of congestion and perfusion based on physical exam:
Low perfusion at rest (warm vs. cold)
The patient is: | |||||||||||||||||||||||||||||||||
Order tests: Routine (Class I, level of evidence C)
❑ BNP or NT-pro BNP (if diagnosis is uncertain)
❑ Chest X-ray (Class I, level of evidence C)
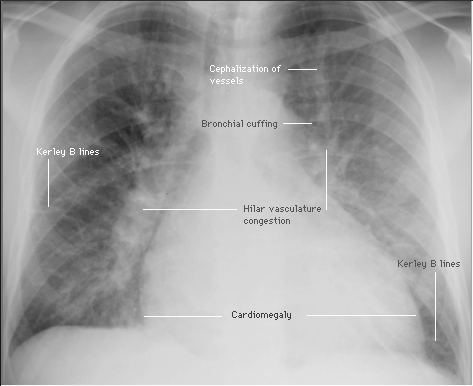 ❑ ECG (to help identify the cause of heart failure)
❑ 2-D echocardiography with Doppler
❑ Radionuclide ventriculography or MRI
❑ Coronary angiography looking for CAD Order additional tests to rule out other etiologies: | |||||||||||||||||||||||||||||||||
Consider alternative diagnoses:
| |||||||||||||||||||||||||||||||||
Assess the stage of heart failure using the ACCF/AHA staging system to guide chronic therapy
| |||||||||||||||||||||||||||||||||
Stage C ❑ Patients with structural heart disease
❑ Signs or symptoms of heart failure | |||||||||||||||||||||||||||||||||
Prevention of Heart Failure in Stage A and B
Shown below is an algorithm depicting the management of stage A and B heart failure.[1]
Abbreviations: ACE I: Angiotensin converting enzyme inhibitor; ACS: Acute coronary syndrome; CVD: Cardiovascular disease; DM: Diabetes mellitus; EF: Ejection fraction; HF: Heart failure; HTN: Hypertension; ICD: Implantable cardioverter defibrillator; MI: Myocardial infarction; PAD: Peripheral artery disease
What is the stage of heart failure (HF)? | |||||||||||||||||||||||||||
| Stage A At high risk for HF but without structural heart disease or symptoms of HF | Stage B Structural heart disease but without signs or symptoms of HF | ||||||||||||||||||||||||||
❑ Encourage healthy lifestyle and exercise | ❑ Encourage healthy lifestyle and exercise | ||||||||||||||||||||||||||
Consider additional measures in selected patients:
❑ Administer ACE-I if history of MI or ACS and reduced EF to prevent symptoms and reduce mortality (I-A), in all decreased EF to prevent symptoms (I-A) | |||||||||||||||||||||||||||
Treatment of Heart Failure in Stage C and D
Shown below is an algorithm depicting the management of stage C and D heart failure.[1]
Abbreviations: ACE I: Angiotensin converting enzyme inhibitor; ARB: Angiotensin II receptor blocker; ACS: Acute coronary syndrome; BID: Twice a day; BNP: Brain natriuretic peptide; CRT: Cardiac resynchronization therapy CVD: Cardiovascular disease; DM: Diabetes mellitus; EF: Ejection fraction; GDMT: Guideline determined medial therapy; GFR: Glomerular filtration rate; HF: Heart failure; HFrEF: Heart failure reduced ejectoon fraction; HFpEF: Heart failure preserved ejection fraction; HTN: Hypertension; ICD: Implantable cardioverter defibrillator; LVEF: Left ventricular ejection fraction; MCS: Mechanical circulatory support; NYHA: New York Heart Association; MI: Myocardial infarction; PAD: Peripheral artery disease; TID: Three times a day
What is the stage of heart failure (HF)? | |||||||||||||||||||||||||||||||
| Stage C HFrEF Structural heart disease with prior or current symptoms of HF and reduced ejection fraction | Stage C HFpEF Structural heart disease with prior or current symptoms of HF and preserved ejection fraction | Stage D Refractory HF requiring specialized interventions | |||||||||||||||||||||||||||||
Medical therapy:
|
PLUS
PLUS Add-on drugs in selected patients:
| Fluid restriction:
Inotropes
Mechanical circulatory support (MCS)
Cardiac transplantation
| |||||||||||||||||||||||||||||
Medications
| Drug Class | Drug | Daily dose | Maximum daily dose |
|---|---|---|---|
| Loop diuretics | Furosemide (duration of action: 6 to 8 h) |
PO dose for chronic heart failure: 20 to 40 mg once or twice IV dose for acute heart failure:
Initial IV bolus administered slowly over 1 to 2 minutes, then continuous IV infusion rate of 10-40 mg/h|| 600 mg | |
| Bumetanide (duration of action: 4 to 6 h) |
PO dose for chronic heart failure: 0.5 to 1.0 mg once or twice | 10 mg | |
| Torsemide (duration of action: 12 to 16 h) |
PO dose for chronic heart failure: 10 to 20 mg once | 200 mg | |
| Thiazide diuretics | Chlorothiazide (duration of action: 6 to 12 h) |
PO: 250 to 500 mg once or twice | 1000 mg |
| Hydrochlorothiazide (duration of action: 6 to 12 h) |
PO: 25 mg once or twice | 200 mg | |
| Metolazone (duration of action: 12 to 24 h) |
PO: 2.5 mg once | 20 mg | |
| K+- sparing diuretic | Amiloride (duration of action: 24 h) |
PO: 5 mg once | 20 mg |
| Spironolactone (duration of action: 1 to 3 h) |
PO: 12.5 to 25.0 mg once | 50 mg | |
| Triamterene (duration of action: 7 to 9 h) |
PO: 50 to 75 mg twice | 200 mg | |
| ACE inhibitors | Enalapril | 2.5 mg twice | 10 to 20 mg twice |
| Lisinopril | 2.5 to 5 mg once | 20 to 40 mg once | |
| Ramipril | 1.25 to 2.5 mg once | 10 mg once | |
| ARBs | Candesartan | 4 to 8 mg once | 32 mg once |
| Losartan | 25 to 50 mg once | 50 to 150 mg once | |
| Valsartan | 20 to 40 mg twice | 160 mg twice | |
| Beta blockers | Bisoprolol | 1.25 mg once | 10 mg once |
| Carvedilol | 3.125 mg twice | 50 mg twice | |
| Carvedilol CR | 10 mg once | 80 mg once | |
| Metoprolol succinate extended release | 12.5 to 25.0 mg once | 200 mg once | |
| Aldosterone antagonists | Spironolactone | 12.5 to 25.0 mg once | 25 mg once or twice |
| Eplerenone | 25 mg once | 50 mg once | |
| Inotropes | Dopamine | 5 to 10 mcg/kg/min, OR 10 to 15 mcg/kg/min |
|
| Dobutamine | 2.5 to 5 mcg/kg/min, OR 5 to 20 mcg/kg/min |
||
| Milrinone | 0.125 to 0.75 mcg/kg/min | ||
| Vasodilators | Nitroglycerin | 5 to 10 mcg/min, increase dose by 5-10mcg/min every 3-5 mins as tolerated |
Max is 400mcg/min |
| Nitroprusside | 5 to 10 mcg/min, increase dose by 5-10mcg/min every 5 mins as tolerated |
Max is 400mcg/min | |
| Nesiritide | 2 mcg/kg bolus; then 0.01 mcg/kg/minute continuous infusion | Max of 0.03 mcg/kg/minute | |
| Hydralazine and isosorbide dinitrate | Fixed-dose combination | 37.5 mg hydralazine/20 mg isosorbide dinitrate 3 times daily | 75 mg hydralazine/40 mg isosorbide dinitrate 3 times daily |
| Individual doses | Hydralazine: 25 to 50 mg 3 or 4 times daily Isosorbide dinitrate: 20 to 30 mg 3 or 4 times daily |
Hydralazine: 300 mg daily in divided doses Isosorbide dinitrate: 120 mg daily in divided doses | |
| Digoxin |
Loading dose: PO- 10 to 15 mcg/kg (half the total loading dose initially, then 1/4th the loading dose every 6 to 8 hours two times), OR |
Do's
Acute Decompensated Heart Failure
- Differentiate systolic and diastolic heart failure among patients with ADHF in order to guide therapy:
- Inotropic agents that increase contractility are not indicated as important for the patient with acute decompensated systolic heart failure.
- While beta blocker initiation is relatively contraindicated in acute decompensated systolic heart failure, control of tachycardia is very useful in the patient with diastolic heart failure to prolong left ventricular filling time.
- While the initiation of ACE inhibitors may not be recommended in acute decompensated systolic heart failure, ACE inhibition may be of benefit in acute decompensated diastolic heart failure.
- Rely on the patient's volume status to guide the aggressiveness of diuresis in ADHF.
- Continue chronic medications during acute decompensation in the following conditions:
- ACE inhibitor: may be continued if the patient is hemodynamically stable without a rising creatinine or hyperkalemia
- Beta blocker: may be continued in the absence of hypotension
- Aldosterone antagonist: may be continued in the absence of hypotension, hyperkalemia, and impaired renal function
- Digoxin decreases hospitalization but not mortality in the RALES study. It can be used in CHF & afib to reduce the ventricular response. In the RALES study, a level of < 1 ng/ml was associated with efficacy. Levels > 1 ng/ml not associated with greater efficacy and associated with higher mortality. No need to load a CHF patient with dig. For majority of patients with normal Cr, a daily dose of 0.25 mg of digoxin is usually adequate. In the older patient or in those patients with renal impairment, a dose of 0.125 mg per day may be adequate. Drugs that increase the concentration of digoxin include amiodarone, quinidine and verapamil. [6][7][8][9][10][11][12]
- DVT prophylaxis unless contraindicated.[13][14]
- Consider adding another diuretic (e.g. metolazone or thiazides) for worsening congestion despite high doses of loop diuretics.[15][16]
- Daily serum electrolytes, urea nitrogen, and creatinine concentrations should be measured during the use of IV diuretics or active titration of heart failure medications.
- Convert all IV diuretic to oral forms in anticipation of discharge.
- Schedule an early follow-up visit (within 7 to 14 days) and early telephone follow-up (within 3 days) of hospital discharge .[17][18]
Chronic Heart Failure
- Guideline-directed medical therapy (GDMT) is a term which represents the optimal medical therapy in the management of heart failure as defined by ACCF/AHA. These are primarily the class 1 recommendations. It involves the use of ACE inhibitors or (ARBs), beta blockers, aldosterone antagonists, and hydralazine/nitrate medications.
- Order an echocardiogram as soon as possible in the absence of a recent one or if the patient's clinical status is deteriorating.
Don'ts
- Avoid, if possible, NSAIDs, sympathomimetics, tricyclic antidepressants, class I and III antiarrhythmics (except amiodarone), and nondihydropyridine calcium channel blockers (diltiazem, verapamil as they can be harmful in acute decompensated HF. [19][20][21][22][23][24][25]
- Don't administer parenteral inotropes in normotensive patients with acute decompensated HF without evidence of decreased organ perfusion. [26]
- Don't combine an ACEI, ARB, and aldosterone antagonist in patients with HFrEF unless otherwise indicated as this combination carries a risk of renal dysfunction and hyperkalemia.
- Don't use aldosterone receptor antagonists in patients with hyperkalemia or renal insufficiency when serum creatinine is more than 2.5 mg/dL in men or more than 2.0 mg/dL in women (or estimated glomerular filtration rate <30 mL/min/1.73 m2), and/or potassium more than 5.0 mEq/L.[27][28]
- Don't use statins routinely without other indications.[29][30]
- Don't administer K+- sparing diuretic e.g amiloride or triamterene with aldosterone antagonist due to the elevated risk of hyperkalemia.
References
- ↑ 1.0 1.1 1.2 1.3 1.4 Yancy CW, Jessup M, Bozkurt B, Butler J, Casey DE, Drazner MH; et al. (2013). "2013 ACCF/AHA guideline for the management of heart failure: executive summary: a report of the American College of Cardiology Foundation/American Heart Association Task Force on practice guidelines". Circulation. 128 (16): 1810–52. doi:10.1161/CIR.0b013e31829e8807. PMID 23741057.
- ↑ Hunt SA, Abraham WT, Chin MH, Feldman AM, Francis GS, Ganiats TG; et al. (2009). "2009 Focused update incorporated into the ACC/AHA 2005 Guidelines for the Diagnosis and Management of Heart Failure in Adults A Report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines Developed in Collaboration With the International Society for Heart and Lung Transplantation". J Am Coll Cardiol. 53 (15): e1–e90. doi:10.1016/j.jacc.2008.11.013. PMID 19358937.
- ↑ Perna, ER.; Macín, SM.; Parras, JI.; Pantich, R.; Farías, EF.; Badaracco, JR.; Jantus, E.; Medina, F.; Brizuela, M. (2002). "Cardiac troponin T levels are associated with poor short- and long-term prognosis in patients with acute cardiogenic pulmonary edema". Am Heart J. 143 (5): 814–20. PMID 12040342. Unknown parameter
|month=ignored (help) - ↑ McMurray JJ, Adamopoulos S, Anker SD, Auricchio A, Böhm M, Dickstein K; et al. (2012). "ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure 2012: The Task Force for the Diagnosis and Treatment of Acute and Chronic Heart Failure 2012 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association (HFA) of the ESC". Eur Heart J. 33 (14): 1787–847. doi:10.1093/eurheartj/ehs104. PMID 22611136.
- ↑ Fuat A, Murphy JJ, Hungin AP, Curry J, Mehrzad AA, Hetherington A; et al. (2006). "The diagnostic accuracy and utility of a B-type natriuretic peptide test in a community population of patients with suspected heart failure". Br J Gen Pract. 56 (526): 327–33. PMC 1837840. PMID 16638247.
- ↑ The Captopril-Digoxin Multicenter Research Group. Comparative effects of therapy with captopril and digoxin in patients with mild to moderate heart failure. JAMA. 1988;259:539–44.
- ↑ Dobbs SM, Kenyon WI, Dobbs RJ. Maintenance digoxin after an episode of heart failure: placebo-controlled trial in outpatients. Br Med J. 1977;1:749–52
- ↑ Lee DC, Johnson RA, Bingham JB, et al. Heart failure in outpatients: a randomized trial of digoxin versus placebo. N Engl J Med. 1982;306: 699–705.
- ↑ Guyatt GH, Sullivan MJ, Fallen EL, et al. A controlled trial of digoxin in congestive heart failure. Am J Cardiol. 1988;61:371–5.
- ↑ . DiBianco R, Shabetai R, Kostuk W, et al. A comparison of oral milrinone, digoxin, and their combination in the treatment of patients with chronic heart failure. N Engl J Med. 1989;320:677–83.
- ↑ Uretsky BF, Young JB, Shahidi FE, et al., for the PROVED Investigative Group. Randomized study assessing the effect of digoxin withdrawal in patients with mild to moderate chronic congestive heart failure: results of the PROVED trial. J Am Coll Cardiol. 1993;22:955–62.
- ↑ Packer M, Gheorghiade M, Young JB, et al. Withdrawal of digoxin from patients with chronic heart failure treated with angiotensin-convertingenzyme inhibitors. RADIANCE Study. N Engl J Med. 1993;329:1–7.
- ↑ Alikhan R, Cohen AT, Combe S, Samama MM, Desjardins L, Eldor A; et al. (2003). "Prevention of venous thromboembolism in medical patients with enoxaparin: a subgroup analysis of the MEDENOX study". Blood Coagul Fibrinolysis. 14 (4): 341–6. PMID 12945875.
- ↑ Guyatt GH, Akl EA, Crowther M, Gutterman DD, Schuünemann HJ, American College of Chest Physicians Antithrombotic Therapy and Prevention of Thrombosis Panel (2012). "Executive summary: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines". Chest. 141 (2 Suppl): 7S–47S. doi:10.1378/chest.1412S3. PMC 3278060. PMID 22315257.
- ↑ Grosskopf I, Rabinovitz M, Rosenfeld JB (1986). "Combination of furosemide and metolazone in the treatment of severe congestive heart failure". Isr J Med Sci. 22 (11): 787–90. PMID 3793436.
- ↑ Rosenberg J, Gustafsson F, Galatius S, Hildebrandt PR (2005). "Combination therapy with metolazone and loop diuretics in outpatients with refractory heart failure: an observational study and review of the literature". Cardiovasc Drugs Ther. 19 (4): 301–6. doi:10.1007/s10557-005-3350-2. PMID 16189620.
- ↑ Krumholz HM, Chen YT, Wang Y, Vaccarino V, Radford MJ, Horwitz RI (2000). "Predictors of readmission among elderly survivors of admission with heart failure". Am Heart J. 139 (1 Pt 1): 72–7. PMID 10618565.
- ↑ Hernandez AF, Greiner MA, Fonarow GC, Hammill BG, Heidenreich PA, Yancy CW; et al. (2010). "Relationship between early physician follow-up and 30-day readmission among Medicare beneficiaries hospitalized for heart failure". JAMA. 303 (17): 1716–22. doi:10.1001/jama.2010.533. PMID 20442387.
- ↑ Heerdink ER, Leufkens HG, Herings RM, et al. NSAIDs associated with increased risk of congestive heart failure in elderly patients taking diuretics. Arch Intern Med. 1998;158:1108–12.
- ↑ . Herchuelz A, Derenne F, Deger F, et al. Interaction between nonsteroidal anti-inflammatory drugs and loop diuretics: modulation by sodiumbalance. J Pharmacol Exp Ther. 1989;248:1175–81.
- ↑ Gottlieb SS, Robinson S, Krichten CM, et al. Renal response to indomethacin in congestive heart failure secondary to ischemic or idiopathic dilated cardiomyopathy. Am J Cardiol. 1992;70:890–3
- ↑ Bank AJ, Kubo SH, Rector TS, et al. Local forearm vasodilation with intra-arterial administration of enalaprilat in humans. Clin Pharmacol Ther. 1991;50:314–21.
- ↑ The Cardiac Arrhythmia Suppression Trial (CAST) Investigators. Preliminary report: effect of encainide and flecainide on mortality in a randomized trial of arrhythmia suppression after myocardial infarction. N Engl J Med. 1989;321:406–12.
- ↑ The Cardiac Arrhythmia Suppression Trial II Investigators. Effect of the antiarrhythmic agent moricizine on survival after myocardial infarction. N Engl J Med. 1992;327:227–33.
- ↑ Pratt CM, Eaton T, Francis M, et al. The inverse relationship between baseline left ventricular ejection fraction and outcome of antiarrhythmic therapy: a dangerous imbalance in the risk-benefit ratio. Am Heart J. 1989;118:433–40.
- ↑ Cuffe MS, Califf RM, Adams KF, Benza R, Bourge R, Colucci WS, Massie BM, O'Connor CM, Pina I, Quigg R, Silver MA, Gheorghiade M (2002). "Short-term intravenous milrinone for acute exacerbation of chronic heart failure: a randomized controlled trial". JAMA : the Journal of the American Medical Association. 287 (12): 1541–7. PMID 11911756. Retrieved 2012-04-06. Unknown parameter
|month=ignored (help) - ↑ Juurlink DN, Mamdani MM, Lee DS, Kopp A, Austin PC, Laupacis A; et al. (2004). "Rates of hyperkalemia after publication of the Randomized Aldactone Evaluation Study". N Engl J Med. 351 (6): 543–51. doi:10.1056/NEJMoa040135. PMID 15295047.
- ↑ Bozkurt B, Agoston I, Knowlton AA (2003). "Complications of inappropriate use of spironolactone in heart failure: when an old medicine spirals out of new guidelines". J Am Coll Cardiol. 41 (2): 211–4. PMID 12535810.
- ↑ Horwich TB, MacLellan WR, Fonarow GC (2004). "Statin therapy is associated with improved survival in ischemic and non-ischemic heart failure". J Am Coll Cardiol. 43 (4): 642–8. doi:10.1016/j.jacc.2003.07.049. PMID 14975476.
- ↑ Gissi-HF Investigators. Tavazzi L, Maggioni AP, Marchioli R, Barlera S, Franzosi MG; et al. (2008). "Effect of rosuvastatin in patients with chronic heart failure (the GISSI-HF trial): a randomised, double-blind, placebo-controlled trial". Lancet. 372 (9645): 1231–9. doi:10.1016/S0140-6736(08)61240-4. PMID 18757089.